Scarlet fever
Reading File
Finding Sources
Searching PubMed
scarlet fever streptococcal
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Here is a comprehensive overview of scarlet fever.
Scarlet Fever
Definition & Causative Agent
Scarlet fever is an acute febrile illness characterized by exudative pharyngitis, fever, and a scarlatiniform rash. It is most commonly caused by pyrogenic exotoxin-producing Group A β-hemolytic Streptococcus (Streptococcus pyogenes). Group C Streptococcus and, less commonly, Staphylococcus aureus can produce a similar syndrome.
- Primarily a childhood disease, most common in winter and early spring
- Up to 10% of childhood Group A streptococcal pharyngitis cases progress to scarlet fever
Pathogenesis
The rash is caused by erythrogenic (pyrogenic) exotoxins secreted by the streptococcal organism:
- SPEA, SPEB, SPEC — streptococcal pyrogenic exotoxins
- Most modern isolates express the less virulent SPEB and SPEC rather than SPEA, explaining reduced severity compared to historical epidemics
- The mechanism involves a combination of delayed-type hypersensitivity and superantigen-mediated immune activation
- SPEA shares homology with collagen, potentially underpinning rare autoimmune sequelae (rheumatic fever, renal failure)
Clinical Features
Prodrome (12 hours – 5 days post-exposure)
Abrupt onset of:
- High fever
- Pharyngitis / sore throat
- Headache
- Vomiting
- Abdominal pain
Exanthem (appears 1–2 days after onset)
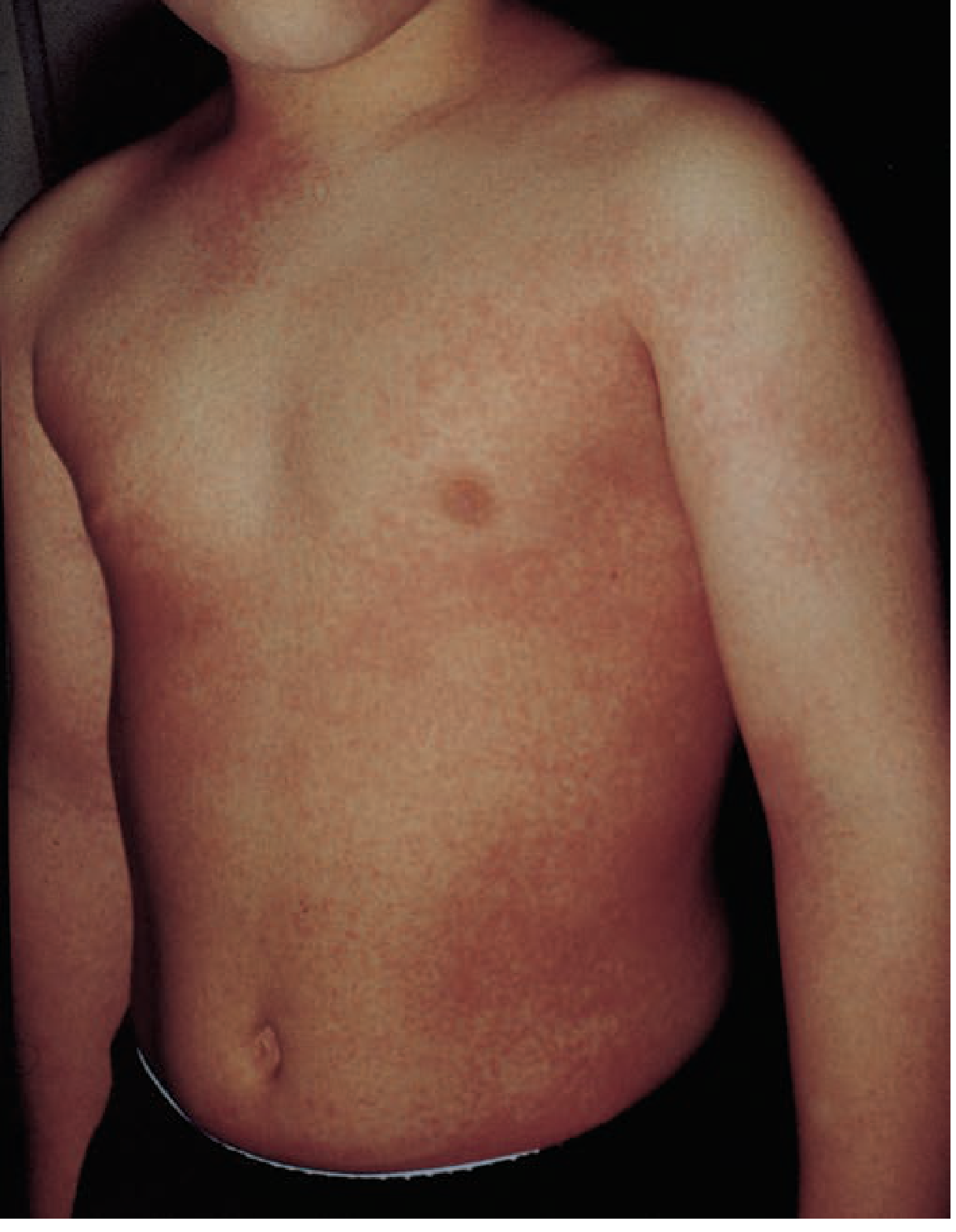
- Begins on the neck, axillae, and groin, spreads to trunk and extremities
- Spares palms and soles
- Fine punctate, 1–2 mm papules with a characteristic sandpaper texture
- Erythema blanches with pressure
- Mildly pruritic but usually not painful
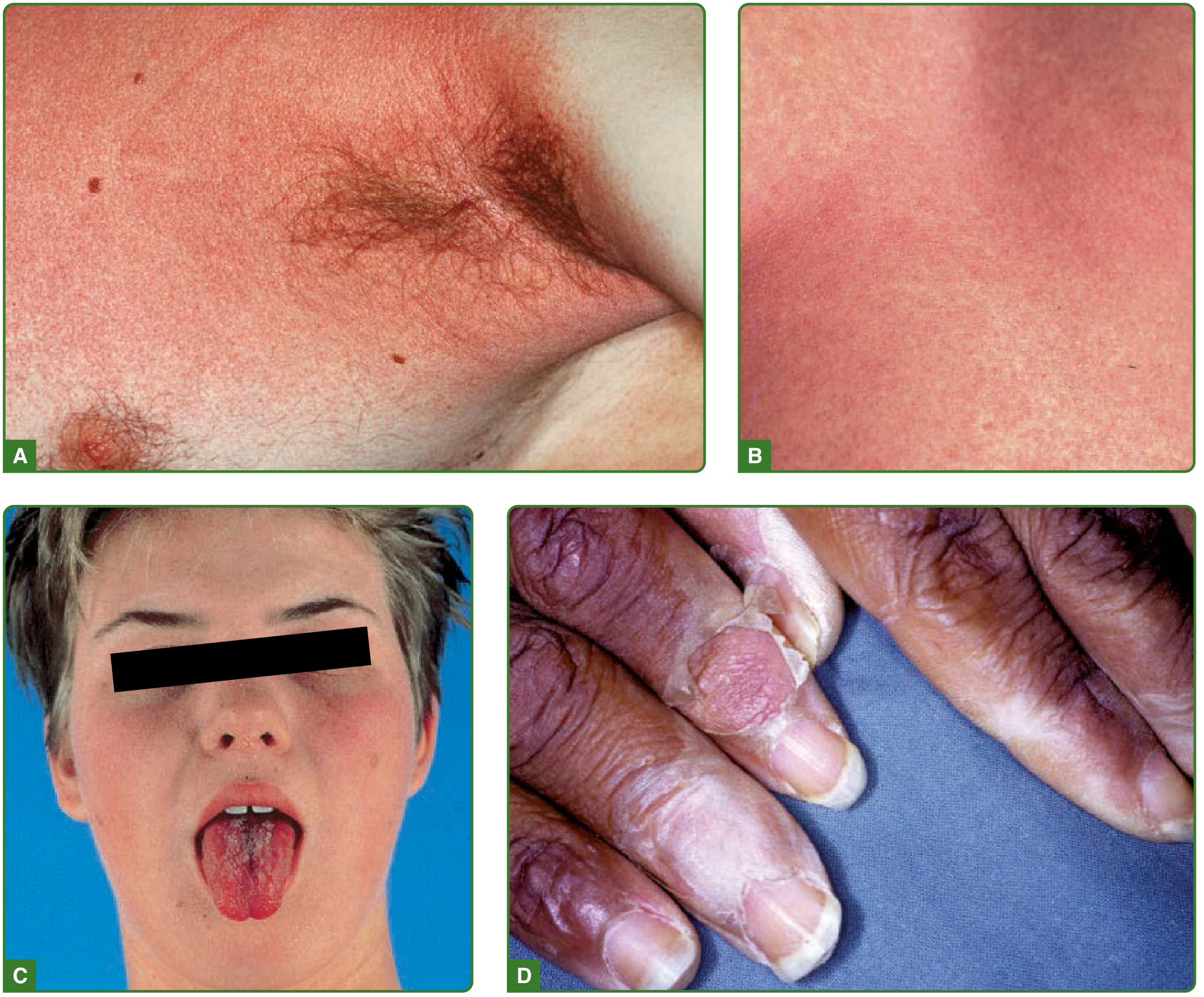
- Pastia lines: linear petechial streaks in antecubital and axillary folds (increased capillary fragility)
- Flushed face with circumoral pallor
- Rash fades at 3–4 days → brawny desquamation beginning on the face, then palms/fingers/soles (~1 week later, lasting up to 1 month)
Enanthem (oral findings)
- Tonsils and pharynx: red, edematous, with yellow/grey/white exudate
- Tender anterior cervical lymphadenopathy
- Forchheimer spots: petechiae and red macules on the soft palate and uvula
- White strawberry tongue (days 1–2): white coating with prominent red papillae projecting through
- Red strawberry tongue (after day 2–4): coating desquamates → bright red tongue with prominent papillae
Diagnosis
- Primarily clinical based on the characteristic signs
- Confirmed by rapid streptococcal antigen test or throat culture (Group A β-hemolytic streptococci)
- Usually benign course; morbidity signals suppurative complications
Complications
Suppurative
- Streptococcal adenitis
- Tonsillitis
- Otitis media
- Respiratory tract infection
Non-suppurative (late)
- Acute rheumatic fever (antibiotic treatment reduces this risk)
- Post-streptococcal glomerulonephritis (antibiotic effect on this is less clear)
Erythema marginatum may be seen in ~10% of cases — annular erythematous lesions that can recur over days to weeks.
Treatment
| Route | Drug | Dose |
|---|---|---|
| Oral | Penicillin VK | Children <27 kg: 250 mg 2–3×/day × 10 days; Adults: 250 mg 4×/day or 500 mg 2×/day × 10 days |
| IM | Benzathine penicillin (Bicillin C-R) | <27 kg: 600,000 units once; ≥27 kg: 1,200,000 units once |
| Oral | Amoxicillin | Alternative first-line |
| Oral (PCN allergy) | Cephalexin or Clindamycin | Preferred penicillin-allergic alternatives |
| Oral (PCN allergy) | Erythromycin / macrolides | Option, but macrolide resistance in GAS is increasing |
- Fever usually resolves within 12–24 hours of antibiotic initiation
- Recurrences are common
Staphylococcal Scarlet Fever (Scarlatiniform Erythroderma)
A distinct variant caused by S. aureus (typically expressing SEB):
- Nidus is usually skin (furuncles, carbuncles, abscesses) — no pharyngitis
- Same generalized sandpaper-texture erythroderma, but more tender
- Thick desquamation follows over ~1 week; no bullae (unlike SSSS)
- No risk of rheumatic fever or glomerulonephritis
- Suspect staphylococcal etiology when rash is present without pharyngitis — look for a skin nidus to culture
Differential Diagnosis
| Condition | Key Distinguishing Features |
|---|---|
| Kawasaki disease | Prolonged fever >5 days, negative cultures, coronary artery aneurysm risk |
| SSSS | Bullae, superficial exfoliation, no pharyngitis |
| Toxic Shock Syndrome | Hypotension, multi-organ involvement |
| Drug hypersensitivity | Drug history, peripheral eosinophilia, less mucosal involvement |
| Staphylococcal scarlet fever | No pharyngitis, skin nidus |
Sources: Fitzpatrick's Dermatology (Vol. 1–2), Tintinalli's Emergency Medicine, Rosen's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.