SYSTEMIC LUPUS Erythematosis
Reading File
Finding Sources
Finding Sources
Searching Images
systemic lupus erythematosus butterfly rash clinical
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
I now have comprehensive information. Let me compile the full response.
Systemic Lupus Erythematosus (SLE)
Definition & Overview
SLE is a generalized autoimmune disease of unknown cause characterized by the production of antibodies to numerous antigens — most importantly, antibodies directed against the cell nucleus (ANAs). Immune complex deposition results in inflammation and vasculitis, causing multiorgan pathology. — Textbook of Family Medicine 9e
Epidemiology
- Predominantly affects young to middle-aged women (peak ages 15–40)
- Female:male ratio is 2:1 before puberty, rising to 4:1 after puberty
- Prevalence ~1 in 1000–2500 in the general population; up to 1 in 250 in African American women aged 18–65
- Strong familial tendency; associated with MHC genes DR2, DR3, DR4, DR5
- 5-year survival rate: ~90% after diagnosis
- Monozygotic twin concordance is only ~25%, indicating environmental triggers are critical
Pathogenesis
| Mechanism | Detail |
|---|---|
| Genetic susceptibility | >100 loci identified; HLA-DR3, C4 null alleles (Europeans), DNASE1L3, TREX1 mutations |
| Autoantibody production | Anti-dsDNA, anti-Sm, anti-Ro/SSA, anti-La/SSB, antiphospholipid antibodies |
| Immune complex deposition | Complement-mediated tissue damage; reduced clearance by reticuloendothelial system |
| T-cell dysfunction | Reduced T-suppressor cell function; B-cell overproduction of γ-globulins |
| Type I interferon pathway | Increased IFN-inducible proteins; nucleic acid sensing gene abnormalities |
| Triggers | UV light (externalizes Ro/SSA antigen), infections, stress, drugs, hormones |
— Andrews' Diseases of the Skin 13e; Textbook of Family Medicine 9e
Clinical Manifestations
(From Harrison's Principles of Internal Medicine 22E, Table 368-1)
| System | Features |
|---|---|
| Constitutional | Fatigue, malaise, fever, weight loss |
| Cutaneous | Photosensitivity, malar rash, discoid rash, SCLE, oral/nasal ulcers, alopecia, bullous lupus, vasculitic lesions |
| Musculoskeletal | Arthralgia, polyarthritis, myalgia, Jaccoud deformity, avascular necrosis |
| Renal | Proteinuria ≥500 mg/24h, cellular casts, nephrotic syndrome, ESRD |
| Neuropsychiatric | Cognitive dysfunction, seizures, psychosis, stroke, transverse myelitis, mood disorders |
| Cardiopulmonary | Pleuritis, pericarditis, myocarditis, Libman-Sacks endocarditis, pneumonitis, pulmonary hypertension |
| Hematologic | Hemolytic anemia, leukopenia, lymphopenia, thrombocytopenia, venous/arterial thrombosis |
| Vascular | Raynaud's phenomenon, stroke, MI, DVT/PE |
| GI | Nausea, abdominal pain, elevated liver enzymes, lupus peritonitis, pancreatitis |
| Ocular | Sicca syndrome, episcleritis, retinal vasculitis |
Cutaneous Manifestations in Detail
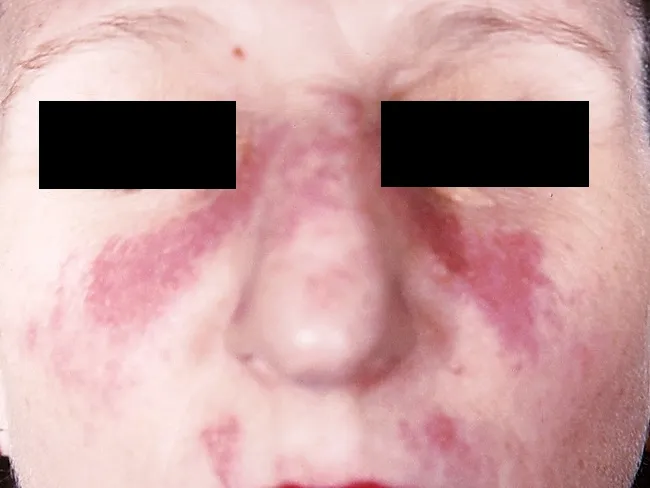
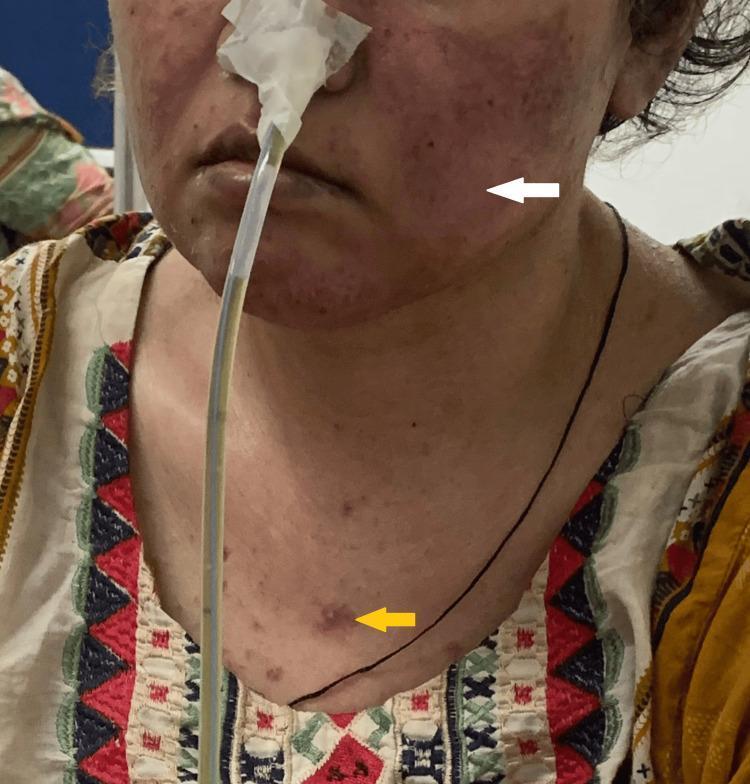
The butterfly (malar) rash — the hallmark that gave lupus its name (Latin: wolf) — appears in only one-third of patients, typically after sun exposure, affecting the malar area and nasal bridge with characteristic sparing of the nasolabial folds (unlike dermatomyositis). Edema may be present; biopsies show interface dermatitis with perivascular lymphoid infiltrate. It resolves without scarring.
Subacute cutaneous LE (SCLE) occurs in sun-exposed areas (upper torso) as annular or papulosquamous lesions; ~70% have anti-Ro antibodies; no scarring.
Discoid LE (DLE): Raised, adherent-scaled plaques with follicular plugging; heals with scarring and dyspigmentation.
Bullous LE: Vesicles or bullae, often widespread.
— Andrews' Diseases of the Skin 13e; Textbook of Family Medicine 9e
Classic Malar (Butterfly) Rash
Diagnostic Criteria
ACR 11-Criteria (≥4 required for diagnosis)
- Malar rash
- Discoid rash
- Photosensitivity
- Oral ulcers
- Arthritis (non-erosive)
- Serositis (pleuritis or pericarditis)
- Renal disorder (proteinuria >0.5 g/day or cellular casts)
- Neurologic disorder (seizures or psychosis without other cause)
- Hematologic disorder (hemolytic anemia, leukopenia, thrombocytopenia)
- Immunologic disorders (anti-dsDNA, anti-Sm, APLAs)
- Positive ANA
Four of these 11 criteria, present serially or simultaneously, confirm the diagnosis. Note that 4 of the 11 are mucocutaneous findings.
SLICC Criteria (higher sensitivity)
≥4 criteria including ≥1 clinical AND ≥1 immunologic, OR biopsy-proven lupus nephritis with positive ANA or anti-dsDNA.
The newer EULAR/ACR 2019 criteria require ANA ≥1:80 as an entry criterion.
— Andrews' Diseases of the Skin 13e; Harrison's 22E
Autoantibodies
| Antibody | Prevalence in SLE | Specificity | Clinical Correlation |
|---|---|---|---|
| ANA | ~95–99% | Low | Best screening test |
| Anti-dsDNA | 40–60% | 75–99% | Disease activity, lupus nephritis |
| Anti-Sm | ~30% | 55–100% | Highly specific for SLE |
| Anti-Ro/SSA | ~30–40% | Moderate | SCLE, photosensitivity, neonatal lupus |
| Anti-La/SSB | ~15–20% | Moderate | Neonatal lupus, secondary Sjögren's |
| Antiphospholipid (APLAs) | ~30–40% | Moderate | Thrombosis, pregnancy loss |
Anti-dsDNA and anti-Sm are essentially diagnostic of SLE when positive.
— Harrison's 22E; Andrews' Diseases of the Skin 13e
Lupus Nephritis
Renal involvement is a major determinant of prognosis. ISN/RPS classes:
| Class | Histology |
|---|---|
| I | Minimal mesangial |
| II | Mesangial proliferative |
| III | Focal proliferative (<50% glomeruli) |
| IV | Diffuse proliferative (≥50% glomeruli) — most severe |
| V | Membranous |
| VI | Advanced sclerotic |
Classes III, IV, V (and combinations) require active immunosuppression.
Special Situations
Neonatal lupus: Anti-Ro/anti-La antibodies cross the placenta → complete heart block, transient cutaneous lupus, and cytopenias in the neonate.
Drug-induced lupus: Hydralazine, procainamide, isoniazid, minocycline, TNF inhibitors. Associated with anti-histone antibodies; resolves on drug withdrawal.
Pregnancy: SLE increases risk of miscarriage (especially with APLAs), fetal growth restriction, and preeclampsia. Postpartum flares are common.
Management
General Principles
- All patients: hydroxychloroquine (reduces flares, organ damage, mortality — mainstay)
- Avoid UV light, use broad-spectrum sunscreen
- Screen for and manage cardiovascular risk factors (accelerated atherosclerosis)
Organ-specific Treatment
| Manifestation | Treatment |
|---|---|
| Mild (skin, joints) | Hydroxychloroquine, NSAIDs, low-dose corticosteroids, topical steroids |
| Moderate–severe | Systemic corticosteroids + immunosuppressants (azathioprine, MMF) |
| Lupus nephritis (class III/IV) | MMF or cyclophosphamide + corticosteroids; belimumab or voclosporin as add-on |
| Refractory nephritis | Rituximab (anti-CD20) |
| Hemolytic anemia / severe thrombocytopenia | Rituximab, corticosteroids |
| APS/thrombosis | Warfarin (preferred over DOACs) |
| CNS lupus (psychosis, vasculitis, TM) | High-dose steroids + MMF, cyclophosphamide, or rituximab |
| Serositis | NSAIDs, colchicine, low-dose steroids |
Biologics
- Belimumab (anti-BLyS): FDA-approved for SLE and lupus nephritis
- Voclosporin (calcineurin inhibitor): FDA-approved (2021) for lupus nephritis
- Anifrolumab (anti-IFN-α receptor): FDA-approved for active SLE
— Harrison's Principles of Internal Medicine 22E; Textbook of Family Medicine 9e; Andrews' Diseases of the Skin 13e
Prognosis & Monitoring
- Major causes of early death: active lupus, infections (immunosuppression), renal failure
- Major causes of late death: cardiovascular disease (accelerated atherosclerosis), damage accrual
- Monitor with anti-dsDNA titers and complement levels (C3/C4) — low C3/C4 + rising anti-dsDNA = impending flare
- Screen regularly for lupus nephritis (urine protein:creatinine ratio, sediment), blood pressure, lipids, and bone density (if on steroids)
This is a shared conversation. Sign in to Orris to start your own chat.