I'm just entering opthal posting, guide me please
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Based on what I've gathered from Kanski's Clinical Ophthalmology and the Wills Eye Manual, here's a practical orientation guide for your ophthalmology posting:
Welcome to Ophthalmology Posting
1. The Ophthalmic History
Every encounter starts with a structured history. Key components:
- Main complaint: onset (sudden vs gradual), severity, duration, frequency
- Past ocular history: prior surgery, trauma, inflammation
- Past medical history: diabetes, hypertension, thyroid disease (all affect the eye)
- Systemic medications: corticosteroids (cause cataracts/glaucoma), tamsulosin (IFIS during cataract surgery), antimalarials (maculopathy)
- Allergies: topical antibiotics, glaucoma drops
- Family history: glaucoma, macular degeneration, inherited retinal disease
- Occupation/hobbies: important for visual demands and injury risk
2. Core Examination Skills to Master Early
Visual Acuity (VA) — your most important measurement
- Test each eye separately; always test the worse eye first
- Use the patient's glasses/contacts first (corrected VA)
- If VA < 6/6, repeat with a pinhole — improvement suggests a refractive cause
- Know the notation: 6/6 (metric) = 20/20 (imperial) = normal
- For very poor VA: record as Counting Fingers (CF), Hand Movements (HM), Perception of Light (PL), or No Perception of Light (NPL)
- Best-corrected VA (BCVA) is the gold standard for clinical decisions
Slit-Lamp Biomicroscopy
- The workhorse of ophthalmic examination
- Systematically examine: lids → conjunctiva → cornea → anterior chamber (look for cells/flare) → iris → lens
- Learn to adjust illumination: diffuse, direct focal, retro-illumination
Fundus Examination
- Learn indirect ophthalmoscopy (wide field) and direct ophthalmoscopy (disc detail)
- Systematic approach: optic disc → cup:disc ratio → vessels → macula → periphery
- Cup:disc ratio >0.6 or asymmetry >0.2 raises suspicion for glaucoma
Tonometry (IOP measurement)
- Normal: 10–21 mmHg
- Goldmann applanation tonometry is the gold standard
- Remember: corneal thickness affects readings — thin corneas underestimate true IOP
Gonioscopy
- Examines the drainage angle of the eye
- Essential for classifying glaucoma (open-angle vs closed-angle)
3. Common Presentations You'll Encounter
| Symptom | Think of |
|---|---|
| Sudden painless loss of vision | CRAO, CRVO, vitreous haemorrhage, retinal detachment |
| Painful red eye + decreased vision | Acute angle closure glaucoma, anterior uveitis, keratitis |
| Gradual painless vision loss | Cataract, glaucoma, AMD, diabetic maculopathy |
| Floaters + flashes | Posterior vitreous detachment → rule out retinal tear/detachment |
| Diplopia | CN III/IV/VI palsy, thyroid eye disease, decompensated phoria |
| Proptosis | Thyroid eye disease, orbital cellulitis, tumour |
| Ptosis | CN III palsy, Horner syndrome, myasthenia gravis, senile |
| Watering eye (epiphora) | Nasolacrimal duct obstruction, ectropion, dry eyes (reflex tearing) |
4. Key Investigations
- Perimetry (visual fields): Humphrey automated perimetry for glaucoma, neurological lesions
- OCT (Optical Coherence Tomography): Cross-sectional retinal imaging — essential for macula and glaucoma
- Fluorescein Angiography: Vascular diseases, AMD, diabetic retinopathy
- B-scan ultrasound: When fundus is not visible (dense cataract, vitreous haemorrhage)
- Corneal topography: For keratoconus, pre-surgical assessment
5. Practical Tips for the Ward & OPD
- Always wash hands and disinfect the slit-lamp chin rest between patients
- When instilling dilating drops (tropicamide 1% ± phenylephrine 2.5%), warn patients about blurred near vision and photophobia for 4–6 hours; advise them not to drive
- In any red eye, check IOP before prescribing steroids — steroids in a herpetic corneal ulcer can be catastrophic
- Never patch a red eye without a diagnosis — you could worsen infectious keratitis
- Always check the relative afferent pupillary defect (RAPD) with the swinging torch test — it's a critical sign of optic nerve or extensive retinal disease
- For trauma cases — do not apply pressure to the eye if globe rupture is suspected
6. Must-Know Emergencies
| Emergency | Key Feature | Immediate Action |
|---|---|---|
| Acute angle-closure glaucoma | Rock-hard eye, hazy cornea, IOP often >40 | IV acetazolamide, topical pilocarpine, urgent laser |
| Central retinal artery occlusion | Sudden painless monocular blindness, cherry-red spot | Ocular massage, refer urgently (within hours) |
| Orbital cellulitis | Proptosis + restricted EOM + fever | IV antibiotics, CT orbit, admit |
| Endophthalmitis | Post-op/post-trauma, severe pain, hypopyon | Intravitreal antibiotics urgently |
| Chemical injury | Acid or alkali splash | Immediate copious irrigation BEFORE anything else |
7. Your Two Main Reference Books in This Posting
- Kanski's Clinical Ophthalmology (10th ed.) — comprehensive, systematic, excellent for building foundations
- Wills Eye Manual — symptom-based, practical, great for quick OPD/ER reference
Use Kanski's for understanding diseases in depth; use Wills for rapid symptom-to-diagnosis navigation.
Good luck in your posting! Ophthalmology has a steep learning curve with equipment and technique, but once you get comfortable with the slit lamp and indirect ophthalmoscope, everything clicks. Focus on the basics — VA, RAPD, slit lamp, fundus — and you'll be well ahead.
What are the common cases and checklist on must clerk case
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Based on both textbooks (Kanski's and Wills Eye Manual), here is a comprehensive guide to the must-clerk cases in ophthalmology and what to cover for each:
Must-Clerk Cases in Ophthalmology Posting
The 10 Core Case Categories
| # | Condition | Why You Must Clerk It |
|---|---|---|
| 1 | Cataract | Most common elective surgery; systemic links |
| 2 | Glaucoma | Chronic, silent; IOP + fields + disc assessment |
| 3 | Diabetic Retinopathy | Most common cause of blindness in working-age adults |
| 4 | Conjunctivitis (bacterial/viral/allergic) | Most common red eye in OPD |
| 5 | Acute Angle-Closure Glaucoma | Ophthalmic emergency |
| 6 | Anterior Uveitis (Iritis) | Red eye + systemic associations |
| 7 | Retinal Detachment | Surgical emergency |
| 8 | Corneal Ulcer / Keratitis | Red eye + vision threat |
| 9 | Ptosis | Broad differential; neurological links |
| 10 | Age-Related Macular Degeneration (AMD) | Most common cause of blindness >50 years |
Case-by-Case Clerking Checklist
1. CATARACT
Presenting complaint: Gradual painless blurring, glare, difficulty reading, colour desaturation
History checklist:
- Age of onset, which eye affected, rate of progression
- Glare worse in sunlight or oncoming headlights? (posterior subcapsular)
- Near vs distance vision — which is worse?
- Systemic: diabetes, steroid use, trauma history
- Family history of early cataract
Examination:
- Best-corrected VA (both eyes)
- Pinhole improvement?
- Red reflex — asymmetry or absent?
- Slit-lamp: type of cataract (nuclear sclerosis / cortical / posterior subcapsular / anterior subcapsular)
- Pupil dilation for fundus assessment (exclude posterior segment disease)
Key to note: Confirm visual needs vs cataract density — surgery indication is functional, not just VA number.
2. GLAUCOMA (Primary Open-Angle)
Presenting complaint: Often asymptomatic; incidental finding; tunnel vision late stage
History checklist:
- Family history of glaucoma (first-degree relative = major risk factor)
- Known myopia (risk factor)
- Steroid use (topical/systemic — steroid-induced glaucoma)
- History of ocular hypertension
- Current eye drops — compliance, side effects
Examination:
- VA (often preserved until late)
- IOP (both eyes) — normal ≠ no glaucoma
- RAPD (if asymmetric damage)
- Slit-lamp: anterior segment, corneal thickness estimate
- Fundus: optic disc — CDR, rim thinning (especially inferior > superior > nasal > temporal = ISNT rule), disc haemorrhages, peripapillary atrophy
- Visual field defects: arcuate scotoma, nasal step, altitudinal defects
3. DIABETIC RETINOPATHY
Presenting complaint: Blurred vision, floaters, sudden visual loss (vitreous haemorrhage)
History checklist:
- Type and duration of diabetes
- HbA1c — current and trend
- BP and lipid control
- Last retinal screening and result
- Renal involvement (nephropathy correlates with retinopathy severity)
- Pregnancy (accelerates DR)
Examination:
- VA both eyes
- IOP (neovascular glaucoma risk)
- Dilated fundus: classify — NPDR (mild/moderate/severe) vs PDR
- Macular oedema — clinically significant? (use OCT if available)
- New vessels at disc (NVD) or elsewhere (NVE)?
- Vitreous — haemorrhage, traction?
Classification to know:
- Non-proliferative DR: microaneurysms → haemorrhages → hard exudates → cotton wool spots → venous beading → IRMA
- Proliferative DR: new vessel formation → vitreous haemorrhage → traction retinal detachment
4. CONJUNCTIVITIS
Presenting complaint: Red eye, discharge, grittiness — usually bilateral and painless
History checklist:
- Discharge type: watery (viral/allergic) vs mucopurulent (bacterial)
- Itching (hallmark of allergic conjunctivitis)
- URTI contact / sick contacts (viral)
- Contact lens wear
- Atopy, hay fever, eczema (allergic)
- Neonatal? (consider gonococcal/chlamydial — important!)
- Any visual blurring? (if yes — not simple conjunctivitis, look further)
Examination:
- VA — should be normal
- Lid: follicles (viral/chlamydial) vs papillae (bacterial/allergic)?
- Discharge character
- Cornea: clear? (if not, consider keratoconjunctivitis)
- Pre-auricular lymphadenopathy (viral conjunctivitis)
5. ACUTE ANGLE-CLOSURE GLAUCOMA
Presenting complaint: Sudden severe eye pain, headache, nausea/vomiting, halos around lights, decreased vision
History checklist:
- Onset — sudden, unilateral?
- Previous similar attacks (subacute closure)?
- Precipitant: dim lighting, mydriatic drops, emotional stress
- Systemic history: hypermetropia (short axial length = risk)
- Medications that can precipitate: anticholinergics, antihistamines, sympathomimetics
Examination:
- VA — reduced
- IOP — typically >40 mmHg, rock-hard eye
- Cornea — hazy (epithelial oedema)
- Pupil — mid-dilated, oval, unreactive
- Anterior chamber — very shallow, flare
- Gonioscopy (once acute attack controlled): closed angle
- Check fellow eye — also narrow angle?
6. ANTERIOR UVEITIS (IRITIS)
Presenting complaint: Painful red eye + photophobia + blurred vision + tearing
History checklist:
- Unilateral or bilateral?
- First episode or recurrent?
- Systemic review: back pain/stiffness (ankylosing spondylitis — most common association), skin rash (psoriasis, sarcoid), bowel symptoms (IBD), joint pain
- STI history (Reiter's, syphilis)
- TB exposure
- Herpetic eye disease history
Examination:
- VA
- Ciliary flush (limbal injection > peripheral injection)
- Cornea: keratic precipitates (KPs) — fine (non-granulomatous) vs large mutton-fat (granulomatous = TB, sarcoid, syphilis)
- Anterior chamber: cells and flare (grade 0–4)
- Pupil: irregular (posterior synechiae)?
- IOP: may be low (ciliary body suppression) or high (trabeculitis)
- Fundus: vitreous spill-over? (if so, think intermediate/panuveitis)
7. RETINAL DETACHMENT
Presenting complaint: Floaters, flashes (photopsia), then a "curtain" or "shadow" across vision
History checklist:
- Onset of floaters/flashes vs onset of field defect — gap matters (time-sensitive surgery)
- Which quadrant is the shadow? (superior field defect = inferior retinal detachment — worse prognosis as macula threatened sooner)
- Is the macula on or off? (VA guide)
- High myopia (major risk factor)
- Prior cataract surgery (aphakic/pseudophakic RD)
- Fellow eye — previous RD or lattice degeneration?
- Trauma history
Examination:
- VA
- Dilated fundus with indirect ophthalmoscopy: location of detachment, find the break, macula status
- IOP: low IOP supports rhegmatogenous RD
8. CORNEAL ULCER / KERATITIS
Presenting complaint: Painful red eye, photophobia, discharge, reduced VA, foreign body sensation
History checklist:
- Contact lens wear (Pseudomonas, Acanthamoeba — must ask!)
- Previous herpes labialis or eye disease (HSV keratitis)
- Recent trauma — vegetative matter? (fungal keratitis)
- Immunocompromised state
- Topical steroid use (masks and worsens infection)
Examination:
- VA
- Slit-lamp:
- Epithelial defect stained with fluorescein (size, location, margins)
- Stromal infiltrate
- Corneal sensation (reduced in HSV — use cotton wisp)
- Dendrites = HSV keratitis (branching, terminal bulbs)
- Hypopyon in anterior chamber?
- Corneal scraping for culture and microscopy (before starting treatment)
9. PTOSIS
Presenting complaint: Drooping upper eyelid — may be cosmetic complaint, or noticed by others
History checklist:
- Unilateral or bilateral?
- Onset — congenital vs acquired; sudden vs progressive?
- Diurnal variation — worse in evening? (myasthenia gravis)
- Diplopia, difficulty chewing/swallowing (myasthenia)
- Headache, dilated pupil (CN III palsy — aneurysm until proven otherwise!)
- Anhidrosis, miosis (Horner syndrome — congenital? carotid/lung pathology?)
- Thymoma, lung cancer (paraneoplastic)
Examination:
- MRD1 (marginal reflex distance) — normal ~4 mm
- Levator function (lid excursion from downgaze to upgaze)
- Upper lid crease height
- Pupil: dilated (CN III), miotic (Horner), normal (aponeurotic/myasthenic)
- Extraocular movements
- Fatigability test (prolonged upgaze — MG)
- Phenylephrine test for Horner's
10. AGE-RELATED MACULAR DEGENERATION (AMD)
Presenting complaint: Central visual distortion (metamorphopsia), central scotoma, difficulty reading or recognising faces — bilateral but often asymmetric
History checklist:
- Age >50, smoking history (strongest modifiable risk factor)
- Family history of AMD
- Fellow eye involvement?
- Sudden recent worsening? (suggests conversion to wet AMD — subretinal haemorrhage)
- Diet (antioxidant intake) and supplements (AREDS2)
Examination:
- VA
- Amsler grid — essential in every AMD patient, check for distortion or scotoma
- Dilated fundus:
- Drusen — size, number, distribution (soft large drusen = high risk)
- Geographic atrophy (dry AMD)
- Subretinal fluid, haemorrhage, CNV membrane (wet AMD)
- OCT: gold standard for detecting subretinal/intraretinal fluid
Quick Summary: What to Always Document in Every Ophthalmic Clerking
□ Presenting complaint + duration
□ VA — each eye separately, with and without correction, pinhole if <6/6
□ RAPD — swinging torch test
□ IOP — both eyes
□ Anterior segment (slit-lamp): lids, conjunctiva, cornea, AC, lens
□ Posterior segment (dilated): disc, macula, vessels, periphery
□ Relevant systemic history (DM, HT, autoimmune, medications)
□ Family history of eye disease
□ Functional impact — driving, work, daily activities
Kanski's Clinical Ophthalmology (10th ed.) and the Wills Eye Manual are your two key references — Kanski for depth on each disease, Wills for rapid symptom-to-diagnosis at the bedside. Good luck!
Can you create a checklist on cases to clerk as common chief complaints and conditions
Reading File
Running Command
Running Command
Writing File
Running Command
Editing File
Editing File
Reading File
Editing File
Editing File
Reading File
Running Command
Running Command
Running Command
Running Command
Running Command
The file is valid — 19 KB, properly structured DOCX with all expected XML parts. Here's your download:
Ophthalmology Clerking Checklist
Word Document · DOCX
The checklist is organised into 4 sections:
| Section | Contents |
|---|---|
| A. Universal Clerking | Applies to every single case — VA, RAPD, IOP, slit-lamp, fundus, systemic Hx |
| B. By Chief Complaint | 7 chief complaint groups with dedicated history + exam checklists |
| C. Quick Reference Grid | 15 must-clerk conditions in a table — key symptom, must-check finding, emergency flag |
| D. Before You Leave | Final signoff checklist before moving to the next patient |
Chief complaints covered: Red Eye · Gradual Painless Vision Loss · Sudden Painless Vision Loss · Floaters/Flashes · Diplopia · Ptosis · Watering Eye
Conditions covered: Cataract · POAG · AACG · Conjunctivitis · Corneal Ulcer · Anterior Uveitis · Diabetic Retinopathy · Retinal Detachment · CRAO · CRVO · Dry & Wet AMD · Ptosis · CN Palsy · Epiphora
Each item has a tick box (☐) so you can use it as a physical checklist during clerking.
We will go through basic eye anatomy Common presenting complaints Visual acuity and basic examination External examination and torch light examination - please read on RAPD Will show you all the basic slit lamp examination Fundus basics
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
That's your complete pre-session study guide covering all 6 topics. A few things worth highlighting before your session:
On RAPD — the most commonly tested clinical sign:
- The key concept is that RAPD is an afferent problem (optic nerve/retina), not an efferent one (no anisocoria at rest)
- The affected eye's pupil dilates when you swing the light to it — because the brain sees less light coming in from that side
- The classic causes to always remember: optic neuritis, CRAO, severe glaucoma (asymmetric), large retinal detachment
- Dense cataract alone does not cause RAPD — this is a classic exam question
On slit-lamp: When your consultant shows you the instrument, ask to be shown:
- A normal corneal optical section (thin slit, oblique beam)
- Fluorescein staining with cobalt blue filter
- AC cells and flare grading
- KPs on retroillumination
On fundus: The two most important things to nail early are finding the optic disc and locating the macula. Everything else follows from there.
Snells chart 6/6 meaning
Finding Sources
Reading File
Here's a clear breakdown, straight from Kanski's:
Snellen Chart — What 6/6 Means
The Snellen fraction is written as:
$$\frac{\text{Distance patient is tested at}}{\text{Distance a normal eye can read that line}}$$
So 6/6 means:
The patient reads at 6 metres what a normal eye can read at 6 metres.
That is the definition of normal vision.
Reading the Fraction
| Snellen | What it means | Interpretation |
|---|---|---|
| 6/6 | Reads at 6 m what normal reads at 6 m | Normal vision |
| 6/9 | Reads at 6 m what normal reads at 9 m | Mildly reduced |
| 6/12 | Reads at 6 m what normal reads at 12 m | Moderately reduced (driving cutoff in many countries) |
| 6/18 | Reads at 6 m what normal reads at 18 m | Significantly reduced |
| 6/36 | Reads at 6 m what normal reads at 36 m | Poor vision |
| 6/60 | Reads at 6 m what normal reads at 60 m | Very poor — legal blindness threshold in some definitions |
Note: Normal corrected VA in young adults is often better than 6/6 (e.g. 6/5 or 6/4) — meaning they can read at 6 m what a standard normal eye would need to be at 5 or 4 m to read.
The US / Imperial Equivalent
The same notation exists in feet (used in the US):
| Metric | Imperial |
|---|---|
| 6/6 | 20/20 |
| 6/12 | 20/40 |
| 6/60 | 20/200 |
The numbers are just the distances in feet instead of metres.
Why Letters Get Smaller Down the Chart
Each row is sized so that its letters subtend a 5-minute arc at the eye from the designated distance for that row. The critical gap within each letter (e.g. the opening in the letter C) subtends 1 minute of arc — this is the minimum angle of resolution (MAR) the normal eye can detect.
So 6/6 = MAR of 1 arcminute — the fundamental definition of normal visual acuity.
Practical Tip in Clinic
- Always record which eye (R/L), whether it is aided or unaided, and whether pinhole was used
- Example:
R VA: 6/18 (unaided) → 6/6 (pinhole)tells you the problem is refractive — correctable with glasses - Example:
R VA: 6/18 (unaided) → 6/18 (pinhole)tells you there is pathology — pinhole did not help
— Kanski's Clinical Ophthalmology, 10th ed.
Ointment and drops for tests and medication
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Here's a complete practical guide to all the eye drops and ointments you'll encounter in clinic — divided into diagnostic and therapeutic use.
Ophthalmic Drops & Ointments — Practical Guide
PART 1 — FOR EXAMINATION / DIAGNOSTIC USE
1. Mydriatics (Pupil Dilating Drops)
Used to dilate the pupil for fundus examination, or therapeutically for uveitis.
There are two mechanisms:
| Mechanism | Drug | How it works |
|---|---|---|
| Sympathomimetic | Phenylephrine | Stimulates iris dilator muscle |
| Cycloplegic (Parasympatholytic) | Tropicamide, Cyclopentolate, Atropine, Homatropine | Blocks iris sphincter AND ciliary muscle |
Drugs in Detail
| Drug | Concentration | Onset | Duration | Used For |
|---|---|---|---|---|
| Tropicamide | 1% | 20–30 min | 4 hours | Routine fundus exam — most common in OPD |
| Phenylephrine | 2.5% | 20 min | 3 hours | Combined with tropicamide for better dilation; does NOT cause cycloplegia |
| Cyclopentolate | 1% | 30 min | 6–24 hours | Children's refraction (cycloplegic refraction), uveitis |
| Atropine | 1% | 40 min | up to 12 days | Penalisation (amblyopia treatment); severe uveitis; children's refraction |
| Homatropine | 5% | 30 min | 1–3 days | Therapeutic cycloplegia for iritis/corneal abrasion |
In your OPD: You will most commonly use Tropicamide 1% alone or combined with Phenylephrine 2.5% for fundus exam.
What to Tell Every Patient Before Dilating
- Vision will be blurred for near for 4–6 hours (tropicamide)
- Eyes will be sensitive to light (photophobia) — bring sunglasses
- Do not drive after dilation
- Warn any patient with narrow angles — dilation can precipitate acute angle-closure glaucoma
Before You Dilate — Always Check
- Is the anterior chamber deep or shallow? (Torch light from temporal side — check for shadow on nasal iris)
- Any history of angle-closure glaucoma?
- Is it a head injury patient whose pupils need monitoring? → Do NOT dilate
2. Topical Anaesthetics
Used to anaesthetise the eye surface for:
- Tonometry (IOP measurement)
- Corneal foreign body removal
- Gonioscopy / contact lens examination
- Corneal scraping for culture
| Drug | Example | Onset | Duration |
|---|---|---|---|
| Proxymetacaine (Proparacaine) 0.5% | Minims | ~30 sec | ~15–20 min |
| Tetracaine (Amethocaine) 0.5–1% | Minims | ~30 sec | ~15–20 min |
| Oxybuprocaine 0.4% | Minims Benoxinate | ~30 sec | ~15–20 min |
Important: Topical anaesthetics are for in-clinic use only. Never give a patient a bottle to take home — they mask pain that protects the cornea, and repeated use is toxic to the corneal epithelium.
3. Fluorescein (Diagnostic Dye)
Fluorescein sodium — stains areas where the epithelium is disrupted (corneal abrasions, ulcers, dendrites). Viewed under cobalt blue light on the slit-lamp — stains bright green/yellow-green.
| Form | Use |
|---|---|
| Fluorescein strips (impregnated strips + saline drop) | Most common, single-use, sterile |
| Minims fluorescein 1–2% | Pre-made single-dose |
| Combined fluorescein + anaesthetic (e.g. Minims Fluorescein + Benoxinate) | Tonometry — one drop does both |
What it reveals:
- Corneal abrasion → uniform green patch
- Corneal ulcer → green-staining epithelial defect with edges
- Dendritic ulcer (HSV) → branching tree pattern with terminal bulbs
- Seidel's sign → aqueous leaking from a wound dilutes fluorescein → streaming dark "waterfall" on blue light = open globe
- Tear film — fluorescein used to measure tear break-up time (TBUT) in dry eye assessment
4. Rose Bengal / Lissamine Green
Stains devitalised (dead or damaged) epithelial cells — used in dry eye disease assessment. Rose Bengal stings; Lissamine green is better tolerated.
PART 2 — FOR TREATMENT / MEDICATION USE
5. Antibiotic Drops and Ointments
| Drug | Form | Use |
|---|---|---|
| Chloramphenicol 0.5% drops / 1% ointment | Drops + oint | Bacterial conjunctivitis — broad-spectrum, first-line |
| Ofloxacin 0.3% drops | Drops | Bacterial conjunctivitis, corneal ulcer |
| Ciprofloxacin 0.3% drops / ointment | Drops + oint | Corneal ulcer (pseudomonal keratitis — frequent dosing) |
| Moxifloxacin 0.5% drops | Drops | Broad-spectrum; no preservative in some formulations |
| Gentamicin 0.3% drops | Drops | Gram-negative coverage |
| Fusidic acid 1% gel | Gel | Staphylococcal blepharitis / conjunctivitis (good lid penetration) |
| Aciclovir 3% ointment | Ointment | HSV dendritic keratitis — 5x/day for 14 days |
| Ganciclovir 0.15% gel | Gel | HSV keratitis alternative |
Ointment vs drops: Ointments have longer contact time, useful at night or for lids (blepharitis). Drops are preferred during the day as they don't blur vision.
6. Anti-inflammatory Drops
Topical Steroids
| Drug | Potency | Use |
|---|---|---|
| Prednisolone acetate 1% | Strong | Anterior uveitis, post-op inflammation |
| Dexamethasone 0.1% | Strong | Uveitis, allergic, post-op |
| Fluorometholone 0.1% (FML) | Mild | Allergic conjunctivitis, superficial inflammation — lower IOP-raising risk |
| Loteprednol 0.5% | Mild-moderate | Allergic — low steroid side-effect profile |
Never start topical steroids without a diagnosis. Steroids on an undiagnosed herpetic ulcer → corneal melt. Steroids can raise IOP (steroid-induced glaucoma) and accelerate cataract formation.
NSAIDs (Topical)
| Drug | Use |
|---|---|
| Diclofenac 0.1% | Post-op pain/inflammation, cystoid macular oedema prevention |
| Ketorolac 0.5% | Allergic conjunctivitis, post-op |
| Bromfenac 0.09% | Post-cataract surgery inflammation |
7. Anti-allergic Drops
| Drug | Class | Use |
|---|---|---|
| Sodium cromoglicate 2–4% | Mast cell stabiliser | Allergic conjunctivitis — prophylactic, needs regular use |
| Nedocromil 2% | Mast cell stabiliser | Same as above |
| Olopatadine 0.1% | Antihistamine + mast cell stabiliser | Allergic conjunctivitis — fast relief |
| Ketotifen 0.025% | Antihistamine + mast cell stabiliser | Over-the-counter allergic conjunctivitis |
| Azelastine | Antihistamine | Seasonal allergic conjunctivitis |
8. Glaucoma Drops (IOP-Lowering)
| Class | Drug | Mechanism | Notes |
|---|---|---|---|
| Prostaglandin analogues | Latanoprost 0.005%, Bimatoprost, Travoprost | Increases uveoscleral outflow | Once daily (night); SE: iris/lash pigmentation |
| Beta-blockers | Timolol 0.25–0.5%, Betaxolol | Reduces aqueous production | Contraindicated in asthma, bradycardia |
| Carbonic anhydrase inhibitors | Dorzolamide 2%, Brinzolamide 1% | Reduces aqueous production | Can cause stinging; systemic: acetazolamide tablets for acute AACG |
| Alpha-2 agonists | Brimonidine 0.2% | Reduces production + increases outflow | Caution in children (CNS depression) |
| Miotics | Pilocarpine 2–4% | Opens drainage angle (pupil constriction) | Used in AACG; causes dim vision, brow ache |
| Rho-kinase inhibitor | Netarsudil | Increases trabecular outflow | Newer agent |
| Combination drops | Cosopt (Timolol + Dorzolamide), Ganfort (Timolol + Bimatoprost) | Dual mechanism | Improves compliance |
9. Lubricants / Artificial Tears
For dry eye disease and ocular surface protection.
| Form | Example | Best For |
|---|---|---|
| Drops (aqueous) | Hypromellose 0.3%, Sodium hyaluronate 0.1–0.4% | Mild–moderate dry eye; frequent use |
| Carbomer gel | Viscotears | Moderate dry eye; longer contact time; slightly blurs vision |
| Ointment | Lacri-Lube, Simple Eye Ointment | Severe dry eye; at night only (blurs vision significantly) |
10. Other Commonly Seen Drops
| Drug | Use |
|---|---|
| Acetylcysteine 5% | Mucus dissolving — filamentary keratitis, dry eye with mucus strands |
| Cyclosporine 0.05–0.1% (Restasis, Ikervis) | Immunomodulatory dry eye (reduces T-cell inflammation on ocular surface) |
| Bevacizumab / Ranibizumab / Aflibercept | Intravitreal injections (not drops) for wet AMD, DMO, CRVO — anti-VEGF |
| Pilocarpine | Miotics for acute angle closure; also reverses tropicamide dilation |
Quick Reference Summary Card
DILATION (fundus exam): Tropicamide 1% ± Phenylephrine 2.5%
CYCLOPLEGIA (refraction): Cyclopentolate 1% (children), Atropine 1%
ANAESTHESIA (before IOP): Proxymetacaine 0.5% or Tetracaine 0.5%
STAINING (ulcer/abrasion): Fluorescein strip + cobalt blue light
BACTERIAL CONJUNCTIVITIS: Chloramphenicol drops/ointment
HSV KERATITIS: Aciclovir 3% ointment — NEVER steroids
UVEITIS: Steroid drops + Cycloplegic (homatropine/atropine)
GLAUCOMA (1st line): Prostaglandin analogue (latanoprost, night)
ACUTE ANGLE CLOSURE: IV Acetazolamide + Pilocarpine drops + Timolol
DRY EYE: Hypromellose / Sodium hyaluronate drops; ointment at night
Sources: Roberts & Hedges' Clinical Procedures in Emergency Medicine | Kanski's Clinical Ophthalmology 10th ed. | Wills Eye Manual
Definition of blindness
Finding Sources
Finding Sources
Reading File
Finding Sources
Here is a complete breakdown, sourced from Harrison's and Kanski's:
Definition of Blindness
Blindness is not a single absolute state — it is defined differently depending on the context (legal, clinical, WHO classification) and whether you are referring to one eye or both.
1. WHO / International Classification (ICD-11)
The World Health Organization classifies visual impairment based on best-corrected visual acuity (BCVA) in the better eye:
| Category | BCVA in Better Eye | Common Term |
|---|---|---|
| Normal vision | 6/6 to 6/12 | Normal |
| Mild visual impairment | < 6/12 to ≥ 6/18 | Mild VI |
| Moderate visual impairment | < 6/18 to ≥ 6/60 | Moderate VI |
| Severe visual impairment | < 6/60 to ≥ 3/60 | Severe VI |
| Blindness | < 3/60 (or VF < 10°) | Blind |
| Total (absolute) blindness | No light perception (NPL) | Totally Blind |
The key cut-off: < 3/60 BCVA in the better eye = WHO blind
2. Legal Blindness
Defined (in most countries) as:
Best-corrected VA of 6/60 (20/200) or worse in the better eye OR a visual field of 20° or less (even if central VA is preserved)
— Harrison's Principles of Internal Medicine, 22nd ed.
Key points:
- It is based on the better eye — if one eye is normal, a person is not legally blind
- Visual field counts — someone with 6/6 vision but severe tunnel vision (e.g. end-stage glaucoma, retinitis pigmentosa) can still qualify as legally blind if their field is ≤ 20°
- Loss of vision in one eye only does not constitute legal blindness
3. Practical Levels of Vision — What Each Means
| Level | Meaning |
|---|---|
| 6/6 | Normal vision |
| 6/12 | Minimum for unrestricted driving in most countries |
| 6/18 | Minimum for driving with conditions in some countries |
| 6/60 | Legal blindness threshold (can only count fingers at ~1 m) |
| 3/60 | WHO blindness threshold |
| Counting fingers (CF) | Can count fingers but cannot read any Snellen line |
| Hand movements (HM) | Cannot count fingers; can only detect hand moving |
| Perception of light (PL) | Aware of light only; no shapes |
| No perception of light (NPL) | Absolute/total blindness — cannot detect any light |
4. Low Vision vs Blindness
| Term | Definition |
|---|---|
| Low vision | BCVA < 6/18 but ≥ 3/60 in the better eye, OR VF < 20° — not correctable by glasses/surgery |
| Blindness | BCVA < 3/60 in the better eye, or NPL |
Low vision means the person still has some usable vision and can benefit from visual rehabilitation (magnifiers, large print, etc.).
5. Quick Summary Table
| Threshold | Meaning |
|---|---|
| < 6/12 | Below normal — investigate |
| < 6/18 | Low vision begins |
| < 6/60 | Legal blindness |
| < 3/60 | WHO blindness |
| NPL | Absolute blindness |
6. Common Causes of Blindness Globally (WHO)
- Uncorrected refractive error — most common cause of visual impairment worldwide (preventable)
- Cataract — most common cause of treatable blindness globally
- Glaucoma — most common cause of irreversible blindness
- Age-related macular degeneration (AMD)
- Diabetic retinopathy
- Trachoma — most common infectious cause of blindness globally
- Onchocerciasis (river blindness) — in endemic areas
In your exam/OSCE: If asked "define blindness" — the expected answer is the WHO definition: BCVA < 3/60 in the better eye, OR visual field < 10°. Also know that legal blindness = < 6/60.
— Harrison's Principles of Internal Medicine, 22nd ed. | Kanski's Clinical Ophthalmology, 10th ed.
Near vision 101 assessment and other infos please
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Here's everything you need to know about near vision assessment, from physiology to the bedside test.
Near Vision — Complete Guide
1. The Physiology — Why We Need Near Vision Testing
Accommodation
To see near objects clearly, the eye must increase its refractive power by making the lens more convex. This is called accommodation.
- Mechanism: Parasympathetic signal (CN III) → ciliary muscle contracts → zonules relax → lens becomes rounder/thicker → focal point moves closer
- Accommodation is measured in diopters (D) — the reciprocal of the near point distance in metres
| Age | Accommodation Amplitude | Clinical implication |
|---|---|---|
| Child | ~14 D | Can focus from very close |
| Age 20 | ~10 D | Good range |
| Age 40–45 | ~2–4 D | Near work becoming difficult |
| Age 50+ | < 2 D | Reading glasses needed |
| Age 70 | ~0 D | Essentially no accommodation |
Presbyopia — The Key Condition
Presbyopia = age-related loss of accommodation due to progressive hardening and enlargement of the lens (denaturation of lens proteins → lens loses elasticity)
- Onset typically age 40–45
- Presents as difficulty reading or needing to hold things further away ("arms not long enough")
- Not a disease — a normal ageing process
- Corrected with reading glasses (plus lenses) — or bifocals if the patient also has a distance refractive error
By age 70, the power of accommodation falls to essentially 0 diopters — the lens remains at a fixed focal length permanently. — Guyton & Hall, Medical Physiology
2. Near Vision Charts — The Notation Systems
Near vision is tested at 33–40 cm (standard reading distance), using one of several notation systems:
a) Jaeger (J) Notation
- The original near vision system — still widely used in clinical practice
- Consists of paragraphs of text in decreasing print sizes, numbered J1 to J14+
- J1 = smallest (finest) print = equivalent to good near vision
- J14+ = largest print = very poor near vision
| Jaeger | Approximate Snellen Equivalent | What it means |
|---|---|---|
| J1 | ~6/6 near equivalent | Normal reading vision |
| J2 | ~6/9 | Mildly reduced |
| J6 | ~6/18 | Moderately reduced |
| J14+ | ~6/60 | Very poor near vision |
b) N (Newspaper) Notation
- Print size measured in point size — labelled N5, N6, N8, N10, N12, N18, N36, N48
- N5 = smallest (newsprint-sized text) = normal near vision
- N8 = average newspaper body text
- This system is intuitive — "N5" means the patient can read 5-point print
| N-notation | Approximate size | Meaning |
|---|---|---|
| N5 | Very small (fine newsprint) | Normal near vision |
| N8 | Standard newspaper text | Good near vision |
| N12–N18 | Large print text | Reduced |
| N36+ | Very large print | Significantly reduced |
c) Rosenbaum Pocket Card (Bedside)
- A pocket-sized card held at 14 inches (35 cm) — equivalent to the Snellen chart at distance
- Results expressed as distance Snellen equivalents (e.g. 20/20, 20/40)
- Extremely useful at the bedside, in ED, and for quick assessments
- Patient must wear their reading glasses if they use them
3. How to Test Near Vision — Step by Step
Setup
- Good lighting — natural light or a bright lamp
- Patient holds the near vision chart at their comfortable reading distance (usually 33–40 cm) — measure and record this distance
- Test each eye separately — cover the other eye
- Patient wears their reading glasses if they use them (especially for presbyopia patients — you must test with their correction to get best-corrected near VA)
Procedure
Step 1: Cover left eye
Step 2: Patient holds near chart at comfortable reading distance
Step 3: Ask patient to read smallest line they can see clearly
Step 4: Record: e.g. J2 or N6 at 33 cm, right eye
Step 5: Repeat for left eye
Step 6: Then test binocularly (both eyes open)
What to Record
Example: R near VA: N6 @ 33 cm (with reading glasses)
Always note:
- Which eye (R/L/binocular)
- The notation result (J or N)
- The distance it was held at
- Whether reading glasses were worn
4. Near Vision vs Distance Vision — Clinical Correlation
| Pattern | Likely Cause |
|---|---|
| Near VA reduced, distance VA normal | Presbyopia (age-related), over-corrected myopia |
| Distance VA reduced, near VA normal | Uncorrected myopia |
| Both near and distance VA reduced | Macular disease (AMD, diabetic maculopathy), corneal/lens/optic nerve pathology |
| Near VA worse than expected even with glasses | Macular disease, optic nerve disease — near VA is a sensitive indicator of macula function |
| Near VA much better than distance VA | Uncorrected myopia — patient reads well up close |
"Near vision testing can be a sensitive indicator of the presence of macular disease." — Kanski's Clinical Ophthalmology, 10th ed.
5. Special Situations
Traumatic Mydriasis
- Trauma can paralyse the iris sphincter → fixed dilated pupil → reduced depth of focus → blurred near vision even in a young patient
- Always test near VA in eye trauma cases
After Dilation Drops
- Tropicamide/cyclopentolate paralyse the ciliary muscle → no accommodation → near vision blurred
- Always warn patients before dilating: "You will not be able to read clearly for a few hours"
- Test near VA before dilating if relevant
Malingering / Non-organic Visual Loss
- If a patient claims they cannot see but near VA is intact or inconsistent, consider non-organic loss
- Use optokinetic nystagmus (OKN) test: pass a striped drum/tape in front of the eye — involuntary tracking movements (nystagmus) indicate an intact visual pathway even if the patient claims blindness
6. Amsler Grid — Near Vision + Macular Function Test
The Amsler grid is a near-distance test held at 33 cm, used specifically to detect macular pathology:
- A grid of fine squares with a central dot
- Patient fixates on the central dot and reports any distortion (wavy lines = metamorphopsia) or missing areas (scotoma)
- Standard test for AMD monitoring — patients can use it at home daily
- If lines appear wavy or a patch is missing → wet AMD, macular oedema → refer urgently
7. Summary Card
Standard near vision testing distance: 33–40 cm
Normal near vision: J1 or N5
Notation systems: J (Jaeger), N (newsprint), Snellen equivalent
Always test WITH reading glasses (if patient uses them)
Test BEFORE dilating drops (dilation removes accommodation)
Near VA reduced + distance VA normal: Think PRESBYOPIA
Both near + distance reduced: Think MACULA or OPTIC NERVE
Macular function test: Amsler grid at 33 cm
Sources: Kanski's Clinical Ophthalmology 10th ed. | Roberts & Hedges' Clinical Procedures in Emergency Medicine | Guyton & Hall Medical Physiology | Ganong's Review of Medical Physiology
Opthalmoscopy/fundoscopy
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Loading Image
Loading Image
Here is a complete guide to ophthalmoscopy / fundoscopy, with real images from Kanski's:
Ophthalmoscopy / Fundoscopy — Complete Guide
1. Why It Matters
The fundus is the only place in the body where you can directly visualise blood vessels and neural tissue non-invasively. A single look can reveal:
- Eye diseases: glaucoma, retinal detachment, diabetic retinopathy, AMD, CRAO, CRVO
- Systemic diseases: hypertension, diabetes, raised intracranial pressure, leukaemia, sickle cell, endocarditis
2. Types of Ophthalmoscopy
| Method | Instrument | Image | Field of View | Magnification | When Used |
|---|---|---|---|---|---|
| Direct | Handheld direct ophthalmoscope | Upright, virtual | Small (~5°) | 15x | Bedside, general ward, GP, ED |
| Indirect (slit-lamp) | Slit lamp + 78D/90D lens | Inverted | Wide (~50°) | 3–5x | Clinic gold standard |
| Binocular indirect | Headband ophthalmoscope + 20D/28D lens | Inverted + reversed | Very wide | 3x | Peripheral retina, RD, surgery |
3. Direct Ophthalmoscopy — The Bedside Skill
The Instrument
- A handheld device with a light source and a rotating lens wheel
- Lens wheel corrects for refractive error of both examiner and patient
- Apertures: large (dilated pupil), small (undilated), red-free (green filter for vessels), cobalt blue (with fluorescein)
Before You Start
- Darken the room — essential for an undilated pupil
- Dilate if possible (tropicamide 1%) — gives a far better view
- Ask patient to fixate on a distant target on the wall (reduces accommodation and pupil constriction)
- Remove your own glasses if you have mild refractive error (correct with the lens wheel instead)
- Check the battery and light intensity
Technique — Step by Step

Fig. 1.31 — Technique of direct ophthalmoscopy. Note the examiner is close, approaching from the temporal side, with the free hand resting on the patient's forehead. — Kanski's Clinical Ophthalmology
1. Start with lens wheel at "0"
2. Right eye of patient → use YOUR right eye, hold scope in right hand, stand on patient's right
3. Left eye of patient → use YOUR left eye, hold scope in left hand, stand on patient's left
(Same-side rule: avoids nose-to-nose contact)
4. Rest your free hand on patient's FOREHEAD — stabilises your position
5. From arm's length, shine light at pupil → look for the RED REFLEX first
(dull/absent reflex = cataract, vitreous haemorrhage, retinoblastoma)
6. Approach slowly from the TEMPORAL SIDE at a slight angle (~15°)
7. Come in close — ideally 3–4 cm from the eye
(Most students stay too far away — this is the most common mistake)
8. When close, the OPTIC DISC should come into view
If blurry → rotate lens wheel until disc is sharp
9. Correct for refractive error:
- Hypermetrope (far-sighted patient/examiner) → plus lenses (GREEN numbers)
- Myope (short-sighted) → minus lenses (RED numbers)
4. What You See — The Normal Fundus
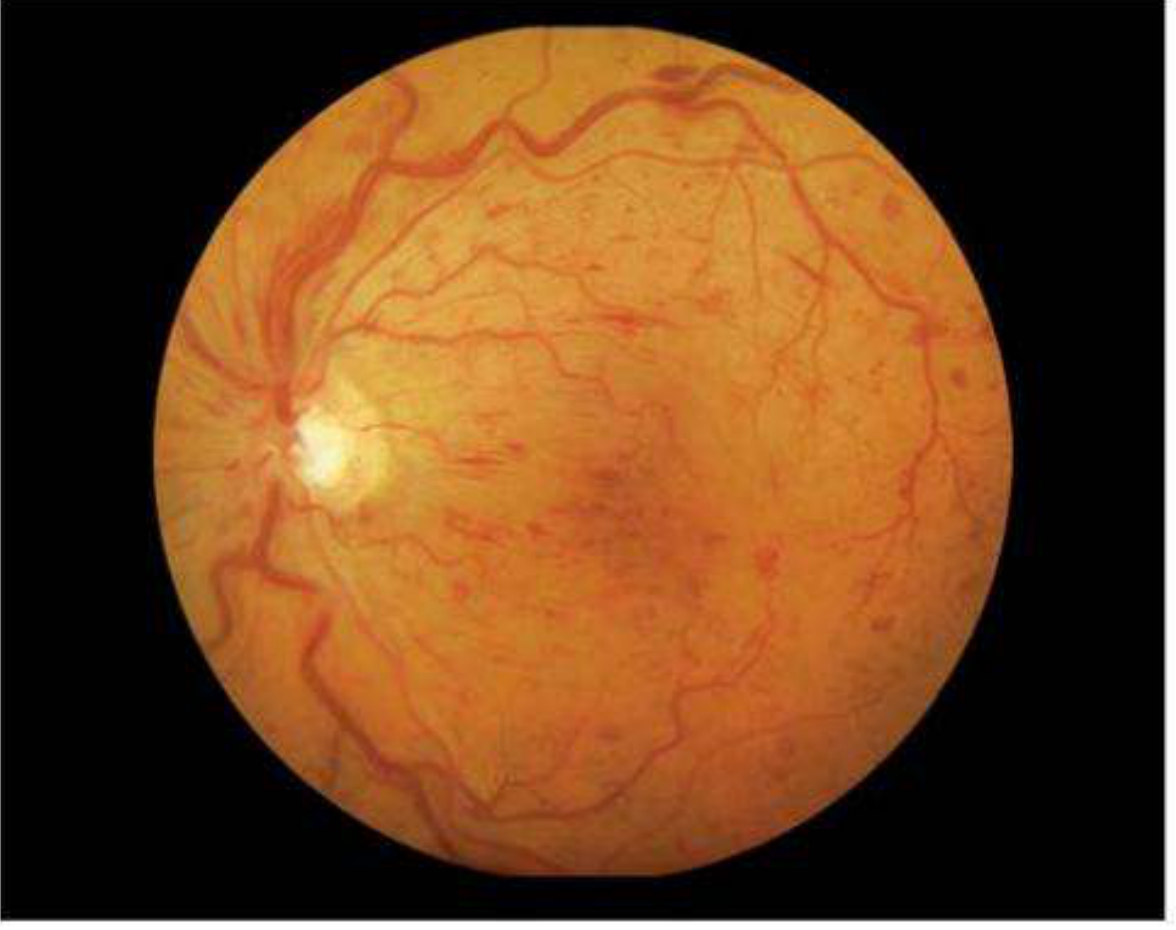
Fig. 1.29 — Magnified image from direct ophthalmoscope showing normal fundus: disc visible upper-left, blood vessels radiating outward, uniform orange-red background. — Kanski's Clinical Ophthalmology
Systematic Examination — Always in This Order
Step 1: Optic Disc
Find the disc first — it's your landmark. Follow a vessel inward (vessels get larger as you approach the disc).
| Feature | Normal | Abnormal |
|---|---|---|
| Colour | Creamy-pink / orange | Pale = optic atrophy; Hyperaemic = papilloedema / neuritis |
| Margins | Sharp, well-defined | Blurred = papilloedema, neuritis; Drusen can mimic blurring |
| Elevation | Flat | Raised = papilloedema; Cupped = glaucoma |
| Spontaneous venous pulsation | Present in ~80% | Absent can suggest raised ICP |
Step 2: Cup:Disc Ratio (CDR)
___________
| | = Disc (whole disc diameter)
| _____ |
| |cup | | = Cup (central pale area — no neural tissue)
| |_____| |
|___________|
CDR = Diameter of cup ÷ Diameter of disc
| CDR | Interpretation |
|---|---|
| 0.3–0.4 | Normal (most people) |
| ≤ 0.5 | Upper limit of normal |
| > 0.6 | Suspicious for glaucoma |
| Asymmetry > 0.2 between eyes | Suspicious for glaucoma |
ISNT Rule — normal neuroretinal rim thickness follows:
Inferior > Superior > Nasal > Temporal Any violation of this rule = suspicious for glaucomatous damage
Step 3: Blood Vessels
- Follow vessels out from the disc in all 4 quadrants (superior, inferior, nasal, temporal)
- Arteries = narrower, brighter red, have a light reflex
- Veins = wider, darker red, no light reflex
- Normal artery:vein ratio = 2:3
| Finding | Disease |
|---|---|
| Narrow arteries (AV ratio < 1:2) | Hypertension |
| AV nipping/nicking at crossings | Hypertensive retinopathy |
| Silver/copper wiring | Arteriosclerosis |
| Tortuous veins | CRVO, hyperviscosity |
| New vessels (NVD/NVE) | Proliferative diabetic retinopathy |
| Emboli at bifurcations | Hollenhorst plaques (carotid emboli) |
Step 4: Macula
To find the macula:
Focus on the disc, then move the light 2 disc diameters temporally — or ask the patient to look directly at the light
- Appears slightly darker than surrounding retina
- Foveal reflex = bright central pinpoint light reflection (present in young people; reduced with macular disease)
- The macula has no large vessels — only capillaries
| Finding | Disease |
|---|---|
| Drusen (yellow dots) | AMD — dry |
| Subretinal fluid / haemorrhage | AMD — wet |
| Hard exudates in rings (circinate) | Diabetic maculopathy |
| Cherry-red spot | CRAO |
| Pigment mottling / bull's-eye | Hydroxychloroquine toxicity |
| Macular hole | Central scotoma, elderly |
Step 5: Peripheral Retina
Ask patient to look up, down, left, right — this swings the peripheral retina into view.
- Look for: retinal tears, detachment, pigment changes, laser scars, lattice degeneration
- Retinal detachment appears as elevated, grey, corrugated retina that billows with eye movement
5. Red Reflex — Never Skip This
Before getting close, always check the red reflex at arm's length:
| Red Reflex | Interpretation |
|---|---|
| Bright, equal bilaterally | Normal |
| Dull or dark area (opacity) | Cataract, vitreous haemorrhage |
| Absent | Dense cataract, vitreous blood, complete retinal detachment |
| White reflex (leukocoria) | Retinoblastoma (in children — emergency referral) |
| Asymmetric between eyes | Amblyopia screening, anisometropia |
6. Direct vs Indirect — Key Differences
| Feature | Direct Ophthalmoscopy | Indirect (Slit-lamp 78/90D) |
|---|---|---|
| Magnification | 15x | 3–5x |
| Field of view | Small (~5°) | Large (~50°) |
| Stereopsis (3D) | No | Yes |
| Image orientation | Upright, virtual | Inverted |
| Portability | Yes — bedside | No — needs slit-lamp |
| Peripheral retina | Poor | Excellent |
| Best for | Disc, macula, bedside | Complete fundus, subtle macular changes |
Retinal detachment CANNOT be ruled out by direct ophthalmoscopy alone — indirect ophthalmoscopy is needed to view the peripheral retina where most breaks occur. — Rosen's Emergency Medicine
7. Common Mistakes to Avoid
| Mistake | Correction |
|---|---|
| Staying too far from the eye | Get within 3–4 cm — must be close |
| Using wrong eye/hand | Same-side rule: right eye = your right eye |
| Not darkening the room | Dim lights = larger pupil = better view |
| Not asking patient to fixate on a distant target | Prevents miosis and accommodation |
| Giving up when disc not found immediately | Follow a vessel inward — vessels get larger toward the disc |
| Forgetting the macula | Always look 2 disc diameters temporal after the disc |
| Bright corneal reflection | Slightly de-centre the beam or use the small aperture |
8. Quick Revision Card
Instrument used: Direct ophthalmoscope
Magnification: 15x
Starting lens: 0 (adjust for patient's refraction)
Approach: Temporal side, ~15° angle, ~3–4 cm final distance
Same-side rule: Right eye → your right eye; Left → your left eye
Exam order: Red reflex → Disc → CDR → Vessels → Macula → Periphery
Find macula: 2 disc diameters temporal to disc
Normal CDR: ≤ 0.5 (suspicious if > 0.6 or asymmetry > 0.2)
Normal AV ratio: Artery:Vein = 2:3
Sources: Kanski's Clinical Ophthalmology, 10th ed. | Rosen's Emergency Medicine | Roberts & Hedges' Clinical Procedures
Uveitis
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Reading File
Loading Image
Loading Image
Here is a comprehensive guide to uveitis, fully sourced from Kanski's:
Uveitis — Complete Guide
1. What Is Uveitis?
Uveitis = inflammation of the uveal tract (iris + ciliary body + choroid). The term is used broadly to include any intraocular inflammatory disease, even when the primary site is the retina or vitreous.
2. Anatomical Classification (SUN / IUSG)
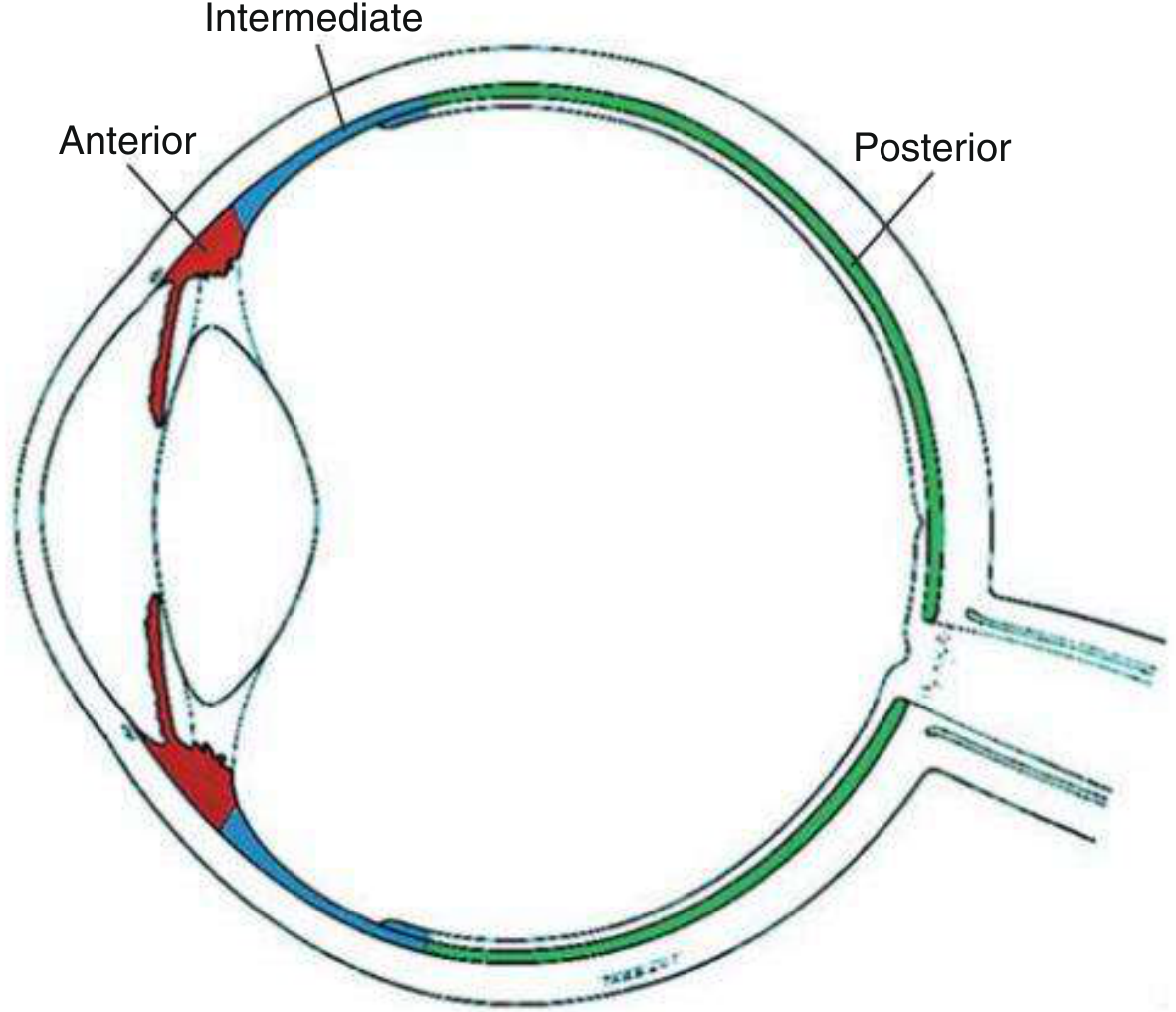
Fig. 12.1 — Anatomical zones of uveitis: Anterior (red = iris/ciliary body), Intermediate (blue = vitreous/pars plana), Posterior (green = retina/choroid). — Kanski's Clinical Ophthalmology
| Type | Primary Site | Key Structure |
|---|---|---|
| Anterior uveitis | Anterior chamber | Iris + anterior ciliary body (iritis / iridocyclitis) |
| Intermediate uveitis | Vitreous | Pars plana, vitreous base (pars planitis) |
| Posterior uveitis | Posterior segment | Retina (retinitis) and/or choroid (choroiditis) |
| Panuveitis | All segments | All uveal structures |
Anterior uveitis is the most common form and the one you will see most in OPD.
3. Aetiological Classification
| Category | Examples |
|---|---|
| Infectious | Herpes simplex/zoster, TB, syphilis, toxoplasmosis, CMV, fungi |
| Non-infectious — systemic association | HLA-B27 spondyloarthropathies, sarcoidosis, JIA, Behçet, IBD |
| Non-infectious — idiopathic | Most common — no identifiable cause |
| Masquerade syndromes | Lymphoma, retinoblastoma, leukaemia (mimic uveitis) |
4. Course Classification
| Term | Definition |
|---|---|
| Acute | Sudden onset, limited duration (≤3 months) |
| Recurrent | Repeated episodes with inactive intervals between |
| Chronic | Persistent >3 months; relapses within 3 months of stopping treatment |
| Remission | No cells (inactive) for ≥3 months off treatment |
5. Anterior Uveitis — The Must-Know Type
Symptoms
- Pain (deep, aching) — due to ciliary spasm
- Photophobia — often severe
- Lacrimation (watering)
- Blurred vision — from cells/flare in AC + corneal oedema
- Ciliary flush — limbal injection (circumcorneal violet-red ring)
Onset is typically sudden in HLA-B27-related disease and insidious in JIA and Fuchs uveitis syndrome.
Slit-Lamp Signs — What to Look For
A. Keratic Precipitates (KPs)
Inflammatory cells deposited on the corneal endothelium. Their character tells you the type of uveitis:
| KP Type | Appearance | Granulomatous? | Associated with |
|---|---|---|---|
| Fine/stellate | Small, scattered | Non-granulomatous | HLA-B27, herpetic, idiopathic |
| Mutton-fat | Large, greasy, irregular | Granulomatous | TB, sarcoidosis, syphilis, VKH |
| Stellate (diffuse) | Fine, spread all over endothelium | Special type | Fuchs uveitis syndrome |

Large mutton-fat KPs on the corneal endothelium — granulomatous uveitis (TB, sarcoidosis, syphilis). — Kanski's Clinical Ophthalmology
B. Anterior Chamber Cells — SUN Grading
Cells are graded using a 1 mm × 1 mm slit beam:
| Grade | Cells in field |
|---|---|
| 0 | < 1 (none) |
| 0.5+ | 1–5 |
| 1+ | 6–15 |
| 2+ | 16–25 |
| 3+ | 26–50 |
| 4+ | > 50 |
C. Anterior Chamber Flare — SUN Grading
Flare = protein leaked from inflamed iris vessels into the aqueous (makes the slit-beam look hazy, like headlights in fog):
| Grade | Description |
|---|---|
| 0 | None |
| 1+ | Faint |
| 2+ | Moderate — iris and lens still clear |
| 3+ | Marked — iris and lens hazy |
| 4+ | Intense — fibrin or "plastic aqueous" |
D. Posterior Synechiae (PS)
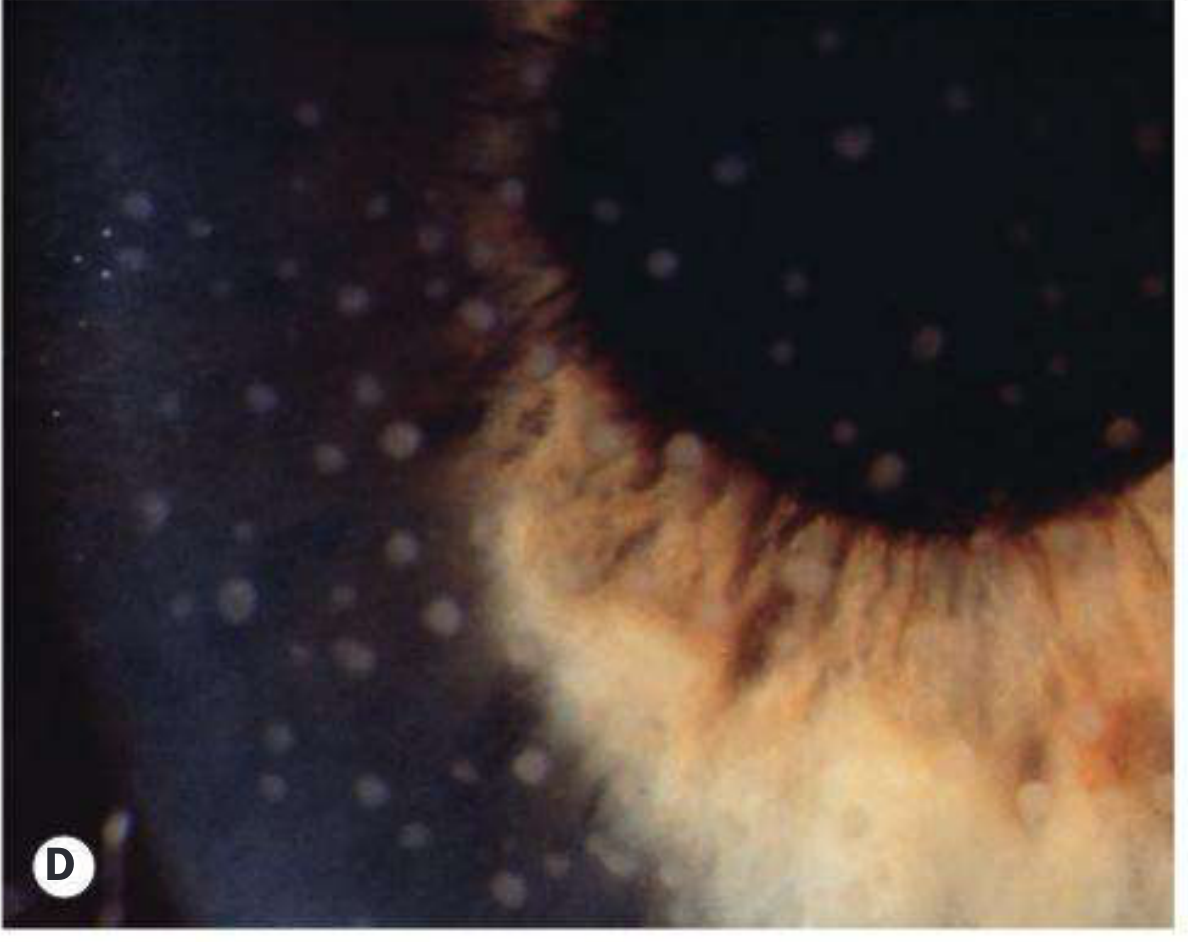
Posterior synechiae — iris adherent to the anterior lens capsule (visible as irregular pupil), with fine white KPs on the endothelium. — Kanski's Clinical Ophthalmology
- Iris adhesed to anterior lens capsule due to inflammation
- Cause: irregular pupil shape
- If 360° = seclusio pupillae → aqueous cannot flow → iris bombé → angle-closure glaucoma
- Prevention: cycloplegics (dilate pupil, prevent adhesion)
- Breaking fresh PS: phenylephrine + cycloplegic; subconjunctival Mydricaine if drops fail
E. IOP Changes in Uveitis
| Direction | Mechanism |
|---|---|
| Low IOP | Ciliary body inflammation → reduced aqueous production |
| High IOP | Trabeculitis, PS → blocked drainage, steroid response |
6. Systemic Associations — Must Know
HLA-B27 Associated (Most Common Non-Infectious Cause)
The HLA-B27 gene is associated with a group of seronegative spondyloarthropathies, all of which can cause uveitis:
| Condition | Mnemonic |
|---|---|
| Ankylosing spondylitis | A |
| Reactive arthritis (Reiter's syndrome) | R |
| Psoriatic arthritis | P |
| Inflammatory bowel disease (Crohn's, UC) | I |
Mnemonic: ARPI or remember "HLA-B27 = Back, Bowel, Behave (behave badly — recurs)"
HLA-B27 uveitis features:
- Unilateral, alternating
- Acute onset, recurrent episodes
- Non-granulomatous (fine KPs)
- Responds well to topical steroids
- Ask about: lower back pain/stiffness (worse in morning, better with activity), skin rash, bowel symptoms, urethritis
Other HLA Associations
| HLA | Disease |
|---|---|
| HLA-B27 | Recurrent acute anterior uveitis (AS, Reiter's, IBD, psoriatic arthritis) |
| HLA-A29 | Birdshot retinochoroidopathy |
| HLA-B51 | Behçet syndrome |
| HLA-DR4 | Sympathetic ophthalmia, Vogt-Koyanagi-Harada (VKH) |
Other Key Systemic Associations
| Condition | Features of uveitis |
|---|---|
| Sarcoidosis | Granulomatous (mutton-fat KPs), bilateral, chronic; iris nodules (Koeppe/Busacca); serum ACE elevated |
| Tuberculosis | Granulomatous; can cause chronic panuveitis; QuantiFERON-TB positive |
| Syphilis | "The great mimicker" — any type; bilateral; VDRL/RPR + TPHA |
| Juvenile Idiopathic Arthritis (JIA) | Chronic anterior uveitis, bilateral, asymptomatic (no red eye) — most insidious; ANA positive |
| Behçet disease | Bilateral, severe; oral and genital ulcers; hypopyon; HLA-B51 |
| Toxoplasmosis | Posterior uveitis; focal necrotising retinochoroiditis; "headlights in fog" appearance |
| Herpes simplex/zoster | Anterior uveitis + keratitis; unilateral; iris atrophy; high IOP |
7. Investigations for Uveitis
First-Line (All Cases)
- FBC — leucocytosis (infection), eosinophilia (parasites)
- ESR / CRP — non-specific inflammation marker
- HLA-B27 — seronegative spondyloarthropathy
- Serum ACE + lysozyme — sarcoidosis (ACE elevated in ~80% acute sarcoid)
- VDRL/RPR + TPHA — syphilis serology (both tests needed)
- QuantiFERON-TB Gold / Mantoux — tuberculosis
- ANA — JIA (especially in children with CAU)
- CXR — sarcoidosis, TB
Additional (Selected Cases)
- ANCA — if associated scleritis (GPA/Wegener's)
- HIV serology — opportunistic infections
- Toxoplasma IgG — posterior uveitis
- Lyme serology — if endemic area
8. Complications of Uveitis
| Complication | Mechanism |
|---|---|
| Posterior synechiae | Iris-lens adhesion → irregular pupil |
| Iris bombé | 360° PS → aqueous trapped → iris bulges forward |
| Secondary glaucoma | Trabeculitis, angle closure from iris bombé, steroid response |
| Cataract | Inflammation + prolonged steroid use → posterior subcapsular |
| Cystoid macular oedema (CMO) | Most common cause of visual loss in uveitis |
| Hypotony | Chronic ciliary body damage → low IOP → phthisis bulbi |
| Band keratopathy | Calcium deposition in Bowman's layer (JIA especially) |
9. Treatment
Acute Anterior Uveitis (AAU) — Standard Regimen
Step 1: Topical steroids (prednisolone acetate 1% or dexamethasone 0.1%)
Typical tapering regimen:
Week 1: hourly (or every 2 hours)
Week 2: 4x daily
Week 3: 3x daily
Week 4: 2x daily
Week 5: 1x daily → stop
(Total ~5–6 weeks; adjust based on response)
Step 2: Cycloplegic (to prevent/break posterior synechiae + relieve ciliary spasm)
- Cyclopentolate 1% — mild/moderate cases (lasts 12–24 hrs)
- Homatropine 5% — moderate disease (lasts 3 days)
- Atropine 1% — severe disease (lasts 7–10 days)
Step 3: Break fresh posterior synechiae (if present)
- Phenylephrine 2.5–10% + cycloplegic drops
- If drops fail → subconjunctival Mydricaine (atropine + adrenaline + procaine injection)
- If dense fibrin → intracameral TPA (tissue plasminogen activator) 12.5–25 μg
Chronic Anterior Uveitis (CAU)
- Target: complete suppression — zero cells AND zero flare
- Even low-grade activity causes complications
- May need long-term maintenance drops
- Steroid-sparing agents (methotrexate, mycophenolate) for refractory cases
Complications of Topical Steroids to Monitor
- IOP rise (steroid responders) — check IOP at every visit
- Cataract — posterior subcapsular
- Secondary infection (bacterial, fungal, HSV reactivation)
- Corneal melting — rare
10. Quick Summary
Most common type: Anterior uveitis (iritis/iridocyclitis)
Classic triad: Pain + Photophobia + Ciliary flush
Key slit-lamp signs: KPs, AC cells/flare, posterior synechiae
KP type matters: Fine = non-granulomatous; Mutton-fat = granulomatous
Most common RF: HLA-B27 (ankylosing spondylitis, IBD, psoriatic, Reiter's)
Granulomatous causes: TB, Sarcoid, Syphilis, VKH, Sympathetic ophthalmia
Most common complication causing blindness: Cystoid macular oedema
Treatment pillars: Topical steroid (taper) + Cycloplegic
Never steroid without diagnosis — exclude herpetic keratitis first
Source: Kanski's Clinical Ophthalmology, 10th ed. (Chapter 12 — Uveitis)
Refractive error lecture
Finding Sources
Finding Sources
Finding Sources
Finding Sources
This is a shared conversation. Sign in to Orris to start your own chat.