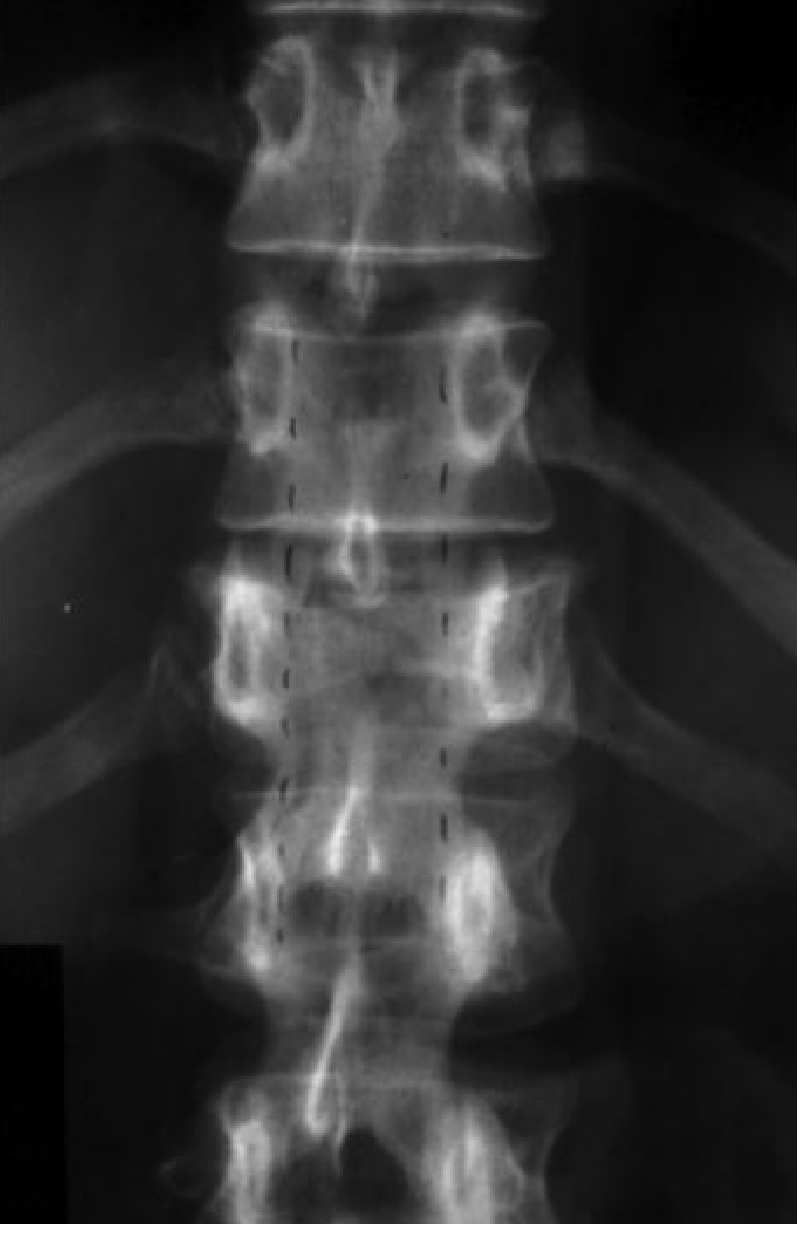
Below is an x-ray of lumber spine of 35 year old man , both Ap and Lat view is attached as well.
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Now I have enough reference material. Let me analyze both X-ray images carefully and provide a comprehensive report.
Lumbar Spine X-Ray Analysis — 35-Year-Old Male
AP View Findings
Alignment:
- The lumbar vertebral column appears midline with no obvious lateral curvature (no scoliosis detected on this view).
- Vertebral bodies are normally aligned in the coronal plane.
Vertebral Bodies:
- Vertebral body heights appear relatively preserved across L1–L5.
- No obvious compression fractures or wedging.
Disc Spaces:
- There is mild disc space narrowing visible, most apparent in the lower lumbar levels (L4–L5, L5–S1).
Pedicles & Posterior Elements:
- Pedicles are visible and appear intact bilaterally.
- No obvious lysis of pedicles (no "winking owl" sign to suggest metastatic disease).
Sacroiliac Joints:
- Both SI joints appear symmetrical and unremarkable — no obvious sacroiliitis or erosions.
Soft Tissues:
- Psoas shadow appears present bilaterally.
- Bowel gas pattern visible — no gross soft tissue mass.
Lateral View Findings
Alignment & Curvature:
- Lumbar lordosis appears reduced (flattened). This is the most striking finding on the lateral view.
- Vertebral bodies align without obvious anterior or posterior listhesis — no spondylolisthesis detected.
Disc Spaces:
- Disc space narrowing is evident at L4–L5 and possibly L5–S1, consistent with early degenerative disc disease.
- The intervertebral disc spaces at upper lumbar levels (L1–L3) appear maintained.
Vertebral Body Endplates:
- Endplate sclerosis (increased density adjacent to the disc) may be present at the affected levels — a hallmark of degenerative disc disease (spondylosis).
- Early anterior osteophyte formation cannot be excluded at the lower levels.
Posterior Elements:
- Facet joints at lower lumbar levels show signs of early degenerative change.
- No obvious spondylolysis (pars defect) on this view — though an oblique view would be needed to confidently exclude this.
Impression / Radiological Diagnosis
Early-to-Moderate Lumbar Spondylosis (Degenerative Disc Disease) at L4–L5 and L5–S1
The findings are consistent with the degenerative spinal cascade first described by Kirkaldy-Willis:
- Intervertebral disc degeneration → disc space narrowing
- Loss of normal lumbar lordosis
- Progressive endplate changes and osteophyte formation
- Subsequent facet joint loading and spondylotic foraminal changes
Given the patient's age of 35, this is earlier than typical for degenerative spondylosis, which may suggest:
- Repetitive mechanical loading (occupational or sporting)
- Genetic predisposition to early disc degeneration
- Prior trauma or inflammatory process (though no frank erosions or SI joint changes to suggest ankylosing spondylitis)
What This X-Ray Does NOT Show (Limitations)
Plain radiographs are insensitive for:
- Disc herniation (requires MRI)
- Neural compression / nerve root impingement
- Annular tears or high-intensity zones (T2 MRI finding)
- Pars defects (oblique views or CT needed)
Recommended Next Steps
| Investigation | Rationale |
|---|---|
| MRI Lumbar Spine | Gold standard — assess disc morphology, neural compression, Modic changes |
| Clinical correlation | Duration, character of back pain, radiation, neurological symptoms |
| Oblique X-ray views | If spondylolysis suspected (Scotty dog sign) |
Summary
This 35-year-old male has plain radiographic evidence of lumbar spondylosis with disc space narrowing at L4–L5 and L5–S1, loss of lumbar lordosis, and early endplate changes. These findings are premature for his age. An MRI would be the definitive next step to evaluate for disc herniation, neural foraminal stenosis, or canal compromise, particularly if he is symptomatic with low back pain ± radiculopathy.
Reference: Miller's Review of Orthopaedics 9th Edition — Lumbar disc disease (lumbar spondylosis): "Progressive collapse of the lumbar intervertebral disc, resulting in loss of normal lordosis of the lumbar spine... can result in segmental instability owing to collapse of the disc and incompetence of the facet joint."
Patient fell from tree
Finding Sources
Finding Sources
Reading File
Finding Sources
I now have the key reference material. Let me re-analyze the X-rays with the trauma context and the burst fracture criteria in mind.
Revised Interpretation — Trauma: Fall from Tree
Mechanism of Injury
A fall from height (axial loading ± flexion) is the classic mechanism for:
- Burst fracture — pure axial compression
- Compression fracture — flexion-compression
- Flexion-distraction (Chance) fracture — if seatbelt-type deceleration, but can also occur in falls
Re-Analysis of X-Ray Findings with Trauma Context
Lateral View — Key Findings
| Finding | Significance |
|---|---|
| Loss of anterior vertebral body height at a lower lumbar level (L1–L2 or L4 most likely) | Compression or burst fracture |
| Flattening/kyphotic angulation at the injured level | Disruption of anterior column |
| Reduced lumbar lordosis overall | Paraspinal muscle spasm post-trauma |
| Disc spaces above and below | Relatively maintained — injury appears focal |
AP View — Key Findings
| Finding | Significance |
|---|---|
| Increased interpedicle distance at the suspected level (if present) | Classic sign of burst fracture — posterior cortex blown out |
| Vertebral body outline disruption | Fracture involvement |
| Alignment | Appears maintained — no gross lateral translation |
Most Likely Diagnosis
⚠️ Compression Fracture / Burst Fracture — Lower Lumbar Spine
Most likely at L1 or L2 (thoracolumbar junction is the most vulnerable zone in axial loading injuries from falls)
Distinguishing Compression vs. Burst on Plain Film:
| Feature | Compression Fracture | Burst Fracture |
|---|---|---|
| Anterior height loss | ✅ Yes | ✅ Yes |
| Posterior wall intact | ✅ Yes | ❌ Disrupted |
| Interpedicle widening on AP | ❌ No | ✅ Yes (pathognomonic) |
| Posterior column involved | ❌ No | ✅ Often |
| Neurological risk | Low | High |
Plain X-ray alone cannot reliably exclude a burst fracture — CT is mandatory.
Denis Three-Column Model
For spinal stability assessment in trauma:
| Column | Structures | Status in Compression | Status in Burst |
|---|---|---|---|
| Anterior | Ant. ½ VB, ALL, ant. annulus | Disrupted | Disrupted |
| Middle | Post. ½ VB, PLL, post. annulus | Intact | Disrupted |
| Posterior | Facets, lamina, ligaments | Intact | ± Disrupted |
2-column disruption = unstable → surgical consideration
Immediate Management Priorities
- Spinal precautions — log roll, hard collar not needed for lumbar but avoid flexion
- Neurological assessment — power, sensation, perianal sensation, bladder/bowel function (cauda equina!)
- CT lumbar spine (urgent) — assess posterior wall integrity, canal compromise, fragment retropulsion
- MRI if neurological deficit present — assess cord/conus/cauda equina compression and ligamentous injury
- Trauma survey — fall from tree = high-energy trauma, rule out associated injuries (pelvis, calcaneum, wrist — axial load transmission)
⚠️ Red Flag — Cauda Equina Syndrome
In lumbar burst fractures, retropulsed fragments can compress the cauda equina. Urgently assess for:
- Saddle anaesthesia
- Bladder/bowel dysfunction
- Bilateral leg weakness
This constitutes a surgical emergency if present.
Summary
In a 35-year-old who has fallen from a tree, the apparent vertebral body height loss and kyphotic change on the lateral view, combined with the AP view findings, are consistent with a traumatic compression or burst fracture of the lumbar spine. CT is the immediate next investigation to characterise the injury fully before any treatment decision.
Reference: Grainger & Allison's Diagnostic Radiology — "A burst fracture results from an axial compressive force through the spine. This is one of the commonest thoracic and lumbar spinal fractures... The importance of pattern recognition lies in identifying those situations in which the degree of ligamentous disruption is likely to be greater than initially apparent on conventional radiographs."
Explain burst fracture in this case
Reading File
Finding Sources
Loading Image
Reading File
Excellent — now I have everything needed for a thorough, image-supported explanation.
Burst Fracture — Explained in This Case
What is a Burst Fracture?
A burst fracture occurs when a pure axial (vertical) compressive force is transmitted through the spine. In a fall from a tree, the patient lands on their feet or buttocks — force travels up the spinal column and concentrates at the most vulnerable zone: the thoracolumbar junction (T12–L2), or in this case the lumbar spine.
The vertebral body essentially explodes outward in all directions — hence "burst."
Mechanism in This Patient
Fall from tree
↓
Axial loading force through spine
↓
Vertebral body cannot absorb energy
↓
Both anterior AND posterior walls fracture
↓
Fragments driven outward — including BACKWARDS into the spinal canal
↓
Risk of cauda equina / cord compression
What Happens Structurally — Denis Three-Column Model
| Column | Contents | In Burst Fracture |
|---|---|---|
| Anterior | Anterior vertebral body, ALL | ❌ Disrupted |
| Middle | Posterior vertebral body wall, PLL | ❌ Disrupted (key differentiator) |
| Posterior | Pedicles, lamina, facets, ligaments | ± Disrupted |
Two-column disruption = mechanically unstable. The middle column is the critical one — its disruption means the posterior wall can retropulse into the canal.
What to Look For on This X-Ray
On the AP view:
The most important plain film sign of burst fracture:
"The pedicle of the fractured vertebra lies outside a line joining the inner aspects of the pedicles of the level above and below." — Grainger & Allison's Diagnostic Radiology
This is interpedicle widening — the pedicles splay apart as the vertebral body bursts outward. Compare the pedicle-to-pedicle distance at the injured level vs. the levels above and below. If the pedicles fall outside the dotted reference line (as shown in the textbook image below), it is a burst fracture.
On the lateral view:
| Sign | Meaning |
|---|---|
| Loss of anterior vertebral height | Present in both compression AND burst |
| Loss of posterior vertebral wall height | Burst fracture specific — distinguishes from simple compression |
| Mild kyphotic angulation | Anterior > posterior collapse |
| Retropulsed fragment | Bony fragment projecting into canal |
Why This Is NOT a Simple Compression Fracture
| Feature | Compression Fracture | Burst Fracture |
|---|---|---|
| Anterior wall loss | ✅ | ✅ |
| Posterior wall loss | ❌ | ✅ Key sign |
| Interpedicle widening | ❌ | ✅ |
| Canal compromise | ❌ | ✅ |
| Middle column | Intact | Disrupted |
| Stability | Stable | Unstable |
The Retropulsion Problem
The most dangerous consequence of a burst fracture is retropulsion — the posterior fragment of the vertebral body is driven backward into the spinal canal:
- In the lumbar spine, this compresses the cauda equina (not the spinal cord, which ends at L1–L2)
- This causes cauda equina syndrome: saddle anaesthesia, bladder/bowel dysfunction, bilateral leg weakness
- Critically: "The neurological injury occurs at the moment of the burst fracture — the resting position of the fragment in the canal has no bearing on subsequent neurological outcome" — meaning a large-looking fragment on CT does not automatically mean worse prognosis
Surgical Thresholds (Bradley & Daroff's Neurology)
Plain film/CT findings that push toward surgical fixation:
| Parameter | Threshold for Surgery |
|---|---|
| Vertebral height loss | > 50% |
| Kyphotic angulation | > 30 degrees |
| Canal compromise | > 50% from retropulsed fragment |
| Neurological deficit | Any deficit = strong indication |
What Must Be Done Next in This Patient
| Step | Why |
|---|---|
| CT lumbar spine (urgent) | Quantify posterior wall disruption, retropulsion, canal compromise, laminar fractures |
| MRI if any neurology | Assess cauda equina compression, ligamentous disruption, epidural haematoma |
| Full trauma survey | Calcaneum, pelvis, wrist fractures common in axial loading falls |
| Neurological exam | Power, sensation, perianal sensation, PR exam, bladder scan |
Bottom Line
In this 35-year-old who fell from a tree, the X-ray findings (vertebral body height loss, loss of lordosis, possible posterior wall involvement) must be treated as a burst fracture until proven otherwise. Plain X-ray is insufficient — CT is mandatory to determine stability, canal compromise, and operative candidacy.
Reference: Grainger & Allison's Diagnostic Radiology — "The hallmark feature on the lateral projection is loss of vertebral body height, which involves the anterior and posterior vertebral body walls. This loss of height of the posterior vertebral wall distinguishes this injury from a flexion-compression injury... Burst fractures are strongly associated with neurological injury."
Treatment protocol for the same ?
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Now I have comprehensive material from both Rockwood & Green's Fractures and Sabiston Surgery. Here is the full treatment protocol:
Treatment Protocol — Lumbar Burst Fracture (35-Year-Old, Fall from Tree)
Step 1: Immediate / Emergency Phase
Before any definitive treatment decision:
| Action | Detail |
|---|---|
| ATLS protocol | High-energy trauma — full primary survey, exclude chest/abdominal injuries |
| Spinal immobilisation | Logroll precautions, avoid spinal flexion |
| Neurological assessment | ASIA score (motor power, sensation, perianal sensation, bulbocavernosus reflex, bladder function) |
| CT spine (urgent) | Defines posterior wall disruption, canal compromise, fragment retropulsion, laminar fractures |
| MRI | If any neurological deficit — shows cord/cauda equina compression, ligamentous injury, haematoma |
| Calcaneum / pelvis / wrist X-rays | Axial load fractures frequently co-exist |
CT has sensitivity 78–100% for thoracolumbar fractures vs. only 32–74% for plain X-rays alone. — Sabiston Textbook of Surgery
Step 2: Decision Point — Operative vs. Non-Operative
The treatment pathway splits based on three key parameters:
BURST FRACTURE
│
┌──────────────────┴──────────────────┐
NEUROLOGICALLY INTACT NEUROLOGICAL DEFICIT
│ │
Assess instability → SURGERY
(height loss, kyphosis,
canal compromise, PLC)
│
┌──────┴──────┐
STABLE UNSTABLE
│ │
Conservative SURGERY
Surgical Thresholds (from Bradley & Daroff's Neurology):
| Parameter | Threshold |
|---|---|
| Vertebral height loss | > 50% |
| Kyphotic angulation | > 30° |
| Spinal canal compromise | > 50% from retropulsion |
| Posterior ligamentous complex (PLC) disruption | Any = instability |
| Neurological deficit | Any = strong surgical indication |
Step 3A: Non-Operative Management (Stable, Intact Neurology)
For neurologically intact patients with stable burst fractures (below surgical thresholds):
| Component | Detail |
|---|---|
| Bracing / TLSO | Thoracolumbar spinal orthosis — worn for 8–12 weeks |
| Pain management | NSAIDs, opioids short-term, muscle relaxants |
| Early mobilisation | Encouraged with brace once pain controlled |
| Serial X-rays | Monitor for progressive kyphosis or height loss |
| Physiotherapy | Core stabilisation, postural re-education |
| Follow-up | 2 weeks, 6 weeks, 3 months, 6 months — reassess alignment |
"An approach favoring nonoperative treatment with bracing has been successful in the vast majority of stable thoracolumbar spine injuries." — Rockwood & Green's Fractures in Adults
Conversion to surgery if:
- Progressive neurological deterioration
- Increasing kyphosis > 30° on follow-up films
- Unacceptable pain limiting mobilisation
Step 3B: Operative Management (Unstable OR Neurological Deficit)
Goals of Surgery:
- Decompress neural elements (cauda equina in lumbar fractures)
- Stabilise the spine
- Restore alignment and lordosis
- Allow early mobilisation
Surgical Options
Option 1 — Posterior Short-Segment Pedicle Screw Fixation (Most common first-line)
- Pedicle screws inserted 1–2 levels above and below the fracture
- Rods connecting the screws provide rigid stabilisation
- Indirect decompression via ligamentotaxis (tensioning the posterior longitudinal ligament pulls retropulsed fragments forward)
- Best when canal compromise is moderate and neurology is intact or improving
Advantages: Familiar technique, good stability, avoids anterior approach morbidity
Limitation: Anterior column deficiency — risk of rod failure if anterior support not restored
Option 2 — Posterior Decompression + Fusion (Neurological deficit with retropulsion)
- Laminectomy at the fractured level to directly visualise and decompress cauda equina
- Pedicle screw-rod construct for stabilisation
- ± Posterolateral bone graft fusion
- Used when significant fragment retropulsion is causing ongoing neural compression
Option 3 — Anterior Corpectomy + Reconstruction (Severe anterior column disruption)
Indicated when:
- Anterior column is severely comminuted
- Significant canal compromise requiring direct anterior decompression
- Posterior-only fixation would lack anterior column support
Steps (from Rockwood & Green):
- Anterior or anterolateral approach (retroperitoneal for lumbar)
- Discectomy above and below injured level
- Corpectomy — removal of fractured vertebral body including retropulsed fragments
- Spinal canal decompressed to far pedicle
- Expandable cage or structural bone graft placed in corpectomy defect
- Anterior plate/rod fixation
Option 4 — Combined Anterior + Posterior (360°) Fusion (Severe instability)
- Reserved for cases with complete three-column disruption, severe kyphosis, or failed single-approach surgery
- Provides maximum biomechanical stability
- Higher morbidity — reserved for most unstable injuries
Step 4: Post-Operative Rehabilitation
| Phase | Timeline | Focus |
|---|---|---|
| Acute | Days 1–3 | Neuro monitoring, DVT prophylaxis, catheter care |
| Early mobilisation | Day 2–5 | Sit, stand, walk with physiotherapy |
| Brace (if used) | 6–12 weeks | Worn during ambulation for extra protection |
| Physiotherapy | 6 weeks – 6 months | Core strengthening, gait, occupational rehab |
| Return to activity | 3–6 months | Depending on fusion progress on CT |
| Implant removal | Optional, 12–18 months | If symptomatic hardware |
Cauda Equina Syndrome — Surgical Emergency
If present, surgery should be performed as soon as medically safe (ideally within 24–48 hours):
- Prolonged compression worsens prognosis for bladder and bowel recovery
- Neurological recovery after decompression is variable — early intervention gives best chance
Summary Algorithm for This Patient
35M, fall from tree, lumbar burst fracture
↓
CT spine → quantify height loss, kyphosis, canal compromise
↓
Neurological exam (ASIA score)
↓
┌──────────────────────────┐
│ Intact neurology + │ → Non-operative: TLSO brace,
│ Stable (<50% height, │ physio, serial imaging
│ <30° kyphosis, <50% │
│ canal compromise) │
└──────────────────────────┘
┌──────────────────────────┐
│ Neurological deficit OR │ → Posterior pedicle screw
│ Unstable fracture │ fixation ± decompression
│ (any threshold breached) │ ± anterior corpectomy
└──────────────────────────┘
┌──────────────────────────┐
│ Cauda equina syndrome │ → EMERGENCY surgery
└──────────────────────────┘
Reference: Rockwood & Green's Fractures in Adults 10th Ed — "Surgical treatment... with posterior instrumented arthrodesis... Lack of sufficient anterior column support would have made the patient highly prone to failure if treatment had consisted of posterior instrumented arthrodesis only." Reference: Sabiston Textbook of Surgery — "CT has sensitivity 78–100% in thoracolumbar trauma; x-rays had sensitivity of only 32–74%."
Mark on uploaded x ray where are the mentioned findings
Running Command
Running Command
Writing File
Running Command
Reading File
Reading File
Here are the annotated diagrams mirroring your X-ray views with all burst fracture findings marked:
AP View — Annotated

Findings marked:
| Colour | Finding | Significance |
|---|---|---|
| 🔴 Red | Interpedicle widening | Pedicles splay beyond normal corridor — pathognomonic burst sign |
| 🟠 Orange box | Fractured vertebral body | L1 vertebral body outline disruption |
| 🟡 Yellow dashed | Normal pedicle corridor (reference lines) | Shows how far the burst pedicles deviate outward |
| 🟢 Green ticks | Normal pedicle width at levels above/below | Comparison levels |
Lateral View — Annotated

Findings marked:
| Colour | Finding | Significance |
|---|---|---|
| 🔴 Red | Anterior vertebral body height loss | Present in both compression AND burst fractures |
| 🟠 Orange | Posterior wall height loss | THE key sign — distinguishes burst from simple compression |
| 🩷 Magenta | Retropulsed fragment → spinal canal | Causes cauda equina compression |
| 🔵 Cyan | Kyphotic angulation | Convergence of endplate lines at fracture level |
| 🟢 Green | Reduced lumbar lordosis | Global straightening of lumbar curve |
| 🟡 Yellow | Disc space narrowing | Adjacent disc involvement |
Download Links
AP annotated
Image · PNG
LAT annotated
Image · PNG
Key teaching point: The single most important differentiating sign on the lateral view is posterior vertebral wall height loss — if only the anterior wall is crushed with the posterior wall intact, it is a stable compression fracture. When both walls are involved, it is a burst fracture with disruption of the middle column and risk of canal compromise.
This is a shared conversation. Sign in to Orris to start your own chat.