Elephantiasis
Reading File
search_medical_text
elephantiasis lymphatic filariasis etiology pathophysiology diagnosis management
search_medical_image
elephantiasis lymphedema filariasis clinical presentation
GradeResponse
GradeResponse
Elephantiasis
Elephantiasis is a chronic, disfiguring condition characterized by massive swelling and thickening of skin and subcutaneous tissues, most commonly affecting the lower limbs and genitalia.
Etiology
The overwhelming majority of cases are caused by lymphatic filariasis — infection by filarial nematodes, most commonly:
| Parasite | Distribution | Predominant Feature |
|---|---|---|
| Wuchereria bancrofti | Worldwide tropics | Lower limb + genital involvement |
| Brugia malayi | South/Southeast Asia | Lower limb; spares genitalia |
| Brugia timori | Lesser Sunda Islands | Lower limb; spares genitalia |
Transmission is via mosquito bites (various Culex, Anopheles, Aedes species). Non-filarial elephantiasis (podoconiosis) occurs due to chronic exposure to volcanic red clay soils; it is common in the Ethiopian highlands.
Pathophysiology
Adult filarial worms take up residence in the lymphatic vessels and lymph nodes. The host inflammatory response to the worms — combined with worm death and secondary bacterial/fungal superinfection — causes:
- Lymphangitis and lymphadenitis (early)
- Lymphatic dilation and valve incompetence
- Transient pitting lymphedema → permanent brawny edema
- Subcutaneous fibrosis, hyperkeratosis, and skin fissuring
- Repeated secondary bacterial infections accelerate skin changes
In W. bancrofti infection, retroperitoneal lymphatic obstruction can rupture renal lymphatics, causing chyluria (milky urine). Hydrocele and scrotal lymphedema are also common in bancroftian filariasis (Harrison's, p. 6620).
Clinical Presentation
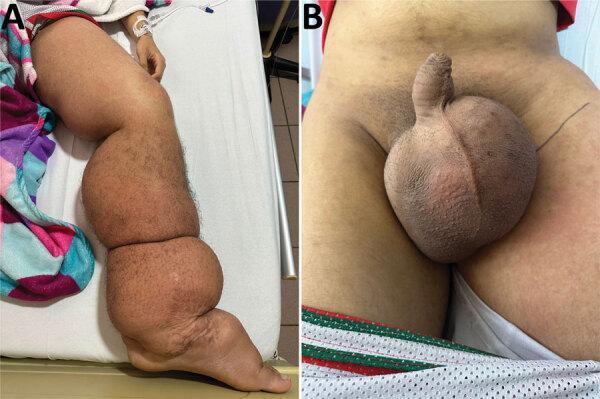
Stages:
- Asymptomatic microfilaremia — most infected individuals; no overt disease
- Acute dermatolymphangioadenitis (ADLA) — fever, painful lymphadenitis/lymphangitis, often triggered by secondary infection
- Chronic lymphedema — progressive, irreversible swelling; brawny, non-pitting texture
- Elephantiasis — massive limb/scrotal enlargement, skin folds, verrucous (warty) hyperkeratosis, fissures, and recurrent infections
Diagnosis
| Test | Notes |
|---|---|
| Microfilaria on blood smear | Gold standard; blood drawn at midnight (nocturnal periodicity of W. bancrofti) |
| Antigen detection (ICT card) | Detects W. bancrofti circulating antigen; no nocturnal timing needed; highly sensitive |
| Serology (ELISA/IgG4) | Useful for Brugia spp. |
| Ultrasound (lymphatic) | May reveal "filarial dance sign" — live worms moving in dilated lymphatics |
| Lymphoscintigraphy | Delineates lymphatic architecture |
Management
Antiparasitic Therapy
- Diethylcarbamazine (DEC) — kills both microfilariae and adult worms; first-line in most endemic settings
- Ivermectin + albendazole — used in mass drug administration (MDA) programs in areas co-endemic with onchocerciasis (DEC avoided there due to reactions)
- Doxycycline 4–6 weeks — targets Wolbachia endosymbionts in the worm; macrofilaricidal, improves lymphedema in some studies
Lymphedema Morbidity Management (MMDP)
Antiparasitic drugs do not reverse established elephantiasis. Management focuses on:
- Limb hygiene — daily washing, skin care, antifungal treatment
- Compression therapy — bandaging and compression garments
- Exercise and elevation
- Prompt treatment of ADLA episodes (antibiotics)
- Surgery — debulking procedures (Charles procedure) or microsurgical lymphovenous anastomosis in selected cases
Hydrocele
Surgical repair is recommended for large hydroceles.
Complications
- Recurrent bacterial cellulitis and lymphangitis
- Disability and loss of livelihood
- Psychological burden and social stigma
- Chyluria (retroperitoneal involvement)
- Chylous ascites / chylothorax (rare)
Epidemiology & Global Burden
- ~120 million people infected worldwide; ~40 million clinically disabled
- Endemic in 72 countries across tropics/subtropics
- The WHO Global Programme to Eliminate Lymphatic Filariasis (GPELF) uses annual MDA campaigns
- Elimination defined as interrupting transmission + reducing morbidity
Differential Diagnosis
| Condition | Distinguishing Features |
|---|---|
| Podoconiosis | Non-filarial; bilateral; no microfilaremia; soil exposure history |
| Chronic venous insufficiency | Stasis dermatitis, varicosities; no filarial serology |
| Milroy disease | Congenital primary lymphedema; familial |
| Malignant lymphedema | Unilateral; underlying cancer; rapid onset |
| Lipedema | Bilateral lower limbs + spares feet; predominantly women |
This is a shared conversation. Sign in to Orris to start your own chat.