Angle closure glaucoma
Reading File
Finding Sources
Searching PubMed
"angle closure glaucoma"[MeSH Terms] AND management
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
Loading Image
Reading File
Reading File
I now have comprehensive information from Kanski's Clinical Ophthalmology, Goldman-Cecil Medicine, and Tintinalli's Emergency Medicine. Let me compile a thorough, well-structured answer.
Angle Closure Glaucoma
Definition & Overview
Angle closure glaucoma refers to obstruction of the trabecular meshwork by the peripheral iris (iridotrabecular contact — ITC), blocking aqueous outflow and raising intraocular pressure (IOP). It can be:
- Primary — occurs in anatomically predisposed eyes
- Secondary — caused by another ocular or systemic factor
Primary angle-closure glaucoma (PACG) accounts for up to half of all glaucoma cases globally and is disproportionately common in Asia. It progresses more rapidly and causes more visual loss than primary open-angle glaucoma (POAG). — Kanski's Clinical Ophthalmology, 10e
Classification (Spectrum)
| Stage | Definition |
|---|---|
| Primary angle-closure suspect (PACS) | Occludable angle on gonioscopy, no ITC, no raised IOP, no optic nerve damage |
| Primary angle closure (PAC) | ITC in ≥3 quadrants ± raised IOP, but no glaucomatous optic neuropathy |
| Primary angle-closure glaucoma (PACG) | ITC + raised IOP + glaucomatous optic neuropathy |
| Acute primary angle closure (APAC) | Sudden complete closure causing acute crisis |
Pathophysiology
The dominant mechanism is relative pupillary block:
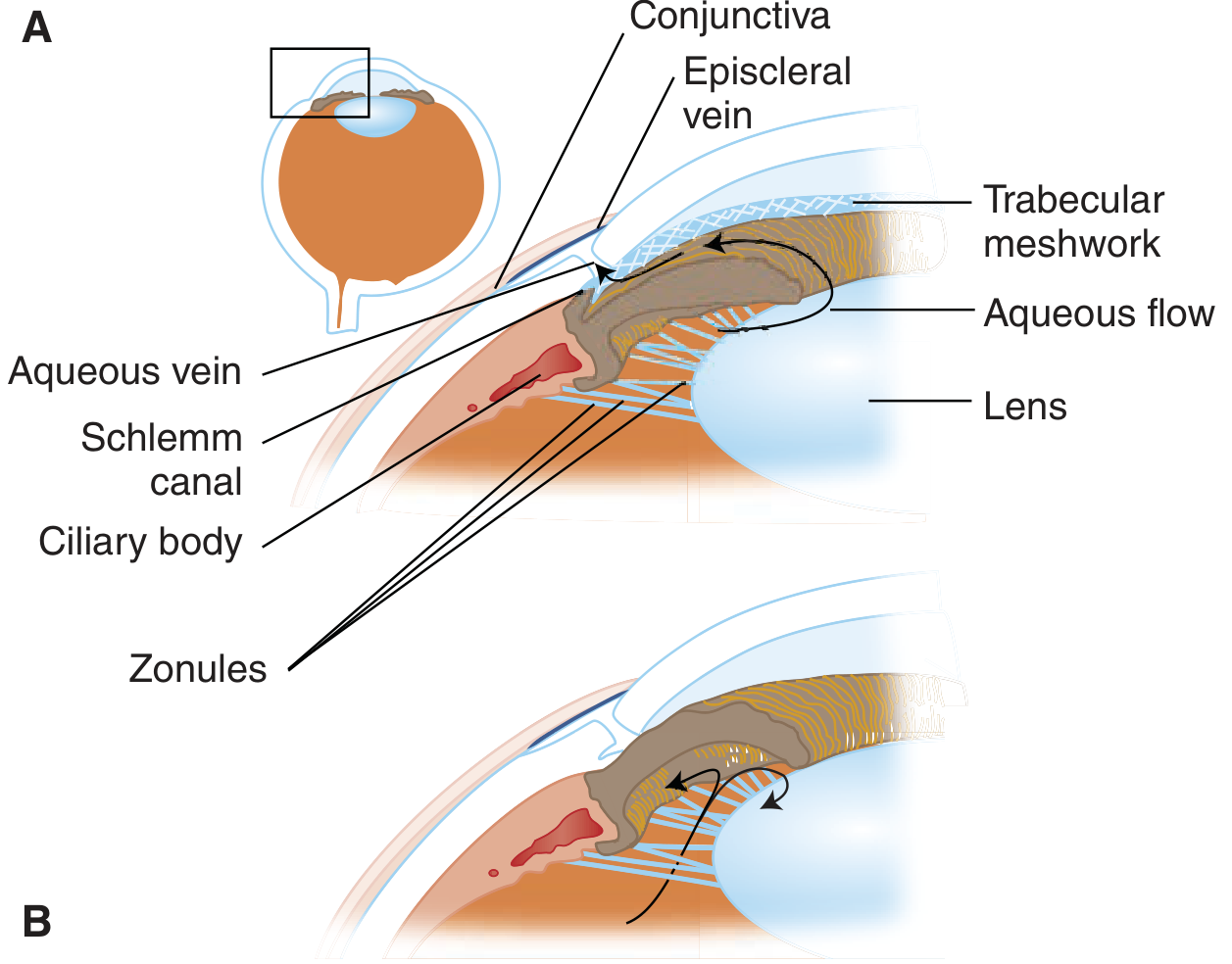
Normal aqueous flow (A) vs angle closure with pupillary block and iris bombé (B) — Tintinalli's Emergency Medicine
- Aqueous is produced by the ciliary body and normally flows from the posterior chamber → through the pupil → into the anterior chamber → exits via the trabecular meshwork into Schlemm's canal.
- When the posterior iris surface contacts the anterior lens surface, a pressure differential builds between the posterior and anterior chambers.
- This bows the peripheral iris forward (iris bombé), narrowing and eventually closing the trabecular meshwork angle.
- IOP rises rapidly — from a normal 10–20 mmHg to 50–80+ mmHg.
- When IOP exceeds the corneal pump's capacity, corneal epithelial oedema develops → blurred vision and halos.
The mid-dilated pupil state is the most dangerous: the iris is thickest peripherally while still partially covering the lens, maximising pupillary block. Dilation to a widely dilated or miotic state actually reduces risk.
Additional mechanisms (especially in Asians):
- Plateau iris configuration — anteriorly rotated ciliary processes hold the peripheral iris in a forward position; not relieved by iridotomy alone
- Phacomorphic closure — swollen or anteriorly subluxated lens
Risk Factors
| Factor | Detail |
|---|---|
| Hypermetropia (farsightedness) | Short axial length, shallow anterior chamber, narrow angle; up to 1 in 6 hyperopes ≥1 D are PACS |
| Age | Lens thickens with age, pushing iris forward |
| Female sex | More commonly affected than males |
| Asian ethnicity | Far Eastern and Indian Asians particularly at risk |
| Family history | Genetic factors, increased prevalence in first-degree relatives |
| Short axial length / nanophthalmos | Axial length <20 mm = very high risk |
| Cataracts | Increase lens vault |
Precipitating Factors for Acute Attack
- Pharmacological mydriasis (atropine, antihistamines, TCAs, cold/flu remedies, motion sickness patches)
- Sympathomimetics (epinephrine, pseudoephedrine, intranasal cocaine)
- Nebulized bronchodilators (albuterol + ipratropium) in ICU patients
- Topiramate and other sulfa derivatives (cause ciliary body effusion)
- Dim illumination / watching TV in a dark room
- Semi-prone position (e.g. reading)
- Acute emotional stress
Clinical Features
Symptoms
- Acute: sudden severe periocular/orbital pain, markedly decreased vision, nausea and vomiting (may simulate acute abdomen), headache
- Subacute/intermittent: blurring ("smoke-filled room") and haloes around lights from transient corneal oedema
Signs
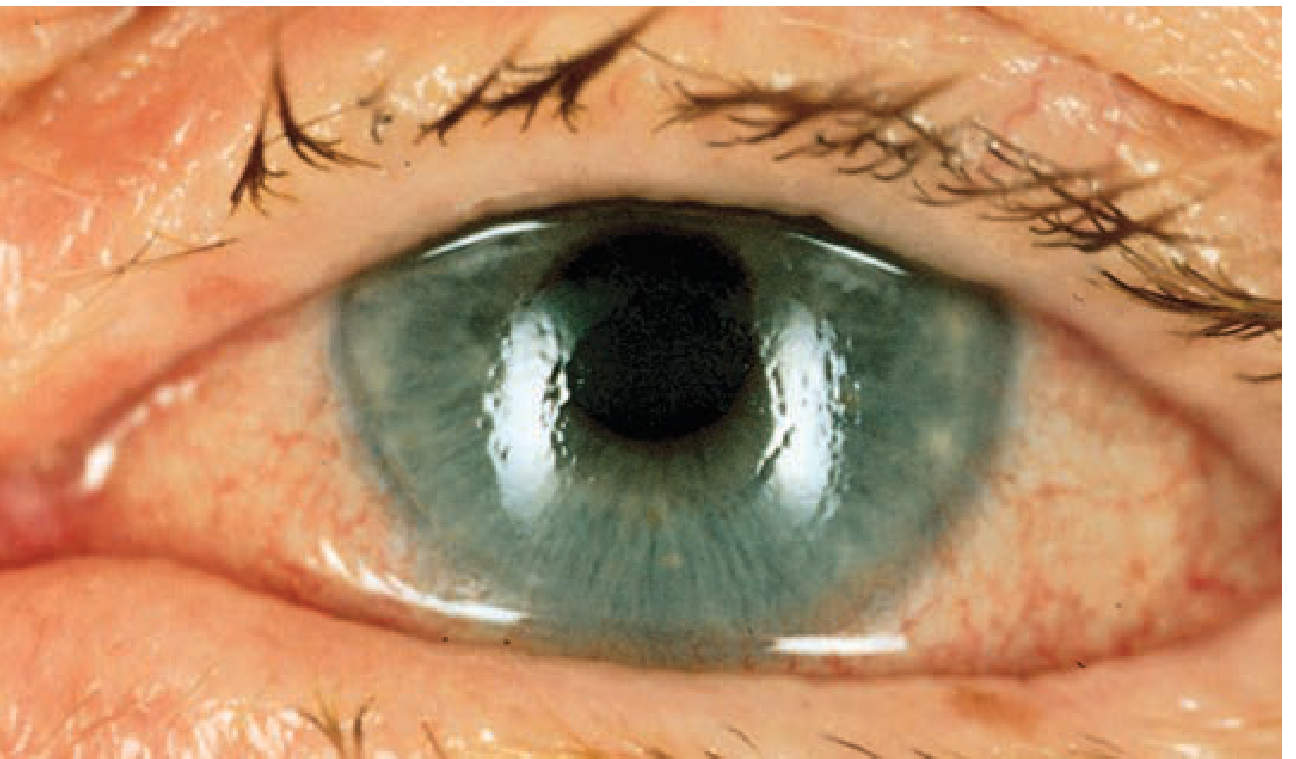
Acute angle closure: corneal cloudiness with circumcorneal injection — Tintinalli's Emergency Medicine
- Visual acuity typically 6/60 to hand movements
- IOP 50–80 mmHg (rock-hard globe)
- Hazy/steamy cornea (corneal epithelial oedema)
- Circumcorneal (ciliary) injection with violaceous hue
- Fixed, mid-dilated, vertically oval pupil — classic and pathognomonic
- Shallow anterior chamber with aqueous flare
- Fellow eye typically shows an occludable angle
After Resolution (Resolved APAC)
- Early: folds in Descemet's membrane, low IOP (ciliary body shutdown)
- Late: glaukomflecken (white foci of anterior lens necrosis), iris atrophy with spiral pattern, posterior synechiae, irregular pupil
Diagnosis
Gonioscopy is the definitive tool — it directly visualises the angle and grades closure. Key systems:
| Grade | Angle width | Structures visible |
|---|---|---|
| 4 (35–45°) | Wide open | Ciliary body visible |
| 3 (25–35°) | Open | Scleral spur visible |
| 2 (20°) | Narrow | Trabeculum visible, no scleral spur |
| 1 (10°) | Very narrow | Schwalbe line ± top of trabeculum |
| 0 | Closed | Iridocorneal contact |
Van Herick slit-lamp method screens angle width by comparing peripheral anterior chamber depth to corneal thickness — a ratio <1/4 warrants urgent gonioscopy.
Additional investigations: UBM (ultrasound biomicroscopy) to diagnose plateau iris; AS-OCT (anterior segment OCT) for angle imaging.
Differential Diagnosis of Acute IOP Elevation
- Acute APAC
- Lens-induced angle closure (swollen/subluxated lens)
- Malignant glaucoma (aqueous misdirection) — especially post-operatively
- Secondary angle closure (neovascular, inflammatory)
- Hypertensive uveitis / herpetic trabeculitis / Posner-Schlossman syndrome
- Scleritis with angle involvement
Treatment
Immediate (Acute Attack)
Position: Lay patient supine — gravity shifts the lens posteriorly, reducing pupillary block.
Medical IOP reduction (combine multiple agents):
| Agent Class | Drug & Dose |
|---|---|
| Carbonic anhydrase inhibitor | Acetazolamide 500 mg IV or PO, then 250 mg q4h (max 1 g/day); or topical dorzolamide/brinzolamide |
| Topical β-blocker | Timolol 0.5% — 1 drop to affected eye |
| Topical α₂-agonist | Apraclonidine 1% or brimonidine 0.2% — 1 drop |
| Hyperosmotic agent (if no IOP response at 1 hour) | IV mannitol 1.5–2 g/kg over 30 min; or oral glycerine |
⚠️ Pilocarpine is no longer recommended acutely — at very high IOP, the ischaemic iris sphincter is unresponsive; cholinergic agents can paradoxically shallow the anterior chamber and worsen closure. — Tintinalli's, 10e
Analgesia/antiemetics: Fentanyl is preferred (lowers IOP); ondansetron is safe (no IOP effect). Vomiting increases IOP and should be controlled.
Definitive Treatment
Peripheral laser iridotomy (PI) — creates a full-thickness hole in the peripheral iris to equalize anterior and posterior chamber pressures, bypassing the pupillary block. Performed once the cornea is clear and IOP is controlled.
- Bilateral PI is standard (the fellow eye has an occludable angle)
- Does not help plateau iris — laser peripheral iridoplasty or lens extraction needed in those cases
Clear lens extraction / phacoemulsification with IOL — the EAGLE trial demonstrated that early lens extraction is more effective and cost-effective than laser PI for PAC and PACG with elevated IOP. Achieves IOP control in ~80% preoperatively elevated eyes and corrects hypermetropia.
Trabeculectomy (with mitomycin C) — reserved for persistent IOP elevation despite an open angle, though carries a risk of malignant glaucoma.
Prophylaxis for PACS
The ZAP trial showed laser PI has only a small protective benefit over 6 years; selective prophylactic PI is appropriate for higher-risk patients (symptoms of intermittent closure, need for frequent dilation, atropine-like medications, limited access to eye care).
Summary Flowchart
Acute red eye + severe pain + fixed mid-dilated pupil + cloudy cornea
↓
Measure IOP (≥40–50 mmHg) → APAC
↓
Supine position + Acetazolamide + Timolol + Apraclonidine
↓
If IOP not ↓ in 1 hr → IV Mannitol
↓
Urgent ophthalmology consult → Peripheral laser iridotomy
↓
Prophylactic PI to fellow eye
Key references: Kanski's Clinical Ophthalmology: A Systematic Approach, 10e | Tintinalli's Emergency Medicine, 10e | Goldman-Cecil Medicine, 26e
This is a shared conversation. Sign in to Orris to start your own chat.