Mechanism of photo therapy
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
On bilirubin
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Loading Image
The user asked about the mechanism of phototherapy on bilirubin — here is a comprehensive answer synthesized from multiple authoritative textbooks:
Mechanism of Phototherapy on Bilirubin
Why Phototherapy Is Needed in Neonates
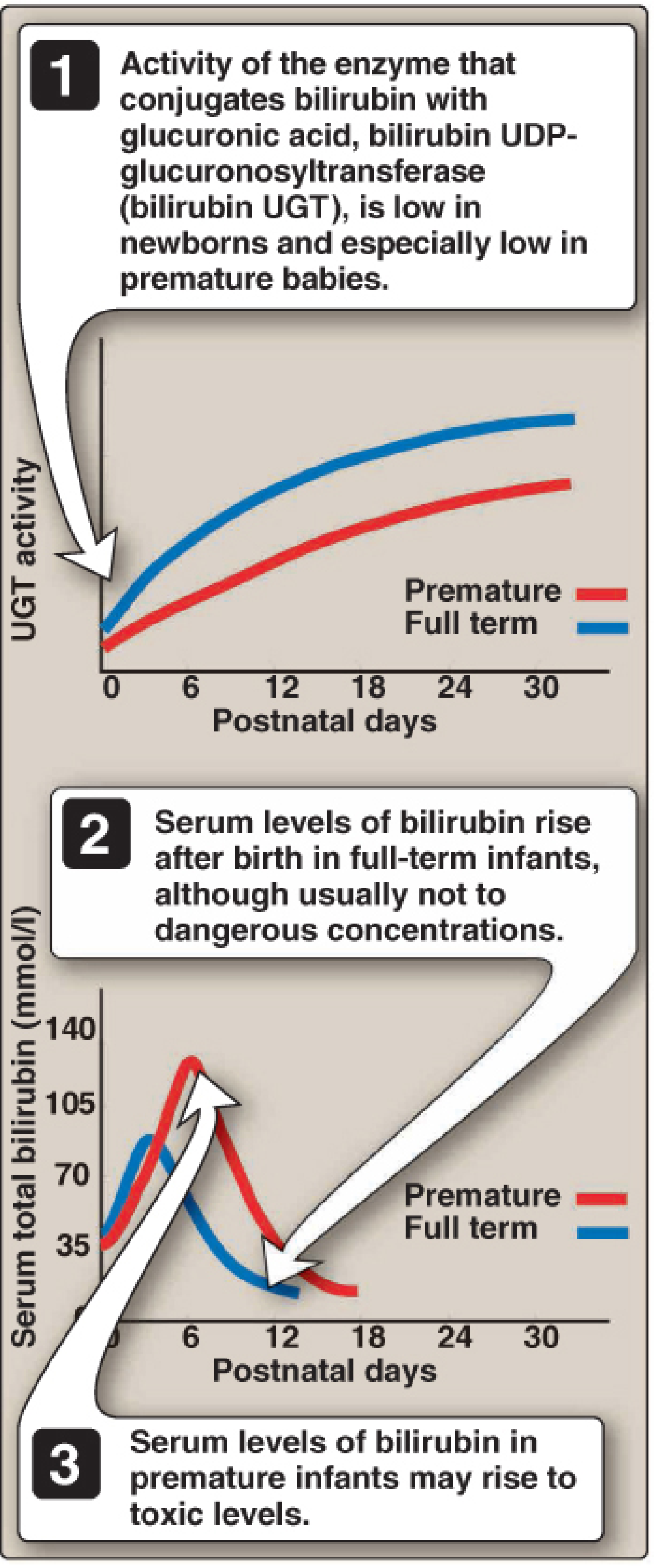
At birth, bilirubin UDP-glucuronosyltransferase (UGT) activity is low — especially in premature infants — making the liver unable to conjugate bilirubin adequately. Plasma unconjugated bilirubin (UCB) rises from <1 mg/dL normally to ~5 mg/dL in the first 3 days of life. When UCB exceeds the albumin-binding capacity (~20–25 mg/dL), free bilirubin crosses the blood–brain barrier, depositing in the basal ganglia and causing kernicterus (toxic encephalopathy, mental retardation).
The Light Source
Phototherapy uses blue-green light, optimally at a peak of 478 nm, which corresponds to the absorption maximum of bilirubin. This wavelength penetrates the skin and reaches bilirubin in the superficial microcirculation.
Three Photochemical Reactions
When bilirubin in the skin is exposed to blue-green light, three distinct reactions occur:
1. Configurational (Geometric) Isomerization (fastest, reversible)
- Native bilirubin exists as the 4Z,15Z form, stabilized by internal hydrogen bonds that make it lipophilic and unable to be excreted without conjugation.
- Light converts it to 4Z,15E and 4E,15Z photoisomers (Z→E rotation around the double bonds).
- These configurational isomers are more polar (internal H-bonds disrupted) and can be excreted directly into bile without conjugation.
- This reaction is reversible — in the dark or gut, E-isomers revert to the Z form.
2. Structural Isomerization → Lumirubin (slower, irreversible)
- A more permanent cyclization reaction converts bilirubin to lumirubin (a cyclobilirubin/intramolecular cyclization product).
- Lumirubin is water-soluble and can be excreted in both bile and urine without conjugation.
- This is considered the most clinically important pathway because it is irreversible.
3. Photo-oxidation (slowest)
- Bilirubin is oxidized to colorless, water-soluble small molecules (e.g., maleimide, propentdyopents).
- These are excreted in urine.
- This pathway is quantitatively minor under clinical phototherapy conditions.
Net Result
| Photoproduct | Solubility | Excretion Route | Reversibility |
|---|---|---|---|
| Configurational isomers (4Z,15E) | More polar | Bile (without conjugation) | Reversible |
| Lumirubin | Water-soluble | Bile + Urine | Irreversible |
| Photo-oxidation products | Water-soluble | Urine | Irreversible |
All three pathways bypass the liver's conjugation step, allowing unconjugated bilirubin to be eliminated from the body. The net effect is a rapid decrease in plasma UCB, reducing neurotoxicity risk.
"Blue fluorescent light (phototherapy)... converts bilirubin to more polar and, therefore, water-soluble isomers. These photoisomers can be excreted into the bile without conjugation to glucuronic acid." — Biochemistry, Lippincott Illustrated Reviews, 8th ed.
"Phototherapy is performed by exposing the infant to light in the blue-green wavelength range, preferably at an optimal peak of 478 nm. This light converts unconjugated bilirubin (mainly in the microcirculation of the skin) to the water-soluble bilirubin isomer that can be excreted in the urine and feces." — Guyton and Hall Textbook of Medical Physiology
Clinical Notes
- Phenobarbital is an adjunct that induces bilirubin UGT, accelerating conjugation — useful in Crigler-Najjar type II.
- In Crigler-Najjar type I (complete absence of UGT), phototherapy reduces bilirubin somewhat but phenobarbital has no effect; the disease is often fatal without liver transplantation.
- HPLC has been used to identify and quantify bilirubin photoisomers in neonatal blood to study these pathways in vivo. — Tietz Textbook of Laboratory Medicine, 7th ed.; Harper's Illustrated Biochemistry, 32nd ed.; Robbins & Kumar Basic Pathology
This is a shared conversation. Sign in to Orris to start your own chat.