Diagnosis and management .. Pain and swelling with irritation
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Reading File
I now have comprehensive information. Here is the diagnosis and management:
Diagnosis: Preseptal (Periorbital) Cellulitis
The images show diffuse eyelid edema with erythema, tense swelling, and epiphora (watery discharge), with the eye nearly unable to open — classic features of preseptal cellulitis, an infection of the subcutaneous tissues anterior to the orbital septum.
Reference image from Wills Eye Manual:
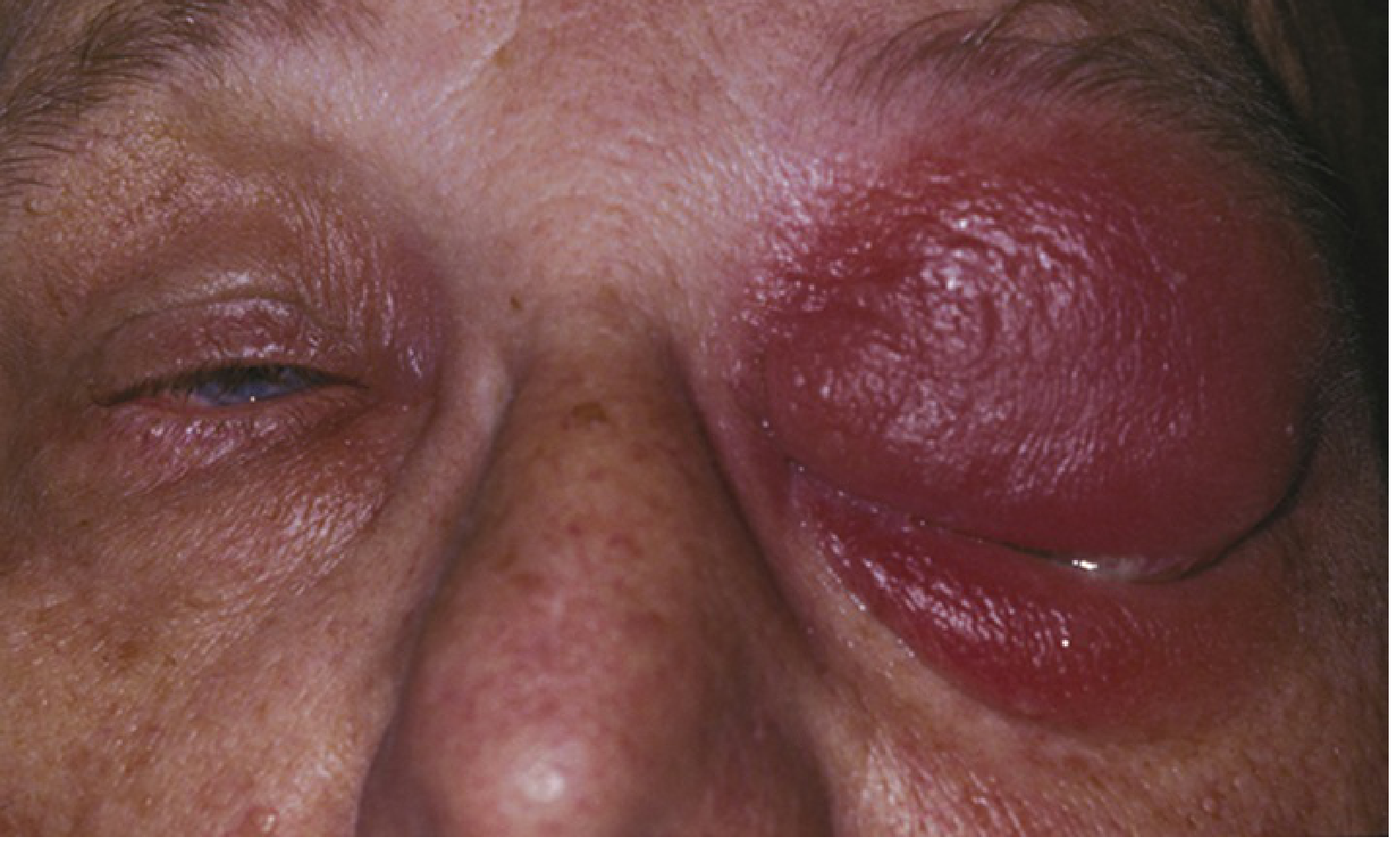

Clinical Features (as seen here)
| Feature | Present? |
|---|---|
| Eyelid erythema | ✓ |
| Tense edema, warmth, tenderness | ✓ |
| Epiphora (watery discharge) | ✓ |
| Eye nearly closed from edema | ✓ |
| No proptosis | (cannot assess fully from image) |
| No restricted eye movements | (must be assessed clinically) |
Key Differentials to Exclude
| Condition | Distinguishing Features |
|---|---|
| Orbital cellulitis | Proptosis, pain on eye movement, restricted motility, visual compromise — requires urgent CT + IV antibiotics |
| Allergic edema | Sudden onset, non-tender, itchy, bilateral |
| Herpes zoster/simplex | Vesicular rash, dermatomal pattern |
| Chalazion/Hordeolum | Focal nodule, not diffuse |
| Cavernous sinus thrombosis | Proptosis + multiple cranial nerve palsies |
Workup
- History: prior trauma, insect bite, sinusitis, hordeolum, hair epilation, prior MRSA infections?
- Full ocular exam: check visual acuity, pupil reactivity, extraocular movements, and for proptosis
- Check facial sensation (CN V1/V2 distribution)
- Vital signs and check for fever/toxicity
- Gram stain + culture of any open wound or discharge
- CT orbits + sinuses with contrast (axial and coronal) if:
- Orbital cellulitis cannot be excluded
- Significant trauma
- Suspected abscess or sinusitis
- No response to oral antibiotics in 24–48h
- CBC + blood cultures if febrile or systemically unwell
Treatment
Mild preseptal cellulitis (afebrile, >5 years, reliable follow-up)
Oral antibiotics for 10–14 days:
- Amoxicillin/clavulanate 875/125 mg PO q12h (adults); 25–45 mg/kg/day in 2 doses (children)
- OR Cefpodoxime 200 mg PO q12h (adults)
- OR Cefdinir
If MRSA suspected (risk factors: prior MRSA, recurrent skin infections, healthcare exposure, IV drug use, poor hygiene):
- Trimethoprim/sulfamethoxazole 160/800 mg (1–2 DS tablets) PO q12h
- OR Doxycycline 100 mg PO b.i.d. (adults only)
- OR Clindamycin 450 mg PO t.i.d.
Moderate-to-severe / Admission criteria
Admit for IV antibiotics if any of:
- Systemically toxic appearance
- Age ≤5 years
- Possible non-compliance
- No improvement or worsening after 24–48h of oral therapy
IV regimen:
- Vancomycin 0.5–1 g IV q12h (adults) PLUS
- Ampicillin/sulbactam 3 g IV q6h OR Piperacillin-tazobactam 4.5 g IV q6h
Follow-Up
- Review within 24–48 hours of starting antibiotics
- If worsening: CT scan and re-evaluate for orbital cellulitis/abscess requiring surgical drainage
— The Wills Eye Manual, pp. 403–409; Kanski's Clinical Ophthalmology 10th Ed., p. 139
Preseptal (Periorbital) Cellulitis management
Reading File
Finding Sources
Reading File
Reading File
Reading File
I now have detailed, comprehensive data from three authoritative sources. Here is the full management:
Preseptal (Periorbital) Cellulitis — Management
Overview
Preseptal cellulitis is an infection of the soft tissues anterior to the orbital septum. It is generally manageable in the outpatient setting, but must be clearly distinguished from postseptal (orbital) cellulitis, which is vision- and life-threatening.
Step 1: Confirm the Diagnosis & Rule Out Orbital Cellulitis
| Feature | Preseptal | Orbital (Postseptal) |
|---|---|---|
| Eyelid edema/erythema | ✓ | ✓ |
| Proptosis | ✗ | ✓ |
| Pain on eye movement | ✗ | ✓ |
| Restricted ocular motility | ✗ | ✓ |
| Visual compromise / APD | ✗ | ✓ |
| Chemosis | ✗ | ✓ |
If any orbital features are present → treat as orbital cellulitis (urgent CT + IV antibiotics + hospital admission).
Step 2: Investigations
- History: prior trauma, insect bite, sinusitis, hordeolum, dacryocystitis, prior MRSA, recent healthcare exposure
- Full ocular exam: VA, pupils, EOM, proptosis, fundus
- Vital signs — fever/systemic toxicity?
- Gram stain + culture of any wound/discharge
- CT orbits + sinuses with contrast (axial + coronal) if:
- Orbital cellulitis cannot be excluded
- Significant trauma or suspected foreign body
- Suspected subperiosteal/orbital abscess or sinusitis
- No improvement after 24–48h of oral antibiotics
- CBC + blood cultures in severe cases or if febrile
CT is not routinely required if the exam clearly confirms preseptal involvement only and the patient responds to therapy.
Step 3: Antibiotic Treatment
🟢 Mild Preseptal Cellulitis — Outpatient (Oral) Therapy
Criteria: afebrile, age >5 years, reliable follow-up, no systemic toxicity
First-line (non-MRSA):
| Drug | Adult Dose | Pediatric Dose |
|---|---|---|
| Amoxicillin/clavulanate | 875/125 mg PO q12h | 25–45 mg/kg/day in 2 divided doses (max 90 mg/kg/day) |
| Cefpodoxime | 200 mg PO q12h | 10 mg/kg/day in 2 doses (max 400 mg/day) |
| Cefdinir | Standard adult dose | Weight-based dosing |
| Moxifloxacin | 400 mg PO daily | ❌ Contraindicated in children |
If MRSA suspected (risk factors: prior MRSA, recurrent skin infections, healthcare facility exposure in past year, IV drug use, incarceration, hemodialysis, sports with skin contact, poor hygiene):
| Drug | Adult Dose | Pediatric Dose |
|---|---|---|
| TMP-SMX (Co-trimoxazole) | 1–2 DS tablets (160/800 mg) PO q12h | 8–12 mg/kg/day TMP + 40–60 mg/kg/day SMX in 2 doses |
| Doxycycline | 100 mg PO b.i.d. | ❌ Contraindicated in children, pregnant/nursing women |
| Clindamycin | 450 mg PO t.i.d. | 10–30 mg/kg/day in 3–4 divided doses |
Duration: 10–14 days for all oral regimens
🔴 Moderate-to-Severe — Inpatient (IV) Therapy
Admit to hospital if ANY of the following:
- Systemically toxic / unwell appearance
- Age ≤5 years
- Possible non-compliance with outpatient treatment
- No improvement or worsening after 24–48h of oral antibiotics
- High fever or bacteremia suspected
IV Regimen:
| Drug | Adult Dose | Pediatric Dose |
|---|---|---|
| Vancomycin (MRSA cover) | 0.5–1 g IV q12h (adjust for renal function) | 10–15 mg/kg IV q6h |
| PLUS one of: | ||
| Ampicillin/sulbactam | 3 g IV q6h | 300 mg/kg/day IV in 4 divided doses |
| Piperacillin-tazobactam | 4.5 g IV q6h | 240 mg/kg/day IV in 3 divided doses |
Step 4: Supportive Measures
- Warm compresses to the affected lid
- Treat underlying source (e.g., hordeolum, dacryocystitis, sinusitis)
- Analgesics (e.g., NSAIDs/paracetamol) for pain relief
- If abscess is present → surgical incision and drainage
Step 5: Follow-Up
- Review at 24–48 hours after initiating therapy
- If worsening: obtain CT, escalate to IV antibiotics, reassess for orbital extension or abscess
- Transition from IV to oral once clinically improving
Potential Complications (if untreated/undertreated)
- Abscess formation
- Progression to orbital (postseptal) cellulitis
- Meningitis
- Cavernous sinus thrombosis
- Subperiosteal abscess
— The Wills Eye Manual, pp. 403–409; Kanski's Clinical Ophthalmology 10th Ed., p. 139; Tintinalli's Emergency Medicine, p. 1575
which topicals can be used
Finding Sources
Finding Sources
Reading File
Reading File
Here is a focused answer on topical agents in preseptal cellulitis:
Topical Agents in Preseptal Cellulitis
Important Context First
Preseptal cellulitis is a systemic (skin/soft tissue) infection — topical ophthalmic preparations do not penetrate the infected periorbital tissues and cannot replace oral or IV antibiotics. Topicals are adjunctive only, used for specific secondary ocular involvement.
When Topicals Are Used
1. Secondary Conjunctivitis
If conjunctival injection or discharge is present alongside the cellulitis:
| Agent | Form | Dose |
|---|---|---|
| Polymyxin B / Bacitracin | Ointment | q.i.d. |
| Tobramycin | Drops or ointment | q.i.d. |
| Erythromycin | Ointment | b.i.d. – q.i.d. |
| Bacitracin | Ointment | b.i.d. |
"Polymyxin B/bacitracin ointment to the eye q.i.d. if secondary conjunctivitis is present." — Wills Eye Manual, p. 410
2. Associated Hordeolum (Stye) — The Primary Source
When the cellulitis arose from a hordeolum, topical antibiotics are used to treat the local lid margin infection:
| Agent | Form | Dose |
|---|---|---|
| Erythromycin | Ointment | b.i.d. (1–2 weeks) |
| Bacitracin | Ointment | b.i.d. |
| Tobramycin | Drops/ointment | b.i.d. |
"Consider a short course of a topical antibiotic for hordeolum (e.g., bacitracin, tobramycin, or erythromycin ointment b.i.d. for 1–2 weeks)" — Wills Eye Manual, p. 382
3. Topical Steroid-Antibiotic Combination
For an associated chalazion (which may co-exist):
- Neomycin/Polymyxin B/Dexamethasone (e.g., Maxitrol) q.i.d. for 1–2 weeks
- Monitor IOP if used (steroid-related risk)
Summary: Role of Topicals
| Situation | Topical Agent |
|---|---|
| Secondary conjunctivitis | Polymyxin B/Bacitracin ointment q.i.d. |
| Associated hordeolum | Erythromycin / Tobramycin / Bacitracin ointment b.i.d. |
| Associated chalazion | Neomycin/Polymyxin B/Dexamethasone q.i.d. |
| The cellulitis itself | ❌ Topicals are ineffective — systemic antibiotics required |
— The Wills Eye Manual, pp. 382 & 410; Roberts and Hedges' Clinical Procedures in Emergency Medicine, p. 1511
pain is aggravated while lying down or bending down
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
This symptom is highly clinically significant and changes your approach. Here is the full analysis:
What This Symptom Tells You
Pain aggravated by lying down or bending forward is a hallmark sign of paranasal sinusitis — specifically maxillary or ethmoid sinusitis. These positions increase hydrostatic pressure within the sinus cavities, worsening pain and pressure.
In the context of periorbital cellulitis, this is a red flag indicating:
Sinusitis is likely the primary source driving the preseptal (or possibly orbital) cellulitis — not a simple skin/lid infection.
Why This Matters Clinically
Sinogenic preseptal cellulitis carries a higher risk of progression to:
| Complication | Risk |
|---|---|
| Orbital (postseptal) cellulitis | Infection spreads posterior to orbital septum via ethmoid/maxillary sinuses |
| Subperiosteal abscess | Pus collects between orbital wall and periosteum |
| Orbital abscess | Direct orbital pus collection → vision threat |
| Cavernous sinus thrombosis | Life-threatening; 20% mortality even when treated, up to 100% untreated |
| Meningitis | Intracranial spread |
The ethmoid sinus is the most commonly implicated sinus in sinogenic orbital/periorbital cellulitis due to its direct anatomical proximity to the medial orbital wall (lamina papyracea).
Revised Management Plan
1. Imaging — Now Mandatory
CT orbits + sinuses with IV contrast (axial + coronal) is now strongly indicated to:
- Confirm sinusitis
- Rule out orbital cellulitis, subperiosteal abscess, or orbital abscess
- Identify the specific sinus involved
2. Antibiotic Escalation
Since sinusitis is now the likely source, antibiotic coverage must include anaerobes and sinus organisms (Streptococcus pneumoniae, H. influenzae, Moraxella, S. aureus, anaerobes):
| Setting | Preferred Agent |
|---|---|
| Outpatient (mild) | Amoxicillin/clavulanate 875/125 mg PO q12h — covers sinus pathogens + anaerobes |
| Inpatient (moderate-severe) | Ampicillin/sulbactam 3g IV q6h ± Vancomycin (if MRSA risk) |
3. Treat the Sinusitis Directly
| Intervention | Details |
|---|---|
| Nasal decongestants | Oxymetazoline 0.05% nasal spray b.i.d. for ≤3–5 days (rebound risk) OR oral pseudoephedrine |
| Intranasal saline irrigation | Helps drain secretions, reduce mucosal edema |
| Intranasal corticosteroids | Mometasone or fluticasone spray — reduces mucosal inflammation |
| Analgesics | NSAIDs/paracetamol for pain and fever |
| Head elevation | Sleep with head of bed elevated 30–45° to reduce sinus pressure and eyelid edema |
| Steam inhalation / warm compresses | Symptomatic relief |
4. ENT Referral
Sinusitis-driven periorbital cellulitis warrants ENT co-management:
- Nasal endoscopy to assess sinus drainage
- Surgical drainage (FESS — functional endoscopic sinus surgery) if:
- Subperiosteal or orbital abscess identified on CT
- No response to IV antibiotics within 24–48h
5. Opthalmology Referral
Concurrent ophthalmology evaluation to monitor for progression to orbital cellulitis.
Key Warning Signs — Admit Immediately If Any Present
| Sign | Significance |
|---|---|
| Proptosis (eyeball pushed forward) | Orbital cellulitis / abscess |
| Pain on eye movement | Orbital involvement |
| Restricted extraocular movements | Orbital cellulitis |
| Reduced visual acuity | Optic nerve compression — emergency |
| Altered consciousness / meningism | Intracranial spread |
| High fever + bilateral eye signs | Cavernous sinus thrombosis |
Summary of Revised Diagnosis
| Component | Finding |
|---|---|
| Primary diagnosis | Preseptal (periorbital) cellulitis |
| Underlying cause | Acute sinusitis (ethmoid/maxillary most likely) |
| Key symptom | Pain worse on lying down / bending forward = sinus pressure |
| Urgent need | CT orbits + sinuses to exclude orbital extension |
| Treatment | Amoxicillin/clavulanate + nasal decongestant + saline irrigation + head elevation; escalate to IV if severe |
— Tintinalli's Emergency Medicine; The Wills Eye Manual, p. 409–410; Kanski's Clinical Ophthalmology 10th Ed.
how many days after treatment initiation swelling and pain comes down
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
The textbooks do not give a single fixed "day X — swelling resolves" timeline (because no controlled trial pins it to an exact number), but they provide clear clinical benchmarks that guide expectations. Here is what the evidence and clinical reasoning tell you:
Expected Timeline of Recovery
Oral Antibiotics (Outpatient)
| Timeframe | What to Expect |
|---|---|
| 24–48 hours | First signs of improvement should be visible — reduced tenderness, slight softening of edema. If there is NO improvement or it is WORSENING at this point → admit for IV antibiotics |
| 48–72 hours | Erythema and warmth begin to noticeably decrease |
| Day 3–5 | Swelling visibly reducing, pain significantly less, eye begins to open more |
| Day 7–10 | Most of the edema resolved; eyelid approaching normal appearance |
| Day 10–14 | Full resolution expected — complete the antibiotic course regardless |
"No noticeable improvement or worsening after 24 to 48 hours of oral antibiotics → admit to hospital for IV antibiotics" — Wills Eye Manual, p. 409
"Follow up daily until clear and consistent improvement is demonstrated, then every 2–7 days until totally resolved." — Wills Eye Manual, p. 410
IV Antibiotics (Inpatient)
- Faster response: noticeable improvement typically within 24–48 hours
- Transition to oral once improving
- Total course still 10–14 days
Factors That Slow Recovery
| Factor | Effect |
|---|---|
| Sinusitis as underlying cause (as in this patient) | Slower resolution — sinus must also clear |
| MRSA organism | Poor response to standard antibiotics — needs TMP-SMX / clindamycin |
| Abscess formation | Won't resolve on antibiotics alone — needs drainage |
| Orbital extension | Much slower, requires IV + possible surgery |
| Delayed treatment initiation | Prolongs overall course |
| Immunocompromised patient | Slower healing |
Practical Guidance for This Patient
Given that sinusitis is the likely driver in this case:
- Expect swelling and pain to take 5–7 days to meaningfully subside (slightly longer than isolated lid infection)
- Pain on bending/lying down (sinus component) may persist 7–10 days even with antibiotics
- Nasal decongestants + saline irrigation will help resolve the sinus component faster and speed overall recovery
- If no improvement by 48 hours on oral therapy → CT scan + hospital admission
— The Wills Eye Manual, pp. 409–410
This is a shared conversation. Sign in to Orris to start your own chat.