what is tendinopathy in podiatry
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Loading Image
Here is a comprehensive overview of tendinopathy as it relates to podiatry (foot and ankle).
Tendinopathy in Podiatry
Definition & Terminology
Tendinopathy is an umbrella term for painful, impaired tendon conditions. It encompasses:
- Tendinitis — historically used, implying tendon inflammation
- Tendinosis — now preferred in many cases; describes a degenerative process with disorganized collagen, mucoid degeneration, and minimal inflammatory cells rather than true inflammation
Histopathological analysis of most tendinopathies reveals degenerative pathology with few inflammatory cells, which is why "tendinopathy" has replaced "tendinitis" as the preferred term.
— ROSEN's Emergency Medicine, Textbook of Family Medicine 9e
Pathophysiology
The underlying mechanism is mechanical overload and repetitive microtrauma to the musculotendinous unit. Both tensile overload and compression contribute (fiber bundles contacting each other, or friction/shearing against bone).
Intrinsic risk factors:
- Age, obesity, blood type O, tobacco use
- Malalignment, joint laxity, muscle weakness/imbalance
Extrinsic risk factors:
- Abnormal movements, excessive training load, frequency or intensity changes
- Ergonomic problems, environmental conditions
Systemic/pharmacological triggers:
- Fluoroquinolone antibiotics — increase risk of tendon rupture (especially Achilles), particularly in patients >60 years, on corticosteroids, or with renal disease
- Statins (2% incidence)
- Systemic diseases: diabetes mellitus, gout, coronary artery disease
— ROSEN's Emergency Medicine
Common Tendinopathies in the Foot & Ankle
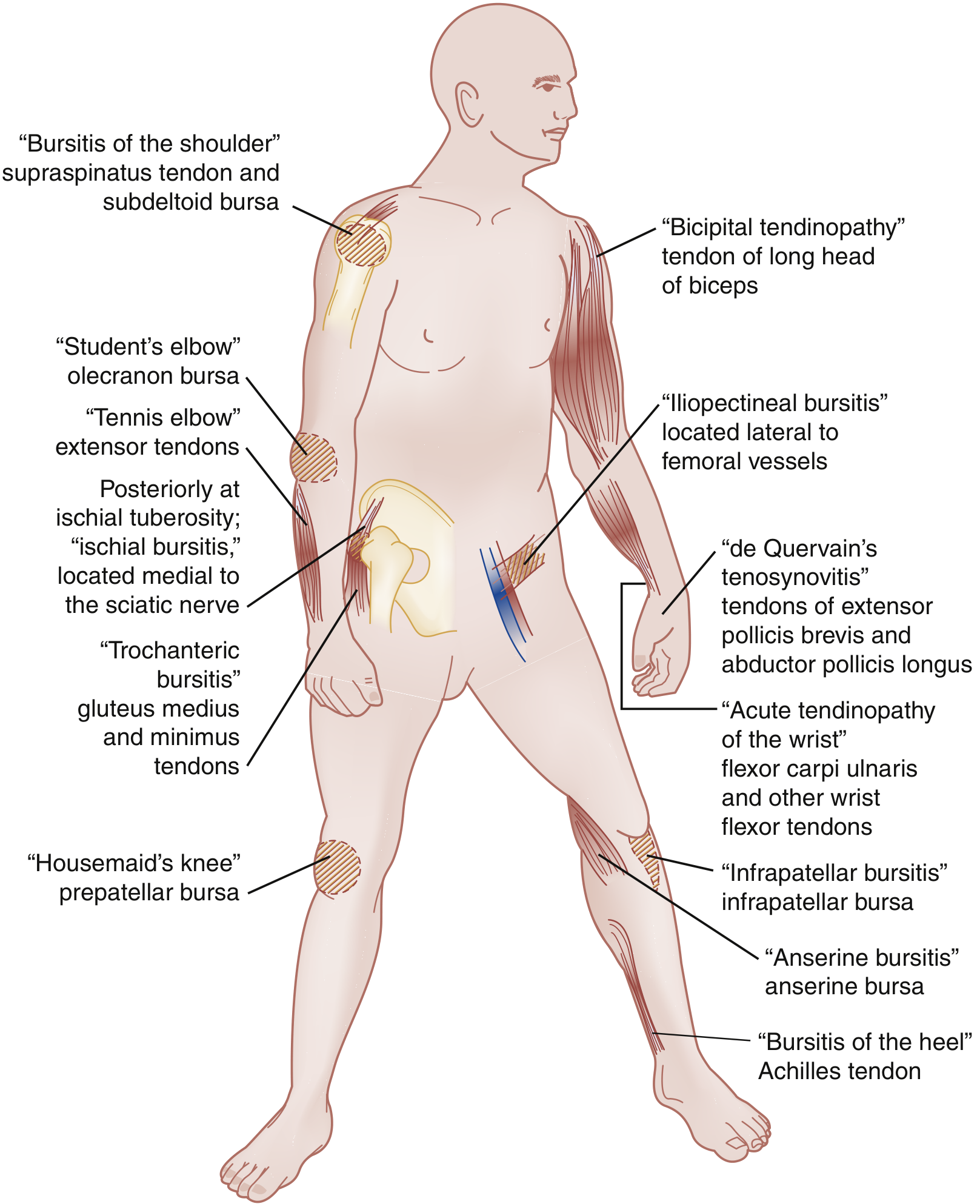
1. Achilles Tendinopathy (most common in podiatry)
The Achilles tendon — the strongest and largest tendon in the body — is the most frequently affected tendon in the lower limb. Two subtypes exist:
Insertional Achilles tendinopathy (~25% of cases):
- Pain, swelling, burning, and stiffness at the posterior heel
- Tenderness localized to the Achilles insertion on the posterior calcaneus (midline)
- Progressive bony prominence enlargement with pain from shoe pressure
- X-ray: bone spur and intratendinous calcification (lateral foot view)
- Often co-exists with Haglund deformity (prominent superior calcaneal tuberosity) and retrocalcaneal bursitis
Noninsertional Achilles tendinopathy:
- Pain in the posterior lower leg/heel, worsened with push-off activities (running, stairs, hills)
- Tenderness at the mid-tendon (2–6 cm above insertion), possible palpable swelling, firmness, and "wet crepitus" (fluid in peritenon)
- Thompson test used to assess tendon integrity: prone, knee at 90°, squeeze gastrocnemius — absence of plantarflexion = positive (rupture)
2. Posterior Tibial Tendinopathy
- Tendon runs posteromedially; primary dynamic stabilizer of the medial arch
- Strongly associated with adult acquired flatfoot deformity
3. Peroneal Tendinopathy
- Peroneal longus and brevis are primary evertors and pronators of the foot
- Chronic tendinopathy can predispose to dislocation or rupture at the posterior peroneal sulcus
4. Flexor Hallucis Longus / Flexor Digitorum Longus Tendinopathy
- Posteromedial ankle tendons
- The tibialis posterior is the strongest of the posteromedial group
Imaging
| Modality | Role |
|---|---|
| X-ray | First-line in chronic cases; detects calcific tendinopathy, Haglund deformity, enthesophytes |
| Ultrasound | Identifies tendon thickening, partial tears, tendon disruption; vascular integrity assessment |
| MRI | Best for partial tears, extent of degeneration; changes persist even after functional recovery |
Imaging changes (US/MRI) can persist in the tendon even after the patient has clinically recovered.
— Textbook of Family Medicine 9e
Treatment
Conservative (first-line, typically 6–12 weeks minimum)
- Relative rest and activity modification
- Ice and NSAIDs (short-term)
- Stretching and eccentric strengthening — eccentric training programs (e.g., Alfredson protocol for Achilles) show promising results
- Shoe wear modification, heel lifts, silicone heel pads/sleeves
- Physiotherapy / proprioception exercises
- Nitroglycerin patches (some tendinopathies)
- Bracing/splinting as needed
Injections
- Corticosteroids: AVOID — associated with tendon rupture risk (especially Achilles)
- Platelet-rich plasma (PRP): no benefit over saline for chronic Achilles tendinopathy in trials
- Prolotherapy: mixed short-term evidence
Advanced / Refractory
- Extracorporeal shock wave therapy (ESWT): studied in chronic insertional and noninsertional disease; evidence mixed
- Surgical debridement: for chronic, failed conservative cases — includes removal of degenerative tissue, calcifications
- If >50% of Achilles tendon is detached/excised: FHL tendon transfer is indicated
- Dorsal closing-wedge calcaneal osteotomy (Zadek) for Haglund cases without large posterior ossification
- Lateral/medial/midline J-shaped incision approaches described
Nonoperative treatment is beneficial in approximately 50–70% of insertional cases.
— Miller's Review of Orthopaedics 9th Edition, Textbook of Family Medicine 9e, ROSEN's Emergency Medicine
Key Points for Podiatry Practice
- Tendinopathy accounts for ~30% of all musculoskeletal ED/urgent care presentations
- Up to 50% of sports injuries involve tendinopathy
- Always allow at least 6–12 weeks of conservative treatment before escalating
- Steroid injections around the Achilles tendon are contraindicated
- Recurrence is common (49% in patellar tendinopathy); manage patient expectations accordingly
This is a shared conversation. Sign in to Orris to start your own chat.