step by step demonstrate cranial nerve examination properly
Reading File
Finding Sources
Finding Sources
Searching Images
cranial nerve examination clinical
Reading File
Reading File
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
I now have comprehensive textbook content and clinical images. Here is the complete, step-by-step cranial nerve examination guide:
Cranial Nerve Examination — Step-by-Step
Bare minimum to always perform: Check fundi, visual fields, pupil size and reactivity, extraocular movements, and facial movements.Examine CNs in numerical order, but group CN III, IV, VI together because of their shared function.
CN I — Olfactory Nerve
Test: Smell
- Often omitted unless inferior frontal lobe pathology is suspected (e.g., meningioma, anosmia post-head injury)
- Ask the patient to close their eyes
- Present a mild, familiar odorant (toothpaste, coffee) to each nostril separately
- Ask them to identify the smell
- Abnormal: Anosmia or hyposmia — unilateral suggests local pathology; bilateral suggests cribriform plate involvement or central cause
CN II — Optic Nerve
Test: Visual acuity, visual fields, and fundi
1. Visual Acuity
- Use a Snellen chart with the patient's glasses/contacts in place
- Test each eye separately
- Abnormal: Reduced acuity → optic neuritis, compressive lesion, glaucoma
2. Visual Fields (Confrontation)
- Face the patient at ~0.6–1.0 m (2–3 ft)
- Place your hands at the periphery of your visual fields in the plane midway between you and the patient
- Instruct the patient to look at the centre of your face and indicate when they see finger movement
- Test all four quadrants (inferior then superior), bilaterally and simultaneously
- Abnormal patterns:
- Monocular loss → ipsilateral optic nerve
- Bitemporal hemianopia → optic chiasm (e.g., pituitary adenoma)
- Homonymous hemianopia → contralateral optic tract/radiation
3. Fundoscopy (Ophthalmoscope)
- Examine the optic disc: colour, size, margins, swelling/elevation (papilloedema)
- Examine the retinal vessels: calibre, AV nicking, haemorrhages, exudates
CN III, IV, VI — Oculomotor, Trochlear, Abducens
Test: Pupils + extraocular movements (EOMs)
1. Pupils
- Note size, shape, and symmetry at rest (in room light and dim light)
- Test direct and consensual pupillary light reflex with a bright light
- Test accommodation: ask the patient to follow your finger as it approaches the bridge of the nose — look for miosis and convergence
- Abnormal findings:
- Fixed dilated pupil → CN III compression (parasympathetic fibres on the outside are compressed first)
- Pinpoint reactive pupils → pontine lesion (sympathetic tracts interrupted)
- Afferent pupillary defect (RAPD/Marcus Gunn) → optic nerve lesion
- Horner's syndrome (miosis + ptosis + anhidrosis) → sympathetic chain interruption
2. Extraocular Movements
- Ask the patient to keep their head still and follow your fingertip
- Move the target in an H pattern covering all six cardinal directions of gaze
- Observe for: paresis, diplopia, nystagmus, or abnormal smooth pursuit (saccadic intrusions)
- Test horizontal nystagmus at 45° (not at extreme lateral gaze) — hold the target for ≥ a few seconds to detect latent nystagmus
- Ask whether the patient sees double in any direction — true diplopia resolves when one eye is covered
- Lesion patterns:
- CN III palsy: "down and out" eye, ptosis, dilated unreactive pupil
- CN IV palsy: failure of intorsion; vertical diplopia worse on down-gaze; head tilt to opposite side
- CN VI palsy: failure of abduction; horizontal diplopia on ipsilateral gaze
CN V — Trigeminal Nerve
Test: Facial sensation + jaw muscles
1. Sensory (Three Divisions)
- Test light touch and temperature (two modalities from different pathways) over the forehead (V1 — ophthalmic), cheek (V2 — maxillary), and jaw (V3 — mandibular) bilaterally
- A cotton wisp for light touch and a cool tuning fork for temperature are sufficient for screening
- Abnormal: Unilateral or divisional loss → cavernous sinus, skull base, trigeminal neuralgia, MS plaque
2. Corneal Reflex (if indicated)
- Lightly touch the cornea with a wisp of cotton from the side (avoid the conjunctiva and air current)
- Normal response: bilateral blink (afferent = CN V, efferent = CN VII)
- Absent direct reflex: ipsilateral CN V or CN VII lesion
3. Motor (Jaw Muscles)
- Ask the patient to clench their teeth — palpate the masseters bilaterally
- Ask the patient to open their mouth against resistance
- Abnormal: Jaw deviates toward the weak side on opening (pterygoids); unilateral wasting of masseter
CN VII — Facial Nerve
Test: Facial expression muscles (upper vs. lower face distinction is critical)
- Observe for facial asymmetry at rest and with spontaneous expression
- Ask the patient to:
- Raise their eyebrows / wrinkle the forehead
- Close their eyes tightly (try to open them) — Bell's phenomenon (upward eye roll) is normal
- Show their teeth / smile
- Puff out their cheeks (hold air in against resistance)
- UMN vs. LMN:
- UMN lesion (contralateral cerebral hemisphere): lower face weakness (nasolabial fold flattening, corner of mouth drooping), forehead spared (bilateral cortical representation)
- LMN lesion (peripheral — e.g., Bell's palsy, parotid): entire ipsilateral face affected including forehead wrinkling and eye closure
Also test taste on the anterior 2/3 of the tongue (sweet/salty) if a peripheral lesion is suspected — chorda tympani branch of CN VII.

CN VIII — Vestibulocochlear Nerve
Test: Hearing + vestibular function
1. Hearing (Cochlear)
- Screen with a finger rub or whispered voice beside each ear while occluding the other
- Rinne test (512 Hz tuning fork): compare air conduction (fork beside ear) vs. bone conduction (fork on mastoid)
- Air > Bone = Normal OR sensorineural loss
- Bone > Air = Conductive loss (e.g., otosclerosis, effusion)
- Weber test (512 Hz fork on vertex): lateralises to the worse ear in conductive loss, better ear in sensorineural loss
2. Vestibular
- Observe for spontaneous nystagmus (direction, fixation suppression)
- Head impulse test (HIT/Halmagyi): rapidly turn the head 10–20° to one side — corrective saccade indicates peripheral hypofunction
- Dix-Hallpike manoeuvre: for BPPV
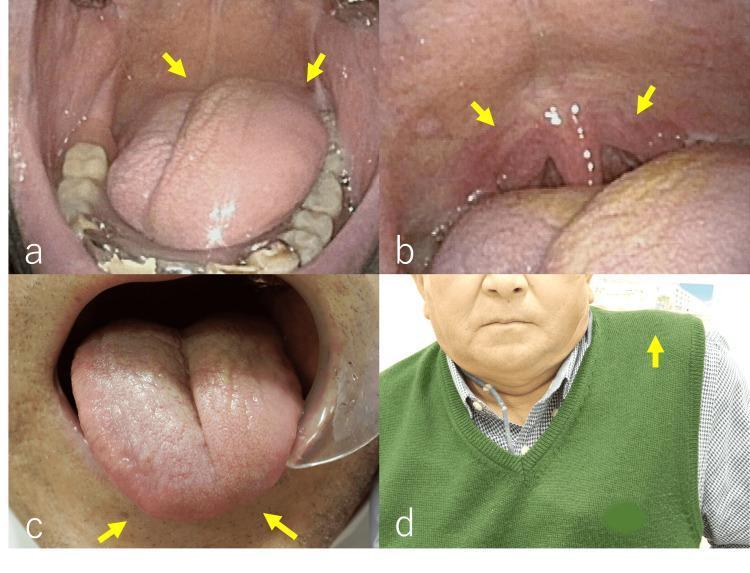
CN IX & X — Glossopharyngeal & Vagus Nerves
Test together (overlapping functions)
- Listen to the patient's voice — hoarseness or nasal quality suggests CN X palsy
- Ask the patient to open their mouth and say "Aah"
- Observe the soft palate: it should rise symmetrically in the midline
- Uvular deviation: deviates away from the weak side (pulled toward the normal side)
- Gag reflex (use only when clinically necessary — uncomfortable):
- Touch the posterior pharyngeal wall with a spatula
- Afferent = CN IX; Efferent = CN X
- An absent gag has low clinical significance in isolation; compare both sides
- Swallowing: ask about or observe for dysphagia/aspiration
CN XI — Spinal Accessory Nerve
Test: Sternocleidomastoid (SCM) + trapezius
- Trapezius: ask the patient to shrug their shoulders against your downward resistance — look and feel for asymmetry
- SCM: ask the patient to turn their head to one side against resistance — the contralateral SCM contracts (CN XI innervates ipsilateral SCM but turns head contralaterally)
- Abnormal: Ipsilateral shoulder drop, winging of scapula, weakness turning head away from lesion side
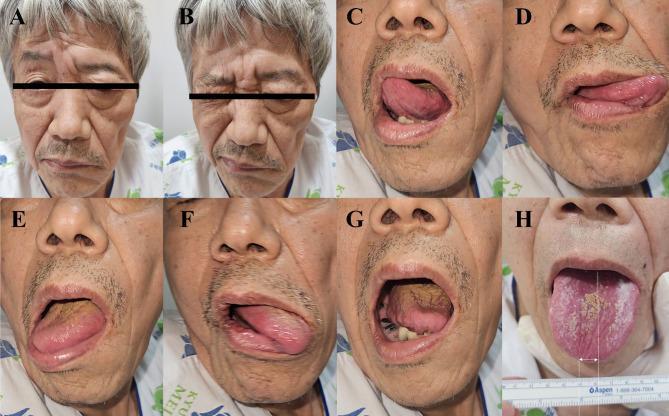
CN XII — Hypoglossal Nerve
Test: Tongue movement
- Ask the patient to open their mouth — inspect the tongue at rest for wasting or fasciculations (LMN lesion)
- Ask the patient to protrude the tongue
- Deviation = toward the weak/lesion side (the unopposed contralateral genioglossus pushes it that way)
- Ask the patient to push the tongue into each cheek against your resistance
Summary Table
| CN | Name | Key Test | Abnormal Finding |
|---|---|---|---|
| I | Olfactory | Identify odour (each nostril) | Anosmia |
| II | Optic | Acuity, fields, fundi | Field defects, papilloedema |
| III | Oculomotor | Pupil, EOM ("down-out"), ptosis | Fixed dilated pupil, EOM palsy |
| IV | Trochlear | Down-and-in movement | Vertical diplopia, worse on down-gaze |
| VI | Abducens | Lateral gaze | Failure to abduct |
| V | Trigeminal | Face sensation, jaw clench, corneal reflex | Divisional sensory loss, jaw deviation |
| VII | Facial | Facial expression, eye closure | UMN (lower face) vs. LMN (whole face) |
| VIII | Vestibulocochlear | Whisper, Rinne/Weber, HIT | Hearing loss, nystagmus |
| IX/X | Glossopharyngeal/Vagus | Palate elevation, voice, gag | Uvular deviation, hoarseness |
| XI | Accessory | Shrug, head turn | Shoulder drop, weakness |
| XII | Hypoglossal | Tongue protrusion | Deviation toward weak side |
Sources: Harrison's Principles of Internal Medicine 22E; Goldman-Cecil Medicine (International Edition)
This is a shared conversation. Sign in to Orris to start your own chat.