SDH
Reading File
Asking for Preferences
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Subdural Hematoma (SDH)
Definition & Anatomy
A subdural hematoma is a collection of blood in the potential space between the dura mater and the arachnoid membrane, caused by tearing of bridging veins that traverse the subdural space carrying venous blood from the cerebral cortex to the dural sinuses.
Pathophysiology
- Mechanism: Sudden acceleration-deceleration forces shear the bridging dural veins → venous bleeding into the subdural space
- Blood accumulates slowly (venous, low pressure) — unlike the arterial bleeding of epidural hematoma
- Frequently associated with concurrent brain parenchymal damage (contusions, diffuse axonal injury)
- Acute SDH may also result from: anticoagulant use, aneurysm rupture into the subdural space (rare), or non-accidental trauma in infants
Risk Groups
| Group | Reason |
|---|---|
| Elderly | Cerebral atrophy → longer, more mobile bridging veins |
| Chronic alcoholics | Atrophic brain + coagulopathy |
| Anticoagulant users | Continued venous leakage, failure to tamponade |
| Infants <2 years | Thin skull, large head-to-neck ratio |
| Hemodialysis patients | Heparinization + uremic platelet dysfunction |
Classification
Acute SDH (onset within 14 days of injury)
- Usually follows severe trauma; patient often presents in coma
- Associated with underlying cerebral contusions and edema
- Surgical emergency — early evacuation improves outcome
- Mortality remains significant due to underlying brain damage
Subacute SDH (days 4–14)
- Isodense on CT; harder to identify — may require IV contrast or MRI
Chronic SDH (>14 days)
- Common in elderly, alcoholics, anticoagulated patients
- Often follows trivial or unrecalled trauma
- A membrane forms around the hematoma; friable neovascularization leads to re-bleeding
- Osmotic expansion: breakdown products draw in water → enlarging mass
Clinical Features
- Headache (majority, but not universal)
- Fluctuating level of consciousness — hallmark, can mimic metabolic encephalopathy or TIA
- Tenderness to skull percussion at the hematoma site
- Focal signs in 15–30%: hemiparesis, seizures, visual field defects
- Unusual features: parkinsonism, dystonia, asterixis
- Bilateral in ~20%; occasional interhemispheric location → bilateral leg weakness
A useful clinical rule: "It could always be a subdural" — imaging is required even without focal signs in any comatose patient. — Plum and Posner's Diagnosis and Treatment of Stupor and Coma
CT Imaging
| Stage | CT Appearance |
|---|---|
| Acute | Hyperdense (white), crescent-shaped, crosses suture lines |
| Subacute | Isodense — easily missed |
| Chronic | Hypodense (dark) — iron has been metabolized |
Chronic SDH CT (labeled):
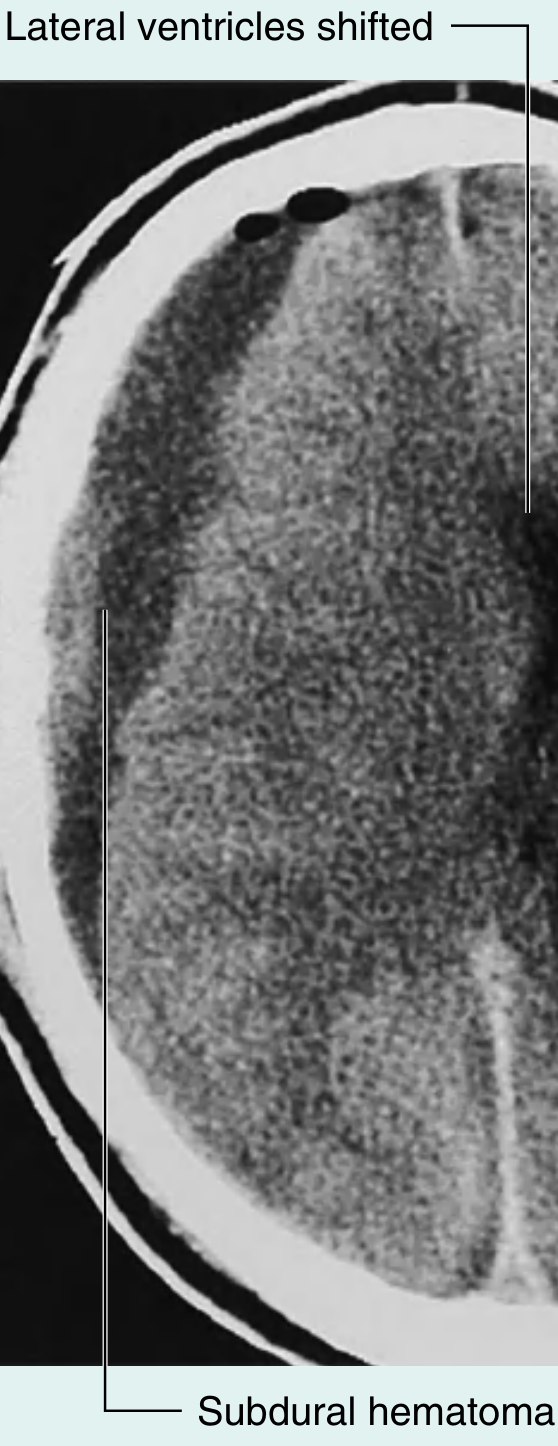
Acute SDH CT:
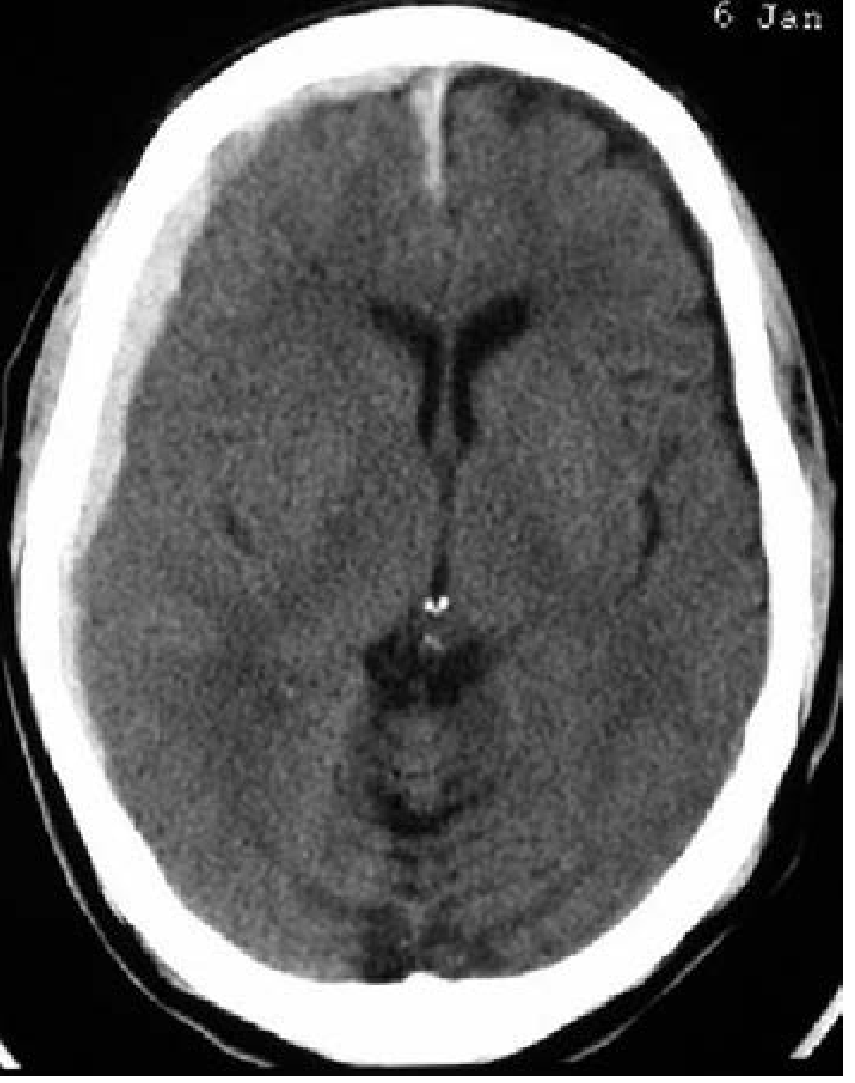
Management
| Type | Management |
|---|---|
| Acute/subacute | Surgical evacuation (craniotomy) — high mortality, higher need for surgery |
| Chronic | May be managed conservatively if small/minimally symptomatic; burr-hole drainage for larger collections |
| Anticoagulated | Reverse anticoagulation promptly |
| Corticosteroids | Reduce vasogenic edema from the hematoma membrane; can rapidly reverse symptoms in chronic SDH |
Sources: Tintinalli's Emergency Medicine, A Comprehensive Study | Plum and Posner's Diagnosis and Treatment of Stupor and Coma | Gray's Anatomy for Students
This is a shared conversation. Sign in to Orris to start your own chat.