Anomalies of development. trauma. foreign bodies. inflammatory diseases of the outer ear and their complications.
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
I now have comprehensive information to compose a thorough response. Let me put it all together.
Diseases of the Outer Ear: Developmental Anomalies, Trauma, Foreign Bodies, and Inflammatory Diseases
I. Anatomy Overview
The outer ear consists of three parts: the auricle (pinna), the external auditory canal (EAC) (~2.5 cm long, average volume 2 cm³), and the outer surface of the tympanic membrane (TM). The EAC acts as a resonance chamber for 2000–5500 Hz. The TM has three layers (outer epithelial, middle fibrous, inner mucosal) in its pars tensa; the pars flaccida has only two layers.
— K.J. Lee's Essential Otolaryngology
II. Developmental Anomalies
Embryology
- 5 weeks' gestation: The auricle develops from the 1st (mandibular) and 2nd (hyoid) branchial arches, forming six Hillocks of His. Hillock 1 → tragus; 2 → helical crus; 3 → helix; 4 → antihelix; 5 → antitragus; 6 → lobule.
- 8 weeks: The cartilaginous outer third of the EAC forms from the 1st branchial groove; the bony inner two-thirds forms from the meatal plug.
- 21 weeks: Epithelial cells resorb to canalize the bony EAC — incomplete resorption causes atresia or stenosis.
- Postnatally, the pinna is 80% of adult size by age 5, reaching full size by age 9.
A. Preauricular Tag
- Most common ear anomaly; caused by a supernumerary hillock.
- May be associated with branchio-oto-renal (BOR) syndrome (hearing loss, branchial cleft cyst, renal anomalies).
- Treatment: elective removal.
B. Preauricular Pit
- Caused by failure of hillock fusion; most common at the helical root.
- A pit below the tragus is more likely a 1st branchial cleft anomaly.
- Also associated with BOR syndrome.
- Acute infection → antibiotics ± drainage; definitive treatment is excision of the entire tract including the cartilage base to prevent recurrence.
C. Protruding Ears
- Due to underdevelopment of the antihelix and a deep conchal bowl.
- Usually bilateral.
- Otoplasty at age 5–6: Mustarde sutures recreate the anthelical fold; Furnas sutures set back the conchal bowl.
D. Microtia
- Prevalence: 1:600–12,000; more common in males, unilateral, right side.
- Weerda classification:
- Grade I: All components present but small; minimal extra tissue needed.
- Grade II: Some components present (rudimentary helix); partial reconstruction.
- Grade III: Structures present but unrecognizable (peanut ear) or anotia; total reconstruction.
- Associations: Goldenhar/hemifacial microsomia (oculo-auriculo-vertebral spectrum), Treacher Collins, BOR, CHARGE syndrome. 90% have associated hearing loss.
- Management:
- Non-surgical: hair masking, adhesive prosthesis.
- Bone-anchored auricular prosthesis (BAAP).
- Surgical repair (autogenous rib — Brent 3-stage or Nagata 2-stage method; Medpore synthetic implant; irradiated rib is largely abandoned due to resorption). Timing: age 5–6 when rib is large enough.
E. Aural Atresia
- Incidence: 1:20,000; male, unilateral, right side predominance.
- Associated syndromes: Apert, Crouzon, Pfeiffer, Goldenhar, Treacher Collins, Trisomies 13/18/21.
- Assessment: Bone-conduction ABR before 4 months of age; high-resolution CT of temporal bone before surgical planning.
- Jahrsdoefer scoring (CT-based, /10) predicts surgical success — score ≥8 predicts good outcome. Key criteria: stapes present (2 pts), oval/round windows patent, middle ear space, facial nerve position, malleus-incus complex, mastoid pneumatization.
- Management:
- Bilateral: early bone-conduction hearing aid.
- Unilateral: air-conduction aid in the patent ear; bone-conduction aid on the atretic side.
- Surgical: BAHA (percutaneous abutment or transcutaneous magnet) or formal atresia repair (after age 5, after microtia repair).
— K.J. Lee's Essential Otolaryngology
III. Trauma of the Outer Ear
A. Lacerations
- Simple (with or without cartilage), stellate from blunt trauma, or avulsion.
- Treatment: deep cleaning, debridement, surgical repair; consider bolster dressing to prevent hematoma.
- Complications: perichondritis, cartilage necrosis.
B. Auricular Hematoma
- Typical cause: blunt trauma (common in wrestlers/boxers → "cauliflower ear").
- Treatment: incision and drainage with through-and-through sutures and bolster dressing; systemic fluoroquinolones.
- Complications: fibrosis, cauliflower/wrestler's ear, perichondritis.
C. Frostbite
- Cold exposure causes endothelial disruption, erythrocyte extravasation, platelet aggregation, and sludging.
- Symptoms: pain, burning, discoloration, reduced pliability, sensory loss.
- Treatment: slow warming; antibiotics; anticoagulants; debridement only after demarcation. No pressure dressings.
D. Bites
- Lobe most commonly affected; human bites carry greater infection risk.
- Treatment: meticulous cleaning, systemic antibiotics, surgical repair.
E. Keloids and Hypertrophic Scars
- Higher rates in African American and Hispanic populations (up to 30%).
- Treatment: steroid injection, excision, pressure dressings, rarely radiotherapy.
— K.J. Lee's Essential Otolaryngology, p. 471
IV. Foreign Bodies of the External Auditory Canal
- Common objects: insects, nuts, beans, gum, putty, beads, toys.
- Key rule: avoid irrigation — vegetable matter will expand with water; blind instrumentation risks bleeding, canal edema, or TM perforation.
- Treatment:
- Local anesthetic block; microscopic examination and careful instrumentation.
- Mineral oil or antibiotic solution may facilitate removal.
- Topical antibiotics after removal if canal is irritated.
— K.J. Lee's Essential Otolaryngology, p. 472
V. Inflammatory Diseases of the Outer Ear
A. Acute Otitis Externa (AOE) — "Swimmer's Ear"
- Definition: Rapid-onset (<48 hours) EAC inflammation; generally unilateral.
- ~2.4 million US healthcare visits/year; peak age 5–10 years; more common in summer.
- Predisposing factors: narrow EAC, exostoses, eczema/seborrhoea/psoriasis, hearing-aid trauma, excess wax removal, water exposure.
Microbiology:
- Bacterial: >90% of cases — P. aeruginosa (most common), S. epidermidis, S. aureus.
- Fungal: Aspergillus, Candida (<2% primary; more common after antibiotic treatment).
- Viral (rare): varicella, measles, herpesvirus. Herpes zoster oticus (HZO) without facial palsy; Ramsay Hunt syndrome = HZO + facial palsy ± SNHL or vertigo.
Signs & Symptoms:
- Moderate-to-severe otalgia worsened by pinna manipulation (key differentiator from mastoiditis where mastoid tip is tender).
- Pruritus, erythema, scant clear → seropurulent discharge; edema, feeling of fullness, conductive hearing loss.
- Preauricular/cervical lymphadenopathy.
Treatment:
- Topical therapy is first-line (oral antibiotics are not effective). Options: fluoroquinolone drops or aminoglycoside + second antibiotic. Add corticosteroid to reduce inflammation. Acetic acid (50% diluted) useful in early mild cases.
- Caution with aminoglycosides if TM integrity uncertain (ototoxicity risk); neomycin contact hypersensitivity is common.
- EAC debridement is an important adjunct. If TM not visible, place a wick (cotton, Merocel sponge, or antibiotic-impregnated gauze) to stent the canal open and allow topical delivery.
- Preventive: occlusive earplugs for swimming; avoid cotton-tipped applicators.
B. Chronic Otitis Externa (COE)
- Bilateral in >50% of patients; affects 3–5% of the population.
- Mechanisms:
- Allergic: contact dermatitis from neomycin, hair sprays, hearing-aid molds.
- Systemic: amyloidosis, sarcoidosis, granulomatosis with polyangiitis, Sjögren's, psoriasis, lichen planus.
- Chronic infection: granular OE from bacteria/fungi causing granulation and excoriation of the canal.
- Local factors: moisture, elevated pH.
- Signs: Pruritus, mild discomfort, aural fullness; secretory (wet) or squamous (dry) types; atrophy and stenosis of canal skin (Fig. 138.1 in Cummings).
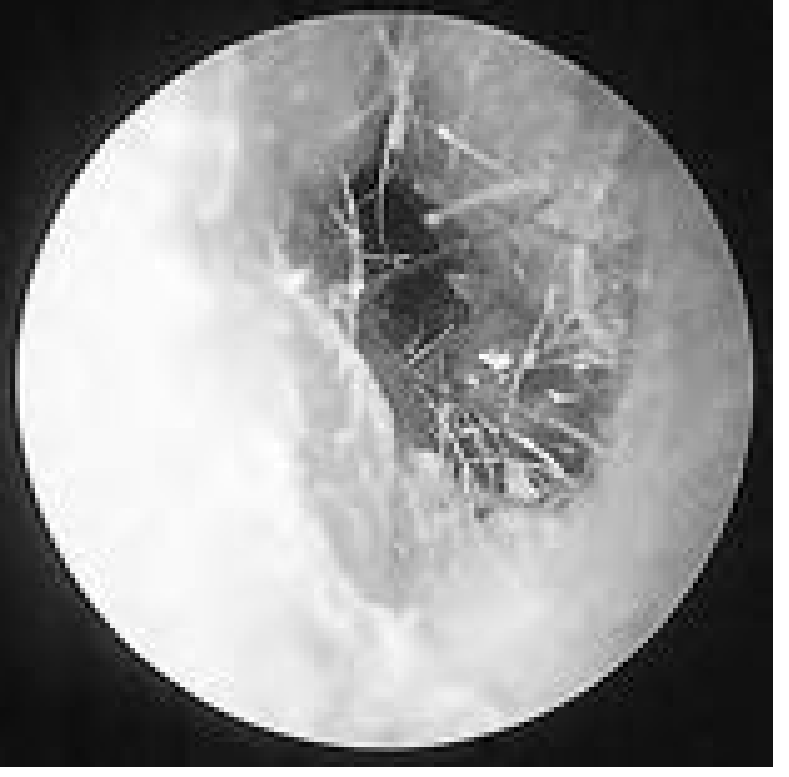
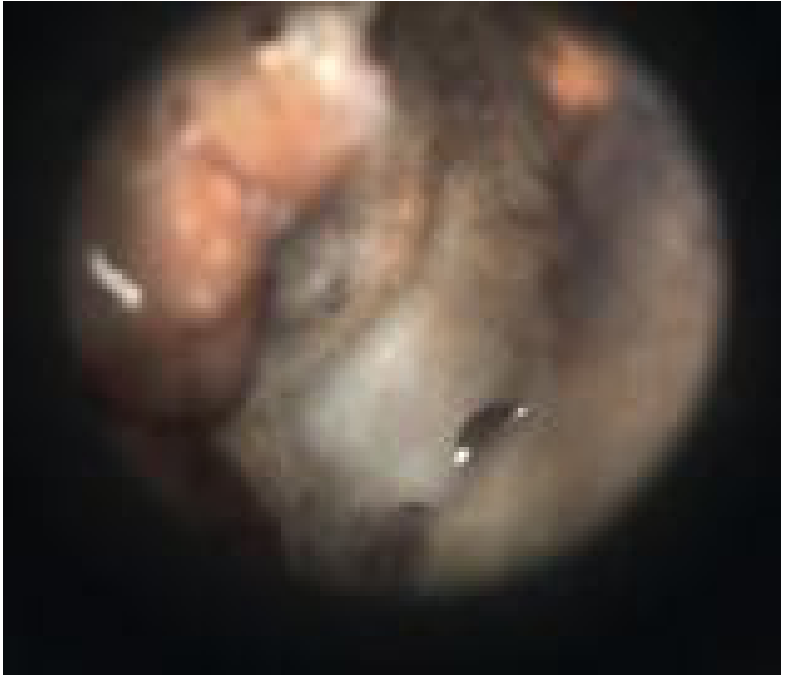
- Fungal OE (otomycosis): Severe pruritus, clear drainage, "cotton-like" debris. Candida: white plug. Aspergillus: moist white plug with black debris ("wet newspaper") — more aggressive infection of epithelial/subcutaneous tissues.
- Treatment: Dry ear precautions; meticulous EAC cleaning under microscopy; topical antibiotics long-term; for fungal OE: topical antifungals (e.g., clotrimazole 1%), EAC acidification. High recurrence rate.
- Severe COE may result in postinflammatory medial canal fibrosis — blind-ending canal.
C. Other EAC Conditions
| Condition | Features | Treatment |
|---|---|---|
| Seborrhoeic dermatitis / Eczema | Itching, weeping, scaly/fissured skin, crusting, canal stenosis | 1% hydrocortisone; betamethasone for acute flares |
| Keratosis obturans | Rapid keratin plug, painless canal expansion, poor epithelial migration | Frequent cleaning; topical steroids |
| EAC cholesteatoma | Keratin accumulation with osteitis and bone necrosis on canal floor; pain | Cleaning; steroids; surgical debridement; canal wall-down mastoidectomy if severe |
| Exostoses | Lamellar bone thickening from cold water/air exposure; canal stenosis, cerumen impaction | Canaloplasty ± skin graft |
| Osteoma | Pedunculated bone mass at suture lines | Surgical removal if obstructing |
VI. Complications of Otitis Externa
Perichondritis / Chondritis
- Extension of infection into auricular cartilage; can follow trauma, AOE, ear piercing.
- Presents as red, hot, swollen, painful auricle (sparing the lobule, which lacks cartilage).
- Causative organism: P. aeruginosa.
- Treatment: fluoroquinolones (systemic); may require surgical drainage.
Malignant (Necrotizing) Otitis Externa (MOE/NOE)
- Most feared complication — aggressive osteomyelitis of the EAC, mastoid, and skull base.
- Pathophysiology: Microangiopathy (especially in diabetics) and elevated cerumen pH allow bacterial invasion → vascular thrombosis → coagulative tissue necrosis. Spreads via fissures of Santorini and the tympanomastoid suture to the stylomastoid and jugular foramina. Does NOT spread through pneumatized tracts; middle ear is spared until late.
- Risk factors: Diabetes mellitus (up to 90% of cases), HIV/AIDS, myeloid malignancies, immunosuppression. Rare in immunocompetent patients.
- Causative organism: P. aeruginosa in >90%; also S. aureus, S. epidermidis, Proteus mirabilis, fungi (esp. Aspergillus fumigatus in HIV+).
- Mortality: 5–20% even in the antibiotic era.
Signs & Symptoms:
- Severe, deep-seated otalgia out of proportion to examination findings, worse at night.
- Otorrhoea, EAC edema.
- Pathognomonic: granulation tissue at the bony-cartilaginous junction (isthmus) of the EAC.
- Cranial nerve palsies (CN VII–XII): CN VII most commonly affected (stylomastoid foramen). Multiple CN deficits = worse prognosis.
- "Picket-fence" spiking fevers with septic thrombophlebitis of the sigmoid sinus.
- Meningeal signs when intracranial spread occurs.
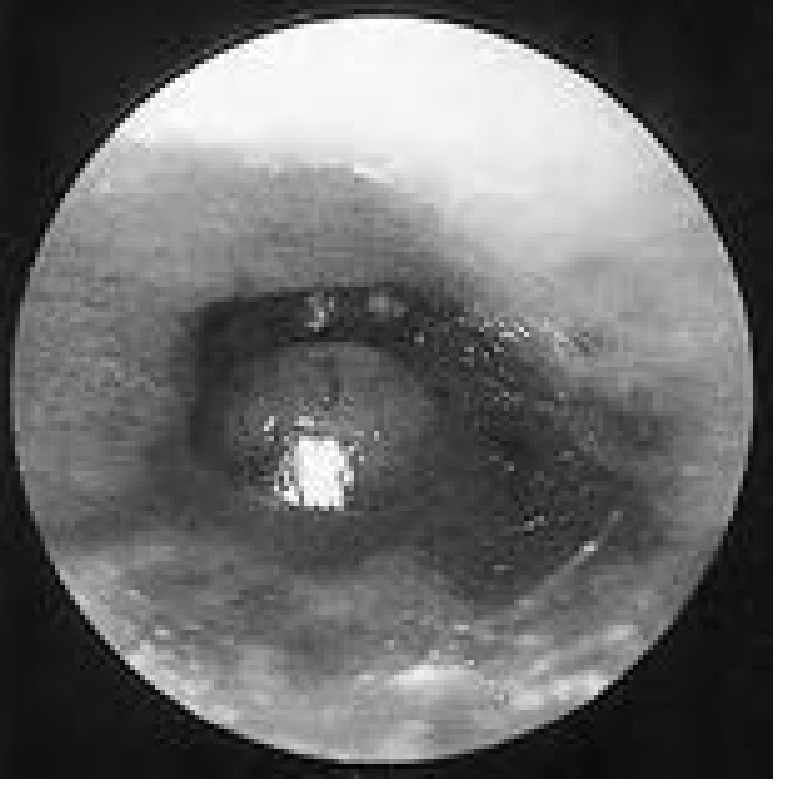
Diagnosis:
- Biopsy granulation tissue — mandatory to exclude squamous cell carcinoma (identical presentation).
- ESR: markedly elevated (nonspecific; used to monitor treatment response and recurrence).
- Bacterial and fungal cultures.
- Imaging:
- CT (first-line): cortical bone erosion, soft-tissue abnormalities around EAC/skull base. Limited for monitoring response (bony changes persist after cure).
- MRI: superior for soft tissue/dural involvement; useful for follow-up.
- Tc-99m bone scan (SPECT): imaging of choice for confirming diagnosis; detects osteoblastic activity before CT shows changes. Cannot distinguish infection from malignancy. Not used for follow-up (remains positive after cure).
- Gallium-67 or In-111 leukocyte scan: shows inflammatory activity; normalizes with treatment — preferred for monitoring response (every 4 weeks).
Treatment:
- Multidisciplinary: otolaryngology, endocrinology, infectious disease, radiology, microbiology.
- Culture-directed, antipseudomonal coverage. Early disease: oral fluoroquinolone (ciprofloxacin). Advanced disease: IV antipseudomonal antibiotics for 6–8 weeks.
- Note: Fluoroquinolone-resistant Pseudomonas is an increasing concern — fluoroquinolones are the only oral agents with antipseudomonal activity.
- Strict glycaemic control in diabetics.
- Surgery: debridement of necrotic tissue; rarely extensive skull base surgery for unresponsive disease.
— K.J. Lee's Essential Otolaryngology, p. 438; Cummings Otolaryngology, pp. 2650–2655
Summary Table
| Category | Key Entity | Hallmark / Distinguishing Feature |
|---|---|---|
| Developmental | Preauricular tag | Most common anomaly; BOR association |
| Developmental | Microtia (Grade III/anotia) | Weerda grade III; rib reconstruction at age 5–6 |
| Developmental | Aural atresia | Jahrsdoefer score guides atresia repair |
| Trauma | Auricular hematoma | I&D + bolster; prevents cauliflower ear |
| Trauma | Frostbite | Slow rewarming; no pressure dressings |
| Foreign body | Vegetable matter | No irrigation; microscopic removal |
| Inflammatory | Acute OE | Topical therapy; wick if canal swollen |
| Inflammatory | Otomycosis | "Wet newspaper" — Aspergillus; clotrimazole |
| Complication | Malignant OE | Granulation at isthmus; diabetic/immunocompromised; CN VII palsy; antipseudomonal Rx |
This is a shared conversation. Sign in to Orris to start your own chat.