Describe clavicular nerve
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Finding Sources
Reading File
Reading File
I now have comprehensive information to give a thorough answer. Here is a complete description of the clavicular (supraclavicular) nerves:
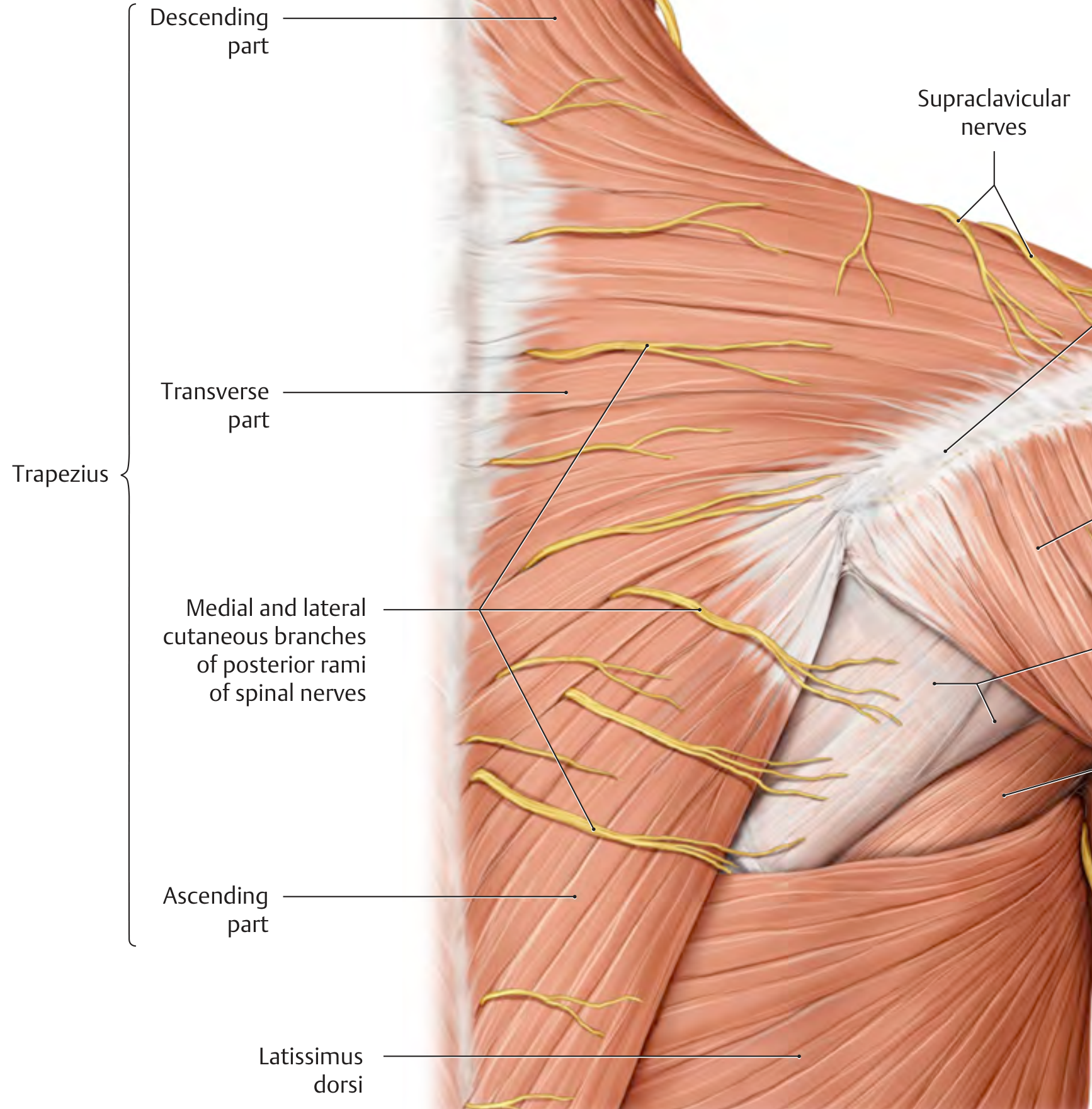
Supraclavicular Nerves (Clavicular Nerves)
The term "clavicular nerve" is an older or informal designation for the supraclavicular nerves — a group of cutaneous nerves that cross the clavicle and supply skin in the clavicular and shoulder region.
Origin
The supraclavicular nerves arise from the cervical plexus, which is formed by the anterior (ventral) rami of cervical nerves C1–C4, located just lateral to the transverse processes of the vertebrae. The supraclavicular nerves specifically originate from C3 and C4.
The cervical plexus has four cutaneous branches in total:
- Lesser occipital nerve (C2)
- Greater auricular nerve (C2, C3)
- Transverse cervical nerve (C2, C3)
- Supraclavicular nerves (C3, C4)
— Morgan & Mikhail's Clinical Anesthesiology, 7e; Localization in Clinical Neurology, 8e
Course
The supraclavicular nerves emerge from a common trunk behind the posterior border of the sternocleidomastoid muscle — at the "Erb's point," roughly halfway between the mastoid process and clavicle, where all superficial cervical plexus branches converge.
From here, the nerves descend across the clavicle, crossing it superficially from medial to lateral.
— Rockwood & Green's Fractures in Adults, 10e; Cummings Otolaryngology Head & Neck Surgery
Branches
There are typically three major branches:
| Branch | Alternative Name | Distribution |
|---|---|---|
| Anterior (medial) | Medial supraclavicular nerve | Skin over the medial clavicle, sternoclavicular joint, upper chest to rib II |
| Middle (intermediate) | Intermediate supraclavicular nerve | Skin over the mid-clavicle and upper anterior chest |
| Posterior (lateral) | Lateral supraclavicular nerve | Skin over the acromion, posterolateral shoulder |
All three branches cross the clavicle superficially and descend to supply the skin over the clavicle, shoulder, and chest.
— Rockwood & Green's Fractures in Adults, 10e
Sensory Distribution
The supraclavicular nerves supply cutaneous (sensory) innervation to:
- Skin immediately above the clavicle
- Skin over the shoulder and deltoid region
- Skin of the anterior upper chest as far inferiorly as rib II
- The upper portion of the breast (alongside intercostal nerve branches)
— Gray's Anatomy for Students; THIEME Atlas of Anatomy, General Anatomy & Musculoskeletal System
Function
The supraclavicular nerves are purely sensory (cutaneous). They carry no motor fibers.
Clinical Relevance
1. Clavicle fracture and plate fixation surgery
The supraclavicular nerves cross the clavicle superficially and are directly at risk during surgical approaches. Division of these nerves causes a patch of numbness inferior to the surgical incision (over the upper chest and shoulder). Although this often improves over time, a painful neuroma in the scar — though rare — can produce a difficult-to-manage complication. A vertical incision or nerve-sparing technique reduces this risk.
— Rockwood & Green's Fractures in Adults, 10e
2. Cervical plexus block (regional anaesthesia)
The superficial cervical plexus block targets these nerves as they emerge from behind the sternocleidomastoid. It provides analgesia for neck surgery, clavicle surgery, and shoulder procedures, and is commonly used as a supplement to interscalene block.
— Morgan & Mikhail's Clinical Anesthesiology, 7e; Miller's Anesthesia, 10e
3. Neck dissection (oncology)
During modified radical neck dissection, the supraclavicular nerves exit at Erb's point alongside the great auricular, lesser occipital, and transverse cervical nerves. Sacrificing them results in shoulder and chest wall numbness.
— Cummings Otolaryngology Head & Neck Surgery
4. Referred pain ("shoulder-tip sign")
Because diaphragmatic irritation (e.g., from subphrenic blood, abscess, or ectopic pregnancy) stimulates the phrenic nerve (C3–C5), referred pain is felt in the dermatomal territory of C3–C4 — precisely the supraclavicular distribution — explaining the classic "shoulder-tip pain" sign.
This is a shared conversation. Sign in to Orris to start your own chat.