CVP and its importantance . Make md anaesthesia notes
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Running Command
Writing File
Here are your comprehensive anaesthesia notes on CVP:
CVP Anaesthesia Notes
MD File · MD
Central Venous Pressure (CVP) — Anaesthesia Notes
1. Definition
CVP = pressure in the superior vena cava / right atrium ≈ right atrial pressure (RAP)
Reflects:
- RV preload
- Circulating blood volume
- Venous tone
- RV performance
Normal CVP: 2–8 mmHg
2. Physiological Basis
| Factor | Effect on CVP |
|---|---|
| Hypovolaemia | ↓ |
| Right heart failure | ↑ |
| Cardiac tamponade | ↑ |
| Tension pneumothorax | ↑ |
| PEEP | ↑ |
| Vasodilation (sepsis, anaesthesia) | ↓ |
| Tricuspid regurgitation | ↑ (ventricularised) |
CVP reflects right-sided heart function — NOT left ventricular performance. (Barash Clinical Anaesthesia 9e)
3. Indications for CVC Insertion
- CVP monitoring in haemodynamically unstable patients and major surgery
- Transvenous cardiac pacing
- Infusion of vasoactive drugs, TPN, chemotherapy, vesicant agents
- Rapid fluid resuscitation (large-bore introducer)
- Pulmonary artery catheterisation
- Aspiration of air emboli
- No peripheral access; repeated blood sampling
4. Access Sites
| Site | Key Points |
|---|---|
| Right IJ | Highest success; direct route to RA/RV; preferred for pacing + PA catheter |
| Subclavian | Highest pneumothorax risk — avoid in emphysema and OLV cases |
| Left IJ / EJ | 3–5 cm longer to SVC; EJ kinks in lateral decubitus (problem in thoracotomy) |
| Femoral | Useful when neck immobilised (trauma); infection risk |
Site selection:
- Coagulopathy → IJ or EJ (compressible); avoid subclavian
- Emergency pacing → right IJ (most direct to RV)
- Trauma with cervical collar → femoral or subclavian
- OLV / thoracic surgery → avoid subclavian; avoid EJ (Barash 9e)
5. CVP Waveform — Normal Components
(Miller's Anaesthesia 10e — Table 32.3)
| Wave | Phase | Mechanical Event | ECG timing |
|---|---|---|---|
| a | End-diastole | Atrial contraction (atrial kick) | After P wave |
| c | Early systole | Tricuspid closure + isovolumic RV contraction | End QRS |
| x descent | Mid-systole | Atrial relaxation + annular descent | Before T wave |
| v | Late systole | Venous atrial filling (tricuspid still closed) | After T wave |
| y descent | Early diastole | Tricuspid opens; RA → RV filling | Before next P |
| h wave | Mid-diastole | Plateau (only at slow HR or high CVP) | — |
Mnemonic: atrial contraction → closure of tricuspid → exit (atrial relaxation) → venous filling → yield to ventricle
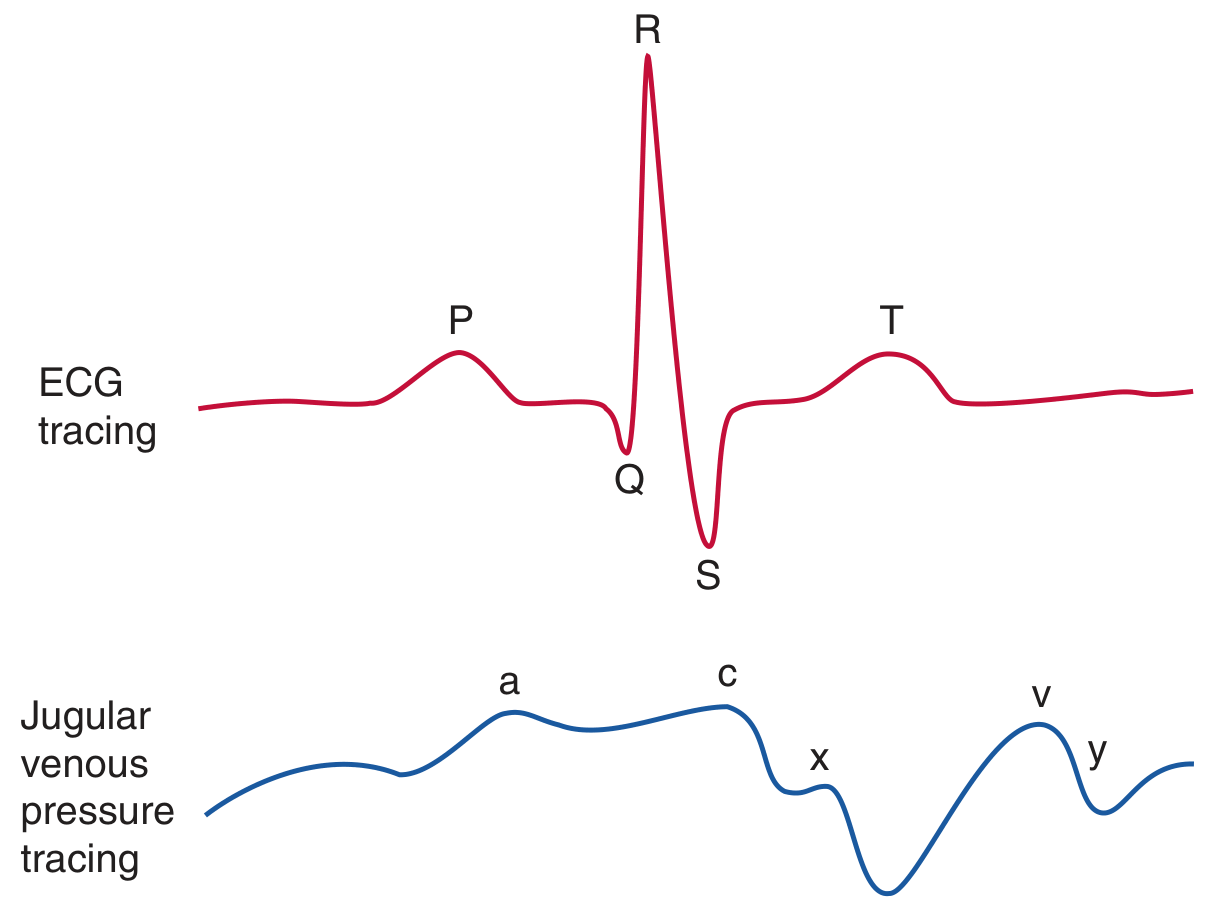
Read CVP at the base of the c wave at end-expiration
6. CVP Waveform Abnormalities
| Condition | Change | Mechanism |
|---|---|---|
| Atrial fibrillation | Loss of a wave | No organised atrial contraction |
| AV dissociation | Cannon a waves | Atrium contracts against closed tricuspid |
| Tricuspid regurgitation | Tall systolic c-v wave; loss of x descent | Regurgitant RA filling in systole |
| Tricuspid stenosis | Tall a wave; attenuated y descent | Impaired diastolic RA emptying |
| Cardiac tamponade | Dominant x descent; absent/attenuated y | Extrinsic compression; impaired diastolic filling |
| Pericardial constriction | Steep x AND y descents; M/W pattern | Exaggerated pressure equalisation |
| RV ischaemia / infarction | Tall a + v; steep x + y; M/W pattern | Reduced RV compliance |
7. Measurement — Practical Points
- Zero reference: 5 cm below sternal angle OR mid-thoracic level (phlebostatic axis)
- Always consistent levelling throughout monitoring period
- Measure at end-expiration (both spontaneous and PPV)
- PEEP artificially elevates CVP — factor this in
- Use ultrasound guidance (strongly recommended; mandatory for IJ per most guidelines) (Miller's 10e)
8. CVP and Fluid Responsiveness
CVP is a POOR predictor of fluid responsiveness. Multiple RCTs and systematic reviews confirm:
- No reliable relationship between CVP and circulating blood volume
- A single static CVP cannot predict haemodynamic response to a fluid bolus
- Guidelines recommend dynamic variables instead:
| Dynamic Variable | Method |
|---|---|
| Pulse pressure variation (PPV) | Arterial line |
| Stroke volume variation (SVV) | LiDCO / Vigileo |
| Passive leg raise (PLR) | Clinical |
| Oesophageal Doppler | Probe |
| Point-of-care echocardiography (POCUS) | TOE / TTE |
(Fishman's Pulmonary 5e; Miller's Anaesthesia 10e)
9. CVP in Shock
| Shock Type | Expected CVP |
|---|---|
| Hypovolaemic | ↓ Low |
| Distributive (sepsis, anaphylaxis) | ↓ Low |
| Cardiogenic (right heart failure) | ↑ High |
| Obstructive (tamponade, tension PTX, massive PE) | ↑ High |
10. Complications
Up to 15% of patients experience some adverse event. (Miller's 10e)
Mechanical
- Arterial puncture (1.9–15%) — most common acute complication
- Pneumothorax (↑ subclavian)
- Haemothorax / hydrothorax / chylothorax (L subclavian)
- Air embolism
- Catheter malposition, arrhythmias (guide wire in RV)
Thromboembolic
- DVT, PE, catheter-related thrombosis
Infectious
- CLABSI (central line-associated bloodstream infection)
- Prevention: chlorhexidine prep, maximal sterile barrier, insertion checklist, daily need review
11. Exam Summary — 10 High-Yield Facts
- CVP = RAP ≈ RV preload — not LV preload
- Normal: 2–8 mmHg; read at end-expiration, base of c wave
- Waveform: a, c, v peaks; x, y descents — timed against ECG
- Cannon a waves = AV dissociation; loss of a = AF; c-v fusion + no x = tricuspid regurgitation
- Tamponade: dominant x descent, absent y — Constriction: steep x AND y (M/W)
- CVP is a poor predictor of fluid responsiveness — dynamic variables preferred
- Right IJ = best site for pacing wires and PA catheters
- Subclavian = highest pneumothorax risk; avoid in emphysema and OLV
- EJ kinks in lateral decubitus — avoid for thoracotomy
- Always use ultrasound guidance; complications occur in up to 15% of insertions
Sources: Miller's Anaesthesia 10e; Barash, Cullen & Stoelting's Clinical Anaesthesia 9e; Fishman's Pulmonary Diseases and Disorders 5e; Morgan & Mikhail's Clinical Anaesthesiology 7e
This is a shared conversation. Sign in to Orris to start your own chat.