Role of Vitamin B12 and Folic acid in Red blood cells production
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Searching Images
vitamin B12 folic acid megaloblastic anemia DNA synthesis erythropoiesis
Reading File
Searching Images
folate cycle thymidylate synthesis DNA methionine synthase cobalamin diagram
Reading File
Loading Image
Reading File
I now have comprehensive information to provide a well-sourced, detailed answer. Let me compile it.
Role of Vitamin B12 and Folic Acid in Red Blood Cell Production
Overview
Vitamin B12 (cobalamin) and folic acid (folate) are both essential for the production of healthy red blood cells (RBCs). Their primary shared role is enabling DNA synthesis in rapidly dividing cells of the bone marrow. Deficiency of either vitamin impairs this process and results in megaloblastic anemia — a condition where RBC precursors grow abnormally large but fail to divide properly, producing defective, short-lived red cells.
"The cause is usually a deficiency of either cobalamin (vitamin B12) or folate, but megaloblastic anemia may occur because of genetic or acquired abnormalities that affect the metabolism of these vitamins or because of defects in DNA synthesis not related to cobalamin or folate." — Harrison's Principles of Internal Medicine 22E
The Biochemical Mechanism: How They Enable DNA Synthesis
The diagram below illustrates the interconnected folate cycle and methylation cycle — the two pathways through which B12 and folate cooperate to drive DNA synthesis and cell replication:
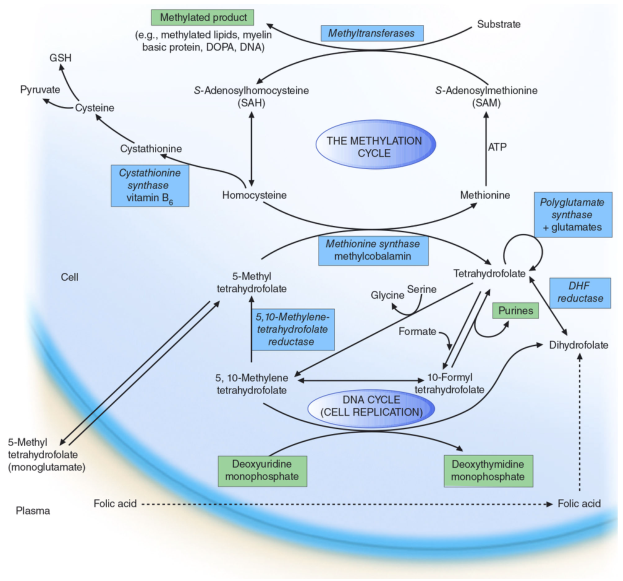
Step-by-step pathway:
1. Folate's role — supplying single-carbon units for DNA building blocks
Folate, as intracellular polyglutamate derivatives of tetrahydrofolate (THF), acts as a coenzyme carrying single-carbon units. These are used for:
- Purine synthesis (2 reactions) — needed for adenine and guanine in DNA
- Pyrimidine synthesis (1 reaction) — specifically, conversion of deoxyuridine monophosphate (dUMP) → deoxythymidine monophosphate (dTMP), the critical step to make thymine for DNA
The coenzyme form for this last reaction is 5,10-methylene-THF. Without adequate folate, dTMP cannot be produced, halting DNA replication.
"Two of these reactions are involved in purine synthesis and one in pyrimidine synthesis necessary for DNA and RNA replication." — Harrison's Principles of Internal Medicine 22E, p. 824
2. Vitamin B12's role — regenerating active folate via the methionine synthase reaction
B12 (as methylcobalamin) is the cofactor for the enzyme methionine synthase, which converts:
5-methyl-THF + Homocysteine → THF + Methionine
This reaction is critical for two reasons:
- It regenerates free THF, which can re-enter the folate cycle to synthesize 5,10-methylene-THF for DNA synthesis
- It allows folate polyglutamation (the form retained inside cells), since the polyglutamate synthase enzyme uses THF, not 5-methyl-THF, as its substrate
Without B12, folate is "trapped" as 5-methyl-THF — it accumulates in plasma but cannot be converted to usable intracellular folate coenzymes. This is called the "methyl-folate trap", and it explains why B12 deficiency produces the same hematological picture as folate deficiency.
"In cobalamin deficiency, 5-MTHF accumulates in plasma, and intracellular folate concentrations fall due to failure of formation of THF, the substrate on which polyglutamate synthase acts." — Harrison's Principles of Internal Medicine 22E
The Consequence: Megaloblastic Anemia
When DNA synthesis fails in erythroid precursors:
| Feature | Explanation |
|---|---|
| Megaloblasts | Large, abnormal RBC precursors with immature nuclei and abundant cytoplasm — cell grows but cannot divide |
| Hypersegmented neutrophils | Classically ≥5-lobed neutrophils; a hallmark smear finding |
| Macrocytic anemia | Large (high MCV) but poorly functioning RBCs released into circulation |
| Pancytopenia | All rapidly dividing marrow cells affected — WBCs and platelets also reduced |
| Ineffective erythropoiesis | Marrow is hypercellular but output is low — precursors die before maturing |
"The common feature of all megaloblastic anemias is a defect in DNA synthesis that affects rapidly dividing cells in the bone marrow." — Harrison's Principles of Internal Medicine 22E, p. 825
Why B12 and Folate Deficiencies Are NOT Identical
Although both cause megaloblastic anemia, only B12 deficiency causes neurological damage:
- B12 is also the cofactor for methylmalonyl-CoA mutase (in mitochondria), which converts methylmalonyl-CoA to succinyl-CoA
- Without B12, methylmalonyl-CoA accumulates → subacute combined degeneration of the spinal cord (posterior and lateral column demyelination)
- Folate does NOT participate in this reaction, so folate deficiency does NOT cause neurological disease
"Folate deficiency does not cause the characteristic neurologic syndrome seen in vitamin B12 deficiency." — Katzung's Basic and Clinical Pharmacology 16E
Summary Table
| Feature | Vitamin B12 | Folic Acid |
|---|---|---|
| Active form | Methylcobalamin (cytoplasm), Adenosylcobalamin (mitochondria) | THF polyglutamates |
| Key enzyme | Methionine synthase | Thymidylate synthase, purine synthesis enzymes |
| Role in RBC production | Regenerates THF from 5-methyl-THF | Directly provides single-carbon units for dTMP and purines |
| Deficiency effect | Methyl-folate trap → impaired DNA synthesis | Direct shortage of DNA precursors |
| Result | Megaloblastic anemia + neurological disease | Megaloblastic anemia only |
| Dietary sources | Animal products only (meat, fish, dairy) | Green leafy vegetables, legumes, fortified foods |
| Daily requirement | ~1–3 μg/day | ~400 μg/day (higher in pregnancy) |
| Body stores | 2–3 mg (lasts 3–4 years) | ~5–10 mg (lasts ~4 months) |
Key Takeaway
Vitamin B12 and folic acid form a biochemically interdependent pair. Folate directly supplies the building blocks for DNA synthesis in RBC precursors. B12 keeps folate cycling in its active, usable form inside cells. Deficiency of either nutrient breaks this cycle, halting erythropoiesis and producing megaloblastic anemia — but only B12 deficiency also damages the nervous system.
— Harrison's Principles of Internal Medicine 22E; Katzung's Basic and Clinical Pharmacology 16E; Basic Medical Biochemistry 6E
Summarize and give me 4 bullet points on this
Vitamin B12 & Folic Acid in Red Blood Cell Production
Both vitamins are essential for DNA synthesis in bone marrow. Without them, RBC precursors cannot divide properly, leading to megaloblastic anemia — large, dysfunctional red cells with impaired oxygen-carrying capacity.
-
DNA synthesis depends on folate — Folic acid provides the single-carbon units needed to build thymine and purines, the core building blocks of DNA in dividing RBC precursors. Without it, cell replication stalls.
-
B12 keeps folate active — Vitamin B12 (as methylcobalamin) runs the methionine synthase reaction, which converts inactive 5-methyl-THF back into usable THF. Without B12, folate gets "trapped" and cannot enter the DNA synthesis cycle — this is the methyl-folate trap.
-
Deficiency of either causes megaloblastic anemia — RBC precursors grow large but fail to divide, producing oversized, fragile red cells (macrocytes) and hypersegmented neutrophils on blood smear, along with low RBC count and pancytopenia.
-
B12 deficiency goes further — it damages nerves too — Unlike folate, B12 is also needed for myelin maintenance (via methylmalonyl-CoA mutase). Its deficiency uniquely causes subacute combined degeneration of the spinal cord; folate deficiency does not affect the nervous system.
This is a shared conversation. Sign in to Orris to start your own chat.