Hey orris
Hey! How can I help you?
Can u plss teach me VESTIBULAR,DIZZINESS AND VERTIGO IN DETAIL related to full body from where the patient can feel dizziness,plss provide me the full detail like a short book
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
Now I have rich, comprehensive information from Harrison's, Rosen's Emergency Medicine, and Ganong's physiology. Let me compile the full detailed response.
🧠 Vestibular System, Dizziness & Vertigo — A Complete Guide
Sources: Harrison's Principles of Internal Medicine 22E | Rosen's Emergency Medicine | Ganong's Review of Medical Physiology
PART 1: WHAT IS DIZZINESS?
Dizziness is an imprecise symptom — patients use it to describe many different sensations. Clinically, it breaks into four distinct categories:
| Category | What the Patient Feels |
|---|---|
| Vertigo | Illusion of spinning or motion (room spinning, or self spinning) |
| Near-syncope | Feeling faint or lightheaded (brain under-perfused) |
| Disequilibrium | Unsteadiness when walking, no spinning sensation |
| Nonspecific dizziness | Vague, hard to describe — often polysensory or anxiety-related |
The challenge in diagnosis is that patients often cannot distinguish between these, and the words they choose do not reliably indicate the underlying cause.— Harrison's Principles of Internal Medicine 22E
PART 2: THE VESTIBULAR SYSTEM — ANATOMY & PHYSIOLOGY
Where Is It?
The vestibular apparatus sits inside the inner ear (labyrinth), embedded in the petrous portion of the temporal bone (deep inside the skull, behind the ear).
What Does It Contain?
The labyrinth has two functional parts:
1. Three Semicircular Canals
- Oriented in three planes (horizontal, anterior, posterior)
- Detect angular (rotational) head movement
- Filled with endolymph fluid
- Paired left and right — normally respond symmetrically
2. Two Otolithic Organs
- Utricle — detects head tilt and vertical linear acceleration (e.g., going up in an elevator). Contains otoliths (calcium carbonate crystals on hair cells).
- Saccule — detects vertical linear motion
How Does the Signal Travel?
Inner Ear (Labyrinth)
↓
CN VIII (Vestibulocochlear nerve)
↓
Enters brainstem below the pons, anterior to cerebellum
↓
4 Vestibular Nuclei (brainstem) ←→ Cerebellum
↓ ↓
Medial Longitudinal Vestibulospinal Tract
Fasciculus (MLF) (to limb muscles)
↓
Eye muscles (VOR) Postural muscles
- The MLF connects vestibular nuclei to the eye muscles → controls eye movements to compensate for head motion
- The vestibulospinal tract connects to limb motor neurons → maintains posture and balance
- Autonomic connections → explain why vertigo causes sweating, nausea, and vomiting
- Cerebral cortex connections → conscious perception of motion and spatial orientation
The Three Systems That Maintain Balance
Equilibrium and spatial awareness depend on the integration of three systems, processed through the cerebellum via the vestibular nuclei:
| System | What It Contributes |
|---|---|
| Vestibular | Head position, acceleration, rotation |
| Visual | Environmental reference frame |
| Proprioceptive | Body position, joint sense (from muscles, joints, skin) |
Any disease that causes a mismatch of information from any two of these three systems may give rise to symptoms of vertigo.— Rosen's Emergency Medicine
PART 3: WHERE IN THE BODY CAN DIZZINESS COME FROM?
This is the key question. Dizziness has a broad anatomical origin — from the inner ear all the way to the heart.
🔴 A. PERIPHERAL VESTIBULAR CAUSES (Inner Ear / Vestibular Nerve)
These are the most common causes — generally benign but can be severely symptomatic.
1. Benign Paroxysmal Positional Vertigo (BPPV)
- Most common cause of recurrent vertigo
- Caused by displaced otoconia (calcium carbonate crystals) that have broken free from the utricular macula and floated into one of the semicircular canals (usually the posterior canal)
- When the head position changes, gravity moves the crystals through the canal → triggers sudden vertigo
- Onset: Sudden, lasts <1 minute (typically 15–20 sec)
- Triggers: Lying down, rolling in bed, looking up, rising from supine
- Nystagmus pattern: Upward + torsional (toward the affected ear)
- Treatment: Repositioning maneuvers (Epley maneuver)
Modified Epley Maneuver (Treatment for BPPV):
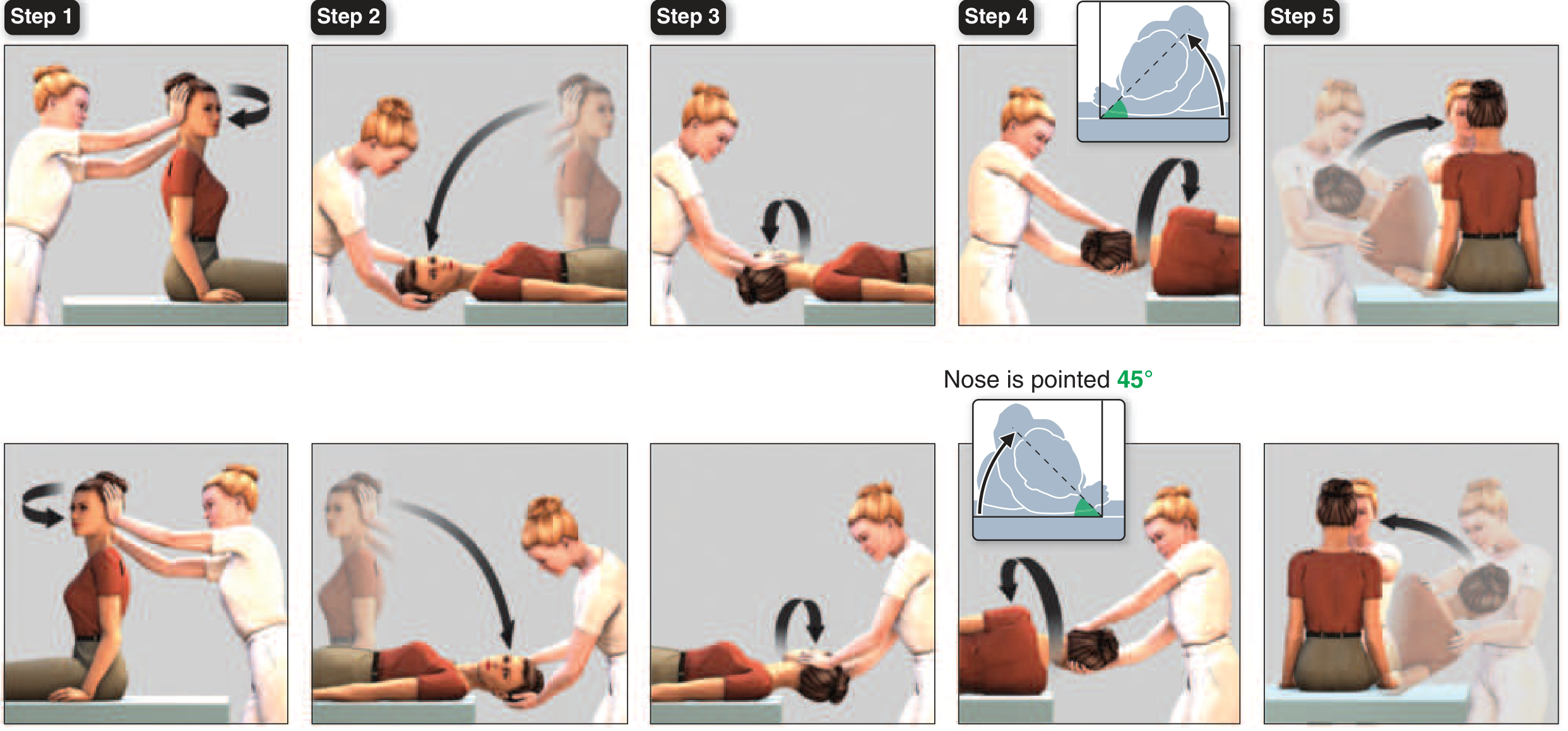
Steps: The patient's head is turned 45° toward the affected ear, then rapidly laid back (head hanging), then head turned 90° to opposite side, then body rolled, then patient sits up — guiding the crystals out of the canal.
2. Vestibular Neuritis
- Sudden acute unilateral vestibular lesion (likely viral, possibly reactivation of herpes simplex)
- Causes: constant vertigo, nausea, vomiting, oscillopsia (visual scene appears to move), imbalance
- Unlike BPPV, vertigo persists even when the head is still
- Represents an acute asymmetry of input from the two labyrinths — the brain interprets this as constant rotation
- Duration: Hours to days
- Nystagmus: Horizontal-torsional, unidirectional, fast phase beating away from the affected ear
- Treatment: Vestibular suppressants acutely (meclizine), then vestibular rehabilitation. Steroids considered. Avoid prolonged suppressant use — it impedes central compensation.
3. Labyrinthitis
- Like vestibular neuritis but also involves cochlear (hearing) function
- Causes: vertigo + sensorineural hearing loss
4. Ménière's Disease (Endolymphatic Hydrops)
- Caused by excess endolymph fluid in the inner ear
- Classic triad: Episodic vertigo + low-frequency hearing loss + tinnitus + ear fullness/pressure
- Attacks last minutes to hours
- Hearing loss is a key distinguishing feature (not seen in BPPV or vestibular neuritis)
- Audiometry shows asymmetric low-frequency hearing loss during attacks
- Treatment: Diuretics + sodium restriction → middle ear injections (steroids or gentamicin) → surgery (endolymphatic sac decompression) if refractory
5. Vestibular Schwannoma (Acoustic Neuroma)
- Slow-growing benign tumor at the cerebellopontine angle, compressing CN VIII
- Causes slowly progressive unilateral sensorineural hearing loss + vestibular hypofunction
- Typically no vertigo — the deficit develops so slowly that the brain compensates as it goes
- Diagnosis: MRI of internal auditory canals
- Head impulse test shows deficient response toward the affected side
6. Bilateral Vestibular Hypofunction
- Both labyrinths lose function (simultaneously or sequentially)
- No vertigo (no asymmetry) — instead: loss of balance, especially in the dark + oscillopsia while walking
- Causes: aminoglycoside ototoxicity (especially gentamicin), neurofibromatosis type 2, autoimmune disease, meningitis, peripheral neuropathy
- Romberg sign positive; bilateral abnormal head impulse test
🟠 B. CENTRAL VESTIBULAR CAUSES (Brainstem / Cerebellum)
These are less common but more dangerous — must always be ruled out.
1. Posterior Circulation Stroke / TIA
- Strokes in the vertebrobasilar territory affect the medulla, pons, midbrain, cerebellum
- May present as isolated acute vertigo — mistaken for peripheral disease
- Key arteries involved:
- PICA (posterior inferior cerebellar artery) — branch of vertebral artery → Wallenberg syndrome
- AICA (anterior inferior cerebellar artery) — branch of basilar artery
- Wallenberg Syndrome (Lateral Medullary Syndrome):
- Vertigo + nausea/vomiting + ataxia
- Loss of pain/temperature on same-side face, opposite-side body
- Hoarseness, dysphagia
- Horner syndrome (ipsilateral ptosis, miosis, anhidrosis)
- A normal head impulse test in a patient with new-onset constant vertigo = red flag for stroke (not peripheral)
2. Vestibular Migraine
- Most common cause of episodic vertigo that is often underdiagnosed
- Vertigo occurs during or (more often) without the headache phase
- Duration: minutes to hours; some patients have prolonged disequilibrium lasting days
- Features: motion sensitivity, sensitivity to visual motion, photophobia, phonophobia, visual aura
- Treatment: Standard migraine prophylaxis medications
3. Multiple Sclerosis (MS)
- Vertigo is the presenting symptom in 7–10% of MS patients; appears in one-third over disease course
- Can cause horizontal, rotary, or vertical nystagmus
- Nystagmus may persist after vertigo resolves
- Key finding: Internuclear ophthalmoplegia (INO) — on lateral gaze, the adducting eye barely moves while the abducting eye moves normally → caused by demyelination of the MLF
4. Cerebellar Hemorrhage
- Medical emergency
- Sudden severe vertigo + severe headache + vomiting + true ataxia (dysmetria)
- May have ipsilateral CN VI palsy
5. Other Central Causes
- Brain tumors (especially posterior fossa)
- Superficial siderosis
- Meningeal infection or tumor
🟡 C. CARDIOVASCULAR / SYSTEMIC CAUSES (Pre-syncope / Near-syncope)
These cause near-syncope dizziness (not true vertigo) — the feeling of faintness from reduced brain blood flow.
| Cause | Mechanism |
|---|---|
| Orthostatic hypotension | Blood pressure drops on standing; brain under-perfused |
| Cardiac arrhythmia | Dysrhythmia reduces cardiac output → reduced cerebral perfusion |
| Vasovagal syncope | Vagal reflex → bradycardia + hypotension |
| Aortic stenosis | Fixed low cardiac output |
| Medications | Antihypertensives, diuretics, vasodilators |
Faintness and syncope should always be considered when evaluating patients with brief dizziness or dizziness that occurs with upright posture.— Harrison's Principles of Internal Medicine 22E
🟢 D. NON-VESTIBULAR NEUROLOGICAL CAUSES
These cause disequilibrium (unsteadiness, not spinning):
- Sensory neuropathy — loss of proprioception in the feet (common in diabetes, B12 deficiency) removes ground-sense input
- Parkinsonism — gait and postural instability
- Cerebellar ataxia — poor pursuit, dysmetric saccades, true limb ataxia
- Normal pressure hydrocephalus — magnetic gait + cognitive decline + urinary incontinence
🔵 E. PSYCHIATRIC / FUNCTIONAL CAUSES
Persistent Postural-Perceptual Dizziness (PPPD)
- Formerly called: phobic postural vertigo, chronic subjective dizziness
- Chronic dizziness persisting after a vestibular, neurological, or psychiatric trigger event
- Aggravated by: upright posture, movement, visual stimuli, complex visual patterns (shopping malls, crowds, movies)
- Not due to ongoing structural vestibular disease — it is a functional neurological disorder
- Strong association with anxiety and panic disorder
- Treatment: vestibular rehabilitation, SSRIs/SNRIs, cognitive behavioral therapy
PART 4: PERIPHERAL vs. CENTRAL VERTIGO — KEY DIFFERENCES
| Feature | Peripheral | Central |
|---|---|---|
| Onset | Sudden | Gradual or sudden |
| Severity | Severe initially, then fades | Mild to severe |
| Duration | Seconds (BPPV) to days (neuritis) | Weeks to months; or brief (TIA) |
| Nystagmus direction | Torsional+upbeat (BPPV); horizontal-torsional (neuritis) | Purely vertical, purely torsional, direction-changing |
| Fixed by head position | Yes (BPPV) | Usually not |
| Neurological signs | None | Usually present (diplopia, ataxia, weakness) |
| Hearing loss | May be present | Usually absent (unless near CN VIII entry) |
| Head impulse test | Abnormal (catch-up saccade) | Normal → red flag |
| Nystagmus suppressed by fixation? | Yes | No |
PART 5: NYSTAGMUS — THE CARDINAL SIGN
Nystagmus = involuntary rhythmic eye movements.
- Slow phase: drift of eyes toward the side of the lesion (vestibular drive)
- Fast phase (quick phase): rapid saccadic correction back to midline (cortical reset)
- Direction named by fast phase (by convention)
Types:
- Unidirectional horizontal: peripheral lesion (fast phase beats away from the sick ear)
- Direction-changing with gaze: central lesion
- Downbeat nystagmus (fast phase toward nose): cerebellar pathway lesion
- Vertical/torsional at rest: central lesion
- Mixed vertical-torsional, transient: BPPV (posterior canal)
Caloric Testing (COWS mnemonic):
- Cold water → nystagmus to Opposite side
- Warm water → nystagmus to Same side
- If nystagmus is reduced/absent on one side → vestibular lesion on that side
PART 6: CLINICAL APPROACH — 3 KEY QUESTIONS
When a patient presents with dizziness, ask:
- Is it dangerous? (arrhythmia? TIA/stroke?)
- Is it vestibular?
- If vestibular — is it peripheral or central?
Timing & Triggers Framework (Most Useful Clinically):
| Pattern | Think of... |
|---|---|
| Seconds, triggered by head position | BPPV |
| Minutes, spontaneous, recurrent | Vestibular migraine, TIA, Ménière's |
| Hours, recurrent with hearing symptoms | Ménière's disease |
| Constant, days to weeks, first episode | Vestibular neuritis vs. posterior fossa stroke |
| Chronic, worsens with movement/crowds | PPPD |
| On standing up | Orthostatic hypotension |
PART 7: IMPORTANT CLINICAL SIGNS (HINTS Exam)
HINTS = Head Impulse test, Nystagmus pattern, Test of Skew
Used at the bedside in patients with acute constant vertigo to differentiate stroke from vestibular neuritis:
| Test | Peripheral (Safe) | Central (Dangerous) |
|---|---|---|
| Head Impulse | Abnormal (catch-up saccade) | Normal |
| Nystagmus | Unidirectional | Direction-changing |
| Skew deviation | Absent | Present (vertical eye misalignment) |
A normal head impulse test in a patient with new-onset constant vertigo is a red flag for a central (stroke) cause — the absence of a catch-up saccade means the vestibular nerve is intact, and the lesion is likely central.
PART 8: TREATMENT OVERVIEW
| Condition | Treatment |
|---|---|
| BPPV | Epley maneuver (repositioning); no medications needed |
| Vestibular neuritis | Meclizine/antihistamines (short-term only); vestibular rehab; consider steroids |
| Ménière's disease | Diuretics + low-sodium diet; middle ear injections; surgery if refractory |
| Vestibular migraine | Migraine prophylaxis (beta-blockers, amitriptyline, valproate) |
| Posterior fossa stroke | Emergent imaging + stroke protocol |
| Bilateral vestibulopathy | Vestibular rehabilitation; stop offending drugs |
| PPPD | SSRIs/SNRIs + CBT + vestibular rehab |
| Orthostatic hypotension | Hydration, compression stockings, fludrocortisone, midodrine |
Vestibular suppressant medications should be avoided beyond the first few days in vestibular neuritis — they interfere with central compensation and recovery.— Harrison's Principles of Internal Medicine 22E
SUMMARY: Every System That Can Make You Dizzy
INNER EAR → BPPV, vestibular neuritis, Ménière's, labyrinthitis, schwannoma
VESTIBULAR NERVE → Schwannoma, neuritis, ototoxicity
BRAINSTEM/PONS → Stroke (AICA/PICA), MS, Wallenberg syndrome
CEREBELLUM → Hemorrhage, infarct, tumor, ataxia
CORTEX/MIGRAINE → Vestibular migraine, PPPD
EYES → Diplopia (breaks visual-vestibular match)
PROPRIOCEPTION → Sensory neuropathy (DM, B12 deficiency)
HEART → Arrhythmia, orthostatic hypotension, aortic stenosis
BLOOD VESSELS → Vertebrobasilar insufficiency (TIA/stroke)
PSYCHOLOGY → Anxiety, panic disorder, PPPD
MEDICATIONS → Antihypertensives, aminoglycosides, anticonvulsants, alcohol
This is the full picture of dizziness from inner ear to heart and mind. Let me know if you want any section expanded — for example, a deeper dive into Ménière's, the full Epley maneuver steps, HINTS bedside exam, or management of specific conditions.
Provide me full details tests and results WRITE by neurologist medicine dr and neurootologist and ENTS
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
Dix-Hallpike test positional vertigo BPPV nystagmus
Excellent — I now have rich, detailed content from Harrison's, Rosen's Emergency Medicine, and Cummings Otolaryngology. Let me now compile the full, comprehensive reference document.
📋 Complete Vestibular Testing Guide
Written from the Perspective of Neurology, Neuro-Otology & ENT/Otolaryngology
Sources: Harrison's Principles of Internal Medicine 22E | Rosen's Emergency Medicine | Cummings Otolaryngology Head & Neck Surgery | Ganong's Physiology
INTRODUCTION — Why Testing Matters
The vestibular system cannot be examined directly like the skin or the eye. Its function must be inferred through a structured series of bedside tests, provocative maneuvers, and laboratory investigations. The purpose of vestibular testing is threefold:
- Site-of-lesion localization — peripheral (inner ear / CN VIII) vs. central (brainstem / cerebellum)
- Functional assessment — how well is the patient using their remaining vestibular function?
- Compensation status — is the brain adapting to the deficit or not?
No single test is sufficient. The vestibular test battery must be interpreted in light of the full history, symptom duration, and medical background of the patient.— Cummings Otolaryngology
═══════════════════════════════════════════
SECTION A — BEDSIDE CLINICAL EXAMINATION
═══════════════════════════════════════════
(Performed by Neurologist, Neuro-Otologist, ENT)
🔵 TEST 1: SPONTANEOUS NYSTAGMUS OBSERVATION
What it is: Observing for involuntary rhythmic eye movements while the patient looks straight ahead, then in different directions of gaze.
How it is done:
- Examine first with Frenzel goggles (self-illuminated magnifying goggles that prevent visual fixation) or infrared video goggles — these prevent fixation suppression of peripheral nystagmus
- Observe the eyes in primary gaze, then lateral gaze (left and right), then vertical (up and down)
What to look for and interpret:
| Nystagmus Pattern | Interpretation |
|---|---|
| Unidirectional horizontal, suppressed by fixation | Peripheral (fast phase away from the damaged ear) |
| Direction-changing on lateral gaze | Central lesion |
| Purely vertical (downbeat or upbeat) | Central (cerebellar pathways) |
| Purely torsional at rest | Central |
| Mixed vertical + torsional, brief, triggered by position | BPPV (posterior canal) |
| Horizontal, not suppressed by fixation | Central or vestibular neuritis acute phase |
Peripheral nystagmus is inhibited by visual fixation. Central nystagmus is not. This is a key distinguishing feature. — Harrison's Principles of Internal Medicine 22E
Abnormal nystagmus is the cardinal sign of inner ear disease and the principal objective evidence of vestibular dysfunction. — Rosen's Emergency Medicine
🔵 TEST 2: HEAD IMPULSE TEST (HIT) / HEAD THRUST TEST
Also called: Vestibulo-Ocular Reflex (VOR) Test at high velocity
What it tests: Integrity of the VOR — specifically the high-velocity response of the horizontal semicircular canals
How it is done:
- Examiner stands face-to-face with the patient
- Both hands placed on either side of the patient's head
- Patient fixates on the examiner's nose
- Head is rapidly (unexpectedly) rotated ~10–20° to one side at high velocity (~1000–4000°/s/s)
- Observe whether the eyes stay on target or slip with the head
Results:
| Finding | Meaning |
|---|---|
| Normal: Eyes stay fixed on target throughout | VOR intact → suggests central lesion if patient has acute vertigo |
| Abnormal (Positive test): Eyes slip with the head, then a "catch-up saccade" brings gaze back | VOR deficient → suggests peripheral vestibular hypofunction on the side you turned toward |
If the head impulse test is normal in a patient with acute constant vertigo, a peripheral lesion is unlikely. A central cause (stroke) must be considered. — Harrison's Principles of Internal Medicine 22E
Eliciting a positive head impulse test indicates a benign peripheral cause such as vestibular neuritis. — Rosen's Emergency Medicine
Important caveat: The head must be turned rapidly enough — a slow turn gives a false-negative result, which would incorrectly suggest a central cause.
🔵 TEST 3: DIX-HALLPIKE MANEUVER (Hallpike / Nylen-Barany Test)
Used by: ENT, Neuro-Otologist, Neurologist
Diagnoses: Posterior canal BPPV (most common BPPV variant)
How it is done:
- Patient sits upright on examination table
- Examiner turns patient's head 45° toward the side being tested
- Patient is rapidly moved from sitting → supine with head hanging over edge of table (~20–30° below horizontal)
- Eyes are observed carefully for nystagmus after a brief latency period
- Patient is brought back to sitting; test repeated to the other side
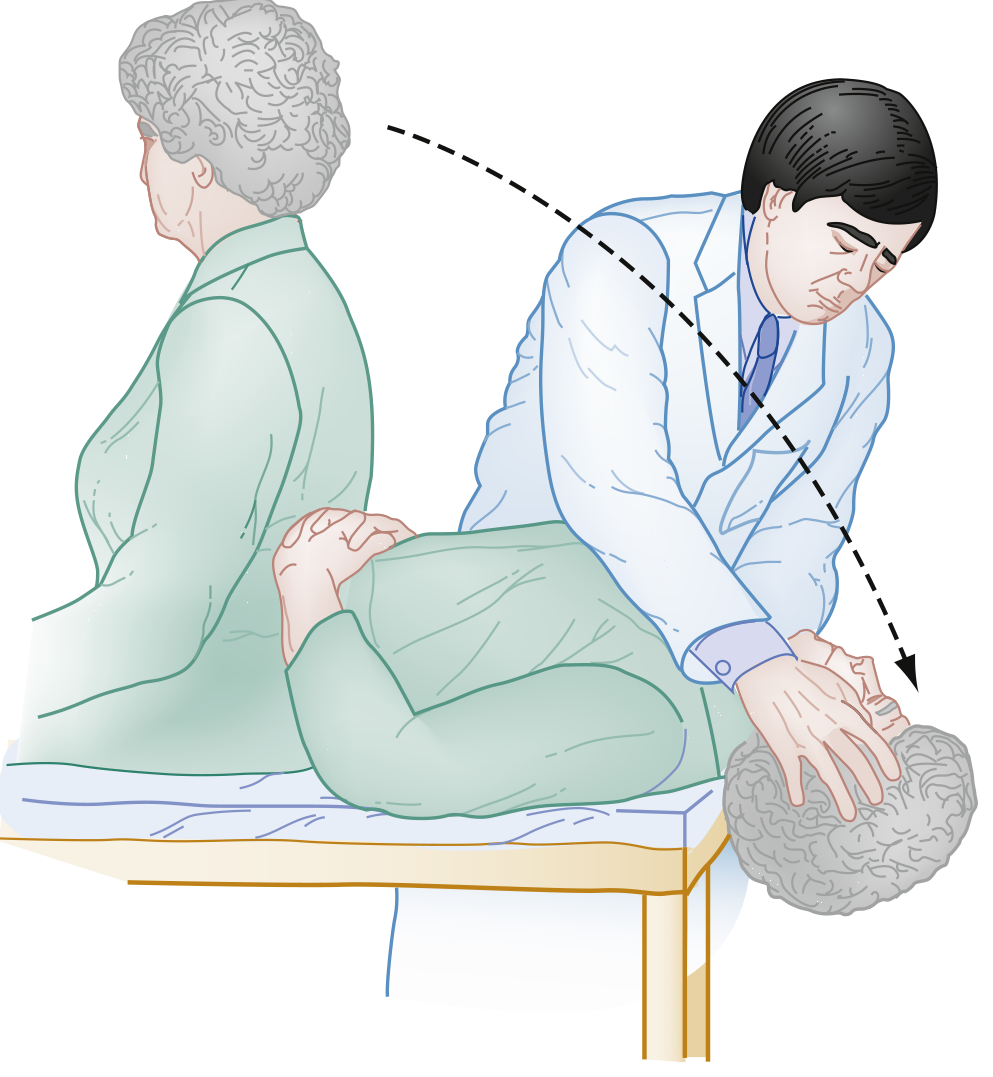
Classic Positive Findings for Posterior Canal BPPV:
| Feature | What You See |
|---|---|
| Latency | Nystagmus begins after 3–10 seconds (up to 30s on rare occasions) |
| Direction of nystagmus | Upbeat (fast phase toward forehead) + torsional (top poles of eyes beating toward the downward/affected ear) |
| Duration | Vertigo + nystagmus last 5–30 seconds, then slowly resolve |
| Buildup then fade | Intensity escalates then diminishes |
| Reversal on sitting up | Nystagmus briefly reverses direction when patient returns to sitting |
| Fatigability | Nystagmus decreases with repeated testing |
Interpretation:
- Positive on one side only: The downward ear = the affected side → start treatment on that side
- Nystagmus persisting >90 seconds: Consider central positional nystagmus (fixed otolith lesion or CNS pathology)
- If both sides seem positive: may have bilateral BPPV; repeat carefully
When NOT to perform Dix-Hallpike:
- Patient with acute vestibular syndrome (constant vertigo at rest) — this is inconsistent with BPPV; provocative testing may worsen symptoms and mislead diagnosis
Clinicians should diagnose posterior semicircular canal BPPV when vertigo associated with torsional, upbeating nystagmus is provoked by the Dix-Hallpike maneuver. This is a strong recommendation in clinical guidelines.
🔵 TEST 4: SUPINE ROLL TEST (Log Roll / Pagnini-McClure Test)
Diagnoses: Horizontal (lateral) canal BPPV
When to use: If Dix-Hallpike is negative or shows horizontal-only nystagmus
How it is done:
- Patient lies supine (face up)
- Head rapidly rolled 30° to the right → observe nystagmus
- Return to neutral; then head rapidly rolled 30° to the left → observe nystagmus
Results:
| Pattern | Interpretation |
|---|---|
| Geotropic (nystagmus beats toward the floor/ground) on BOTH sides, but stronger on one side | Horizontal canal BPPV — affected ear is the side with STRONGER nystagmus |
| Apogeotropic (nystagmus beats toward ceiling) on both sides | Horizontal canal BPPV (cupulolithiasis variant) |
🔵 TEST 5: HINTS EXAMINATION (Bedside Stroke Screen)
Full name: Head Impulse, Nystagmus, Test of Skew
Used in: Acute vestibular syndrome (constant vertigo, first episode, lasting >24h)
Purpose: Differentiate posterior fossa stroke from benign vestibular neuritis at the bedside
The three components:
Component 1 — Head Impulse Test (H)
| Result | Interpretation |
|---|---|
| Positive (catch-up saccade) | Peripheral (VOR impaired) → suggests vestibular neuritis |
| Negative (no saccade) | Red flag → central cause (stroke) |
Component 2 — Nystagmus Pattern (N)
| Result | Interpretation |
|---|---|
| Unidirectional horizontal | Peripheral |
| Direction-changing with gaze | Central (stroke) |
Component 3 — Test of Skew (T)
- Perform alternate cover test: alternately cover each eye while patient fixates on a target
- Look for vertical realignment of the uncovered eye
| Result | Interpretation |
|---|---|
| No skew deviation | Peripheral |
| Skew deviation present (vertical misalignment) | Brainstem stroke |
HINTS pattern interpretation:
| HINTS Pattern | Likely Diagnosis |
|---|---|
| Abnormal HIT + Unidirectional nystagmus + No skew | Peripheral (vestibular neuritis — relatively safe) |
| Normal HIT + Direction-changing nystagmus + Skew present | Central (stroke) — imaging urgently |
HINTS should only be used in patients with a first-ever episode of constant vertigo (acute vestibular syndrome) — not in episodic or positional vertigo. It requires experience to perform correctly. — Rosen's Emergency Medicine
🔵 TEST 6: ROMBERG TEST
Tests: Postural control and proprioceptive contribution to balance
How it is done:
- Patient stands with feet together, hands crossed over chest
- Eyes open first → then eyes closed
- Observe for excessive sway or falling
Results:
| Finding | Meaning |
|---|---|
| Sways/falls with eyes closed but not open | Positive Romberg = sensory deficit (vestibular, cerebellar, OR proprioceptive) |
| Falls with eyes open | Cerebellar ataxia (does not improve with vision) |
| Falls with eyes closed, toward affected side | Suggests unilateral peripheral vestibular weakness |
This test does not localize the lesion — vestibular deficits, cerebellar lesions, and peripheral neuropathy can all cause a positive Romberg. — Cummings Otolaryngology
🔵 TEST 7: FUKUDA STEPPING TEST (Unterberger Test)
Tests: Peripheral labyrinthine function (unilateral)
How it is done:
- Patient marches in place for 50 steps, eyes closed, arms outstretched
- Observe for rotation (turning clockwise or counterclockwise)
Results:
| Finding | Meaning |
|---|---|
| Rotation >30–45° | Positive — suggests ipsilateral peripheral labyrinthine weakness |
| Direction of rotation | Does not indicate which side is affected (both can cause either direction) |
Limitations: Does not distinguish compensated from uncompensated lesions. Remains positive long after central compensation. Most sensitive for severe or profound unilateral dysfunction.
🔵 TEST 8: OCULAR MOTILITY EXAMINATION
(Neurologist-focused)
What is assessed:
| Test | How | Abnormal Finding | Implication |
|---|---|---|---|
| Range of motion | Follow finger in H-pattern | Restricted, disconjugate | CN III, IV, or VI palsy |
| Smooth pursuit | Follow slowly moving target | Catch-up saccades, broken pursuit | Central (cerebellar) pathology |
| Saccades | Rapid alternating gaze between two targets | Dysmetria (over/undershoot) | Cerebellar lesion |
| Cover test | Alternate cover while fixating | Vertical misalignment (skew deviation) | Brainstem/cerebellar lesion |
| Gaze-evoked nystagmus | Hold gaze at extremes of horizontal/vertical | Direction-changes with gaze direction | Central |
| Downbeat nystagmus | Observe in primary gaze | Fast phase beats toward nose | Cerebellar flocculus lesion |
| Internuclear ophthalmoplegia (INO) | Lateral gaze | Adducting eye lags, abducting eye has nystagmus | MLF lesion → MS |
INO (adducting eye weak + abducting eye nystagmus) is virtually pathognomonic of multiple sclerosis affecting the brainstem. — Rosen's Emergency Medicine
🔵 TEST 9: DYNAMIC VISUAL ACUITY (DVA) TEST
Tests: Functional integrity of the VOR during head movement
How it is done:
- Patient reads an eye chart first with head still (static acuity)
- Then patient tries to read while head is oscillated by the examiner (or self)
- Loss of >2 lines of acuity during head movement = abnormal
Result: Quantifies how well the VOR maintains stable vision during movement. Reduced DVA confirms VOR dysfunction and is especially useful for monitoring vestibular rehabilitation progress.
🔵 TEST 10: CEREBELLAR FUNCTION TESTS
(Adjuncts used by neurologists to exclude cerebellar pathology)
| Test | Abnormal Finding | Meaning |
|---|---|---|
| Finger-nose-finger | Past-pointing, tremor, dysmetria | Cerebellar disease |
| Rapid alternating movements (dysdiadochokinesia) | Irregular, slow | Cerebellar |
| Heel-to-shin test | Deviation off shin | Cerebellar |
| Tandem gait | Cannot walk heel-to-toe | Cerebellar or vestibular |
| Wide-based gait | Broad base, lurching | Cerebellar ataxia |
🔵 TEST 11: ORTHOSTATIC VITAL SIGNS
(Used when near-syncope is a component of dizziness)
How it is done: Blood pressure and heart rate measured lying → sitting → standing
Positive finding (Orthostatic Hypotension):
- Systolic BP drop ≥20 mmHg OR diastolic drop ≥10 mmHg within 3 minutes of standing
- Often accompanied by symptoms of lightheadedness or near-faint
═══════════════════════════════════════════
SECTION B — ENT / OTOSCOPY EXAMINATION
═══════════════════════════════════════════
(Performed by ENT Surgeon / Otolaryngologist)
🟢 TEST 12: OTOSCOPY
What it examines: External ear canal + tympanic membrane
| Finding | Clinical Significance |
|---|---|
| Cerumen impaction / foreign body | Can cause mild vertigo |
| Fluid in middle ear (effusion) | Otitis media → mild vertigo |
| Perforated/scarred tympanic membrane | May indicate perilymphatic fistula (especially with prior trauma) |
| Vesicles on pinna/ear canal | Ramsay Hunt syndrome (herpes zoster oticus) — vertigo + facial palsy + hearing loss |
| Cholesteatoma | Erosive middle ear disease — can involve semicircular canal |
🟢 TEST 13: TUNING FORK TESTS
(Gross screening for hearing loss type — conductive vs. sensorineural)
Weber Test
- 512 Hz tuning fork placed on the midline of skull (forehead or vertex)
- Ask: "Does the sound go to one side or stay in the middle?"
| Result | Interpretation |
|---|---|
| Lateralizes to the symptomatic ear | Conductive hearing loss on that side |
| Lateralizes to the opposite ear | Sensorineural hearing loss on the symptomatic side |
| Central (equal both sides) | Normal or symmetric |
Rinne Test
- Fork placed on mastoid bone (bone conduction) → when no longer heard, moved to external ear (air conduction)
| Result | Interpretation |
|---|---|
| AC > BC (positive Rinne) | Normal or sensorineural hearing loss |
| BC > AC (negative Rinne) | Conductive hearing loss |
═══════════════════════════════════════════
SECTION C — LABORATORY / ANCILLARY TESTS
═══════════════════════════════════════════
(Ordered by Neurologist / Neuro-Otologist / ENT based on clinical suspicion)
🟡 TEST 14: PURE TONE AUDIOMETRY (PTA)
The foundational hearing test — should be done in ALL patients with suspected vestibular disorder
What it measures: Air and bone conduction thresholds at frequencies 250 Hz – 8000 Hz
How to read the audiogram:
| Pattern | Suggests |
|---|---|
| Unilateral sensorineural hearing loss (SNHL) | Vestibular schwannoma (acoustic neuroma), labyrinthitis, Ménière's |
| Low-frequency SNHL (worse at 250–1000 Hz) | Ménière's disease (characteristic) |
| High-frequency SNHL | Noise-induced hearing loss, presbycusis, aminoglycoside ototoxicity |
| Conductive hearing loss | Middle ear disease, otosclerosis |
| Bilateral SNHL | Bilateral vestibulopathy, autoimmune inner ear disease |
Audiometry should be performed whenever a vestibular disorder is suspected. Unilateral SNHL supports a peripheral vestibular disorder such as vestibular schwannoma. — Harrison's Principles of Internal Medicine 22E
🟡 TEST 15: VIDEONYSTAGMOGRAPHY (VNG) / ELECTRONYSTAGMOGRAPHY (ENG)
The gold standard laboratory vestibular test battery
What it does: Records eye movements using infrared video cameras worn as goggles, under multiple conditions
Subtests included:
a) Spontaneous Nystagmus Recording
- Eyes open in darkness (goggles eliminate fixation)
- Identifies residual spontaneous nystagmus not visible at bedside
- Clinically significant spontaneous nystagmus suggests incomplete compensation or active peripheral lesion
b) Positional Nystagmus Testing
- Patient moved into various positions (supine, left lateral, right lateral, Hallpike positions)
- Records nystagmus characteristics in each position
- Differentiates BPPV from other positional disorders
c) Caloric Testing — THE KEY VNG SUBTEST
Isolates and compares each horizontal semicircular canal independently
How it is done:
- Warm water (44°C) and cold water (30°C) are instilled into each external ear canal, one at a time (4 irrigations total)
- Temperature difference sets up convection currents in the endolymph → stimulates the horizontal canal
- Resulting nystagmus is recorded
COWS Mnemonic: Cold = Opposite side nystagmus; Warm = Same side nystagmus
What is measured and interpreted:
| Measurement | What It Means |
|---|---|
| Unilateral Weakness (UW) | If one ear's response is <25% of the other's — canal paresis on that side → peripheral lesion (vestibular neuritis, Ménière's, schwannoma) |
| Directional Preponderance (DP) | Asymmetry between responses beating left vs. right → indicates ongoing vestibular imbalance |
| Bilateral Weakness | Both ears hypo-responsive → bilateral vestibular hypofunction |
| Normal caloric responses | Horizontal canal function intact bilaterally |
Limitations: Tests only the low-frequency range of the horizontal canal; does not test vertical canals.
🟡 TEST 16: VIDEO HEAD IMPULSE TEST (vHIT / VHIT)
The modern high-tech version of the bedside head impulse test
How it works:
- High-speed infrared camera (250–500 fps) tracks eye movements during rapid passive head rotations in all 6 canal planes
- Computer measures VOR gain (eye velocity / head velocity ratio)
- Detects both overt saccades (visible, after head stops) and covert saccades (during head movement — only detectable by machine)
Normal VOR gain: ~1.0 (eyes move exactly opposite to the head)
| Finding | Interpretation |
|---|---|
| Reduced gain (<0.8) + catch-up saccades on one side | Unilateral canal hypofunction |
| Reduced gain bilaterally | Bilateral vestibular hypofunction |
| Normal gain in all 6 canals | Peripheral lesion unlikely; central cause suspected |
| Covert saccades only | Early/partial peripheral lesion with partial compensation |
vHIT is being utilized in emergency departments as part of a clinical algorithm to distinguish central causes of acute vestibular syndrome from peripheral causes. It expands caloric testing by covering all six semicircular canals. — Cummings Otolaryngology
🟡 TEST 17: ROTARY CHAIR TESTING (Rotational Chair)
What it does: Stimulates both horizontal semicircular canals simultaneously across a wide range of frequencies and head velocities — the only test that evaluates low-frequency vestibular function bilaterally at once
How it works:
- Patient sits in a motorized chair in complete darkness, rotating at various speeds and frequencies
- VOR is measured: gain (amplitude), phase (timing lag), and symmetry
Results interpreted:
| Finding | Meaning |
|---|---|
| Reduced VOR gain bilaterally | Bilateral vestibular hypofunction |
| Phase lead (eyes move before expected) | Peripheral vestibular loss |
| Asymmetry (directional preponderance) | Uncompensated unilateral peripheral lesion — vestibular system still generating an asymmetric signal |
| Normal rotational responses | Peripheral vestibular hypofunction less likely |
Persistent asymmetry (bias) in slow-phase eye velocity responses during rightward vs. leftward rotation strongly suggests the peripheral lesion is physiologically uncompensated. — Cummings Otolaryngology
Advantage over caloric: Tests the low-frequency VOR that caloric testing cannot reach; especially useful for bilateral vestibular loss.
🟡 TEST 18: VESTIBULAR EVOKED MYOGENIC POTENTIALS (VEMP)
Tests the otolith organs (saccule and utricle) — something caloric testing cannot do
a) Cervical VEMP (cVEMP) — Tests the SACCULE
How it works:
- Patient turns head to one side (activating the sternocleidomastoid / SCM muscle)
- Loud clicks (95–105 dB) delivered to the ear via headphones
- SCM muscle EMG is recorded
- Normally: an inhibitory potential at 13 ms followed by excitatory potential at 21 ms after the stimulus
| Finding | Meaning |
|---|---|
| Normal bilateral cVEMP | Saccular and inferior vestibular nerve pathways intact |
| Absent or reduced amplitude ipsilaterally | Saccular dysfunction (inferior vestibular nerve loss) |
| Enhanced amplitude (increased in one ear) | Ménière's disease (endolymphatic hydrops — classic pattern) |
| Absent bilaterally | Bilateral saccular dysfunction or bilateral vestibulopathy |
b) Ocular VEMP (oVEMP) — Tests the UTRICLE
How it works:
- Loud clicks delivered; small electrodes under the eyes record the response from the contralateral inferior oblique and inferior rectus muscles
- Normal: excitatory potential at 10 ms, inhibitory potential at 16 ms
| Finding | Meaning |
|---|---|
| Normal bilateral oVEMP | Utricular and superior vestibular nerve pathways intact |
| Absent contralateral oVEMP | Utricular dysfunction |
| Enhanced oVEMP amplitude | Ménière's disease / endolymphatic hydrops |
Clinical value of VEMP:
- Helps localize lesion to inferior vs. superior vestibular nerve division
- Detects otolith organ dysfunction missed by caloric/rotary chair
- Particularly useful in diagnosing Ménière's disease and superior semicircular canal dehiscence (SSCD)
🟡 TEST 19: DYNAMIC POSTUROGRAPHY (Computerized Dynamic Posturography / CDP)
Tests: Functional use of all three balance systems (vestibular, visual, proprioceptive) in an integrated way
How it works:
The patient stands on a force platform that can tilt and sway. Vision is altered by a moving screen. The test is divided into the Sensory Organization Test (SOT) with 6 conditions:
| Condition | Surface | Vision | What It Tests |
|---|---|---|---|
| 1 | Fixed | Eyes open | Baseline (all systems available) |
| 2 | Fixed | Eyes closed | Somatosensory + vestibular (vision removed) |
| 3 | Fixed | Moving visual scene | Vestibular + somatosensory (visual conflict) |
| 4 | Sway-referenced | Eyes open | Visual + vestibular (proprioception disrupted) |
| 5 | Sway-referenced | Eyes closed | Vestibular only (most sensitive for vestibular loss) |
| 6 | Sway-referenced | Moving visual scene | Vestibular (all other inputs unreliable) |
Results:
| Finding | Meaning |
|---|---|
| Fails conditions 5 and 6 | Vestibular dysfunction (can't use vestibular input) |
| Fails conditions 3 and 6 | Visual dependence (ignores vestibular/proprioceptive input) |
| Fails conditions 2, 3, 5, 6 | Somatosensory dysfunction (peripheral neuropathy) |
| Normal overall | Compensation complete; functional balance restored |
Dynamic posturography provides information about balance system function that is not available through other vestibular testing modalities. It is primarily a test of functional capability rather than site-of-lesion evaluation. — Cummings Otolaryngology
🟡 TEST 20: ELECTROCOCHLEOGRAPHY (ECoChG)
Used by: ENT / Neuro-Otologist for Ménière's disease diagnosis
What it tests: Electrical potentials generated by the cochlea in response to sound stimuli; measures endolymphatic hydrops
Key measurement: The SP/AP ratio (Summating Potential / Action Potential ratio)
| SP/AP Ratio | Interpretation |
|---|---|
| ≤0.4 | Normal |
| >0.4 (elevated) | Suggests endolymphatic hydrops → Ménière's disease |
An elevated SP/AP ratio is the electrophysiologic signature of excessive endolymph pressure distorting the basilar membrane.
🟡 TEST 21: AUDITORY BRAINSTEM RESPONSE (ABR / BAER)
Used by: ENT, Audiologist, Neurologist
What it tests: Integrity of the auditory pathway from cochlea → CN VIII → brainstem
How it works: Clicks delivered through headphones; electrodes on scalp record 5 waves (Waves I–V) representing successive relay stations:
- Wave I = cochlear nerve
- Wave III = cochlear nucleus / pons
- Wave V = inferior colliculus
What to look for:
| Finding | Interpretation |
|---|---|
| Prolonged Wave I–III interwave latency | CN VIII / retrocochlear lesion → vestibular schwannoma |
| Prolonged Wave III–V interwave latency | Brainstem lesion |
| Absent or abnormal waves (asymmetric) | Retrocochlear pathology — warrants MRI |
| Normal ABR | Cochlear cause more likely |
🟡 TEST 22: OTOACOUSTIC EMISSIONS (OAEs)
Used by: ENT / Audiologist
What it tests: Outer hair cell function of the cochlea
- Transient OAEs (TEOAEs): Presence indicates outer hair cells are functioning; absent in hearing loss >30 dB
- Distortion Product OAEs (DPOAEs): Provides frequency-specific information
In vestibular context: Normal OAEs with abnormal ABR = retrocochlear (CN VIII) lesion → suspect schwannoma. Absent OAEs = cochlear dysfunction.
═══════════════════════════════════════════
SECTION D — NEUROIMAGING
═══════════════════════════════════════════
🔴 TEST 23: MRI BRAIN WITH GADOLINIUM (Internal Auditory Canals)
Indications:
- Unexplained unilateral sensorineural hearing loss
- Unexplained unilateral vestibular hypofunction
- Suspected vestibular schwannoma (acoustic neuroma)
- Central vestibular syndrome suspected (abnormal HINTS, direction-changing nystagmus, neurological signs)
- Posterior fossa lesion suspected
What MRI shows:
| Finding | Diagnosis |
|---|---|
| Enhancing mass in internal auditory canal/CP angle | Vestibular schwannoma |
| DWI restriction in posterior fossa (brainstem/cerebellum) | Acute stroke (most critical — rule out in acute vestibular syndrome) |
| Periventricular white matter lesions | Multiple sclerosis |
| Cerebellar atrophy | Cerebellar degeneration |
| Hemorrhage or mass in cerebellum | Cerebellar hemorrhage / tumor |
MRI is the diagnostic modality of choice for posterior fossa lesions, as well as for vestibular schwannoma and MS. Gadolinium contrast is required to detect schwannomas. — Rosen's Emergency Medicine
Important: CT scan has poor sensitivity for posterior fossa strokes (up to 20% of posterior fossa strokes are missed on early CT). MRI-DWI is the gold standard for ruling out posterior fossa ischemia.
🔴 TEST 24: CT SCAN OF TEMPORAL BONE
Ordered by ENT — not for stroke but for structural ear disease
Indications:
| Indication | What CT Shows |
|---|---|
| Suspected cholesteatoma | Erosion of ossicles, mastoid, semicircular canals |
| Superior semicircular canal dehiscence (SSCD) | Thinning/absence of bone over superior canal |
| Temporal bone fracture | Fracture lines; labyrinthine involvement |
| Chronic otitis media | Middle ear opacification, mastoid disease |
| Otosclerosis | Lucency around cochlea (Halos sign) |
Superior canal dehiscence (absence of overlying bone on the superior semicircular canal) causes a unique syndrome: vertigo triggered by loud sounds (Tullio phenomenon) or pressure changes, plus low-frequency conductive hearing loss with normal tympanograms.
═══════════════════════════════════════════
SECTION E — BLOOD AND ROUTINE LABORATORY TESTS
═══════════════════════════════════════════
(Used to exclude systemic causes of dizziness)
| Test | Indication | What It Finds |
|---|---|---|
| Finger-stick blood glucose | Immediate — every vertiginous patient | Hypoglycemia mimicking dizziness |
| CBC (Full blood count) | Lightheadedness, fatigue | Anemia as cause |
| Electrolytes, BUN, creatinine | Dehydration, medication effects | Hyponatremia, dehydration |
| ECG | Pre-syncopal dizziness | Arrhythmia, QT prolongation, ST changes |
| TSH | Fatigue, dizziness, balance issues | Hypothyroidism |
| ANA, ANCA, anti-dsDNA | Bilateral sensorineural hearing loss + vestibular loss | Autoimmune inner ear disease |
| FTA-ABS or RPR (syphilis serology) | Bilateral fluctuating hearing/vestibular loss | Neurosyphilis |
| Vitamin B12 level | Disequilibrium with neuropathy | B12 deficiency neuropathy affecting proprioception |
| Lipid panel, HbA1c, coagulation | TIA/stroke risk assessment | Cardiovascular risk factors |
═══════════════════════════════════════════
SECTION F — COMPLETE TEST RESULT SUMMARY TABLE
═══════════════════════════════════════════
| Test | Normal Result | Peripheral Vestibular | Central Vestibular |
|---|---|---|---|
| Spontaneous Nystagmus | None | Unidirectional horizontal; suppressed by fixation | Direction-changing; not suppressed; purely vertical/torsional |
| Head Impulse Test | No catch-up saccade | Positive (saccade present) | Negative (no saccade) — red flag |
| Dix-Hallpike | No nystagmus | Upbeat + torsional, latency 3–10s, fatigable <30s | No latency, no fatigue, purely vertical/torsional |
| HINTS | — | Positive HIT + unidirectional nystagmus + no skew | Normal HIT + direction-changing + skew = STROKE |
| Romberg | Stable | Falls toward affected side | May fall any direction |
| Caloric Testing | Symmetric responses | Unilateral canal paresis (UW >25%) | May be normal bilaterally |
| vHIT | VOR gain ~1.0 bilaterally | Reduced gain + covert/overt saccades unilateral | Normal gain with vertigo = suspect central |
| Rotary Chair | Normal gain, phase, symmetry | Phase lead, reduced gain; asymmetry if uncompensated | Variable |
| cVEMP | Present bilaterally, normal latency | Absent ipsilateral | May be normal |
| Audiometry | Bilateral symmetric thresholds | Unilateral SNHL (schwannoma); low-frequency SNHL (Ménière's) | Usually normal unless near CN VIII entry zone |
| ECoChG SP/AP | ≤0.4 | Elevated >0.4 in Ménière's | — |
| ABR | Symmetric interwave latencies | Prolonged I–III latency (schwannoma) | Prolonged III–V (brainstem) |
| MRI brain | No lesion | Enhancing mass in IAC | Infarct, hemorrhage, MS plaques |
STANDING ALGORITHM — Emergency / Clinical Decision
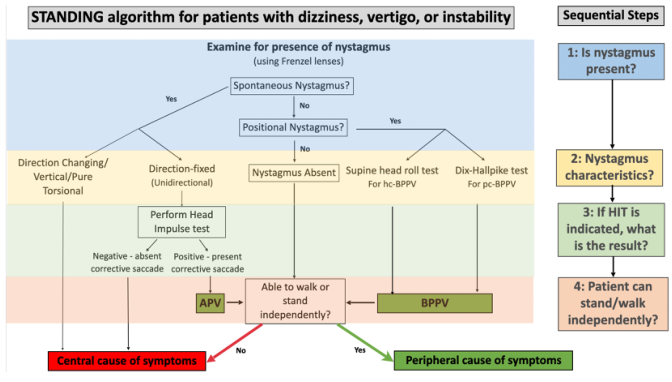
Step-by-step at the bedside:
- Is nystagmus present? (use Frenzel goggles)
- Direction-changing / vertical / pure torsional → Central (stop, image)
- Unidirectional → proceed to Step 2
- Head Impulse Test
- Positive (saccade) + unidirectional nystagmus → Peripheral (vestibular neuritis)
- Negative (no saccade) + any nystagmus → Central (stroke)
- Can patient walk/stand independently?
- No → Central until proven otherwise
- Yes + peripheral signs → Peripheral vestibular cause
QUICK REFERENCE: WHICH TEST FOR WHICH CONDITION
| Suspected Condition | First-Line Tests | Confirmatory Tests |
|---|---|---|
| BPPV | Dix-Hallpike, Supine Roll Test | Clinical — no lab needed |
| Vestibular neuritis | HIT, HINTS, VNG caloric | MRI to exclude stroke |
| Ménière's disease | Audiometry (low-frequency SNHL) | ECoChG (SP/AP >0.4); enhanced cVEMP |
| Vestibular schwannoma | Audiometry (asymmetric SNHL); ABR | MRI with gadolinium (definitive) |
| Posterior fossa stroke | HINTS exam | MRI-DWI (gold standard) |
| Multiple sclerosis | Ocular motility (INO); ABR | MRI brain (periventricular lesions) |
| Bilateral vestibulopathy | Bilateral caloric, vHIT | Rotary chair; DVA testing |
| Autoimmune inner ear disease | Bilateral SNHL pattern; ANA, ANCA | Steroid response trial |
| Superior canal dehiscence | Low-frequency CHL + normal tympanogram | High-resolution CT temporal bone |
Sources: Harrison's Principles of Internal Medicine 22E (Walker & Daroff) | Rosen's Emergency Medicine 9E | Cummings Otolaryngology Head & Neck Surgery 7E | Ganong's Review of Medical Physiology 26E
This is the complete test reference from all three specialist perspectives — neurology, neuro-otology, and ENT. Ask me to go deeper on any specific test, condition, or section.
Now I am a learner pls teach me FULL VNG INTERPRETATION
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Searching Images
VNG videonystagmography caloric test interpretation canal paresis directional preponderance
Reading File
Loading Image
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Reading File
I now have all the textbook content I need. Let me write the comprehensive VNG interpretation guide.
📖 FULL VNG INTERPRETATION — A Complete Learner's Guide
Sources: K.J. Lee's Essential Otolaryngology | Cummings Otolaryngology Head & Neck Surgery | Harrison's Principles of Internal Medicine 22E
WHAT IS VNG?
Videonystagmography (VNG) is the current gold-standard laboratory method for recording and quantifying eye movements in patients with dizziness, vertigo, and balance disorders.
How it works:
- The patient wears infrared goggles/cameras that record eye movements in real time
- Cameras capture the pupil and corneal reflections at high speed
- Eye movements are plotted on a graph (position or velocity vs. time)
- Results are analyzed by a trained audiologist or neuro-otologist
Why it replaced ENG (Electronystagmography):
ENG used skin electrodes measuring the corneoretinal electrical potential — indirect and limited to horizontal movements. VNG uses direct infrared video — more accurate, can measure torsional and vertical movements, and shows recordings in real time.
It is always important to review the original recordings and not rely on the interpretations of others or automated readings of data tracings. — Cummings Otolaryngology
THE VNG BATTERY — 9 SUBTESTS IN 2 CATEGORIES
VNG BATTERY
│
├── OCULOMOTOR SUBTESTS (tests the BRAIN — central pathways)
│ 1. Saccade Testing
│ 2. Smooth Pursuit Testing
│ 3. Optokinetic Testing (OKN)
│ 4. Gaze / Fixation Testing
│
└── VESTIBULAR SUBTESTS (tests the INNER EAR / CN VIII)
5. Spontaneous Nystagmus
6. Gaze-Evoked Nystagmus
7. Positional Nystagmus Testing
8. Positioning Nystagmus (Dix-Hallpike / Supine Roll)
9. Bithermal Caloric Testing ← THE MOST IMPORTANT SUBTEST
══════════════════════════════════
PART 1 — OCULOMOTOR SUBTESTS
══════════════════════════════════
These tests examine the central nervous system's ability to control eye movements. Abnormalities here = central pathology (brainstem, cerebellum, cortex).
🔵 SUBTEST 1: SACCADE TESTING
What Are Saccades?
Saccades are the fast, voluntary, ballistic jumps the eyes make when rapidly shifting gaze from one target to another — like reading a line of text or looking at something that catches your attention.
How the Test is Done:
- Patient sits in front of a light bar or screen
- Random dots/lights appear at various positions (left/right, 5° to 30°)
- Patient jumps eyes to each new target as quickly as possible
- Head is kept still
What is Measured:
| Parameter | What It Measures | Normal Value |
|---|---|---|
| Latency | Time from target appearance to eye movement onset | 180–200 ms |
| Velocity | Speed of the eye movement | Increases with amplitude; ~400–700°/s for large saccades |
| Accuracy (Gain) | Did the eye land on the target? | Gain = 0.9–1.0 |
How to Read the Saccade Tracing:
Normal saccade trace looks like this:
________
| |
________| |_______
target target
(Steps = sharp, quick, accurate)
Abnormal patterns:
Undershoot (hypometria): ___/¯¯¯ (eye falls short, makes correction)
Overshoot (hypermetria): ¯¯¯\___ (eye goes too far, corrects back)
Slow saccades: /¯¯¯¯¯\ (reduced velocity - "round top")
Interpreting Saccade Results:
| Finding | Meaning |
|---|---|
| Prolonged latency (>200 ms) | Frontal lobe, brainstem, or basal ganglia disease |
| Hypometria (undershoot, gain <0.8) | Cerebellar or brainstem disease |
| Hypermetria (overshoot, gain >1.0) | Cerebellar dysfunction — classic finding |
| Slow saccade velocity | Internuclear ophthalmoplegia (INO), brainstem disease, drugs |
| Normal saccades | Central saccadic pathway intact |
Key rule: If saccades are abnormal but caloric test is normal → central pathology is highly likely. — K.J. Lee's Essential Otolaryngology
🔵 SUBTEST 2: SMOOTH PURSUIT TESTING
What Is Smooth Pursuit?
Smooth pursuit is the ability to track a slowly moving target smoothly, keeping the image on the fovea. It requires intact cerebellar and cortical pathways.
How the Test is Done:
- A dot moves slowly and sinusoidally back and forth on the screen
- Frequency: 0.2–0.7 Hz, amplitude: ±20° (total arc of 40°)
- Patient follows the dot without moving their head
What is Measured: Pursuit Gain
- Gain = eye velocity / target velocity
- Normal gain = 0.8–1.0 (eyes keep up smoothly with the target)
How to Read the Pursuit Tracing:
NORMAL (gain ~1.0) — eyes mirror the target:
Target: /\/\/\/\/\/\
Eyes: /\/\/\/\/\/\ ← Perfect smooth tracking
ABNORMAL (saccadic pursuit) — catch-up saccades appear:
Target: /\/\/\/\/\/\
Eyes: /\/|/\/|/\/| ← Staircase pattern with saccades
ABNORMAL (reduced gain) — eyes lag behind:
Target: /\/\/\/\/\/\
Eyes: /\__/\__/\__ ← Flat, lagging
Interpreting Pursuit Results:
| Finding | Meaning |
|---|---|
| Reduced gain (<0.8) + catch-up saccades ("saccadic pursuit") | Cerebellar disease, brainstem lesion |
| Asymmetric pursuit (worse in one direction) | Ipsilateral cortical or cerebellar lesion |
| Mildly reduced bilateral gain | Can be normal with aging — interpret with caution |
| Normal gain | Central pursuit pathway intact |
"Saccadic pursuit" — a staircase pattern — is characteristic of cerebellar disease and also occurs with the decreased pursuit gain of normal aging. — Cummings Otolaryngology
🔵 SUBTEST 3: OPTOKINETIC TESTING (OKN)
What Is the Optokinetic Reflex?
When the entire visual field moves (like watching trees pass from a train window), the eyes automatically follow — this is the optokinetic response. It produces a regular nystagmus: slow-phase follows the moving scene, fast-phase resets.
How the Test is Done:
- A large striped drum or full-field moving pattern is presented
- Moving at 30–60°/s, first in one direction then the other
- VNG records the resulting nystagmus
What is Measured:
- OKN gain = slow-phase eye velocity / stimulus velocity
- Symmetry between leftward and rightward stimulation
Interpreting OKN:
| Finding | Meaning |
|---|---|
| Asymmetric OKN (reduced to one side) | Ipsilateral cerebral hemisphere lesion (directional asymmetry mirrors smooth pursuit deficits) |
| Absent OKN bilaterally | Bilateral peripheral vestibular loss OR brainstem lesion |
| OKN quick-phase abnormalities | Mirror saccade abnormalities |
| Normal symmetric OKN | Central OKN pathways intact |
Slow-phase abnormalities on optokinetic tests parallel those detected with smooth-pursuit testing, whereas quick-phase abnormalities are correlated with saccade testing. — Cummings Otolaryngology
OKAN (Optokinetic After-Nystagmus):
After the OKN stimulus stops, nystagmus persists briefly in darkness — this is OKAN.
- Relies on the velocity storage mechanism (vestibular nuclei + cerebellum)
- Reduced in bilateral peripheral vestibular loss
- Asymmetric in unilateral vestibular hypofunction (greater toward side of lesion)
🔵 SUBTEST 4: GAZE / FIXATION TESTING
What Is Fixation Suppression?
When the eyes fixate on a stationary target, any pre-existing nystagmus (from a peripheral vestibular lesion) should be suppressed by vision. This requires an intact cerebellar flocculus and brainstem.
How the Test is Done:
- Patient looks straight ahead (primary gaze) first with eyes open with fixation target, then in a darkened environment (goggles block light)
- Then patient looks 30° to the right, left, up, down
What is Measured:
- Fixation Index = nystagmus SPV with fixation / SPV without fixation
- Normal: fixation reduces or eliminates nystagmus
Interpreting Gaze/Fixation:
| Finding | Meaning |
|---|---|
| Nystagmus suppressed by fixation | Peripheral vestibular lesion |
| Fixation does NOT suppress nystagmus ("failure of fixation suppression") | Central lesion (cerebellar flocculus damage) |
| Gaze-evoked nystagmus (appears only on lateral/vertical gaze) | Central (brainstem/cerebellar) pathology |
| Direction-changing on lateral gaze | Central |
| Endpoint nystagmus at >30° lateral gaze | Physiologic / normal variant |
══════════════════════════════════
PART 2 — VESTIBULAR SUBTESTS
══════════════════════════════════
🟠 SUBTEST 5: SPONTANEOUS NYSTAGMUS (with and without fixation)
What It Tests:
Whether the vestibular system at rest is generating an abnormal nystagmus due to asymmetric input from the two labyrinths.
How the Test is Done:
- Patient looks straight ahead
- Eyes OPEN with fixation target (light on)
- Eyes in darkness (goggles, no fixation)
- Record any nystagmus
How to Read the Tracing:
Normal: Flat line — no eye movement at rest
_________________________
Abnormal: Regular sawtooth = spontaneous nystagmus present
/|/|/|/|/|/|/|/|/|/|/|
slow fast (jerk nystagmus)
← slow phase ↑fast phase
Interpreting Spontaneous Nystagmus:
| Finding | Meaning |
|---|---|
| No nystagmus (eyes open or closed) | Normal |
| Nystagmus present, suppressed by fixation | Peripheral vestibular lesion |
| Nystagmus present, NOT suppressed by fixation | Central lesion |
| Unidirectional horizontal nystagmus | Peripheral (fast phase away from lesioned ear) |
| Direction-changing nystagmus at rest | Central |
| Purely vertical or torsional at rest | Central |
Alexander's Law — MUST KNOW for VNG:
The slow-phase velocity of peripheral nystagmus increases when the eyes look in the direction of the fast phase and decreases when looking away from it. — K.J. Lee's Essential Otolaryngology
| Degree | Pattern |
|---|---|
| 1st degree nystagmus | Present ONLY when gazing toward the fast phase |
| 2nd degree nystagmus | Present in primary gaze AND when looking toward fast phase |
| 3rd degree nystagmus | Present in ALL gaze directions (most severe acute lesion) |
🟠 SUBTEST 6: GAZE-EVOKED NYSTAGMUS
What It Tests:
Whether the gaze-holding mechanism (brainstem/cerebellum) is working normally.
How Done:
Patient holds gaze at 30° left, right, up, down for ~15–20 seconds each.
Interpretation:
| Finding | Meaning |
|---|---|
| No nystagmus in any gaze direction | Normal |
| Nystagmus only in direction of gaze (gaze-evoked) | Central (cerebellar / brainstem gaze-holding failure) |
| Direction-changing nystagmus (beats right on right gaze, left on left gaze) | Central |
| Downbeat nystagmus (fast phase toward chin, worse on downgaze) | Cerebellar flocculus / Arnold-Chiari malformation |
| Upbeat nystagmus | Brainstem lesion |
| Periodic alternating nystagmus (direction changes every ~2 min spontaneously) | Cerebellar nodulus lesion |
🟠 SUBTEST 7: POSITIONAL NYSTAGMUS TESTING
What It Tests:
Whether placing the head/body in certain static positions (sustained) produces nystagmus.
Positions Tested (Static Holds):
- Supine (lying flat on back)
- Right lateral (lying on right side)
- Left lateral (lying on left side)
- Head-right (supine, head turned right)
- Head-left (supine, head turned left)
Each position held for 30–60 seconds while recording.
Types of Positional Nystagmus:
| Type | Description | Meaning |
|---|---|---|
| Direction-fixed (same direction in all positions) | Nystagmus beats in one consistent direction regardless of position | Usually peripheral (unilateral vestibular hypofunction) |
| Direction-changing geotropic (beats toward the ground in both lateral positions) | Beats right when right side down; beats left when left side down | Peripheral (horizontal canal BPPV — canalithiasis variant) |
| Direction-changing apogeotropic (beats away from ground) | Beats left when right side down; beats right when left side down | Horizontal canal BPPV (cupulolithiasis) OR central |
| Direction-changing in non-positional testing | Spontaneously changes direction | Central |
🟠 SUBTEST 8: POSITIONING NYSTAGMUS (Dix-Hallpike / Supine Roll)
This is the DYNAMIC test — the patient is moved RAPIDLY into position.
Dix-Hallpike — Posterior Canal BPPV
Classic POSITIVE finding on VNG tracing:
- Latency: 3–10 seconds after positioning
- Upbeat + torsional nystagmus
- Duration: 5–30 seconds then stops
- Reversal on return to sitting
- Fatigues with repetition (diminishes each time test is repeated)
Central Positional Nystagmus (Abnormal on Hallpike):
- No latency (begins immediately)
- No fatigability (stays just as strong with repeated testing)
- Purely vertical or torsional (not the mixed upbeat+torsional of BPPV)
- Persists >90 seconds in head-hanging position
PERIPHERAL BPPV (Hallpike tracing):
Time → 0 3s 5s 30s
| |___| |
| /\ \ |___ ← resolves spontaneously
peak decay
↑ latency ↑ fatigues
CENTRAL (Hallpike tracing):
Time → 0 1s steady...
| |______________
| immediate onset, no decay, persists
Supine Roll Test — Horizontal Canal BPPV
| Finding | Type | Affected Ear |
|---|---|---|
| Geotropic (toward floor), stronger on one side | Canalithiasis | Side with STRONGER nystagmus |
| Apogeotropic (away from floor), stronger on one side | Cupulolithiasis | Side with WEAKER nystagmus |
🔴 SUBTEST 9: BITHERMAL CALORIC TESTING — THE HEART OF VNG
This is the most important and most complex VNG subtest. Understand this deeply.
Principle: Why Does Temperature Cause Nystagmus?
The horizontal semicircular canal lies closest to the external ear canal. When temperature changes, convection currents are created in the endolymph:
- Warm (44°C) irrigation → endolymph near the ear rises (less dense) → ampullopetal flow (toward the ampulla) → hair cells excited → nystagmus toward the same (irrigated) ear → "W" in COWS
- Cold (30°C) irrigation → endolymph near the ear sinks (more dense) → ampullofugal flow (away from ampulla) → hair cells inhibited → nystagmus toward the opposite ear → "C" in COWS
COWS Mnemonic:
Cold → Opposite | Warm → Same
The 4 Irrigations of Bithermal Caloric Testing:
| Irrigation | Expected Nystagmus Direction |
|---|---|
| Right ear Warm (44°C) | Fast phase BEATS RIGHT |
| Right ear Cold (30°C) | Fast phase BEATS LEFT |
| Left ear Warm (44°C) | Fast phase BEATS LEFT |
| Left ear Cold (30°C) | Fast phase BEATS RIGHT |
What is Measured: SPV (Slow Phase Velocity)
The key measurement is the peak slow-phase velocity (SPV) of the nystagmus in degrees per second (°/s).
Normal peak SPV for each irrigation: approximately 15–60°/s (laboratory-dependent)
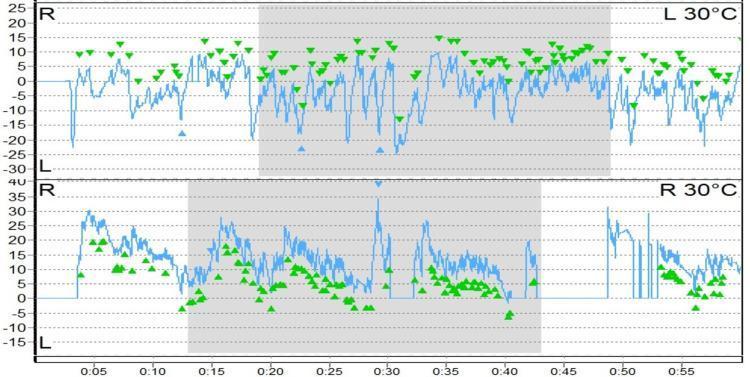
Real VNG Caloric Tracing — What You Are Looking At:
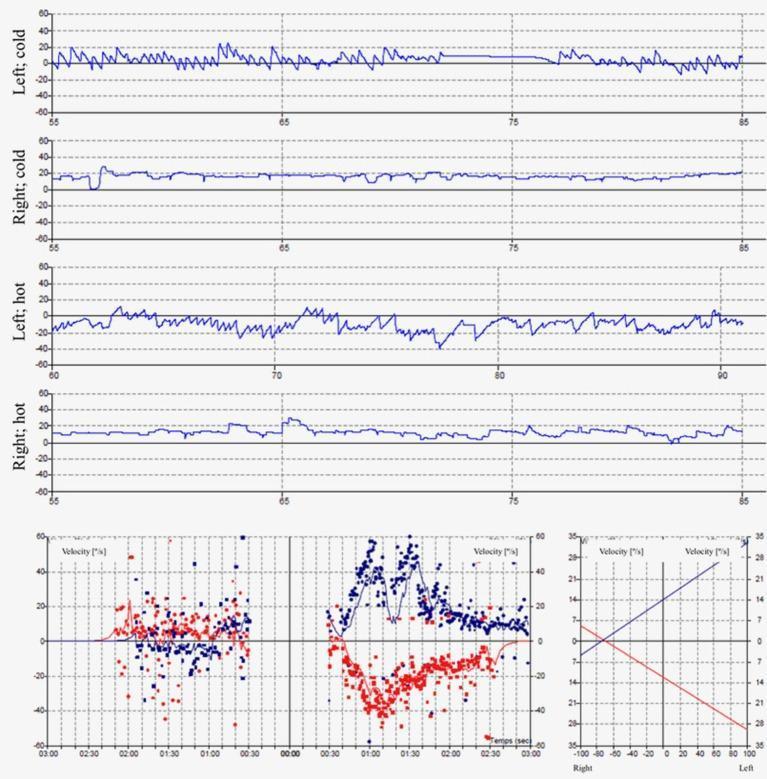
Top 4 panels: SPV tracings for Left Cold, Right Cold, Left Hot, Right Hot irrigations. Note how the left ear gives robust responses (fluctuating traces) while the right ear gives near-flat traces (<5°/s) — classic right vestibular areflexia. Bottom right: the summary caloric chart with two diagonal lines showing the calculated UW and DP.
Jongkees Formulas — THE CALCULATIONS YOU MUST KNOW
Using the peak SPV from each irrigation:
- RW = Right Warm SPV
- RC = Right Cold SPV
- LW = Left Warm SPV
- LC = Left Cold SPV
Formula 1: UNILATERAL WEAKNESS (UW) / Canal Paresis (CP)
[(RW + RC) - (LW + LC)]
UW% = ─────────────────────────── × 100
(RW + RC + LW + LC)
Interpretation:
- UW < 25% = Normal (both ears respond equally)
- UW ≥ 25% = Abnormal — Canal Paresis on the side with SMALLER total response
- If right side has smaller (RW+RC), then there is Right Canal Paresis
Formula 2: DIRECTIONAL PREPONDERANCE (DP)
[(RW + LC) - (LW + RC)]
DP% = ─────────────────────────── × 100
(RW + RC + LW + LC)
(Note: Group the irrigations by their nystagmus direction:
RW beats right + LC beats right vs. LW beats left + RC beats left)
Interpretation:
- DP < 30% = Normal (nystagmus beats equally in both directions)
- DP ≥ 30% = Significant directional imbalance — the brain/vestibular system has a persistent bias toward one direction
- DP directed away from a peripheral lesion (the intact ear dominates)
- DP directed toward a central lesion (less reliable clinically)
Worked Example — Step by Step:
Results recorded:
- RW = 20°/s (right warm)
- RC = 14°/s (right cold)
- LW = 42°/s (left warm)
- LC = 38°/s (left cold)
Step 1 — Calculate UW:
[(20+14) - (42+38)] ÷ (20+14+42+38) × 100
= [34 - 80] ÷ 114 × 100
= -46 ÷ 114 × 100
= -40% → 40% RIGHT canal paresis
→ Right ear produces only 34°/s total; left ear produces 80°/s total — right ear is weak
Step 2 — Calculate DP:
[(20+38) - (42+14)] ÷ 114 × 100
= [58 - 56] ÷ 114 × 100
= 2 ÷ 114 × 100
= 1.7% → Normal DP
→ Interpretation: Right unilateral canal paresis (40% UW), no directional preponderance → RIGHT PERIPHERAL VESTIBULAR LESION (e.g., right vestibular neuritis)
VNG Caloric Finding — "Caloric Inversion"
These two tracings show "caloric inversion" — nystagmus beats in the OPPOSITE direction to what COWS predicts. Cold irrigation causes nystagmus toward the SAME side instead of opposite. This is a rare but important sign strongly suggesting CENTRAL vestibular dysfunction or brainstem pathology. Technical artifacts (TM perforation) must be excluded.
VNG Caloric — Bilateral Weakness (BW):
| Criterion | Meaning |
|---|---|
| Total (LW + LC) < 12°/s AND (RW + RC) < 12°/s | Bilateral vestibular hypofunction |
| Both sides produce barely any response to temperature | Consider: aminoglycoside ototoxicity, neurofibromatosis 2, autoimmune labyrinthitis |
Hyperactive Caloric Response:
| Finding | Meaning |
|---|---|
| SPV peaks > 80–100°/s (very large responses) | Loss of cerebellar inhibition → cerebellum unable to suppress the VOR |
| Seen in: cerebellar lesions, spinocerebellar ataxia | Central pathology (requires intact TM — not a TM defect artifact) |
Special Caloric Consideration — Fixation Suppression During Calorics:
After each caloric irrigation produces a response:
- A fixation light is turned on
- Normally the caloric nystagmus reduces by >50% (peripheral suppression)
- Failure to suppress = Fixation Index <0.5 → central pathology (cerebellar flocculus damage)
══════════════════════════════════
PART 3 — PUTTING IT ALL TOGETHER
══════════════════════════════════
VNG Pattern Recognition — The 5 Essential Patterns
Pattern 1: UNILATERAL PERIPHERAL VESTIBULAR HYPOFUNCTION
(e.g., vestibular neuritis, Ménière's disease, after labyrinthectomy)
| Subtest | Finding |
|---|---|
| Spontaneous nystagmus | Unidirectional horizontal; suppressed by fixation |
| Saccades | Normal |
| Smooth pursuit | Normal |
| OKN | Normal or mildly asymmetric |
| Positional nystagmus | Direction-fixed |
| Caloric | Unilateral weakness ≥25% on affected side |
| Fixation suppression | Intact (nystagmus suppresses) |
Pattern 2: BILATERAL PERIPHERAL VESTIBULAR HYPOFUNCTION
(e.g., gentamicin toxicity, autoimmune, bilateral neuritis)
| Subtest | Finding |
|---|---|
| Spontaneous nystagmus | Absent or minimal |
| Saccades | Normal |
| Smooth pursuit | Normal or mildly reduced |
| OKN | Absent or markedly reduced bilaterally |
| Caloric | Bilateral weakness — total SPV <12°/s each side |
| Rotary chair (if done) | Markedly reduced bilateral VOR gain |
| Oscillopsia test | Loses >5 lines on Snellen chart during head shake |
Pattern 3: BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV)
(Posterior canal most common)
| Subtest | Finding |
|---|---|
| Spontaneous nystagmus | None |
| Saccades | Normal |
| Pursuit | Normal |
| Caloric | Normal |
| Dix-Hallpike | Positive: upbeat + torsional, latency 3–10s, fatigable, <30s duration |
| Other subtests | Normal |
Pattern 4: CENTRAL VESTIBULAR LESION
(e.g., posterior fossa stroke, MS, cerebellar tumor)
| Subtest | Finding |
|---|---|
| Spontaneous nystagmus | Direction-changing OR purely vertical/torsional; NOT suppressed by fixation |
| Saccades | Abnormal — hypermetria (cerebellar), slow (INO), prolonged latency |
| Smooth pursuit | Abnormal — saccadic pursuit, asymmetric |
| OKN | Asymmetric or absent |
| Gaze-evoked nystagmus | Gaze-evoked nystagmus, direction-changing |
| Caloric | Normal OR bilaterally reduced OR hyperactive |
| Fixation suppression | Fails — nystagmus NOT suppressed by fixation |
| Positioning | Nystagmus with no latency, no fatigability, purely vertical |
KEY RULE: Abnormal saccades or saccadic pursuit with normal caloric responses = central pathology until proven otherwise. — K.J. Lee's Essential Otolaryngology
Pattern 5: UNCOMPENSATED PERIPHERAL LESION (Chronic / Rehabilitating)
| Finding | Interpretation |
|---|---|
| Unilateral caloric weakness present | Peripheral lesion remains |
| Directional preponderance away from weak ear | CNS not yet fully compensated — asymmetric vestibular tone persists |
| Spontaneous nystagmus still present in darkness | Incomplete static compensation |
| Good fixation suppression | Peripheral, not central |
| Normal saccades, pursuit | Central pathways intact; rehabilitation appropriate |
QUICK REFERENCE: PERIPHERAL vs. CENTRAL ON VNG
| VNG Subtest | Peripheral Pattern | Central Pattern |
|---|---|---|
| Saccades | Normal | Dysmetric, slow, prolonged latency |
| Smooth Pursuit | Normal | Saccadic (staircase), asymmetric, low gain |
| OKN | Normal or mildly asymmetric | Asymmetric or absent |
| Spontaneous Nystagmus | Unidirectional, suppressed by fixation | Direction-changing, NOT suppressed |
| Gaze Nystagmus | Alexander's law (worsens toward fast phase) | Gaze-evoked nystagmus, direction-changing |
| Positional | Direction-fixed OR geotropic/apogeotropic | Direction-changing without pattern |
| Dix-Hallpike | Upbeat+torsional, latent, fatigable | No latency, no fatigue, purely vertical |
| Caloric UW | ≥25% = peripheral weakness | Normal caloric + other abnormalities = central |
| Caloric Bilateral | History of ototoxicity or labyrinthine disease | No ototoxin history → suspect central |
| Caloric Hyperactive | Not expected | Cerebellar disinhibition |
| Fixation Suppression | Intact (suppresses ≥50%) | Fails (<50% suppression) |
| Caloric Inversion | Rare technical artifact | Brainstem pathology |
COMMON CLINICAL SCENARIOS — VNG INTERPRETATION
🔎 Case 1:
30-year-old, sudden constant vertigo, nausea for 3 days.
VNG: Unidirectional left-beating spontaneous nystagmus; fixation suppresses it; right caloric UW = 35%; saccades normal; pursuit normal.
Interpretation: ✅ Right vestibular neuritis — right canal paresis, peripheral pattern, central tests normal.
🔎 Case 2:
55-year-old, vertigo only when rolling in bed.
VNG: No spontaneous nystagmus; Dix-Hallpike RIGHT → upbeat+torsional nystagmus latency 5s, lasts 15s, reverses, fatigues on repeat; caloric normal.
Interpretation: ✅ Right posterior canal BPPV — classic pattern. Normal caloric confirms no labyrinthine disease.
🔎 Case 3:
60-year-old, recurrent vertigo+hearing loss+tinnitus.
VNG: Left caloric UW = 28%; audiometry: left low-frequency SNHL; ECoChG SP/AP elevated left.
Interpretation: ✅ Left Ménière's disease — unilateral canal paresis + low-frequency SNHL + elevated SP/AP.
🔎 Case 4:
45-year-old, chronic dizziness, no hearing loss, past stroke history.
VNG: Direction-changing gaze-evoked nystagmus; saccadic pursuit; hypermetric saccades; caloric normal; fixation suppression fails.
Interpretation: 🚨 Central vestibular lesion — abnormal saccades + pursuit + gaze nystagmus + failed fixation suppression despite normal calorics = central pathology. MRI needed urgently.
🔎 Case 5:
70-year-old, unsteady gait for 1 year, oscillopsia (vision bounces while walking). History: IV gentamicin 2 years ago.
VNG: No spontaneous nystagmus; caloric bilaterally flat (LW+LC = 4°/s; RW+RC = 5°/s); rotary chair gain markedly reduced; dynamic visual acuity: -6 lines.
Interpretation: ✅ Bilateral vestibular hypofunction from gentamicin ototoxicity — bilateral caloric areflexia.
FACTORS THAT CAN AFFECT VNG ACCURACY — PITFALLS
| Factor | Effect |
|---|---|
| Cerumen impaction | Blocks temperature from reaching the canal → falsely reduced caloric response |
| Tympanic membrane perforation | Water caloric contraindicated; use air; perforated side gives heightened response |
| Medications (sedatives, antihistamines, benzodiazepines, alcohol) | Suppress VOR and pursuit → false central-looking results. Always check medications before testing |
| Poor alertness / drowsiness | Reduces caloric response amplitude → falsely bilateral weakness |
| Head position for caloric | Head must be elevated 30° from supine — if not, the horizontal canal is not vertical and convection doesn't occur properly |
| Age | Caloric responses decrease with age; pursuit gain decreases; saccade latency increases — use age-adjusted norms |
| Contact lenses / glasses | Remove for video recording accuracy |
| Neck pain / limitation | May prevent full Dix-Hallpike positioning |
SUMMARY: HOW TO READ A VNG REPORT IN 5 STEPS
STEP 1 — OCULOMOTOR TESTS (Saccades, Pursuit, OKN, Fixation)
Normal? → No central pathology
Abnormal? → Central lesion likely regardless of caloric result
STEP 2 — SPONTANEOUS NYSTAGMUS
Present? → Suppressed by fixation? (peripheral) / Not suppressed? (central)
Direction? Fixed (peripheral) / Changing (central)
STEP 3 — POSITIONAL / POSITIONING TESTS
Dix-Hallpike positive? → Check: latency, direction, fatigability → BPPV vs. central
Static positions: direction-fixed vs. direction-changing
STEP 4 — CALORIC RESULTS
Calculate UW% and DP%
UW ≥25% → Canal paresis (which ear is weaker)
Bilateral weakness → Think ototoxicity / autoimmune / degeneration
Fixation suppression: Intact (peripheral) / Failed (central)
STEP 5 — INTEGRATE ALL FINDINGS → Pattern Recognition
Peripheral pattern → counsel on diagnosis + treatment
Central pattern → urgent neuroimaging (MRI-DWI)
Mixed pattern → consider neuro-otology referral
Sources: K.J. Lee's Essential Otolaryngology 12E | Cummings Otolaryngology Head & Neck Surgery 7E | Harrison's Principles of Internal Medicine 22E
You now have a complete VNG interpretation reference — from the physics of caloric testing to reading the tracing, calculating Jongkees formulas, and recognizing all the clinical patterns. Ask me to drill down into any specific subtest, work through more case examples, or move on to rotary chair or VEMP interpretation.
This is a shared conversation. Sign in to Orris to start your own chat.