Hereditary skin diseases
Reading File
search_medical_text
hereditary skin diseases genetics classification epidermolysis bullosa ichthyosis
search_medical_text
genodermatoses clinical features diagnosis management treatment
search_medical_image
hereditary skin disease genodermatosis clinical presentation
GradeResponse
GradeResponse
GradeResponse
search_medical_text
neurofibromatosis tuberous sclerosis Marfan syndrome skin manifestations genetics
Here is a comprehensive overview of hereditary skin diseases (genodermatoses):
Hereditary Skin Diseases (Genodermatoses)
Genodermatoses are a large group of genetically determined skin disorders, often multisystemic. They are classified by inheritance pattern, molecular defect, or clinical phenotype — though in practice, classification remains "hybrid" in nature (Harrison's, p. 11725).
Classification by Major Category
1. Disorders of Cornification (Ichthyoses)
Characterized by defective skin barrier and abnormal scaling.
| Disease | Inheritance | Gene/Defect | Key Features |
|---|---|---|---|
| Ichthyosis vulgaris | AD | FLG (filaggrin) | Fine scaling, palmoplantar keratoderma, atopic features |
| X-linked ichthyosis | XR | STS (steroid sulfatase) | Large brown scales, trunk/neck, corneal opacities |
| Lamellar ichthyosis | AR | TGM1, others | Collodion baby at birth, plate-like scales over entire body |
| Epidermolytic ichthyosis | AD | KRT1, KRT10 | Blistering at birth, warty hyperkeratosis later |
| Sjögren-Larsson syndrome | AR | ALDH3A2 | Ichthyosis + spastic diplegia + intellectual disability |
2. Epidermolysis Bullosa (EB)
Mechanobullous disorders characterized by skin fragility and blistering with minor trauma. Subtyped by the level of skin cleavage (Harrison's, p. 11725):
| Subtype | Level of Cleavage | Gene/Protein | Features |
|---|---|---|---|
| EB Simplex | Intraepidermal | KRT5, KRT14 (keratins) | Blisters heal without scarring; mildest form |
| Junctional EB | Lamina lucida | LAMA3, LAMB3, LAMC2 (laminins), COL17A1 | Severe; nail/tooth abnormalities; risk of SCC |
| Dystrophic EB | Sub-lamina densa | COL7A1 (collagen VII) | Scarring, pseudosyndactyly ("mitten deformity"), esophageal strictures |
| Kindler syndrome | Multiple levels | FERMT1 (kindlin-1) | Poikiloderma, photosensitivity, mucosal fragility |
3. Disorders of Pigmentation
| Disease | Inheritance | Gene | Key Features |
|---|---|---|---|
| Oculocutaneous albinism (OCA) | AR | TYR, OCA2, others | Hypopigmentation of skin/hair/eyes, photosensitivity, high SCC risk |
| Waardenburg syndrome | AD | PAX3, MITF | White forelock, heterochromia iridis, sensorineural deafness |
| Piebaldism | AD | KIT | White forelock, depigmented patches on trunk/limbs (stable) |
| Incontinentia pigmenti | XLD | IKBKG (NEMO) | Vesicular → verrucous → pigmented → atrophic stages; lethal in males |
4. Neurocutaneous Syndromes (Phakomatoses)
| Disease | Inheritance | Gene | Skin + Systemic Features |
|---|---|---|---|
| Neurofibromatosis type 1 | AD | NF1 (neurofibromin) | Café-au-lait macules (≥6), axillary/inguinal freckling, neurofibromas, Lisch nodules, optic glioma |
| Neurofibromatosis type 2 | AD | NF2 (merlin) | Bilateral acoustic neuromas; fewer café-au-lait spots |
| Tuberous sclerosis | AD | TSC1/TSC2 | Ash-leaf macules, facial angiofibromas, shagreen patches, periungual fibromas; CNS/renal hamartomas |
| Sturge-Weber syndrome | Somatic mosaic | GNAQ | Port-wine stain (V1), leptomeningeal angioma, seizures, glaucoma |
5. Disorders of DNA Repair
| Disease | Inheritance | Gene | Key Features |
|---|---|---|---|
| Xeroderma pigmentosum (XP) | AR | XPC, XPA, others (NER pathway) | Extreme photosensitivity, early-onset skin cancers (BCC, SCC, melanoma), neurological features in some |
| Cockayne syndrome | AR | ERCC6, ERCC8 | Photosensitivity, progeria-like features, intellectual disability; no skin cancer |
| Bloom syndrome | AR | BLM (RecQL helicase) | Photosensitive telangiectatic erythema, growth retardation, high cancer risk |
6. Connective Tissue Disorders with Skin Manifestations
| Disease | Inheritance | Gene | Skin Features |
|---|---|---|---|
| Ehlers-Danlos syndrome (EDS) | AD/AR | COL5A1, COL3A1, etc. | Hyperextensible skin, easy bruising, poor wound healing, joint hypermobility |
| Marfan syndrome | AD | FBN1 (fibrillin-1) | Striae distensae, skin laxity; aortic root dilatation, ectopia lentis |
| Pseudoxanthoma elasticum | AR | ABCC6 | Yellowish papules ("plucked chicken" skin) on neck/flexures; ocular/cardiovascular involvement |
| Cutis laxa | AD/AR | ELN, ATP6AP2, others | Loose, sagging skin; pulmonary/cardiovascular complications |
7. Palmoplantar Keratodermas (PPK)
Marked thickening of palms and soles:
- Unna-Thost (diffuse, non-epidermolytic) — AD, KRT1
- Vörner (diffuse, epidermolytic) — AD, KRT9
- Papillon-Lefèvre syndrome — AR, CTSC (cathepsin C); PPK + aggressive periodontitis
- Mal de Meleda — AR, SLURP1; transgredient (extends to dorsa)
8. Disorders of Vesicle/Pustule Formation
| Disease | Inheritance | Gene | Features |
|---|---|---|---|
| Darier disease | AD | ATP2A2 (SERCA2) | Greasy warty papules in seborrheic areas, nail changes, mucous membrane involvement |
| Hailey-Hailey disease | AD | ATP2C1 (SPCA1) | Recurrent erosions in flexural areas; exacerbated by friction/heat/infection |
| Familial benign pemphigus | AD | Same as Hailey-Hailey | See above |
9. Ectodermal Dysplasias
Affect hair, teeth, nails, and sweat glands:
- Hypohidrotic ED (Christ-Siemens-Touraine) — XLR, EDA gene; sparse hair, absent/cone-shaped teeth, hypohidrosis, characteristic facies
- Hidrotic ED (Clouston syndrome) — AD, GJB6 (connexin 30); alopecia, nail dystrophy, normal sweating
10. Rare/Complex Genodermatoses
| Disease | Key Features |
|---|---|
| Rothmund-Thomson syndrome | Poikiloderma, photosensitivity, cataracts, short stature, increased osteosarcoma risk (RECQL4) |
| Hereditary Fibrosing Poikiloderma (POIKTMP) | Poikilodermatous skin changes, tendon contractures, myopathy, pulmonary fibrosis, lymphedema — a rare genodermatosis distinguished from Rothmund-Thomson by its systemic features |
| Gorlin syndrome (BCNS) | Multiple basal cell carcinomas, jaw keratocysts, skeletal anomalies (PTCH1) |
| Cowden syndrome | Trichilemmomas, oral papillomas, thyroid/breast cancer risk (PTEN) |
Below is a clinical illustration of Hereditary Fibrosing Poikiloderma (POIKTMP), showing the range of skin and systemic manifestations:
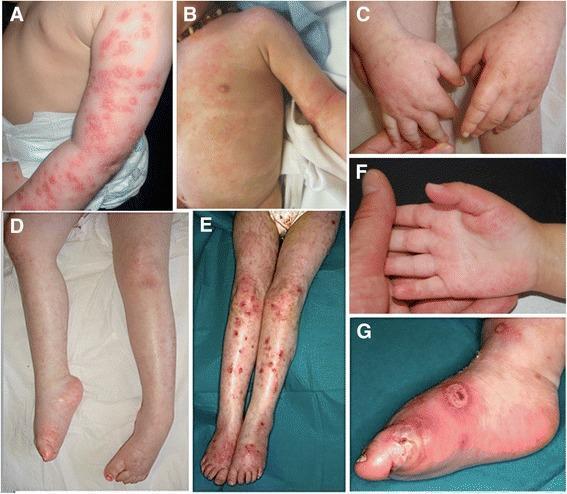
Panels showing erythematous scaly plaques (a–b), chronic lymphedema of hands and lower limbs (c–d, f), and secondary ulcerations/cellulitis (e, g). This multisystemic genodermatosis must be distinguished from Rothmund-Thomson syndrome.
General Principles of Management
- Genetic counseling — essential for all genodermatoses; establish inheritance pattern, recurrence risk, and prenatal testing options.
- Symptomatic skin care — emollients, keratolytics (for ichthyoses), wound care (for EB), sun protection (for XP, OCA, DNA repair disorders).
- Surveillance — skin cancer screening (XP, Gorlin, OCA, Cowden), ophthalmology, cardiology, neurology as indicated by syndrome.
- Emerging therapies:
- Gene therapy — trials ongoing for EB (dystrophic and junctional subtypes)
- mRNA/protein replacement — early stage for some conditions
- Retinoids — for severe ichthyoses and Darier disease
- mTOR inhibitors (everolimus) — for tuberous sclerosis-associated lesions
- Vismodegib (hedgehog inhibitor) — for Gorlin syndrome / extensive BCCs
Key Inheritance Patterns at a Glance
| Pattern | Examples |
|---|---|
| Autosomal dominant (AD) | NF1, tuberous sclerosis, Marfan, EDS (classical), Darier, ichthyosis vulgaris |
| Autosomal recessive (AR) | Lamellar ichthyosis, XP, OCA, junctional EB (most), Papillon-Lefèvre |
| X-linked recessive (XR) | X-linked ichthyosis, hypohidrotic ED (XLR form) |
| X-linked dominant (XLD) | Incontinentia pigmenti (lethal in males) |
| Somatic mosaic | Sturge-Weber, McCune-Albright |
This is a broad field with over 400 recognized genodermatoses. If you'd like a deeper focus on any specific disease — its pathophysiology, diagnostic workup, or management protocols — just ask.
This is a shared conversation. Sign in to Orris to start your own chat.