A 30 yr old male came with Redness of skin in groin area due to high friction in summer . Associated with itching. Management and diagnosis.
Reading File
Finding Sources
Finding Sources
Searching Images
tinea cruris intertrigo groin rash
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Finding Sources
I now have everything needed for a thorough, well-sourced answer.
Diagnosis: Tinea Cruris (Jock Itch / Eczema Marginatum)
This presentation — a 30-year-old male with groin erythema, pruritus, and exacerbation by heat/friction/summer humidity — is classic for tinea cruris, a dermatophyte infection of the groin, genitalia, pubic area, and perineal skin. It is the second most common dermatophytosis worldwide and is 3× more common in men. - Fitzpatrick's Dermatology, p. 2975
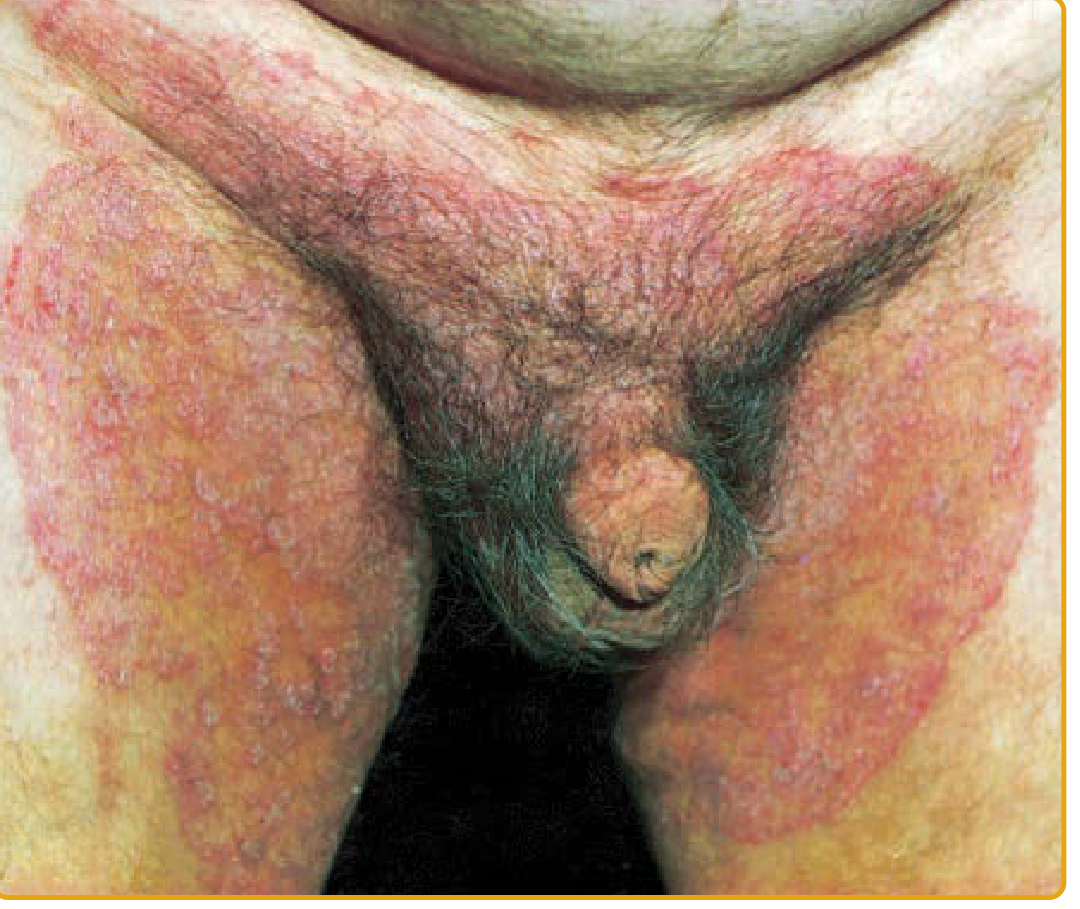
Fig. 160-11 Tinea cruris — Fitzpatrick's Dermatology
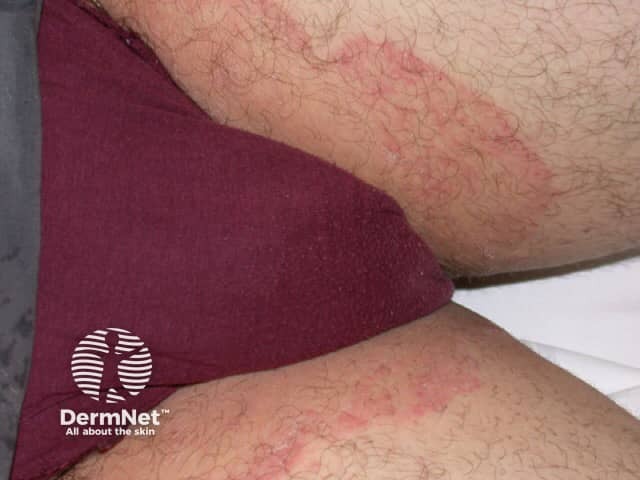
Etiology
| Organism | Notes |
|---|---|
| Trichophyton rubrum | Most common; extends to pubic, perianal, buttock areas |
| Epidermophyton floccosum | More likely to show central clearing; responsible for epidemics |
| T. mentagrophytes / T. interdigitale | Less common |
Spread: direct contact, fomites, and importantly autoinoculation from tinea pedis (patient picks up infection from feet when putting on underwear). - Andrews' Diseases of the Skin, p. 1997
Clinical Features
- Well-demarcated annular/crescent plaque with a raised, scaly, active advancing border
- Extends from the inguinal fold → inner thighs → may involve perineum/perianal area
- Scrotum typically spared (key distinguishing feature from candidiasis and inverse psoriasis)
- Pruritus prominent; pain if macerated or secondarily infected
- Exacerbated by heat, humidity, tight clothing, and summer season
Differential Diagnosis
| Condition | Distinguishing Features |
|---|---|
| Candidal intertrigo | Moister, brighter red; satellite pustules/papules; involves scrotum; collarette scales |
| Erythrasma (Corynebacterium minutissimum) | Copper-brown color; coral-red fluorescence on Wood's lamp |
| Inverse psoriasis | Well-demarcated; may show serpiginous pustules; look for psoriasis elsewhere; does NOT respond to antifungals |
| Seborrheic dermatitis | Also involves chest, axillae, scalp |
| Contact/irritant dermatitis | History of irritant exposure; no advancing border |
| Lichen simplex chronicus | Lichenification from chronic scratching |
- Fitzpatrick's Dermatology, Table 160-18; Andrews' Diseases of the Skin, p. 2001
Diagnosis
| Test | Finding |
|---|---|
| KOH preparation (scraping from leading edge) | Branching septate hyphae — gold standard, quick office test |
| Fungal culture | Species identification; takes 2–4 weeks |
| Wood's lamp | Negative for tinea cruris (positive coral-red for erythrasma) |
| Skin biopsy | Reserved for diagnostic uncertainty |
Scrape the leading edge of the plaque, not the center. Avoid scraping if patient has already applied topical antifungals — can give false negatives. - Tintinalli's Emergency Medicine, p. 1694
Management
1. Topical Antifungals (First-line for localized disease)
| Drug | Class | Regimen |
|---|---|---|
| Terbinafine 1% cream/gel | Allylamine (fungicidal) | Once daily × 1–2 weeks |
| Clotrimazole 1% cream | Azole | Twice daily × 2–4 weeks |
| Miconazole 2% cream | Azole | Twice daily × 2–4 weeks |
| Ketoconazole 2% cream | Azole | Once–twice daily × 2–4 weeks |
| Econazole 1% cream | Azole (also antibacterial) | Preferred if maceration present |
| Butenafine 1% cream | Allylamine derivative | Once daily × 2 weeks |
Allylamines (terbinafine, naftifine, butenafine) are fungicidal and show superior mycologic cure rates vs. azoles. - Dermatology 2-Volume Set 5e; Katzung Pharmacology 16e
2. Systemic Antifungals (For extensive, recurrent, or refractory disease)
| Drug | Dose | Duration |
|---|---|---|
| Terbinafine 250 mg/day PO | Fewer drug interactions | 2–4 weeks |
| Itraconazole 100 mg/day PO | More drug interactions | 1–6 weeks |
| Fluconazole 150 mg/week PO | Weekly dosing | As per response |
Terbinafine is generally preferred over itraconazole due to fewer drug interactions. - Harrison's Principles of Internal Medicine 22E, p. 1258
3. General / Preventive Measures (Critical for recurrence prevention)
- Keep the area dry: powder application daily (plain talc or antifungal powder)
- Loose-fitting cotton underwear and clothing: reduces friction, heat, and occlusion
- Treat tinea pedis concurrently if present (common co-infection)
- Advise patient to put on socks before underwear to prevent autoinoculation from feet
- Apply a zinc-containing barrier cream to protect skin in the groin fold
- Regular bathing; dry thoroughly after washing
- Avoid sharing towels, clothing
- Fitzpatrick's Dermatology, p. 2976; Andrews' Diseases of the Skin, p. 2003
4. Follow-up
- If no resolution in 4–6 weeks: refer to dermatologist; consider systemic therapy or re-evaluate diagnosis
- Recurrence is common without addressing predisposing factors (tinea pedis, obesity, hyperhidrosis)
Summary Table
| Diagnosis | Tinea cruris (jock itch) |
| Causative organism | T. rubrum, E. floccosum |
| Confirmatory test | KOH prep → branching hyphae |
| First-line Rx | Topical terbinafine or azole × 2–4 weeks |
| Systemic Rx | Oral terbinafine 250 mg/day if extensive |
| Key adjunct | Keep area dry, loose clothing, treat tinea pedis |
This is a shared conversation. Sign in to Orris to start your own chat.