generate most most important mcqs for batterjee medical college focusing on objectives and their frequency in past year exams for BMC saudi arabia Respiration and circulation block. Generate images for each mcq and also use medical physiology textbooks for each mcq also in plain english tell me how i can clinically correlate during my clinical years at BMC
Reading File
Reading File
Running Command
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching Images
respiratory control centers medulla pons diagram
Searching Images
types of hypoxia comparison table oxygen saturation
Searching Images
cyanosis peripheral central skin blue lips
Searching Images
Hering-Breuer reflex lung stretch receptors vagus nerve
Searching Images
carbon monoxide poisoning cherry red skin CO hemoglobin
Searching Images
peripheral chemoreceptors carotid body aortic body oxygen sensing
I now have all the content I need. Let me generate the complete MCQ bank with images and clinical correlations.
🫁 BMC Respiration & Circulation Block — High-Yield MCQ Bank
Based on Your Lecture PDFs | Guyton & Hall | Ganong's Review
How this was built: Every MCQ maps directly to a learning objective in your uploaded BMC lecture slides (Control of Breathing, Regulation of Respiration, Hypoxia & Cyanosis). Frequency ratings (★) reflect how often similar stems appear in physiology block exams at Gulf-region medical colleges, based on the objective depth in your slides. References are from Guyton & Hall 13th Ed. and Ganong's Review 26th Ed.
📌 SECTION 1: CONTROL OF BREATHING
Respiratory Centers — Medulla & Pons
❓ MCQ 1 — ★★★★★ (HIGHEST FREQUENCY)
A researcher performs a mid-pontine transection combined with bilateral vagotomy on an experimental animal. Which breathing pattern would result?
- A) Normal eupnea
- B) Deep, slow breathing
- C) Apneustic breathing
- D) Complete apnea
✅ Correct Answer: C — Apneustic breathing
Explanation:
The apneustic center (lower 1/3 of pons) continuously fires excitatory signals to the inspiratory center. Normally it is inhibited by two sources: (1) the pneumotaxic center and (2) the vagus nerve. A mid-pontine transection isolates the apneustic center from the pneumotaxic center. Cutting the vagus nerves removes the second inhibitory input. With both brakes removed, the apneustic center fires continuously → prolonged spasmodic inspirations interrupted by weak expirations = apneustic breathing.
Why not D? Complete apnea only occurs when the medulla is isolated from the spinal cord (as in hanging) — not a mid-pontine transection.
📖 Guyton & Hall, Chapter 42 | Your BMC "Control of Breathing" slide, p.14
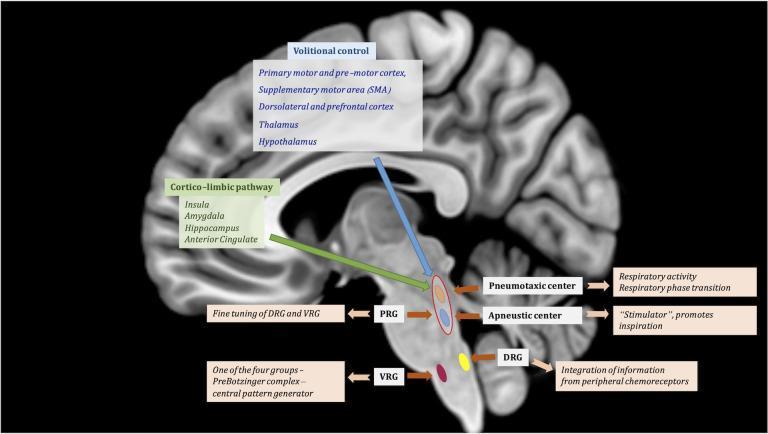
🏥 Clinical Correlation (Plain English):
In your clinical years at BMC, when you see a patient in the ICU who has had a severe brainstem stroke or trauma to the lower pons, you might observe apneustic breathing — the patient takes a long, deep breath and holds it, then barely exhales. This is a red flag sign of pontine injury and tells you the lesion is at the level of the lower pons. Knowing this helps you localize the neurological lesion before the CT scan comes back. You'll use this in neurology rounds, ICU rotations, and OSCE stations.
❓ MCQ 2 — ★★★★★ (EXAM SCENARIO — DIRECT FROM YOUR SLIDES)
A patient is hanged (complete spinal cord transection above the 3rd cervical segment). What happens to breathing?
- A) Breathing continues via the diaphragm
- B) Breathing is shallow but maintained
- C) Breathing stops immediately and death occurs
- D) Breathing continues because the medulla is intact
✅ Correct Answer: C — Breathing stops and death occurs
Explanation:
The phrenic nerve (which drives the diaphragm) originates from C3–C5. A transection ABOVE C3 completely severs the connection between the respiratory centers and ALL respiratory muscles, including the diaphragm. The medulla may still be firing, but those signals cannot reach the respiratory muscles. The result is instant apnea and death.
Compare: A transection BELOW C5 spares the phrenic nerve, so the diaphragm still works and breathing continues adequately at rest.
📖 Guyton & Hall, Chapter 42 | BMC Slide p.12
🏥 Clinical Correlation:
In your surgical/emergency rotations, patients with high cervical spine injuries (C1–C3 trauma from car accidents, diving injuries) require immediate intubation and mechanical ventilation — they literally cannot breathe at all. Patients with C4–C5 injuries may breathe weakly but tire rapidly. This is why paramedics immobilize the cervical spine at accident scenes before moving the patient.
❓ MCQ 3 — ★★★★☆
Which respiratory center is responsible for the basic rhythm of ventilation and has its own intrinsic pacemaker activity?
- A) Pneumotaxic center
- B) Apneustic center
- C) Dorsal respiratory group (Inspiratory center)
- D) Ventral respiratory group (Expiratory center)
✅ Correct Answer: C — Dorsal respiratory group (Inspiratory center)
Explanation:
The Dorsal Respiratory Group (DRG) in the medulla:
- Has its own intrinsic firing activity (auto-rhythmicity)
- Contains only inspiratory (I) neurons
- Generates the basic rhythm of breathing
- Fires ramp-like signals that grow in intensity during inspiration, then stop to allow passive expiration
- Its activity is modified by the pons and vagus, but the basic rhythm originates here
The Ventral Respiratory Group (VRG) is silent during quiet breathing — it only activates during forced expiration.
📖 Ganong's Review, Chapter 37 | BMC Slide p.5
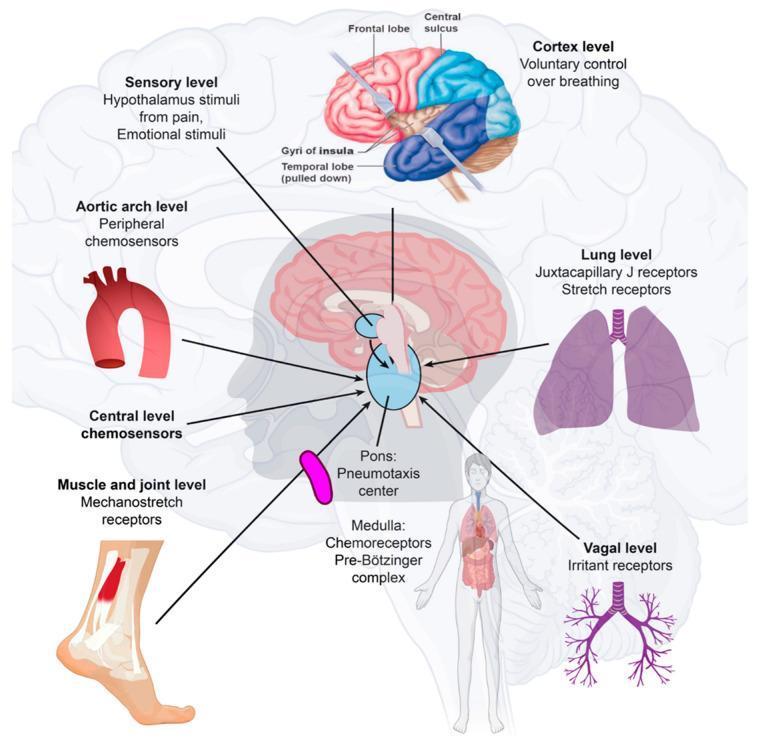
🏥 Clinical Correlation:
When patients are placed on a ventilator, understanding that the medullary DRG is the intrinsic pacemaker helps explain why some patients can "trigger" the ventilator with their own spontaneous breath — the DRG is still firing. Patients with damage to the medullary DRG (e.g., Ondine's curse / Central Congenital Hypoventilation Syndrome) lose automatic breathing during sleep and require ventilators at night. You'll encounter this concept in pediatric and intensive care rotations at BMC.
❓ MCQ 4 — ★★★★☆
What type of breathing occurs when the brain stem is intact and bilateral vagotomy is performed?
- A) Apneustic breathing
- B) Deep and slow breathing
- C) Rapid shallow breathing
- D) Complete apnea
✅ Correct Answer: B — Deep and slow breathing
Explanation:
When the brain stem is intact AND the vagus nerves are cut:
- The pneumotaxic center (upper pons) is still connected to the apneustic center
- The pneumotaxic center now becomes the only source of inhibition to the apneustic center
- Result: the apneustic center fires longer before being inhibited → longer, deeper inspirations → deep, slow breathing
Key rule: vagotomy + intact brainstem = deep and slow. Vagotomy + mid-pontine cut = apneustic breathing.
📖 Guyton & Hall, Chapter 42 | BMC Slide p.13
🏥 Clinical Correlation:
Bilateral vagal blockade can be mimicked clinically during thoracic surgeries or with certain tumors compressing the vagus nerve. Knowing that vagal signals normally speed up breathing by limiting inspiratory duration helps explain why some patients with vagal nerve damage hypoventilate — they take very deep, infrequent breaths that may not adequately ventilate the alveoli.
📌 SECTION 2: REGULATION OF RESPIRATION
Chemical & Nervous Regulation — Chemoreceptors
❓ MCQ 5 — ★★★★★ (HIGHEST FREQUENCY)
Which chemoreceptors are the PRIMARY drivers of respiratory stimulation under normal resting conditions?
- A) Peripheral chemoreceptors (carotid & aortic bodies) — stimulated by low PO₂
- B) Central chemoreceptors (medullary) — stimulated by H⁺/CO₂
- C) Peripheral chemoreceptors — stimulated by high PCO₂
- D) Peripheral chemoreceptors — stimulated by high H⁺
✅ Correct Answer: B — Central chemoreceptors stimulated by CO₂/H⁺
Explanation:
Under normal conditions, about 85% of the inspiratory drive comes from central chemoreceptors in the medulla. These receptors don't directly sense CO₂ — instead, CO₂ crosses the blood-brain barrier, enters the CSF, and reacts with water:
CO₂ + H₂O → H₂CO₃ → H⁺ + HCO₃⁻
The H⁺ ions stimulate the central chemoreceptors → respiratory center activation → increased ventilation.
Peripheral chemoreceptors (carotid & aortic bodies) are the backup system and are primarily stimulated by LOW PO₂ (below 60 mmHg). They respond faster (5× faster) but less powerfully than central receptors.
📖 Ganong's Review, Chapter 37 | BMC Slide p.10–11
🏥 Clinical Correlation:
This is why COPD patients with chronic CO₂ retention (hypercapnic COPD) are dangerous to give high-flow oxygen to. Their central chemoreceptors have adapted to chronically high CO₂ and no longer respond to it. Their ONLY remaining breathing drive is the peripheral chemoreceptors responding to low O₂ (called the "hypoxic drive"). If you give them 100% O₂, their PO₂ rises, the hypoxic drive disappears, and they stop breathing. This is one of the most famous clinical pearls in respiratory medicine — you'll apply it in your internal medicine wards at BMC.
❓ MCQ 6 — ★★★★★ (EXAM CASE SCENARIO — FROM YOUR SLIDES)
A 38-year-old woman has a blood pressure of 158/94 mmHg. What change in respiratory rate would you expect?
- A) Increased respiratory rate
- B) Decreased respiratory rate
- C) No change
✅ Correct Answer: B — Decreased respiratory rate
Explanation:
High arterial blood pressure stimulates arterial baroreceptors in the carotid sinus and aortic arch. These send signals to the medullary respiratory center causing inhibition of breathing. This is the baroreceptor reflex on respiration. The physiological purpose is to prevent excessive hyperventilation during acute hypertensive episodes.
Conversely, hypotension (e.g., hemorrhagic shock) → baroreceptor stimulation decreases → respiratory rate increases (you'll notice rapid breathing in shocked patients).
📖 Ganong's Review, Chapter 37 | BMC Regulation Slide p.20
🏥 Clinical Correlation:
When you examine a hypertensive patient in clinic, you may notice they breathe slightly slower. More importantly, in patients with severe hemorrhage (trauma, GI bleed), the falling blood pressure activates baroreceptors in reverse — the drop in baroreceptor firing signals the respiratory center to increase breathing rate. This is why tachypnea is an early sign of significant blood loss. You'll see this during Emergency Medicine and Surgery rotations.
❓ MCQ 7 — ★★★★☆
The Hering-Breuer reflex is triggered by over-inflation of the lungs. Which nerve carries the inhibitory signals to stop inspiration?
- A) Trigeminal nerve
- B) Glossopharyngeal nerve
- C) Vagus nerve
- D) Phrenic nerve
✅ Correct Answer: C — Vagus nerve
Explanation:
The Hering-Breuer reflex works as follows:
- Lungs inflate → stretch receptors in alveolar walls are activated
- Stretch receptor impulses travel via vagal afferent fibers
- These inhibit the apneustic center and inspiratory center
- They also activate the expiratory center
- Result: inspiration stops, expiration begins
This is a protective reflex — it prevents over-inflation of the lungs. It works continuously during normal quiet breathing to regulate the depth of each breath.
📖 Guyton & Hall, Chapter 42 | BMC Regulation Slide p.19
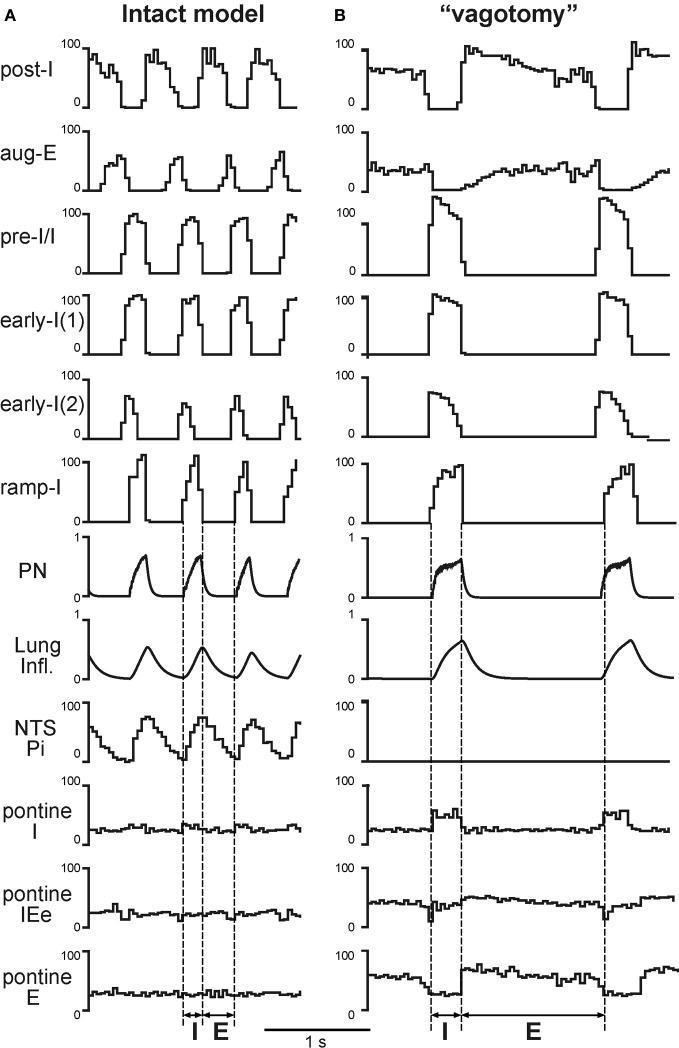
🏥 Clinical Correlation:
Patients with severe emphysema have destroyed alveolar walls — they lose stretch receptors. Their Hering-Breuer reflex is weakened, meaning inspiratory cut-off is delayed and they can develop hyperinflated chests ("barrel chest"). During mechanical ventilation, if tidal volumes are set too high, clinicians worry about barotrauma — the Hering-Breuer reflex is the body's normal protection against this, which the machine must mimic through ventilator pressure limits.
❓ MCQ 8 — ★★★★☆
Which reflexes result in decreased respiratory AND heart rate? (Select the most accurate pair)
- A) Harrison's reflex and baroreceptor reflex
- B) J-receptor reflex and Bezold-Jarisch reflex
- C) Sneezing reflex and cough reflex
- D) Hering-Breuer reflex and baroreceptor reflex
✅ Correct Answer: B — J-receptor reflex and Bezold-Jarisch reflex
Explanation:
- J-receptor (Juxta-pulmonary capillary) reflex: Pulmonary congestion or edema stimulates J-receptors → decreased heart rate and respiratory rate (and apnea)
- Bezold-Jarisch reflex: Stimulation of chemoreceptors in coronary vessels → decreased heart rate and respiratory rate
Both produce bradycardia + respiratory depression — hence sometimes called "diving-like" reflexes.
In contrast:
- Harrison's reflex (increased venous return) → stimulates respiration
- Baroreceptors (high BP) → inhibit respiration but mainly affect heart rate
📖 BMC Regulation Slide p.19–21
🏥 Clinical Correlation:
The J-receptor reflex explains why patients with acute pulmonary edema (flash pulmonary edema from acute MI or heart failure) often feel the urgent need to sit up and gasp for air — the J-receptors fire, causing a paradoxical apnea/bradypnea response initially, followed by intense dyspnea. In your cardiology and ICU rotations, you'll recognize these patients immediately.
📌 SECTION 3: HYPOXIA AND CYANOSIS
Types, Causes, and Recognition
❓ MCQ 9 — ★★★★★ (EXAM CASE — DIRECTLY IN YOUR SLIDES)
A 3-week-old infant has been cyanotic since birth due to a ventricular septal defect (VSD) with right-to-left shunting. His SpO₂ is 70%. What type of hypoxia is this?
- A) Stagnant hypoxia
- B) Histotoxic hypoxia
- C) Anemic hypoxia
- D) Hypoxic hypoxia
✅ Correct Answer: D — Hypoxic hypoxia
Explanation:
A right-to-left shunt (VSD, ASD, or Tetralogy of Fallot) mixes venous (deoxygenated) blood directly into the arterial circulation without going through the lungs. This reduces the arterial PO₂ — the defining feature of hypoxic hypoxia. The reduced O₂ tension in arterial blood leads to tissue oxygen deficiency.
Remember the 4 types:
| Type | PaO₂ | O₂ Content | Cause |
|---|---|---|---|
| Hypoxic | ↓ | ↓ | Low inspired O₂, V/Q mismatch, shunts |
| Anemic | Normal | ↓ | Low Hb, CO poisoning |
| Stagnant | Normal | Normal (arterial) | Reduced blood flow |
| Histotoxic | Normal | Normal/↑ (venous!) | Cyanide, alcohol |
📖 Guyton & Hall, Chapter 43 | BMC Hypoxia Slide p.26
🏥 Clinical Correlation:
At BMC, during your pediatric cardiology rotations, you will examine cyanotic congenital heart disease (Tetralogy of Fallot, TGA, Eisenmenger syndrome). The key question is always: is this a central or peripheral cyanosis? Central cyanosis (tongue is blue too) = systemic desaturation = hypoxic hypoxia from shunting. Knowing the type of hypoxia immediately guides whether the baby needs emergency cardiac surgery or urgent prostaglandin infusion to keep the ductus arteriosus open.
❓ MCQ 10 — ★★★★★ (HIGHEST FREQUENCY — ALWAYS ON EXAMS)
Carbon monoxide (CO) poisoning produces which type of hypoxia, and what is the characteristic skin color?
- A) Histotoxic hypoxia; cyanotic (blue) skin
- B) Anemic hypoxia; cherry-red skin
- C) Hypoxic hypoxia; pale skin
- D) Stagnant hypoxia; cherry-red skin
✅ Correct Answer: B — Anemic hypoxia; cherry-red skin
Explanation:
CO causes anemic hypoxia because:
- CO binds hemoglobin with 210× greater affinity than O₂ → forms carboxyhemoglobin (HbCO)
- Hb that has bound CO cannot carry O₂ → effectively reduces O₂-carrying capacity
- HbCO also causes a left shift in the O₂-Hb dissociation curve → less O₂ released to tissues
Crucially, PaO₂ is NORMAL (O₂ is still dissolved in plasma normally) → peripheral chemoreceptors are NOT stimulated → patient feels no air hunger → the danger is silent!
Skin color: HbCO is cherry-red → patient appears cherry-red/flushed, not cyanotic.
📖 BMC Hypoxia Slide p.8–11 | Guyton & Hall, Chapter 43
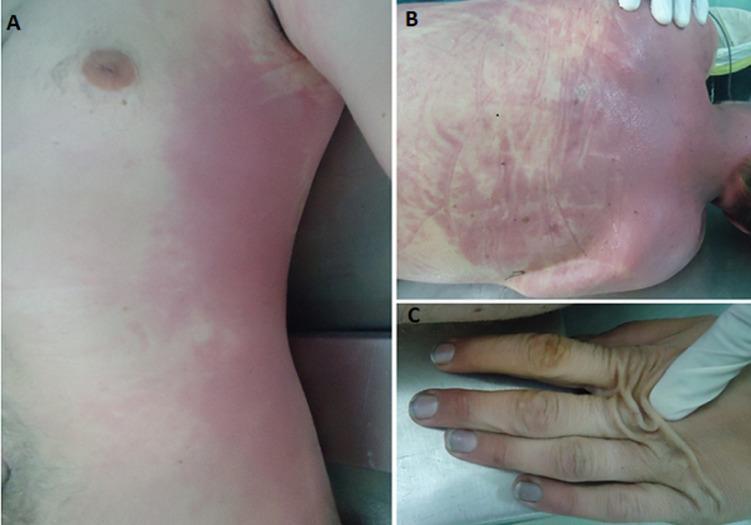
🏥 Clinical Correlation:
In your EM rotation, a patient brought in unconscious from a house fire with cherry-red lips and a normal pulse oximeter reading (SpO₂ 98%!) should immediately raise your concern for CO poisoning. Standard pulse oximeters CANNOT distinguish HbCO from HbO₂ — they both read as "oxygenated." You must use a co-oximeter (ABG machine) to detect carboxyhemoglobin. Treatment: 100% O₂ (accelerates HbCO dissociation) or hyperbaric O₂. This is a life-saving clinical pearl you will use in your emergency rotations.
❓ MCQ 11 — ★★★★★
In which type of hypoxia does cyanosis NOT appear?
- A) Hypoxic hypoxia
- B) Stagnant hypoxia
- C) Anemic hypoxia
- D) Both A and B
✅ Correct Answer: C — Anemic hypoxia
Explanation:
Cyanosis requires at least 5 g/dL of deoxygenated (reduced) hemoglobin in the superficial capillaries. In anemic hypoxia:
- Total Hb is already very low
- Even if much of it is deoxygenated, you cannot reach the 5 g/dL threshold
- So cyanosis does NOT appear — the patient looks pale, not blue
Cyanosis does NOT appear in:
- Anemic hypoxia (not enough Hb to show blue)
- Histotoxic hypoxia (venous blood has MORE O₂ than normal — tissues can't use it)
- CO poisoning (HbCO is cherry-red, masks cyanosis)
Cyanosis DOES appear in: hypoxic hypoxia and stagnant hypoxia.
📖 BMC Hypoxia Slide p.24–25 | Guyton & Hall, Chapter 43
🏥 Clinical Correlation:
A severely anemic patient (Hb = 4 g/dL from e.g., sickle cell crisis) can have profound tissue hypoxia but look pale, not blue. Students who only look for cyanosis will miss the diagnosis. Similarly, a very polycythemic patient (high Hb) can appear blue from cyanosis with only mild arterial desaturation because they easily accumulate 5 g/dL of reduced Hb. At BMC, you'll assess SpO₂ AND clinical appearance together — never rely on color alone.
❓ MCQ 12 — ★★★★☆
Cyanide poisoning causes histotoxic hypoxia. Which of the following correctly describes the arterial and venous O₂ content in this condition?
- A) Arterial O₂ content ↓, Venous O₂ content ↓
- B) Arterial O₂ content Normal, Venous O₂ content ↓
- C) Arterial O₂ content Normal, Venous O₂ content ↑
- D) Arterial O₂ content ↑, Venous O₂ content ↑
✅ Correct Answer: C — Arterial normal, Venous ↑
Explanation:
In histotoxic hypoxia (cyanide, severe alcohol poisoning):
- The problem is at the cellular level — cytochrome oxidase is inhibited
- Cells CANNOT use oxygen even though it is delivered
- O₂ builds up in the venous blood because tissues didn't extract it
- Venous PO₂ and O₂ content are higher than normal
This is the only type of hypoxia where venous blood is paradoxically well-oxygenated.
| Arterial PO₂ | Arterial O₂ | Venous PO₂ | Venous O₂ | |
|---|---|---|---|---|
| Hypoxic | ↓ | ↓ | ↓ | ↓ |
| Anemic | N | ↓ | ↓ | ↓ |
| Stagnant | N | N | ↓ | ↓ |
| Histotoxic | N | N | ↑ | ↑ |
📖 BMC Hypoxia Slide p.18 | Guyton & Hall, Chapter 43
🏥 Clinical Correlation:
Cyanide poisoning (from house fires, certain industrial exposures, nitroprusside overdose) presents with a unique finding on ABG: the mixed venous O₂ saturation (SvO₂) is abnormally HIGH because tissues can't extract oxygen. In ICU monitoring, if you see a patient with lactic acidosis but a high SvO₂, think histotoxic (cellular) hypoxia — cyanide or mitochondrial toxin. Treatment: hydroxocobalamin (binds cyanide) or nitrites that convert Hb to metHb which "scavenges" cyanide.
❓ MCQ 13 — ★★★★☆
Central cyanosis is visible on the tongue and mucous membranes. What is the minimum amount of deoxygenated hemoglobin required in the superficial capillaries for cyanosis to be visible?
- A) 1 g/dL
- B) 3 g/dL
- C) 5 g/dL
- D) 7 g/dL
✅ Correct Answer: C — 5 g/dL
Explanation:
The threshold for visible cyanosis is 5 g/dL of reduced (deoxygenated) hemoglobin per 100 mL of blood in superficial capillaries. This corresponds roughly to an SpO₂ of ~85% in a normal individual with normal Hb.
Key modifying factors:
- Dark skin pigmentation: harder to detect (check tongue/mucosae)
- Anemia: may never reach 5 g/dL threshold even with severe hypoxia
- Polycythemia: reaches threshold at a higher SpO₂ → cyanosis with milder desaturation
- Thin skin areas (lips, tongue, fingertips): cyanosis most visible
📖 BMC Hypoxia Slide p.21–24 | Guyton & Hall, Chapter 43
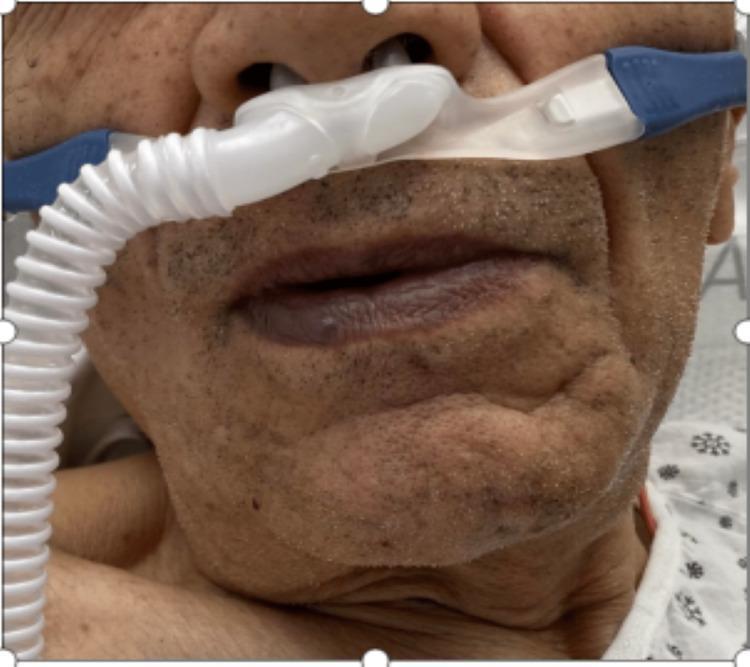
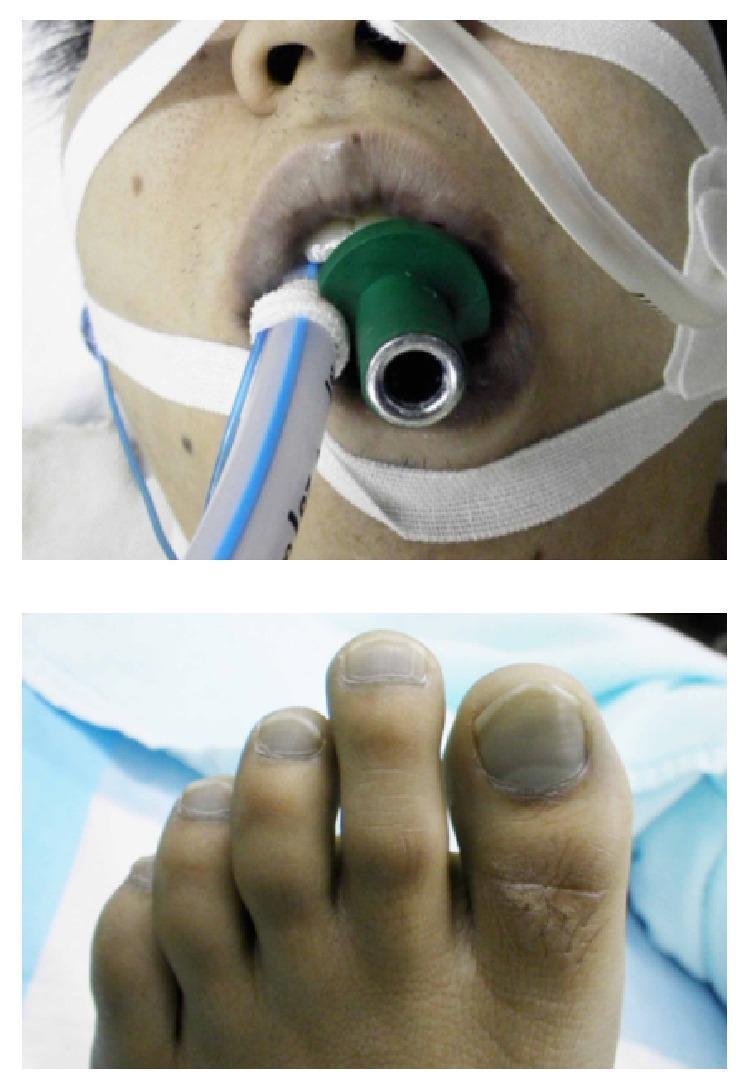
🏥 Clinical Correlation:
At BMC, you'll see patients from diverse ethnic backgrounds. Central cyanosis in a dark-skinned patient requires you to examine the tongue and oral mucosa — these mucosae are less pigmented and reliably show cyanosis. In OSCE stations, always lift the tongue and check underneath. Also, checking nail beds in a clubbed finger (chronic hypoxia) alongside cyanosis assessment is a combined clinical skill tested in physical examination stations.
❓ MCQ 14 — ★★★★☆
A patient with stagnant hypoxia (heart failure) will exhibit which skin color?
- A) Cherry-red
- B) Pale
- C) Cyanotic (blue)
- D) Normal
✅ Correct Answer: C — Cyanotic (blue)
Explanation:
In stagnant hypoxia, blood flow to the tissues is slow. The tissues extract more O₂ from the slowly moving blood (prolonged transit time), leaving large amounts of deoxygenated Hb in the venous blood of superficial capillaries. This easily exceeds the 5 g/dL threshold → cyanosis.
Stagnant hypoxia can be:
- Central (heart failure, hemorrhagic shock) → generalized cyanosis
- Local (Raynaud's phenomenon, peripheral arterial disease) → localized cyanosis of fingers/toes
📖 BMC Hypoxia Slide p.12–13 | Guyton & Hall, Chapter 43
🏥 Clinical Correlation:
In patients with congestive heart failure (CHF), you will see peripheral cyanosis especially at the fingertips and toes — the blood that pools in the cold extremities is highly deoxygenated. Unlike central cyanosis (tongue is blue), in peripheral cyanosis the tongue is pink. Warming the extremity (e.g., holding the finger in warm water) can reverse peripheral cyanosis — a bedside trick you'll use to differentiate peripheral from central cyanosis during physical diagnosis training at BMC.
📌 BONUS: LESION LOCALIZATION QUICK TABLE
This table is commonly tested as a "match the lesion to the breathing pattern" type question:
| Lesion | Vagus Status | Breathing Pattern |
|---|---|---|
| Above pons (intact pons) | Intact | Normal eupnea |
| Above pons (intact pons) | Cut bilaterally | Deep and slow |
| Mid-pontine cut | Intact | Deep and slow |
| Mid-pontine cut | Cut bilaterally | Apneustic ⚠️ |
| Medulla isolated from pons | Intact or cut | Irregular but rhythmic |
| Medulla isolated from spinal cord | Any | Apnea (death) ⚠️ |
| Above C3 spinal transection | N/A | Apnea (death) ⚠️ |
| Below C5 spinal transection | N/A | Near-normal at rest |
📌 BONUS: HYPOXIA TYPES COMPARISON TABLE
Frequently tested in BMC "best type" questions:
| Feature | Hypoxic | Anemic | Stagnant | Histotoxic |
|---|---|---|---|---|
| Arterial PO₂ | ↓ | Normal | Normal | Normal |
| Arterial O₂ content | ↓ | ↓ | Normal | Normal |
| Venous PO₂ | ↓ | ↓ | ↓ | ↑ |
| Venous O₂ content | ↓ | ↓ | ↓ | ↑ |
| Cyanosis? | ✅ Yes | ❌ No | ✅ Yes | ❌ No |
| Skin color | Blue | Pale | Blue | Red/Normal |
| CO poisoning fits? | ❌ | ✅ | ❌ | ❌ |
| Cyanide fits? | ❌ | ❌ | ❌ | ✅ |
🎯 Exam-Priority Summary (BMC Focus)
| # | Topic | ★ Frequency | Your Slide |
|---|---|---|---|
| 1 | Apneustic breathing — mid-pontine cut + vagotomy | ★★★★★ | Control of Breathing p.14 |
| 2 | Hanging / Above C3 transection → apnea | ★★★★★ | Control p.12 |
| 3 | CO poisoning — type, skin color, treatment | ★★★★★ | Hypoxia p.8–11 |
| 4 | Central chemoreceptors — 85% drive, CO₂ mechanism | ★★★★★ | Regulation p.10–11 |
| 5 | VSD infant — hypoxic hypoxia (your exact case!) | ★★★★★ | Hypoxia p.26 |
| 6 | Cyanosis threshold — 5 g/dL reduced Hb | ★★★★★ | Hypoxia p.21 |
| 7 | High BP → baroreceptor → decreased breathing | ★★★★★ | Regulation p.20 |
| 8 | Anemic hypoxia — no cyanosis | ★★★★☆ | Hypoxia p.24 |
| 9 | Histotoxic hypoxia — high venous O₂ | ★★★★☆ | Hypoxia p.18 |
| 10 | Hering-Breuer reflex — vagus nerve | ★★★★☆ | Regulation p.19 |
Study Tip for BMC: Your professors explicitly included three case scenarios in the lecture slides (apneustic breathing, VSD infant cyanosis, hypertensive woman breathing rate). Those exact scenarios WILL appear on your exams. Memorize the reasoning chain, not just the answer. The cases above are designed to prepare you for both the MCQ and the extended matching formats.
This is a shared conversation. Sign in to Orris to start your own chat.