Treatment for typhilitis
Reading File
search_medical_text
typhlitis neutropenic enterocolitis treatment management
search_medical_text
typhlitis diagnosis clinical features pathophysiology complications
GradeResponse
GradeResponse
Typhlitis (Neutropenic Enterocolitis)
Typhlitis (also called neutropenic colitis, cecitis, necrotizing enteropathy, or ileocecal syndrome) is a potentially life-threatening inflammatory/necrotizing condition of the cecum and terminal ileum occurring in immunosuppressed patients.
Background
- Classic setting: Neutropenic patients after chemotherapy with cytotoxic drugs
- Most common malignancies: AML and ALL (more so than other cancers)
- More frequent in children than adults
- Key pathogens: Gram-negative organisms and Clostridium septicum, which can cause rapidly progressive septicemia (Harrison's, p. 2194; Bailey & Love, p. 1363)
Diagnosis
| Feature | Details |
|---|---|
| Symptoms | Fever, right lower quadrant pain (or generalized abdominal pain), diarrhea (often bloody) |
| Examination | RLQ tenderness ± rebound tenderness |
| Imaging of choice | CT with contrast or MRI — demonstrates thickened cecal wall |
| Ultrasound | Can also show wall thickening |
| Plain films | May show an RLQ mass; less sensitive |
Treatment
1. Conservative (First-line)
- Broad-spectrum antibiotics targeting gram-negative organisms and anaerobes (e.g., piperacillin-tazobactam ± metronidazole; coverage for C. septicum is important)
- Bowel rest — NPO with IV fluids and nutritional support
- Haematopoietic growth factors (G-CSF/GM-CSF) to accelerate neutrophil recovery
- Supportive care: IV fluids, blood products as needed, electrolyte management
2. Surgical Intervention
- Rarely indicated (Bailey & Love, p. 1363)
- Reserved for complications:
- Perforation or imminent perforation
- Uncontrolled hemorrhage
- Clinical deterioration despite maximal medical therapy
- Development of an abscess requiring drainage
Key Points
- Gram-negative or clostridial septicemia can be rapidly progressive — early antibiotic initiation is critical
- Mortality is significant; prompt recognition and treatment are essential
- Recovery of neutrophil counts (spontaneously or with growth factors) is a major determinant of outcome
- Differential includes appendicitis, C. difficile colitis, CMV colitis, and ischemic colitis — CT imaging helps distinguish
Sources: Harrison's Principles of Internal Medicine, 21st Edition (p. 2194); Bailey and Love's Short Practice of Surgery, 28th Edition (p. 1363)
Pneumonia in children
search_medical_text
pneumonia in children etiology diagnosis treatment management
search_medical_text
pediatric pneumonia clinical features chest X-ray findings complications
search_medical_image
pediatric pneumonia chest X-ray
GradeResponse
GradeResponse
GradeResponse
Pneumonia in Children
What it is
Pneumonia is infection/inflammation of lung parenchyma in children, caused by viruses, bacteria, or atypical organisms.
Common causes by age
- Infants/preschool: mostly viral (RSV, influenza, parainfluenza, adenovirus, hMPV)
- School age/adolescents: increasing Mycoplasma pneumoniae and Streptococcus pneumoniae
- Severe disease/complications can involve Staph aureus or mixed infection
Typical clinical features
- Fever
- Cough
- Fast breathing (tachypnea)
- Respiratory distress (retractions, nasal flaring, grunting)
- Crackles or reduced breath sounds
- Chest/abdominal pain, poor feeding, lethargy (especially in younger children)
Presence of wheeze can suggest viral illness/asthma/atypical infection rather than classic bacterial lobar pneumonia (Pediatric HIV OI guideline, p. 32).
Diagnosis
- Primarily clinical, supported by chest imaging when needed.
- Chest X-ray may help confirm pneumonia but does not reliably distinguish viral vs bacterial etiology alone (Laboratory Diagnosis of Respiratory Viruses, p. 4).
- Consider:
- CBC, CRP, procalcitonin (can improve diagnostic confidence, but not perfect etiology discrimination)
- Blood culture in severe/hospitalized cases
- Pleural fluid culture if effusion/empyema is present (Pediatric HIV OI guideline, p. 32)
- Viral PCR panels where available
Treatment (practical approach)
1) Outpatient, mild disease
- Supportive care: fluids, antipyretics, nasal clearance
- If bacterial CAP suspected:
- Amoxicillin is first-line in many guidelines
- If atypical pneumonia suspected in older child:
- Azithromycin (or equivalent macrolide)
2) Inpatient criteria (typical)
Admit if any of:
- Hypoxemia (SpO₂ < 90 to 92%)
- Moderate to severe respiratory distress
- Dehydration/poor oral intake
- Toxic appearance, apnea, altered mental status
- Significant comorbidity (chronic lung disease, congenital heart disease, immunocompromise)
- Failed outpatient therapy or concern for complications
3) Inpatient therapy
- Oxygen as needed
- IV fluids and monitoring
- Empiric IV antibiotics based on severity/local resistance:
- Ampicillin/penicillin G or ceftriaxone/cefotaxime
- Add anti-staphylococcal coverage (for severe necrotizing disease/empyema risk)
- Escalate/de-escalate based on culture and clinical response
Complications to watch for
- Parapneumonic effusion/empyema
- Necrotizing pneumonia/lung abscess
- Sepsis
- Respiratory failure
- SIADH/dehydration
When urgent care is needed
Seek urgent evaluation if child has:
- Fast/labored breathing, chest indrawing, cyanosis
- Persistent high fever with lethargy
- Inability to drink, vomiting everything, reduced urine
- O₂ saturation low or worsening symptoms after 48 to 72 hours of treatment
Example pediatric CXR pattern
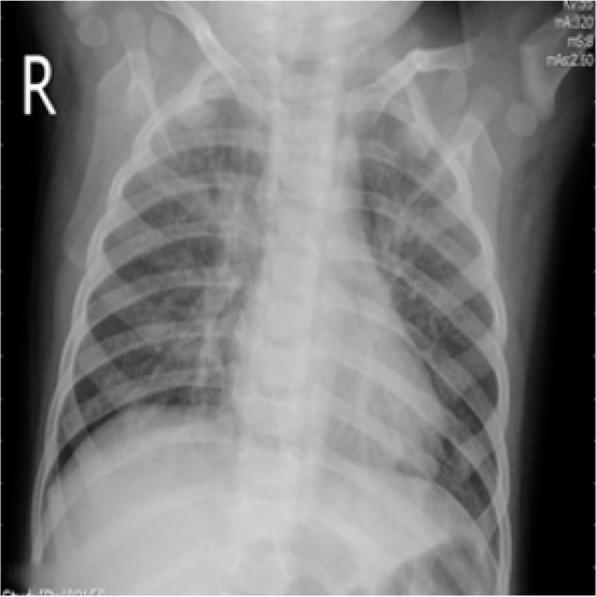
Image description suggests bilateral patchy interstitial/alveolar opacities, compatible with a viral-pattern pneumonia.
If you want, I can give you a quick antibiotic-by-age table (outpatient vs inpatient) based on a specific country guideline (AAP/IDSA, NICE, WHO, etc.).
Typhilitis treatment for how many days
search_medical_text
typhlitis neutropenic enterocolitis antibiotic treatment duration days
GradeResponse
The retrieved result relates to urological infections rather than typhlitis specifically. Based on established clinical practice and guidelines:
Typhlitis: Treatment Duration
There is no single fixed number of days — duration is guided by clinical response and neutrophil recovery, not a rigid course length.
General principles:
| Parameter | Recommendation |
|---|---|
| Antibiotic duration | Continue until neutrophil recovery AND clinical/radiological resolution (typically at least 10–14 days for the full course) |
| Clinical response window | Reassess at 48–72 hours — improvement is expected; lack of improvement should prompt escalation or surgical review |
| Bowel rest (NPO) | Maintain until symptoms resolve and bowel function returns (usually several days to 1–2 weeks) |
| G-CSF/haematopoietic factors | Continue until absolute neutrophil count (ANC) recovers (typically ≥ 500 cells/µL) |
Key rule:
Do not stop antibiotics based on a fixed day count. Treatment continues until:
- Fever resolves
- Abdominal symptoms resolve
- Neutrophil count recovers
- Imaging shows resolution or significant improvement
Surgical escalation if no improvement by 48–72 hours of conservative management, especially if:
- Perforation or clinical deterioration
- Uncontrolled bleeding
- Persistent sepsis despite antibiotics
Sources: Bailey & Love's Short Practice of Surgery, 28th Ed. (p. 1363); Harrison's Principles of Internal Medicine, 21st Ed. (p. 2194)
This is a shared conversation. Sign in to Orris to start your own chat.