make notes Fetal surgery for gastroschisis
Reading File
Finding Sources
Finding Sources
Searching PubMed
gastroschisis fetal surgery intervention
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Loading Image
Loading Image
I now have comprehensive material from all major sources. Here are the complete structured notes:
Fetal Surgery for Gastroschisis
1. Definition & Overview
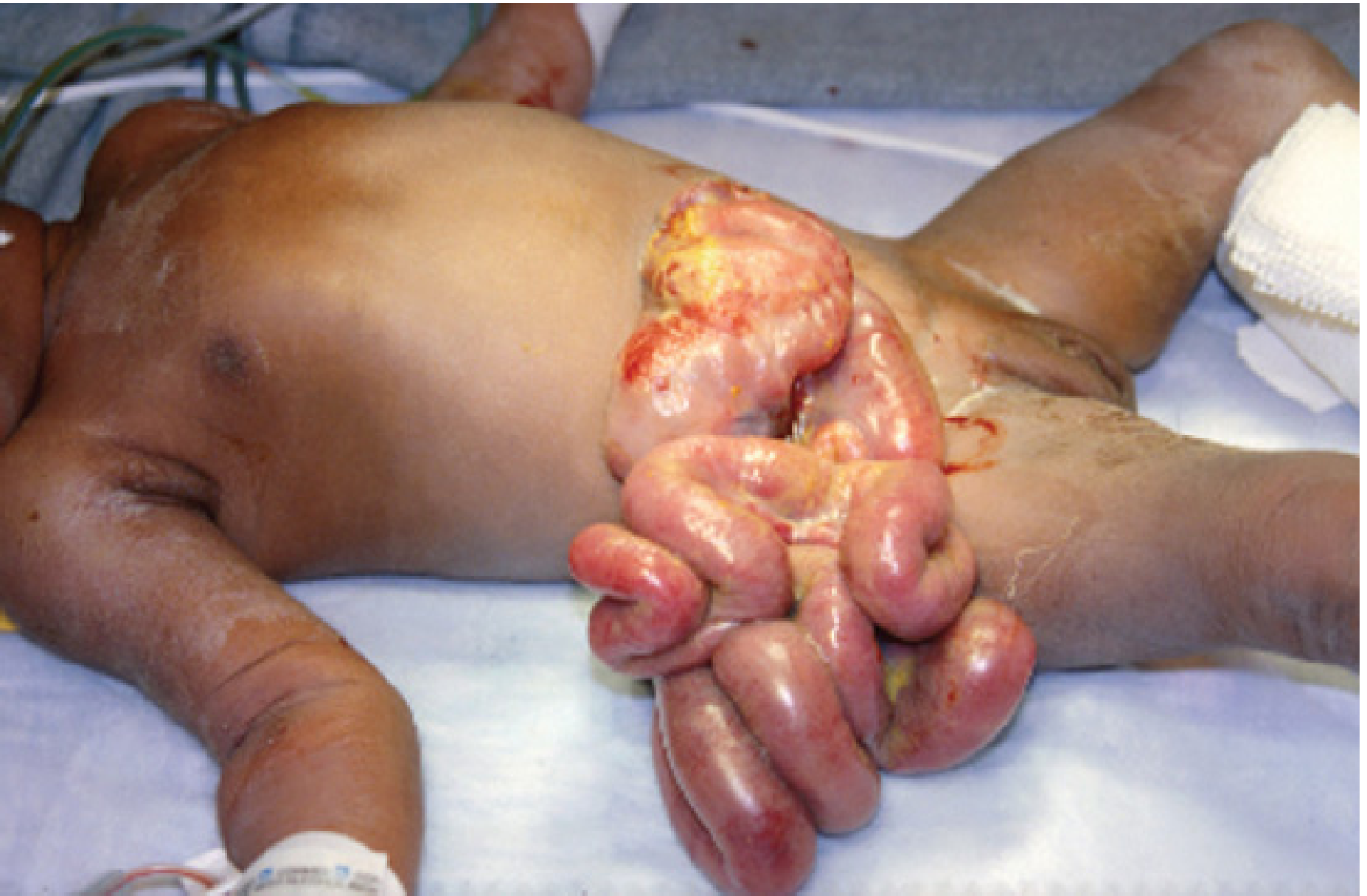
Gastroschisis is a full-thickness paraumbilical abdominal wall defect through which bowel (and occasionally other viscera) herniate freely into the amniotic fluid — without any covering sac.
- Defect is almost always to the right of the umbilicus (right umbilical vein involution theory)
- No overlying membrane (unlike omphalocele)
- Defect size typically < 4 cm
- Herniated organs exposed directly to amniotic fluid → inflammation, thickening, peel formation
2. Epidemiology & Risk Factors
| Parameter | Data |
|---|---|
| Incidence (worldwide) | ~1–5 per 10,000 live births |
| US trend | Tripled 1997–2008 (2.9 → 6.4:10,000), then decreased to 3.3:10,000 by 2018 |
| Peak demographic | Young mothers (< 25 years); risk 2–3× higher; age < 20 → 18:10,000 |
| Smoking | OR = 3.4 (95% CI 1.1–10.5) |
| Alcohol | RR = 1.40 (95% CI 1.13–1.70) |
| Illicit drugs | RR = 2.14 (95% CI 1.48–3.07) |
| Opioid-high areas | 5.1:10,000 vs 3.2:10,000 in low-opioid areas |
| Black women | RR = 0.49 (protective) |
| Familial cases | Distinctly rare |
— Creasy & Resnik's Maternal-Fetal Medicine, 9e
3. Pathogenesis
Embryogenesis remains incompletely understood. Five main theories:
- Somatopleural mesenchyme fails to differentiate → abdominal wall mesoderm fails to form
- Amnion rupture at base of umbilical ring during physiologic gut herniation
- Right umbilical vein premature involution → weakness at resorption site (most widely accepted)
- Right vitelline (omphalomesenteric) artery disruption
- Abnormal body wall folding
- Multifactorial: identified gene variants (NOS3, NPPA, ADD1, ICAM1, ICAM4, ICAM5, MTHFR) interacting with environmental exposures
Routine antenatal US has documented gastroschisis arising from ruptured hernia of the umbilical cord in utero — supporting a mechanical rather than global embryogenetic defect.
— Creasy & Resnik's; Mulholland & Greenfield's Surgery, 7e
4. Prenatal Diagnosis
Ultrasonographic Features
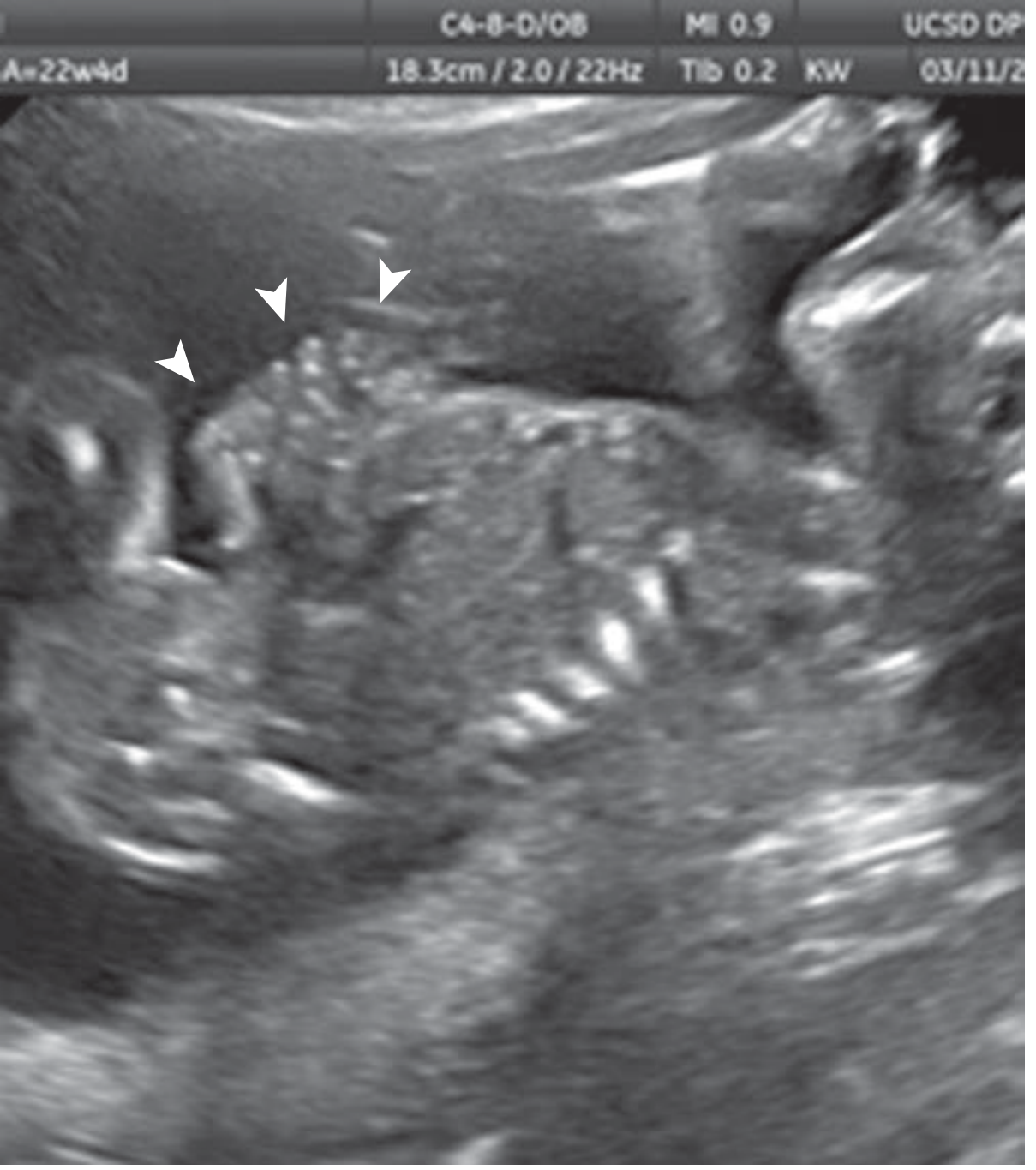
- Multiple loops of bowel floating freely in amniotic fluid — "cauliflower" appearance
- Defect at right side of abdominal cord insertion (color Doppler confirms)
- Intraabdominal and extraabdominal dilated bowel loops may appear late in pregnancy
- Complex gastroschisis: intraabdominal bowel dilation AND/OR liver or bladder herniation
- Maternal serum AFP elevated — 95% of cases diagnosed prenatally with widespread screening
Differential Diagnosis
| Condition | Distinguishing Feature |
|---|---|
| Physiologic gut herniation | Resolves by 12 weeks; before 10 weeks is normal |
| Ruptured omphalocele | Umbilical cord inserts medially within mass (vs. lateral in gastroschisis) |
| Limb-body wall complex | Larger mass, often adherent to placenta, short umbilical cord |
| Pentalogy of Cantrell | Multiple midline defects |
| Bladder/cloacal exstrophy | Different anatomical location |
- Aneuploidy: isolated gastroschisis is NOT typically associated with chromosomal abnormalities → invasive testing not routinely warranted (unlike omphalocele, where 40% have aneuploidy)
5. Classification
| Type | Definition |
|---|---|
| Simple gastroschisis | Isolated bowel herniation, no bowel compromise |
| Complex gastroschisis | Bowel atresia, volvulus, necrosis, perforation, or organ herniation (liver/bladder) — ~10–15% of cases |
6. Associated Anomalies
- ~85% occur in isolation
- Intestinal atresia/stenosis in ~10% (due to mechanical/vascular compromise of herniated bowel)
- Rarely: complete loss of small bowel from volvulus in utero
- Non-GI anomalies (arthrogryposis, cardiac, genitourinary) < 5%
- Oligohydramnios common; polyhydramnios with concomitant bowel atresia
- Fetal growth restriction (FGR) often present — standard Hadlock formula underestimates weight (AC is undersized); use Siemer or Shepard formulas
7. Antenatal Management
- Serial ultrasound to monitor:
- Fetal growth
- Amniotic fluid volume
- Bowel dilation (consistency of data as prognostic marker is limited)
- Doppler assessment of umbilical and cerebral arteries
- Fetal echocardiogram to confirm normal cardiac anatomy
- Non-stress test / biophysical profile twice weekly from 32–34 weeks (earlier if growth restriction)
- Multidisciplinary consultation: neonatology + pediatric surgery pre-delivery
- Delivery planning:
- Consider induction at 37 weeks to reduce bowel damage and shorten time to oral feeds
- Delivery before 37 weeks only if non-reassuring fetal status or poor growth
- No advantage to cesarean over vaginal delivery
- Early delivery (< 36 weeks) → significantly longer hospital stay and time to enteral feeds
8. Rationale for Fetal Intervention
The key problem in gastroschisis is not the defect itself but in utero bowel damage from prolonged amniotic fluid exposure:
- Amniotic fluid is intrinsically toxic to bowel serosa → inflammation, thickening, peel
- Leads to delayed GI motility, prolonged NICU stay, TPN dependence
- Gastroschisis is one of the leading causes of short bowel syndrome and intestinal transplantation in children
- Theoretical goal: intervene in utero to minimize bowel damage before birth
"There is currently no proven effective in utero intervention… To date, maternal-fetal intervention for gastroschisis remains limited to experimental models." — Sabiston Textbook of Surgery, 21e
9. Current Status of Fetal Intervention
9a. Fetoscopic In Utero Repair (Complex Gastroschisis)
- Currently under investigation — open Phase I feasibility study evaluating fetoscopic in utero repair of complex gastroschisis
- Rationale: reduce bowel exposure duration in most severely affected cases
- Technique would mirror fetoscopic MMC repair: minimally invasive endoscopic access to amniotic cavity
- Major limitation: preterm delivery risk, PROM, chorioamnionic separation
9b. Transamniotic Stem Cell Therapy (TRASCET) — Experimental
This is the most promising emerging approach:
Mechanism:
- Amniotic fluid naturally contains fetal mesenchymal stem cells (MSCs) with wound-healing properties
- Amniotic fluid exerts dual effects: it damages bowel (toxicity) but also participates in healing via native stem cells
- TRASCET delivers a concentrated dose of expanded amniotic fetal MSCs via intra-amniotic injection → tips the balance toward healing
Evidence (preclinical):
- Rodent model of gastroschisis: bowel damage reduced when amniotic fetal MSCs delivered in concentrated dose via intra-amniotic injection
- Fetal MSCs show trilineage potential and unique wound-healing capability
- TRASCET also applied to CDH models → reduction in arterial wall thickness vs. untreated group
Proposed workflow:
- Expanded fetal MSCs delivered by intra-amniotic injection in utero
- Infant born → postnatal surgery to reduce abdominal viscera and close defect
- Normal postnatal surgical pathway followed
— Sabiston Textbook of Surgery, 21e
9c. Animal Modeling — Feasibility Established
- Early animal studies confirmed in utero surgical intervention is safe in a fetal sheep model of gastroschisis
- Rodent and ovine models have been primary platforms for testing TRASCET and fetoscopic approaches
10. Postnatal Surgical Treatment (Standard of Care)
All infants with gastroschisis require urgent postnatal surgery. This is important context for understanding what fetal surgery aims to improve upon.
Initial Resuscitation
- Vigorous IV fluid resuscitation: 160–190 mL/kg/day to replace evaporative losses
- Cover exposed bowel to minimize heat and fluid loss
- Prophylactic antibiotics
Surgical Options
| Approach | Indication | Detail |
|---|---|---|
| Primary closure | Pliable bowel, small amount | Bowel reduced, abdominal wall closed primarily; may use mechanical stretching, orogastric decompression, rectal irrigation |
| Staged silo reduction | Thickened/edematous bowel | Plastic spring-loaded silo placed under fascia; graduated daily reduction over 1–2 weeks as edema resolves |
| Non-surgical closure | Selected cases | Umbilical cord placed over defect, covered with transparent occlusive dressing; cord provides natural coverage |
Caution during reduction: monitor bladder or airway pressures to prevent abdominal compartment syndrome from elevated intraabdominal pressure.
Postoperative Course
- Intestinal function returns over several weeks (especially if bowel is thickened/edematous)
- Central line placement + TPN required
- Feeding advancement is slow — weeks to reach full enteral nutrition
- If intestinal atresia present at primary repair → reduce bowel, return in weeks after edema resolves to correct atresia
11. Prognosis
| Outcome | Data |
|---|---|
| Survival (simple gastroschisis) | > 95% |
| Perinatal mortality (complex gastroschisis) | 16.7% (RR = 5.39; 95% CI 2.42–12.01) |
| NICU stay | Average ~30 days to achieve enteral feeds |
| Time to full feeds (complex) | 90 days vs 27 days (simple), P < 0.001 |
| Short bowel syndrome | ~5% |
| Dysfunctional bowel (long-term) | ~50% |
| Necrotizing enterocolitis (short-term) | 4.5% |
| Sepsis | Up to 8.6% |
| Recurrence risk | Up to 5% |
Best prognostic indicator: condition of bowel at birth
- Pliable, non-distended → uncomplicated course likely
- Distended, atretic, or necrotic → worse prognosis
Each earlier week of gestation → OR = 1.4 for adverse outcomes (neonatal death, bowel complications, gastrostomy, NEC).
12. Key Takeaways for Fetal Surgery
| Concept | Summary |
|---|---|
| Standard treatment | Postnatal surgery — primary closure or staged silo |
| Fetal surgery status | Experimental; no proven in utero intervention exists yet |
| Driving rationale | Amniotic fluid toxicity → bowel damage → short bowel, TPN dependence |
| Most promising approach | TRASCET (intra-amniotic MSC injection) — preclinical success in rodent/ovine models |
| Active trial | Open Phase I feasibility study of fetoscopic repair for complex gastroschisis |
| Delivery timing | Induction at 37 weeks; no benefit to cesarean or early delivery |
| Prenatal monitoring | Serial US, Doppler, BPP twice weekly from 32–34 weeks |
Sources:
- Sabiston Textbook of Surgery, 21e — Maternal-Fetal Surgery ch.
- Creasy & Resnik's Maternal-Fetal Medicine, 9e — Gastroschisis ch.
- Mulholland & Greenfield's Surgery, 7e — Gastroschisis ch.
- Schwartz's Principles of Surgery, 11e — Gastroschisis ch.
Recent evidence note: A 2024–2026 systematic review and meta-analysis series (PMID 39180201, PMID 41617611) has examined animal models of complex gastroschisis and biomarkers predicting complex gastroschisis perinatally — confirming active translational research interest in prenatal intervention but no change yet to clinical practice guidelines.
This is a shared conversation. Sign in to Orris to start your own chat.