How to do examination of patient woth potential diagnosis of pemphigus vulgaris or folaciis
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Loading Image
I now have all the material needed for a comprehensive answer. Here is a structured guide to examining a patient with suspected pemphigus vulgaris (PV) or pemphigus foliaceus (PF), drawn from Fitzpatrick's Dermatology.
Examination of a Patient with Suspected Pemphigus Vulgaris or Pemphigus Foliaceus
1. History
Before the physical exam, gather:
- Symptom onset: PV often begins with painful oral ulcers weeks to months before any skin lesions. PF rarely involves mucous membranes.
- Symptoms: Pain/burning in skin lesions (both types); pruritus less common
- Drug history: Penicillamine, captopril, and other thiols/phenols can trigger drug-induced pemphigus — ask specifically
- UV exposure: Both PV and PF can be exacerbated by ultraviolet radiation
- Ethnic background: PV is more prevalent in Jewish, Mediterranean, and Middle Eastern populations
- Associated diseases: Ask about myasthenia gravis and thymoma (associated with pemphigus)
- Family history: Endemic PF (fogo selvagem) has geographic clustering
2. Full Skin Examination
Primary Lesion
- PV: Look for flaccid blisters arising on normal-appearing or erythematous skin. These are fragile and rupture easily, so the more common finding is large erosions that tend to spread at their periphery.
- PF: The primary blisters are typically not found — they rupture so superficially that you see scaly, crusted erosions on an erythematous base instead.
Distribution
| Feature | PV | PF |
|---|---|---|
| Trunk/limbs | Yes — widespread | Yes |
| Face/scalp | Yes | Yes — seborrheic distribution (face, scalp, upper trunk) |
| Intertriginous areas | Common (vegetating lesions) | Less prominent |
| Palms/soles | Typically spared | Typically spared |
PF characteristically starts in a seborrheic distribution (face, scalp, upper chest/back) and may remain localized for years or progress to generalised exfoliative erythroderma.
Nikolsky Sign (Critical Examination Maneuver)
Two components to assess:
- Direct Nikolsky sign: Apply tangential mechanical shear force (lateral pressure or rubbing) to normal-appearing skin distant from active lesions — positive if an erosion is induced
- Marginal Nikolsky (Asboe-Hansen sign): Press the top of an intact blister laterally — positive if the blister extends into adjacent skin
A positive Nikolsky sign is a hallmark of pemphigus. It reflects the fragility of intraepidermal adhesion due to anti-desmoglein antibodies. Note: it is not specific to pemphigus — also positive in staphylococcal scalded skin syndrome, Stevens-Johnson syndrome, and toxic epidermal necrolysis.
Lesion Character
- Note whether erosions are spreading at periphery (typical PV)
- Look for vegetating/papillomatous lesions with crusting, especially in intertriginous areas, scalp, and face — this is pemphigus vegetans, a variant of PV with generally better prognosis
- PF erosions: Scaly, crusted, can become confluent and progress to erythroderma
PV — Extensive Erosions
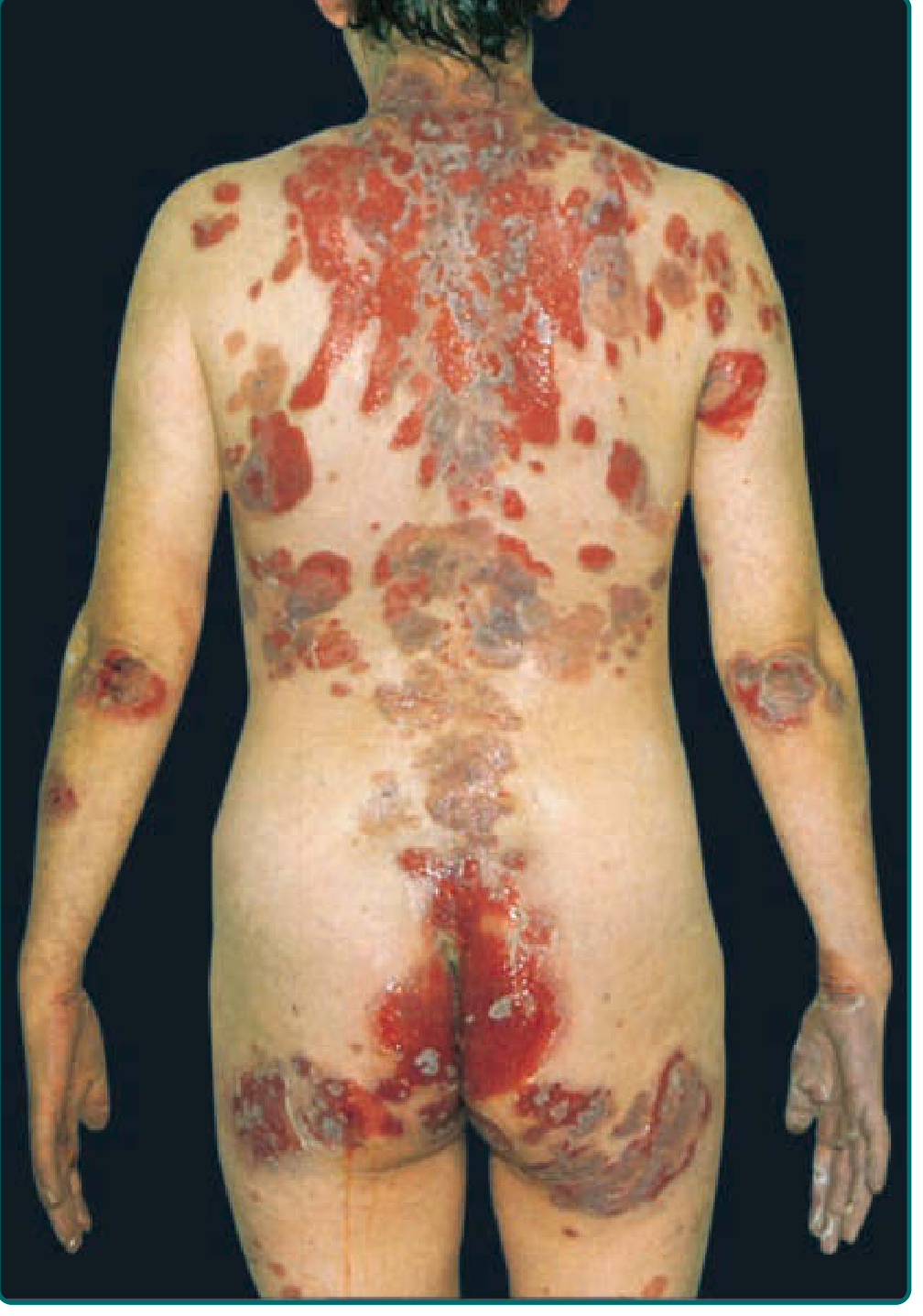
PF — Scaly Crusted Lesions and Erythroderma
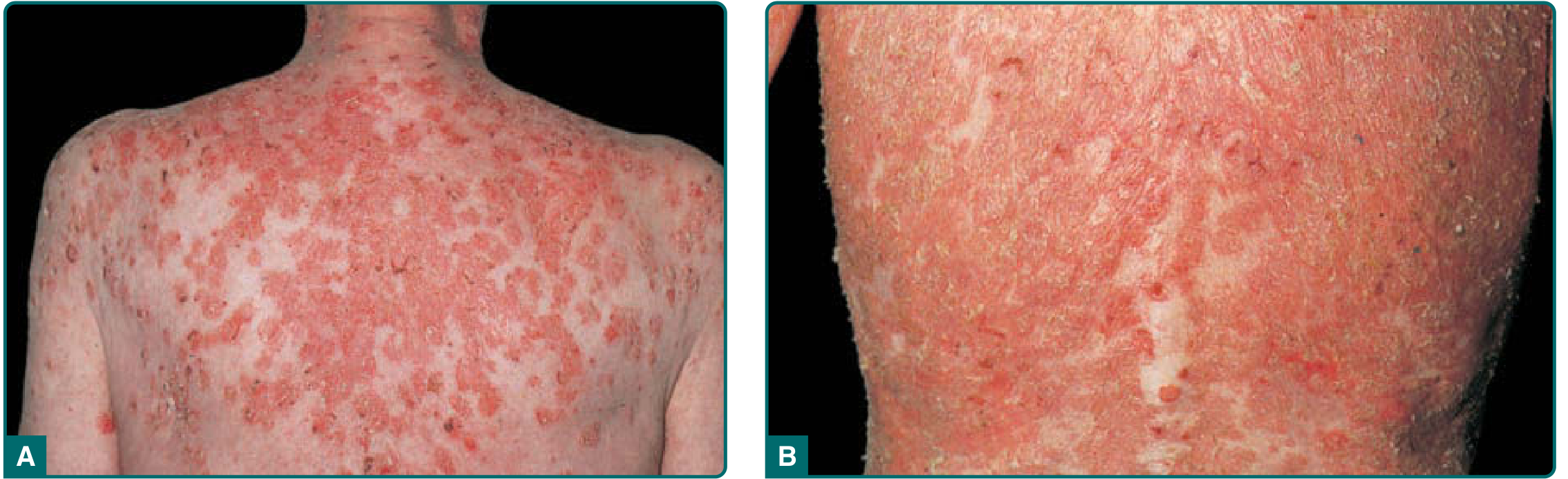
3. Mucous Membrane Examination
This is one of the most differentiating features between PV and PF:
Pemphigus Vulgaris — Mucous Membrane Involvement is the Rule
- 87% of PV patients have ear, nose, or throat lesions (endoscopic data)
- Most commonly: nasal mucosa (76%), pharynx (66%), larynx (55%)
- Oral cavity: Nearly all PV patients develop oral lesions — examine for:
- Erosions on the buccal mucosa, palate, gingiva, and floor of mouth
- Gingival lesions — "desquamative gingivitis" appearance
- Intact blisters are rarely seen intraorally; erosions are the primary finding
- Conjunctiva: Can be involved — look for erosions
- Genitalia and anus: Perianal, vulval, and penile erosions occur — examine these areas
- Oesophagus: Oesophageal involvement occurs; ask about dysphagia
Pemphigus Foliaceus — Mucous Membranes are SPARED
- Mucous membrane involvement is extremely rare, essentially absent in PF, even with widespread disease
- This is a key clinical differentiator
4. Hair and Nails
- Hair loss is not typical in pemphigus, but temporary alopecia occurs in ~5% of PV patients and can rarely be a presenting sign
- Examine the scalp closely, as both PV and PF can have scalp lesions; PF particularly favours the scalp in its seborrheic distribution
5. Summary: Key Clinical Differences Between PV and PF
| Feature | Pemphigus Vulgaris (PV) | Pemphigus Foliaceus (PF) |
|---|---|---|
| Primary lesion | Flaccid blister | Superficial/rarely seen |
| Lesion morphology | Large spreading erosions | Scaly, crusted erosions |
| Distribution | Widespread, any site | Seborrheic (face, scalp, upper trunk) |
| Mucous membranes | Always involved (oral, nasal, genital) | Never involved |
| Nikolsky sign | Positive | Positive |
| Progression | Widespread erosions | Can progress to erythroderma |
| Pain/burning | Pain | Burning > pain |
6. Investigations to Confirm Diagnosis
After clinical examination, the following confirm the diagnosis:
| Test | PV Finding | PF Finding |
|---|---|---|
| Skin biopsy (H&E) | Suprabasal acantholysis (split above basal layer) | Subcorneal/granular layer acantholysis |
| Direct immunofluorescence (DIF) | Intercellular IgG + C3 deposition (cell surface pattern) | Same intercellular IgG pattern |
| Indirect immunofluorescence (IIF) | Circulating anti-desmoglein IgG (monkey oesophagus substrate) | Same pattern |
| Anti-Dsg ELISA | Anti-Dsg3 ± anti-Dsg1 | Anti-Dsg1 only |
Biopsy site selection: Take biopsy from the edge of an active blister or erosion — not from the centre of an old erosion, which yields non-specific findings. For DIF, biopsy perilesional normal-appearing skin (2 cm from a lesion).
Sources: Fitzpatrick's Dermatology (9th ed.), Chapter 52 — Pemphigus
This is a shared conversation. Sign in to Orris to start your own chat.