Venous return mbbs 1st year physiology
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
Reading File
Reading File
I now have all the content needed for a comprehensive MBBS 1st year answer. Let me compile it.
Venous Return — MBBS 1st Year Physiology
Definition
Venous return (VR) is the volume of blood flowing from the systemic circulation back to the right atrium per minute. Under steady-state conditions, venous return exactly equals cardiac output (~5 L/min at rest). Any process that impedes venous return will proportionally decrease cardiac output.
Three Principal Factors Governing Venous Return
- Right atrial pressure (RAP) — acts as a back-pressure; a rising RAP opposes venous inflow and reduces venous return.
- Mean systemic filling pressure (Psf) — the driving force that pushes blood from the periphery toward the heart.
- Resistance to venous return (RVR) — the total vascular resistance between the peripheral vessels and the right atrium.
Mean Systemic Filling Pressure (Psf)
When the heart is stopped experimentally (e.g. ventricular fibrillation), blood flow ceases and pressures everywhere equilibrate to a single value — the mean circulatory filling pressure (~7 mm Hg normally). The corresponding value measured only in the systemic circulation (excluding pulmonary) is the mean systemic filling pressure (Psf), also ~7 mm Hg.
Determinants of Psf:
| Factor | Effect on Psf |
|---|---|
| ↑ Blood volume | ↑ Psf (more stretch on vessel walls) |
| ↓ Blood volume (haemorrhage) | ↓ Psf |
| Sympathetic stimulation | ↑ Psf (venoconstriction reduces venous capacity) |
| Sympathetic inhibition | ↓ Psf (venodilation increases venous capacity) |
The graph below shows how blood volume and autonomic tone affect mean circulatory filling pressure:
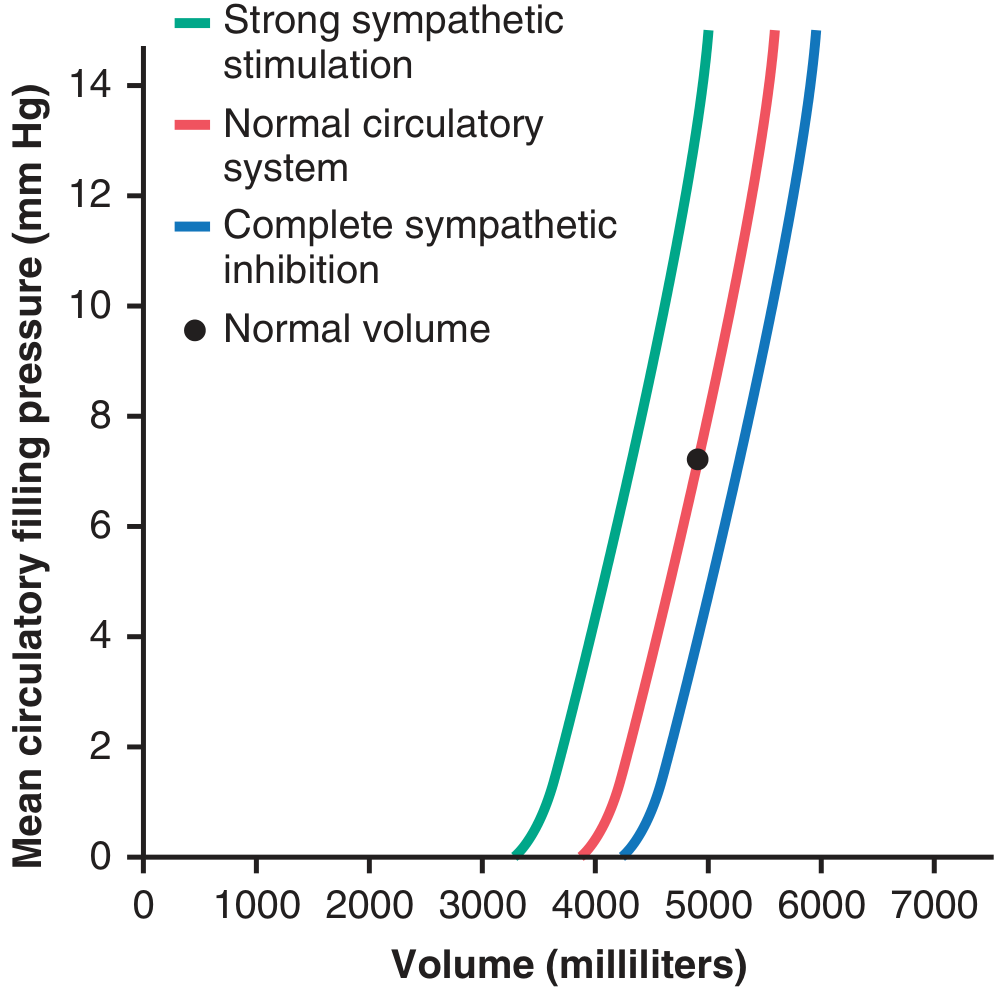
Normal blood volume (~5 L) → Psf = 7 mm Hg. Strong sympathetic stimulation doubles Psf to ~14 mm Hg.
Venous Return Formula
$$VR = \frac{P_{sf} - P_{RA}}{RVR}$$
Where:
- Psf = mean systemic filling pressure (≈ 7 mm Hg)
- P_RA = right atrial pressure (≈ 0 mm Hg normally)
- RVR = resistance to venous return (≈ 1.4 mm Hg/L/min)
The pressure gradient for venous return = Psf − RAP. This is the pressure difference that drives blood from the periphery back to the right atrium.
The Venous Return Curve
The venous return curve plots venous return (L/min) against right atrial pressure (mm Hg):
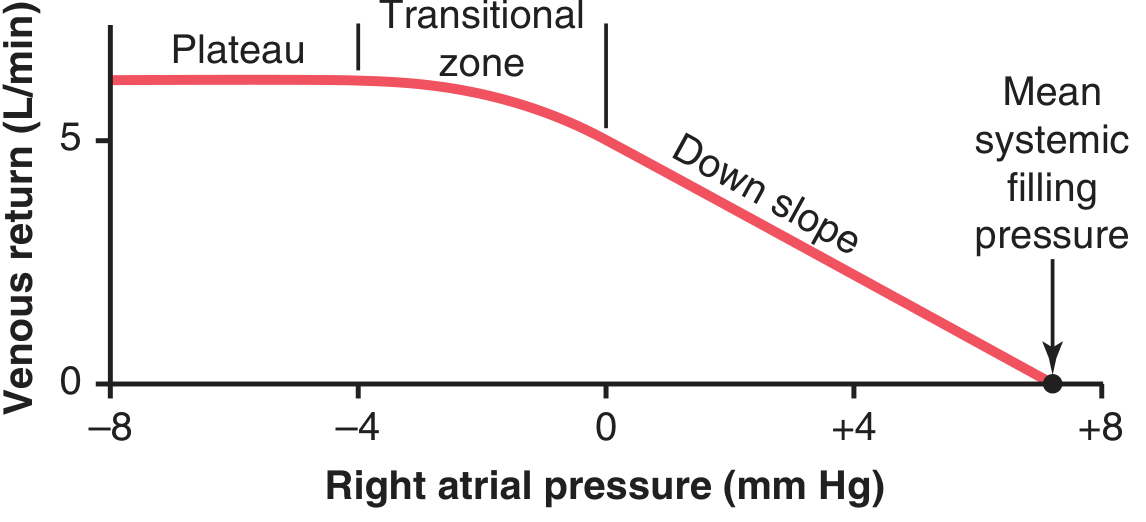
Figure 20.10 — Normal venous return curve. (Guyton & Hall, 13e)
Three Segments of the Curve
| Segment | Right atrial pressure | Explanation |
|---|---|---|
| Plateau | Very negative (< −4 mm Hg) | Large veins entering the chest collapse → venous return cannot increase further even as RAP falls |
| Transitional zone | −4 to 0 mm Hg | Veins partially open; venous return rises as RAP falls |
| Down-slope | 0 to +7 mm Hg | Linear decrease in venous return as RAP rises and opposes blood flow |
| Zero venous return | = Psf (~+7 mm Hg) | No pressure gradient; all flow stops |
Key point: When RAP equals Psf, the driving force (Psf − RAP = 0) and venous return = 0, regardless of how healthy the heart is.
Resistance to Venous Return
Most resistance to venous return resides in veins (~2/3) and the remainder in arterioles/small arteries (~1/3).
- When venous resistance ↑: blood dams in the highly distensible veins → venous pressure rises only slightly → poor compensation → venous return falls sharply.
- When arteriolar resistance ↑: blood dams in arteries (capacitance 1/30th of veins) → arterial pressure rises steeply → partially overcomes the resistance → less dramatic drop in venous return.
Increasing RVR rotates the venous return curve downward (reduced slope); decreasing RVR rotates it upward — but the curve always converges at the same point where RAP = Psf (venous return = 0).
Factors that Increase Venous Return
| Factor | Mechanism |
|---|---|
| ↑ Blood volume | ↑ Psf → ↑ driving pressure |
| Sympathetic stimulation | Venoconstriction → ↑ Psf; also ↑ HR and contractility |
| Exercise (skeletal muscle pump) | Rhythmic muscle contraction compresses veins → propels blood toward the heart; venous valves prevent backflow |
| Inspiration (respiratory pump) | Negative intrathoracic pressure expands the right atrium and great veins → "sucks" blood into the thorax |
| Arteriovenous fistula | Bypasses resistance → sharply ↑ venous return acutely |
| Venoconstriction | ↓ Venous capacitance → ↑ Psf |
Factors that Decrease Venous Return
| Factor | Mechanism |
|---|---|
| Haemorrhage / dehydration | ↓ Blood volume → ↓ Psf |
| ↑ Right atrial pressure | e.g. right heart failure → backpressure dams blood in veins |
| ↑ Peripheral vascular resistance (severe) | ↑ RVR |
| Standing upright | Gravity pools blood in dependent veins → ↓ effective filling |
| Sympathetic inhibition / spinal anaesthesia | Venodilation → ↓ Psf |
| Positive pressure ventilation | ↑ Intrathoracic pressure → compresses great veins → ↓ venous return |
Cardiac Output–Venous Return Matching
The operating point of the cardiovascular system is where the cardiac function curve (cardiac output vs. RAP) intersects the venous return curve. At this intersection, cardiac output = venous return, and the system is in steady state.
- Sympathetic stimulation shifts both curves upward → new intersection at higher cardiac output with little change in RAP
- Heart failure shifts the cardiac function curve down → intersection moves left and down → low cardiac output at higher RAP
- Haemorrhage shifts the venous return curve left (lower Psf) → cardiac output falls
Summary Box
Venous return is driven by the pressure gradient (Psf − RAP) and opposed by RVR. The normal Psf is 7 mm Hg; normal RAP is ~0 mm Hg; normal venous return = 5 L/min. The venous return curve shows that as RAP rises toward Psf, venous return progressively falls to zero. The heart can only pump what it receives — venous return ultimately limits cardiac output.
Sources: Guyton and Hall Textbook of Medical Physiology, 13e (pp. 256–260); Costanzo Physiology, 7th ed. (pp. 163–165)
This is a shared conversation. Sign in to Orris to start your own chat.