Chronic diseases of the larynx. Foreign bodies of larynx. trachea. bronchi. esophagus. Intubation and Tracheostomy.
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
I now have comprehensive material from Cummings Otolaryngology and Sabiston's Surgery. Let me compile the complete answer.
Chronic Diseases of the Larynx · Foreign Bodies · Intubation & Tracheostomy
I. CHRONIC DISEASES OF THE LARYNX
A. Chronic Infectious Laryngitis
The distinction between acute and chronic laryngitis is not strict — many acute disorders may evolve into or contribute to chronic dysfunction.
1. Chronic Bacterial Laryngitis
Superinfection of the larynx may complicate intubation injuries or pre-existing damage (e.g., relapsing polychondritis). Purulent chondritis with prolonged hoarseness and stridor lasting >1 month may result. The most common pathogen is S. aureus. Management requires surgical drainage and prolonged antibiotic therapy; hyperbaric oxygen may have an adjunctive role. — Cummings Otolaryngology
2. Chronic Fungal Laryngitis
Pathogenic fungi include Blastomyces, Histoplasma, Coccidioides, Paracoccidioides, and Cryptococcus. All present with hoarseness and throat discomfort — none have a specific endoscopic appearance. Critical diagnostic pitfall: fungal laryngitis can closely mimic laryngeal carcinoma; biopsies may show pseudoepitheliomatous hyperplasia that can be mistaken for advancing malignancy. Tissue biopsy with fungal stains is required for diagnosis.
- Blastomycosis: endemic in southern US; hematogenous spread to larynx (≤5% of cases); broad-based budding yeast on stain; treat with amphotericin B, ketoconazole, or itraconazole
- Paracoccidioidomycosis: leading cause of invasive fungal laryngitis in South America; ulcerative and exophytic lesions; treat with systemic antifungals
- Histoplasmosis: laryngeal involvement possible; treat systemically
3. Chronic Mycobacterial Laryngitis
Tuberculosis can involve the larynx (typically secondary to pulmonary disease). Biopsy showing caseating granulomas and acid-fast organisms confirms the diagnosis. Treated with standard anti-TB regimens.
B. Noninfectious Chronic Laryngitis
The most clinically significant causes of chronic laryngitis in otolaryngology practice relate to poor laryngeal hygiene (tobacco, alcohol, caffeine) or reflux.
1. Reflux Laryngitis (Laryngopharyngeal Reflux — LPR)
Acidic (and non-acidic) refluxate damages the laryngeal epithelium. Bile and pepsin are increasingly implicated — pepsin maintains injurious activity at pH >4 and can be "reactivated" after entering an acid-neutral environment, even after receptor-mediated uptake into laryngeal epithelial cells. This challenges the paradigm of proton-pump inhibitor therapy alone. Clinical features include hoarseness, throat clearing, globus, and posterior laryngitis on endoscopy. Management: dietary modification, head-of-bed elevation, PPIs — though evidence from blinded trials is limited.
2. Autoimmune Laryngitis
| Condition | Key Features |
|---|---|
| Pemphigus vulgaris | Intraepithelial autoantibodies; up to 80% of patients have otolaryngologic signs; 40% laryngeal; responds to high-dose corticosteroids + immunosuppressives |
| Pemphigoid | Subepithelial autoantibodies; 35% of patients have head/neck symptoms; 50% of these have laryngeal lesions; often asymptomatic |
| Granulomatosis with Polyangiitis (GPA/Wegener's) | c-ANCA or p-ANCA positive; 90% have head/neck manifestations; most common laryngeal feature = subglottic stenosis (20%); treat with endoscopic dilation or open resection; systemic immunosuppression does not reliably prevent restenosis |
| Relapsing Polychondritis (RP) | Autoantibodies to type II collagen; 25–50% have laryngeal involvement ranging from hoarseness to lethal airway obstruction; requires combined medical and surgical management |
3. Systemic Inflammatory Disease
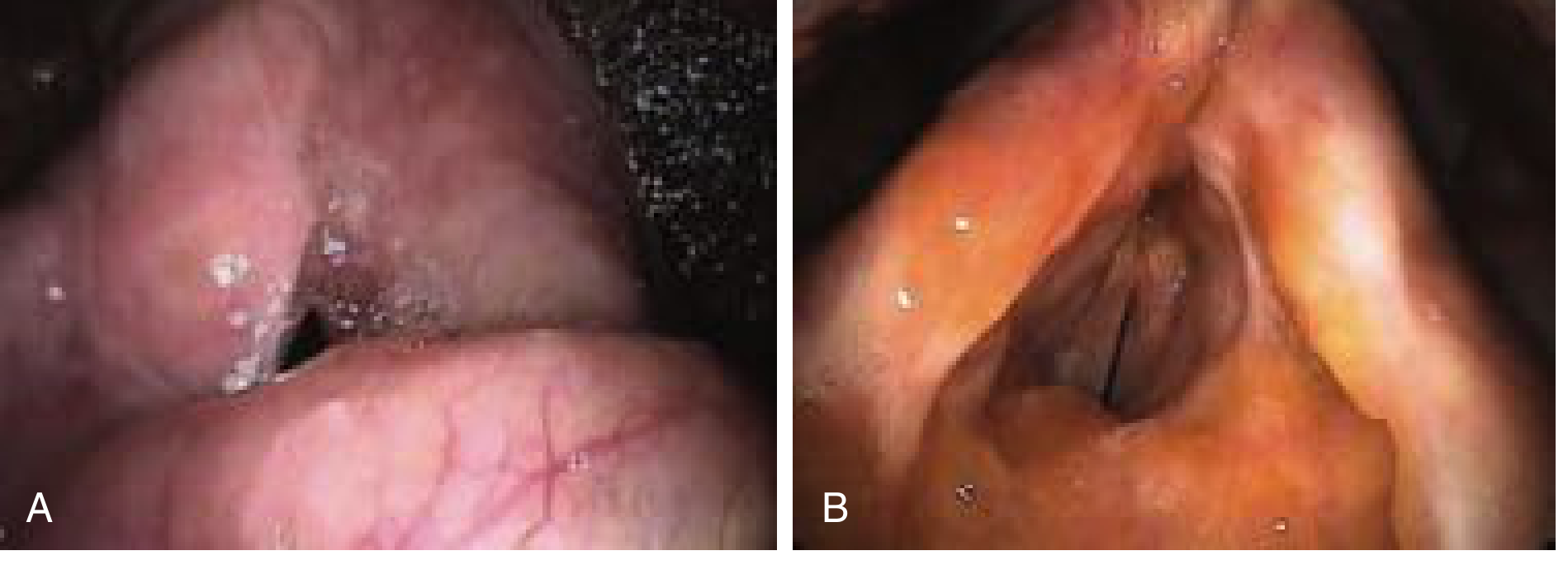
Sarcoidosis: Laryngeal involvement occurs in <1% of patients; typically supraglottic and glottic diffuse edema (Fig. below); diagnosis by histology (noncaseating granulomas); treat with systemic steroids ± endoscopic resection and intralesional steroid injection.
Amyloidosis: Extracellular deposition of abnormal protein; may be primary (localized to larynx) or secondary (to myeloma or chronic inflammatory disease); presents as painless diffuse laryngeal deposits causing hoarseness (Fig. below).
II. FOREIGN BODIES OF THE LARYNX, TRACHEA, BRONCHI, AND ESOPHAGUS
A. Epidemiology & Pathophysiology
Airway/esophageal foreign body asphyxiation is a common cause of death in children. Round foods (peanuts, grapes, raisins, hot dogs) are especially common. Conformable objects (e.g., balloons, latex gloves) are the most difficult to remove and the most likely to cause death.
The esophagus has physiologic and pathologic narrowings where foreign bodies lodge:
- Upper esophageal sphincter / cricopharyngeus
- Level of the aortic arch
- Diaphragmatic hiatus / LES
Bone spicules most commonly lodge in the inferior tonsil, tongue base, or vallecula. Larger objects lodge at pathologic strictures or the anatomic narrowings listed above.
B. Clinical Features
Airway foreign bodies:
- Complete obstruction: inability to speak, poor air exchange, ineffective cough, severe distress, cyanosis
- Partial / lower airway: unilateral wheeze, or delayed presentation as recurrent pneumonia (days to years after aspiration)
- Objects passing through the subglottic space typically lodge in the right mainstem bronchus (due to its more vertical angle)
- A bronchial foreign body may be "coughed up," suddenly causing upper airway re-obstruction
Esophageal foreign bodies:
- Dysphagia, chest pain, drooling, inability to manage saliva
- Adults often have underlying structural abnormality (stricture, ring) — underlying pathology is found in ~90% after food impaction removal
C. Diagnosis
Imaging:
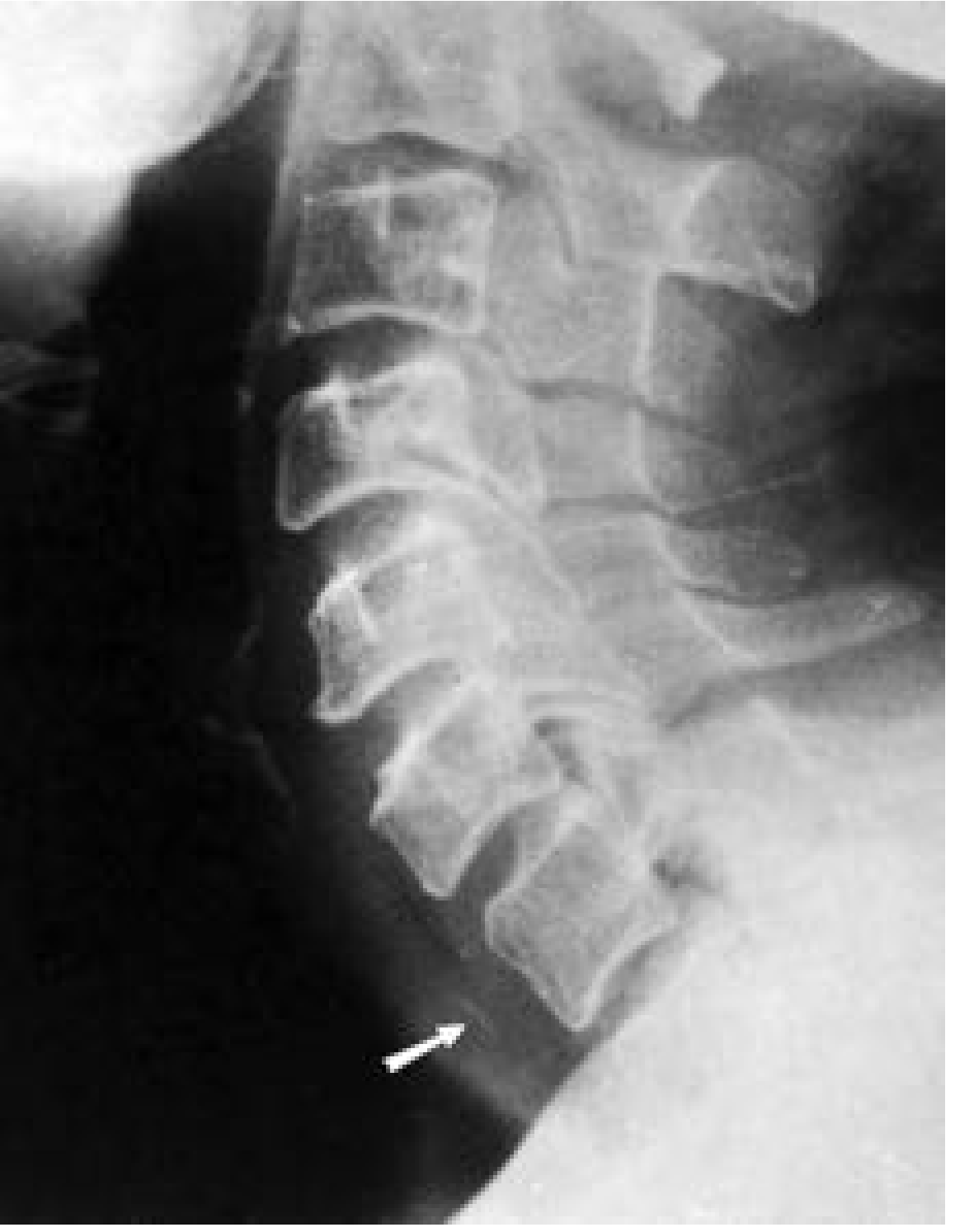
- Lateral soft-tissue neck X-ray + chest X-ray are the first step
- Radiographic signs: radiopaque object, mediastinal shift, emphysema, atelectasis
- Normal chest X-ray does not rule out a non-radiopaque foreign body
- CT scan / virtual bronchoscopy: used in equivocal cases
- Esophagogram: shows filling defects; use water-soluble contrast initially (risk of perforation)
- Secondary signs of perforation: pneumomediastinum, prevertebral swelling, fascial gas
Important radiologic pitfall: Ossification of laryngeal cartilages (cricoid posterior margin, thyroid cartilage) can mimic radiopaque foreign bodies; tonsillar calcifications have a characteristic CT appearance.
D. Management
Acute complete airway obstruction:
- Infants <1 year: 5 back blows between shoulder blades + 5 chest thrusts (head below trunk). No abdominal thrusts, no blind finger sweeps.
- Conscious children >1 year: Heimlich maneuver
- Unconscious: chest compressions
- If no chest rise with bag-mask: laryngoscopy + Magill forceps retrieval; if not visible, push foreign body distally into right mainstem bronchus to ventilate contralateral lung
- Avoid rapid-sequence induction with paralysis in a patient maintaining a partial airway — paralysis can convert partial to complete obstruction
Stable airway foreign body:
- Allow patient to maintain position of comfort and continue spontaneous breathing until operative management is arranged
- Rigid bronchoscopy remains the gold standard for bronchial foreign body removal
Esophageal foreign bodies:
- Any foreign body in the esophagus must be removed (risk of pressure necrosis/perforation)
- Sharp/long objects: 15–35% perforation risk; remove regardless of location
- Small blunt objects that have passed the esophagus usually pass spontaneously
- Endoscopy is the treatment of choice (up to 20% of ingested foreign bodies require intervention); perform within 12 hours for food impaction
- After removal, assess for underlying esophageal pathology (present in ~90%)
III. INTUBATION
Indications
Endotracheal intubation is used for airway protection, ventilatory support, and to facilitate general anaesthesia. It may be oral or nasal (nasotracheal).
Complications
Complications of prolonged intubation include:
- Subglottic stenosis (the most clinically important long-term complication)
- Laryngeal ulceration and granuloma formation
- Tracheomalacia
- Tracheo-esophageal fistula
- Superinfection (bacterial chondritis — often S. aureus)
- Arytenoid dislocation
Can't Intubate, Can't Ventilate (CICV)
- Adults/children >8–10 years: surgical cricothyrotomy is the procedure of choice
- Infants and young children <8 years: anatomy makes cricothyrotomy technically difficult; needle cricothyrotomy is a temporizing bridge only (significant CO₂ retention limits effectiveness)
IV. TRACHEOSTOMY
Indications and Contraindications
| Indications | Contraindications (mostly relative) |
|---|---|
| Upper airway obstruction (tumors, angioedema, trauma) | Recent anterior neck surgery (<7 days) |
| Prolonged mechanical ventilation | High ventilator settings (FiO₂ >50%, PEEP >10 cmH₂O) |
| Neurologic conditions preventing safe extubation (TBI, spinal cord injury, severe agitation) | Elevated intracranial pressure |
| Difficult airway | Hemodynamic instability |
| Significant bleeding risk | |
| Local infection or malignancy at proposed site | |
| Predicted early mortality |
Techniques
Open surgical tracheostomy: standard procedure performed in the OR via midline neck incision.
Percutaneous Dilatational Tracheostomy (PDT): described by Ciaglia (1985); now widely used at the bedside in ICU. Compared to open surgical tracheostomy, PDT shows:
- Decreased wound infection
- Less clinically relevant bleeding
- Greater cost-effectiveness
- Periprocedural mortality <0.2%; major complication rate ~0.15% in large series (>3,000 procedures)
Either bronchoscopic or ultrasound guidance should be used to confirm proper positioning of the tracheostomy tube.
Timing
- Early (<7 days) vs. late (>7 days): most studies show no mortality difference
- The largest RCT (TracMan, >900 UK patients): no mortality difference at 30 days or 2 years; notably, >50% of patients randomized to late tracheostomy never required one (liberated from ventilation first)
- One medical ICU trial showed significant reduction in mortality, pneumonia, and accidental extubation with early tracheostomy (48h vs. 14–16 days) in patients predicted to need >2 weeks of ventilation
- COVID-19: aerosol-generating procedure; airborne precautions required; retrospective data favor tracheostomy after 10–14 days of ventilation
Complications
Perioperative:
- Peristomal bleeding (anterior jugular veins, thyroid isthmus)
- Posterior tracheal / esophageal wall laceration
- Extraluminal (false tract) placement
- Loss of airway
Long-term:
- Tracheal stenosis
- Tracheomalacia
- Tracheo-innominate artery fistula (rare but life-threatening)
- Granulation tissue / stomal infection
- Difficulty decannulating (especially in neurological patients)
Dedicated Tracheostomy Teams
Multidisciplinary tracheostomy teams have been shown to reduce time to decannulation, length of stay, and adverse events. — Sabiston Textbook of Surgery
Key Sources: Cummings Otolaryngology Head and Neck Surgery, 6th ed. | Sabiston Textbook of Surgery, 21st ed. | Rosen's Emergency Medicine, 9th ed.
This is a shared conversation. Sign in to Orris to start your own chat.