eye dark circle
Reading File
Finding Sources
Finding Sources
Searching Images
periorbital dark circles eye hyperpigmentation
Reading File
Here is a comprehensive overview of eye dark circles (Periorbital Hyperpigmentation / Infraorbital Melanosis):
Eye Dark Circles (Periorbital Hyperpigmentation)
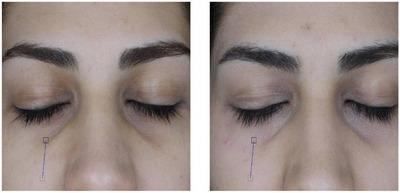
Definition
Dark circles under the eyes are clinically termed periorbital hyperpigmentation (POH) or infraorbital melanosis. They represent brown-black, non-scaly, non-erythematous pigmentation on the upper, lower, or both eyelids.
Epidemiology
- Affects males and females equally
- Most common in individuals with darker skin types (Fitzpatrick types III–VI)
- Onset typically in young adults
- Familial/racial/constitutional forms are especially prevalent in South Asian, Middle Eastern, and African populations
- — Fitzpatrick's Dermatology, Vol. 1 & 2
Causes & Pathogenesis
| Category | Examples |
|---|---|
| Constitutional/Racial | Familial melanin deposition; especially common in people with skin of color |
| Vascular | Venous congestion, chronic allergic conjunctivitis, visible subdermal vessels through thin skin |
| Post-inflammatory | Eczema, contact dermatitis, atopic dermatitis |
| Structural/Anatomical | Age-related dermal thinning, tear trough hollowing, periorbital fat descent |
| Pigmentary dermatoses | Lichen planus pigmentosus, medication-induced hyperpigmentation, pigmented contact dermatitis |
| Lifestyle/Environmental | Chronic sleep deprivation, sun exposure, fatigue |
| Systemic | Rarely: connective tissue disorders (e.g., Ehlers-Danlos syndrome) |
Histologically, constitutional pigmentation shows increased melanin in the basal epidermis and melanophages in the upper dermis.
Clinical Features
- Asymptomatic, bilateral brownish-black discoloration of the periorbital skin
- Accentuation of skin creases
- May show visible vessels beneath the lower eyelid (vascular type)
- Infraorbital edema ("puffiness") may co-exist
- Usually progressive without treatment
Differential Diagnosis
- Lichen planus pigmentosus
- Medication-induced pigmentation (e.g., prostaglandin analogs, anti-malarials)
- Post-inflammatory hyperpigmentation (after eczema/contact dermatitis)
- Periorbital edema (fluid accumulation)
- Heliotrope rash (dermatomyositis — violaceous discoloration, not just dark pigment)
Diagnosis
Primarily clinical. Dermoscopy or Wood's lamp can help distinguish epidermal (superficial melanin — enhanced under Wood's lamp) from dermal or vascular types.
Management
| Approach | Options |
|---|---|
| Topical agents | Hydroquinone, kojic acid, azelaic acid, retinoids, vitamin C, niacinamide, sunscreen |
| Chemical peels | Glycolic acid, TCA peels |
| Laser/light therapy | Q-switched Nd:YAG, fractional lasers, IPL (for vascular type) |
| Injectables | Hyaluronic acid fillers (for tear trough hollowing), carboxytherapy (improves microcirculation) |
| Surgery | Autologous fat transplantation (blepharoplasty for structural causes) |
| Treat underlying cause | Address allergies, dermatitis, medications as applicable |
Key principle: Treatment of the underlying dermatosis (if present) is critical before pursuing cosmetic interventions. Studies on topical therapy, peels, and lasers are difficult to interpret because they often don't specify the underlying cause. — Fitzpatrick's Dermatology, Vol. 1 & 2
Prognosis
Constitutional pigmentation is usually progressive. Vascular and post-inflammatory types are more amenable to targeted treatment. Structural causes respond best to filler or surgical correction.
Hydroquinone, kojic acid, azelaic acid, retinoids, vitamin C, niacinamide, sunscreen give me medicine
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Here is a detailed breakdown of each topical agent used for eye dark circles (periorbital hyperpigmentation):
Topical Medicines for Dark Circles
1. 🔵 Hydroquinone
- Mechanism: Inhibits tyrosinase enzyme → blocks melanin biosynthesis
- Concentrations: 2% OTC (over-the-counter) | 3–4% prescription
- Key products: Lustra, Melanex, Solaquin
- Best combo: Tri-Luma = Hydroquinone + Fluocinolone acetonide (steroid) + Retinoic acid ("Kligman formula") — most effective combination
- Side effects: Local irritation, allergic contact dermatitis, risk of ochronosis with prolonged use
- Note: Most effective tyrosinase inhibitor available. Temporary lightening (not permanent).
- — Katzung's Basic & Clinical Pharmacology, 16th Ed.
2. 🟡 Kojic Acid
- Mechanism: Tyrosinase inhibitor (similar to hydroquinone)
- Concentrations: 1–4%
- Use: Alternative when hydroquinone is not tolerated or during "holiday" breaks from hydroquinone to prevent tachyphylaxis
- Note: Popular in Asia; often combined with glycolic acid or vitamin C
- — Fitzpatrick's Dermatology; Pfenninger & Fowler's Procedures for Primary Care
3. 🟠 Azelaic Acid
- Mechanism: Tyrosinase inhibitor + anti-inflammatory; also reduces post-inflammatory hyperpigmentation
- Concentrations: 15–20%
- Use: Effective for melasma and post-inflammatory hyperpigmentation; also treats acne/rosacea simultaneously
- Advantage: Safe in pregnancy (category B), minimal irritation
- — Dermatology 2-Volume Set 5e
4. 🟣 Retinoids (Retinol / Retinoic Acid / Tretinoin)
- Mechanism:
- Inhibits tyrosinase
- Accelerates desquamation of melanosome-laden keratinocytes (speeds up skin turnover, removing pigmented cells)
- Prevents skin thinning caused by steroids in combination formulas
- Forms: Tretinoin 0.025–0.1% (prescription) | Retinol (OTC, weaker)
- Use: Core component of Kligman formula; can be used as monotherapy
- Side effects: Dryness, irritation, photosensitivity — use at night, apply SPF in morning
- — Fitzpatrick's Dermatology
5. 🟡 Vitamin C (Ascorbic Acid / L-Ascorbic Acid)
- Mechanism: Tyrosinase inhibitor with a different structural pathway than hydroquinone/kojic acid
- Concentrations: 10–15%
- Key advantage: Can be used during hydroquinone "holiday" periods (every 3–6 months) to prevent tachyphylaxis, while still maintaining depigmenting effect
- Additional benefit: Antioxidant, stimulates collagen synthesis, improves skin brightness
- — Fitzpatrick's Dermatology; Dermatology 2-Volume Set 5e
6. 🔴 Niacinamide (Vitamin B3)
- Mechanism: Does not inhibit tyrosinase. Instead, it blocks melanosome transfer from melanocytes to keratinocytes (PAR-2 pathway inhibition)
- Concentration: 4–5%
- Use: Gentle, well-tolerated; suitable for sensitive periorbital skin
- Additional benefits: Reduces fine lines, strengthens skin barrier, anti-inflammatory
- — Fitzpatrick's Dermatology; Dermatology 2-Volume Set 5e
7. ☀️ Sunscreen (SPF 30–50+)
- Mechanism: Absorbs (chemical sunscreen) or reflects (physical — zinc oxide, titanium dioxide) UV radiation → prevents UV-driven melanin production
- Why essential: UV light stimulates melanocytes; without sunscreen, all other treatments are undermined
- Types:
- Chemical: Oxybenzone, avobenzone, octinoxate (UVA + UVB)
- Physical/Mineral: Zinc oxide, titanium dioxide — preferred around the eyes (less irritating)
- Use: Apply every morning, reapply if outdoors
- — Katzung's Basic & Clinical Pharmacology, 16th Ed.
Recommended Regimen Summary
| Step | Time | Agent |
|---|---|---|
| Morning | AM | Vitamin C serum → Niacinamide → Sunscreen SPF 30+ |
| Evening | PM | Retinoid (tretinoin/retinol) → Hydroquinone or Kojic acid or Azelaic acid |
| Prescription combo | PM | Tri-Luma (Hydroquinone 4% + Fluocinolone + Tretinoin) — doctor-supervised |
Important: All these agents should be applied carefully around the eye area — avoid direct contact with the eye itself. Prescription-strength products require dermatologist supervision. Sunscreen is non-negotiable regardless of which other agents are used.
Tri-Luma
Finding Sources
Finding Sources
Reading File
Reading File
Tri-Luma Cream — Complete Drug Profile
What Is It?
Tri-Luma is an FDA-approved prescription triple-combination topical cream, also known as the modified Kligman formula. It combines three active agents that work synergistically to reduce hyperpigmentation.
Composition
| Component | Concentration | Role |
|---|---|---|
| Hydroquinone | 4% | Primary depigmenting agent |
| Fluocinolone acetonide (corticosteroid) | 0.01% | Anti-inflammatory |
| Tretinoin (retinoic acid) | 0.05% | Enhances penetration + speeds skin turnover |
Mechanism of Each Component
1. Hydroquinone 4%
- Inhibits tyrosinase → blocks conversion of DOPA → melanin
- Also: degrades melanosomes, causes reactive oxygen radical production that destroys melanocytes
- Provides the core lightening effect
- — Fitzpatrick's Dermatology; Goodman & Gilman's Pharmacological Basis of Therapeutics
2. Tretinoin 0.05%
- Inhibits transcription of tyrosinase
- Stimulates keratinocyte turnover → accelerates desquamation of pigmented cells
- Decreases melanosome transfer from melanocytes to keratinocytes
- Prevents skin thinning (counteracts the atrophic side effect of the steroid)
- Enhances penetration of hydroquinone into deeper skin layers
- — Fitzpatrick's Dermatology
3. Fluocinolone acetonide 0.01%
- A mild topical corticosteroid
- Suppresses inflammation caused by hydroquinone and tretinoin (reduces redness, irritation)
- Also independently inhibits tyrosinase
- Prevents post-inflammatory hyperpigmentation from irritation
- — Katzung's Basic & Clinical Pharmacology
Why the combination is superior: Each agent addresses a different step — hydroquinone blocks melanin synthesis, tretinoin clears existing pigment and boosts penetration, fluocinolone calms inflammation. Once-daily Tri-Luma was proven more effective than twice-daily hydroquinone 4% alone in moderate-to-severe facial melasma. — Fitzpatrick's Dermatology
Indications
- Melasma (primary FDA-approved indication — facial melasma)
- Periorbital hyperpigmentation (dark circles) — off-label but widely used
- Post-inflammatory hyperpigmentation
- Pre- and post-treatment adjunct for chemical peels, laser procedures
- Erythema ab igne pigmentation
How to Use
| Parameter | Details |
|---|---|
| Frequency | Once daily at night |
| Application | Apply a thin layer to the affected area, approximately 30 min before bedtime |
| Duration | Short-term — typically up to 8 weeks (limit use to avoid steroid-related side effects) |
| Sunscreen | Mandatory every morning (SPF 30+) — sun exposure worsens melasma and negates treatment |
Side Effects
| Side Effect | Cause |
|---|---|
| Irritant/contact dermatitis | Hydroquinone or tretinoin |
| Erythema, dryness, peeling | Tretinoin |
| Skin atrophy (with prolonged use) | Fluocinolone (steroid) |
| Ochronosis (rare, bluish-black discoloration) | Prolonged/excessive hydroquinone use |
| Post-inflammatory hyperpigmentation | Over-irritation (paradoxical worsening) |
| Photosensitivity | Tretinoin |
Contraindications
- Pregnancy (Category C — avoid; hydroquinone and tretinoin carry fetal risks)
- Breastfeeding
- Known hypersensitivity to any component
- Active skin infections or open wounds at application site
Important Notes
- Not for use near the eyes — avoid direct contact with the eye itself; apply only to periorbital skin, keeping distance from the eyelid margin
- Do not use on large body surface areas (systemic steroid absorption risk)
- Discontinue if severe irritation, ochronosis, or paradoxical darkening occurs
- Regular dermatologist follow-up is essential during treatment
Sources: Katzung's Basic & Clinical Pharmacology 16th Ed.; Fitzpatrick's Dermatology Vol. 1 & 2; Goodman & Gilman's Pharmacological Basis of Therapeutics; Pfenninger & Fowler's Procedures for Primary Care
This is a shared conversation. Sign in to Orris to start your own chat.