Iselin disease
Reading File
Finding Sources
Searching the Web
Iselin disease apophysitis 5th metatarsal
Searching PubMed
Iselin disease apophysitis metatarsal
Finding Sources
Reading Web Page
Iselin disease diagnosis treatment imaging
Searching Images
Iselin disease fifth metatarsal apophysitis X-ray
Loading Image
Iselin Disease
Iselin disease (traction apophysitis of the fifth metatarsal base) is an overuse injury of the apophysis — the secondary ossification center — at the base of the fifth metatarsal bone. It was first described by German physician Hans Iselin in 1912.
Anatomy & Pathophysiology
The fifth metatarsal base has an apophysis (growth plate cartilage) where the peroneus brevis tendon inserts. During childhood and adolescence, this cartilaginous growth plate is biomechanically weaker than mature bone. Repetitive traction from the peroneus brevis — especially during running, jumping, and cutting movements — causes microtrauma, inflammation, and pain at this site.
The apophysis fuses:
- ~12 years in girls
- ~14 years in boys
Once fusion occurs, the condition self-resolves.
Epidemiology
- Age: 9–14 years (peak during growth spurts)
- More common in physically active children
- Associated sports: soccer, basketball, football, dance, gymnastics
- Risk factors:
- Growth spurts
- Tight peroneal/calf muscles
- Flat feet or high-arched feet (cavus)
- Narrow/ill-fitting cleats or spikes
- Inversion ankle injury (can acutely worsen symptoms)
Clinical Features
| Feature | Detail |
|---|---|
| Pain location | Lateral midfoot — base of 5th metatarsal (tuberosity) |
| Character | Worsens with activity (running, jumping, cutting), improves with rest |
| Swelling | Mild swelling/prominence over tuberosity |
| Gait | Child may limp or walk on the medial foot to offload the area |
| Trauma history | Usually absent (differentiates from Jones fracture/avulsion fracture) |
On exam: point tenderness directly over the 5th metatarsal tuberosity, reproducible with passive eversion/peroneus brevis loading.
Imaging
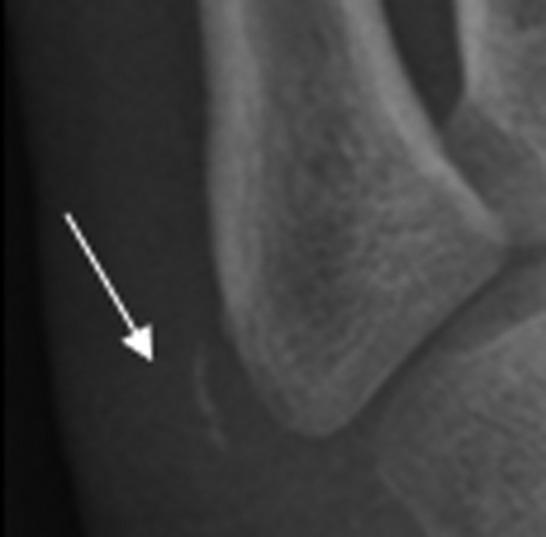
X-ray (oblique view is best)
The apophysis runs parallel to the long axis of the fifth metatarsal (in contrast to an avulsion fracture, which is oriented transversely across the bone). Findings may include:
- Widening or irregularity of the apophyseal plate
- Fragmentation of the ossification center
- Comparing bilateral views is important, as the normal apophysis can appear alarming
MRI (if diagnosis is uncertain):
- Edema over the unfused apophysis
- Mild-to-moderate marrow edema in the adjacent 5th metatarsal
- Useful to exclude stress fracture or other pathology
Bone scan: Increased uptake at the apophysis; rarely needed.
Differential Diagnosis
| Condition | Key Differentiator |
|---|---|
| Jones fracture | Transverse fracture at metaphyseal-diaphyseal junction (Zone 2); in adults or after acute trauma |
| Avulsion fracture (Zone 1) | Fracture line transverse to metatarsal long axis; acute traumatic onset |
| Os vesalianum pedis | Well-corticated accessory ossicle at tuberosity; no apophyseal plate, no acute findings |
| Peroneal tendinopathy | Older patients, more proximal tenderness along tendon |
| Cuboid stress fracture | Different location, different mechanism |
Treatment
Conservative in nearly all cases:
- Activity modification — avoid inciting sports temporarily
- NSAIDs — ibuprofen or naproxen for pain and inflammation
- Ice — after activity
- Immobilization (if severe) — posterior splint or short leg walking cast for 2–4 weeks
- Physical therapy — calf/peroneal stretching and strengthening, gait correction, proprioception
- Footwear — supportive shoes; avoid narrow cleats
Prognosis: Excellent. Most resolve within 3–6 weeks with conservative care. Complete resolution is expected once the apophysis fuses. Surgical intervention is essentially never required.
Key Teaching Points
- Iselin disease is likely underdiagnosed — many clinicians mistake it for a sprain, avulsion fracture, or Jones fracture
- The critical radiographic distinction: apophysis is parallel to the metatarsal (normal variant + Iselin) vs. fracture line is perpendicular/transverse (avulsion fracture)
- Always image both feet to compare apophyseal appearance
- Symptoms lasting 3–6 months before presentation are common — it is a chronic overuse condition, not acute
- A 2023 case report (PMID 36819335) described the unusual presentation of Iselin disease in an elderly patient, highlighting that it can rarely occur outside the typical pediatric age group
This is a shared conversation. Sign in to Orris to start your own chat.