Conjunctivitis children
Reading File
Finding Sources
Searching PubMed
conjunctivitis children management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have all the information needed to provide a comprehensive answer on conjunctivitis in children.
Conjunctivitis in Children
Conjunctivitis is one of the most common causes of the red eye in pediatrics. The clinical challenge is identifying the rare serious infection (gonococcal, herpetic) from the far more common, self-limited viral or mild bacterial forms.
Types and Clinical Features
1. Viral Conjunctivitis (most common)
- Cause: Adenovirus most common; HSV less common but more dangerous
- Symptoms: Watery discharge, bilateral (often starts unilateral), foreign body sensation, preauricular lymphadenopathy, may follow upper respiratory infection
- Exam: Follicles on inferior palpebral conjunctiva; punctate fluorescein staining indicates keratitis
- Key point: Always examine the cornea with fluorescein — a missed herpetic dendrite is a vision-threatening error
2. Bacterial Conjunctivitis
- Cause: S. pneumoniae, H. influenzae, Staphylococcus spp.
- Symptoms: Mucopurulent discharge (eyelids adherent on waking), conjunctival injection, usually painless
- Exam: Clear cornea; chemosis common; preauricular adenopathy absent (except gonococcal)
- Note: Often self-limited, but antibiotics shorten the course
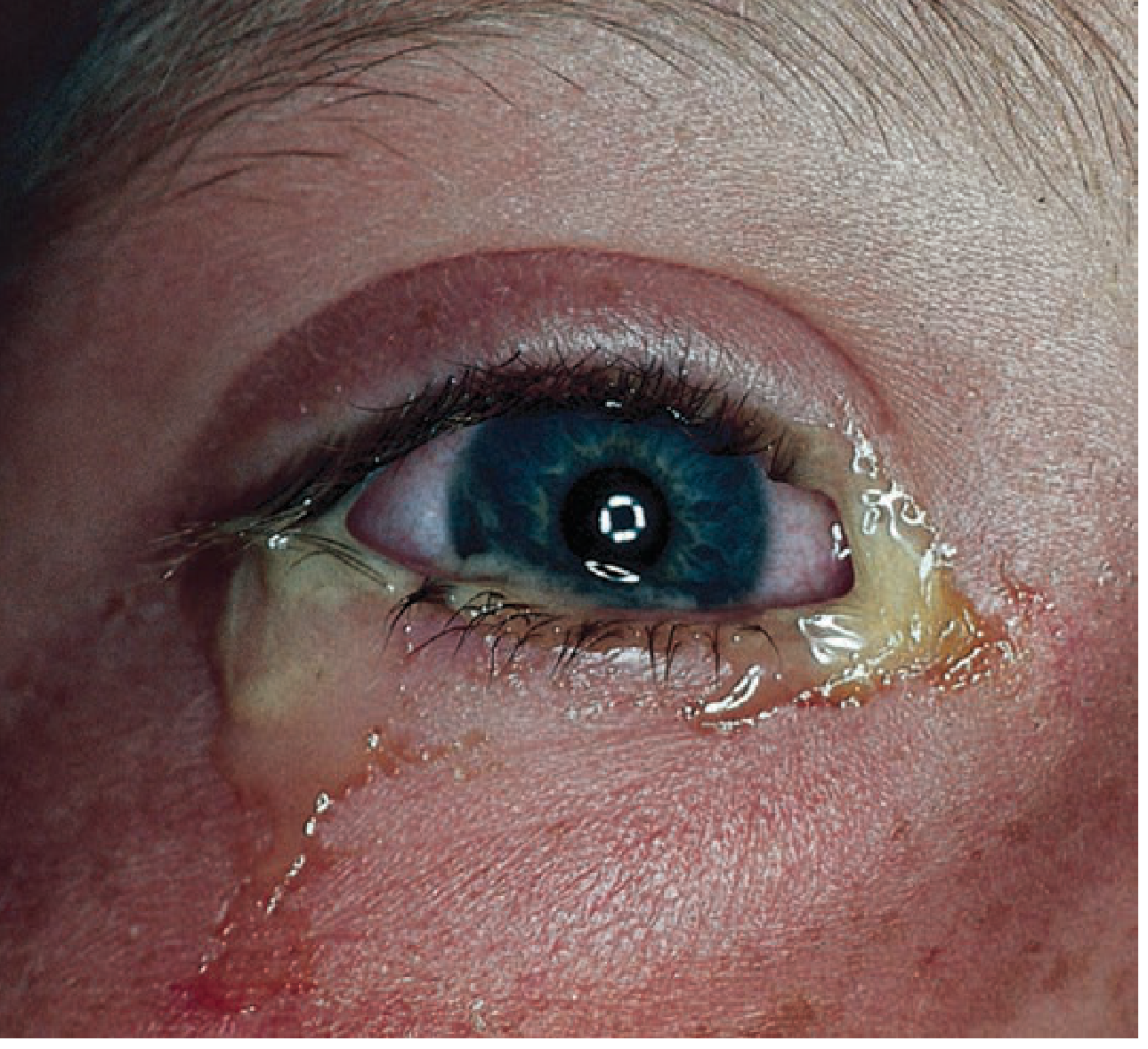
3. Allergic Conjunctivitis
- Symptoms: Bilateral, intensely pruritic, watery discharge, swollen lids
- Exam: Papillae (irregular mounds with central vascular tuft) on inferior conjunctival fornix; prominent chemosis
- Management: Identify and remove allergen; cool compresses
Summary Table (from Harriet Lane Handbook, 23rd ed.)
| Feature | Viral | Bacterial | Allergic |
|---|---|---|---|
| Discharge | Watery | Purulent, crusting | Watery |
| Itching | Mild | Absent | Prominent |
| Laterality | Often bilateral | Uni or bilateral | Bilateral |
| Lymphadenopathy | Yes (preauricular) | No | No |
| Fever | May be present | May be present | Absent |
Neonatal Conjunctivitis (Ophthalmia Neonatorum)
Special consideration in neonates (≤30 days). Categorized by timing of onset:
| Type | Cause | Age of Onset | Key Findings | Treatment |
|---|---|---|---|---|
| Chemical | Erythromycin prophylaxis | First 24 h | Bilateral, watery, negative Gram stain | Watchful waiting; resolves in 48 h |
| Gonococcal | N. gonorrhoeae | 2–7 days | Intense chemosis, copious purulent discharge, gram-negative diplococci | Admit + IV ceftriaxone (50 mg/kg, max 125 mg) single dose; saline eye irrigation; evaluate for disseminated disease |
| Chlamydial | C. trachomatis | 7–14 days | Purulent discharge, intense palpebral erythema | Oral erythromycin 12.5 mg/kg PO q6h × 14 days + erythromycin ophthalmic ointment; may discharge if no pneumonia |
| Other bacterial | S. aureus, H. influenzae, E. coli, Pseudomonas | 7–14 days | Variable; identify by Gram stain | Topical bacitracin-polymyxin; admit for nontypeable H. influenzae |
| Viral (HSV) | HSV-1 or HSV-2 | 14–28 days | Lid edema, dendrites on fluorescein | Admit + IV acyclovir 20 mg/kg q8h × 14–21 days + topical antivirals; avoid steroids |
Gonococcal and herpetic neonatal conjunctivitis can progress to corneal perforation or disseminated disease — both require hospital admission.
Management in Older Children
Bacterial (non-gonococcal, non-chlamydial)
- First-line: Ophthalmic polymyxin B/trimethoprim drops — avoids sulfa and neomycin allergy risk
- Ointments are preferred in young children (easier to administer)
- Contact lens wearers: Treat with a fluoroquinolone (besifloxacin, moxifloxacin, ofloxacin) or tobramycin to cover Pseudomonas
- Gonococcal/chlamydial: Requires systemic antibiotic treatment in addition to topical therapy
Viral
- Supportive: cool compresses, artificial tears (5–6×/day), ocular decongestants (e.g., Naphcon-A)
- Course: 1–3 weeks; highly contagious — hand hygiene, separate towels
- If uncertain bacterial vs. viral: treat empirically with topical antibiotics and re-evaluate
Allergic
- Cool compresses QID
- Mild: artificial tears alone
- Moderate: topical antihistamine/decongestant, mast cell stabilizers, or topical NSAIDs
- Severe: topical steroids only with ophthalmology input (risk of masking herpetic infection)
Red Flags — When to Refer to Ophthalmology
- Photophobia or vision loss
- Severe pain
- Recurrent episodes
- Suspected gonococcal infection
- Any corneal opacity, dendrites, or staining on fluorescein
- Neonatal conjunctivitis with concern for gonorrhea or HSV
Sources:
- The Harriet Lane Handbook (23rd ed.), Head & Neck section
- Tintinalli's Emergency Medicine (9th ed.), Ch. 122 (Eye Emergencies in Infants and Children) and Ch. 241 (Conjunctivitis)
This is a shared conversation. Sign in to Orris to start your own chat.