What is drowsy
Reading File
Finding Sources
Reading File
Drowsiness is a state of reduced wakefulness in which a person cannot sustain alertness without external stimulation. Here is a concise clinical description:
Drowsiness
Definition:
Drowsiness denotes an inability to sustain a wakeful state without the application of external stimuli. Mental, speech, and physical activity are reduced. It is indistinguishable from light sleep, and the person can be roused by speaking to them or applying a tactile stimulus. Unlike deeper impairment (stupor), a drowsy person can sustain alertness for at least a brief period without further external stimuli.
Key features:
- Drooping eyelids
- Slack jaw and limb muscles
- Slowed or reduced speech and movement
- Mild inattentiveness and mild confusion (both improve with arousal)
- Snoring may be present
- The person still shifts body position somewhat naturally
How it differs from stupor:
Stupor is a deeper state — the patient can only be roused by vigorous and repeated stimuli, and quickly drifts back into a deep sleep-like state when left unstimulated. In drowsiness, brief wakefulness is still possible without continuous stimulation.
Practical distinction (Fisher's method):
A verbal command is sufficient to overcome drowsiness, whereas a noxious (painful) stimulus is required to arouse someone from stupor.
In everyday terms, drowsiness is simply feeling very sleepy or having difficulty staying awake. Clinically, it is an important sign that can indicate many conditions — from medication side effects, to sleep disorders (like obstructive sleep apnea), to serious neurological or metabolic disturbances.
— Adams and Victor's Principles of Neurology, 12th Edition
What is dropsee
Finding Sources
Reading File
Reading File
Dropsy (you may also see it spelled "dropsie") is an old medical term — it is not used in modern medicine anymore. Here is what it means:
Dropsy
What it is:
Dropsy is a historical term for severe, abnormal accumulation of fluid in the body's tissues, causing extreme swelling (edema). It was widely used in the 19th century to describe a condition where fluid built up progressively, causing great suffering and, in serious cases, death.
What caused it:
Dropsy was not a single disease — it was a symptom of many different underlying conditions, including:
- Heart failure (fluid backs up into tissues)
- Kidney disease (e.g., nephrotic syndrome, chronic kidney disease)
- Liver disease (e.g., cirrhosis)
- Pulmonary (lung) disease
- Metabolic disorders
Because all these conditions could produce the same visible swelling, 19th-century physicians grouped them under one name — "dropsy" — without fully understanding the underlying mechanisms.
Modern understanding:
Today, the condition is called edema (or oedema) — the expansion of fluid in the interstitial (between-cell) spaces of the body. Once scientists identified the role of salt (sodium) retention in fluid accumulation, targeted treatments became possible, particularly diuretics (medicines that increase urine output to remove excess fluid). The first modern diuretic, chlorothiazide, became available in 1958.
In short:
Dropsy = old name for what we now call edema (fluid swelling), most commonly caused by heart, kidney, or liver failure.
— National Kidney Foundation Primer on Kidney Diseases, 8e | Kaplan & Sadock's Comprehensive Textbook of Psychiatry
What is exudate
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Loading Image
Exudate
An exudate is an extravascular fluid that leaks out of blood vessels into surrounding tissues or body cavities. It is characterized by:
- High protein concentration
- May contain cellular debris, white blood cells (leukocytes), and sometimes red blood cells
- Formed due to increased vascular permeability — a hallmark of inflammation
How it forms
During acute inflammation, the body releases chemical mediators (histamine, bradykinin, leukotrienes). These cause the endothelial cells lining blood vessels to contract, opening up gaps between them. This allows proteins and cells — which normally stay inside vessels — to escape into the tissues. This process is called exudation.
Exudate vs. Transudate
| Feature | Exudate | Transudate |
|---|---|---|
| Protein content | High | Low (mostly albumin) |
| Cells | White cells, debris present | Few or none |
| Cause | Inflammation (increased vascular permeability) | Mechanical pressure imbalance (e.g., heart failure, liver disease, kidney disease) |
| Associated with | Infection, injury, cancer | Heart failure, cirrhosis, nephrotic syndrome |
Special type — Pus
Pus is a purulent exudate — an exudate that is especially rich in neutrophils (white blood cells), dead cell debris, and often microbes. It forms during bacterial infections.
In everyday terms: if you have an infected wound and it produces thick, cloudy, or yellowish fluid — that is an exudate. Clear watery swelling from heart or kidney problems is more likely a transudate.
— Robbins & Kumar Basic Pathology | Robbins, Cotran & Kumar Pathologic Basis of Disease
What is Transudate
Based on the textbook content already retrieved in our previous conversation, I can answer this directly.
Transudate
A transudate is an extravascular fluid that leaks out of blood vessels due to a mechanical pressure imbalance — not inflammation. It is characterized by:
- Low protein content (mostly albumin)
- Little or no cellular material
- Low specific gravity
- Formed without any increase in vascular permeability (the vessel wall itself is intact)
How it forms
A transudate is essentially an ultrafiltrate of blood plasma. It occurs when the normal balance of forces across the vessel wall is disrupted:
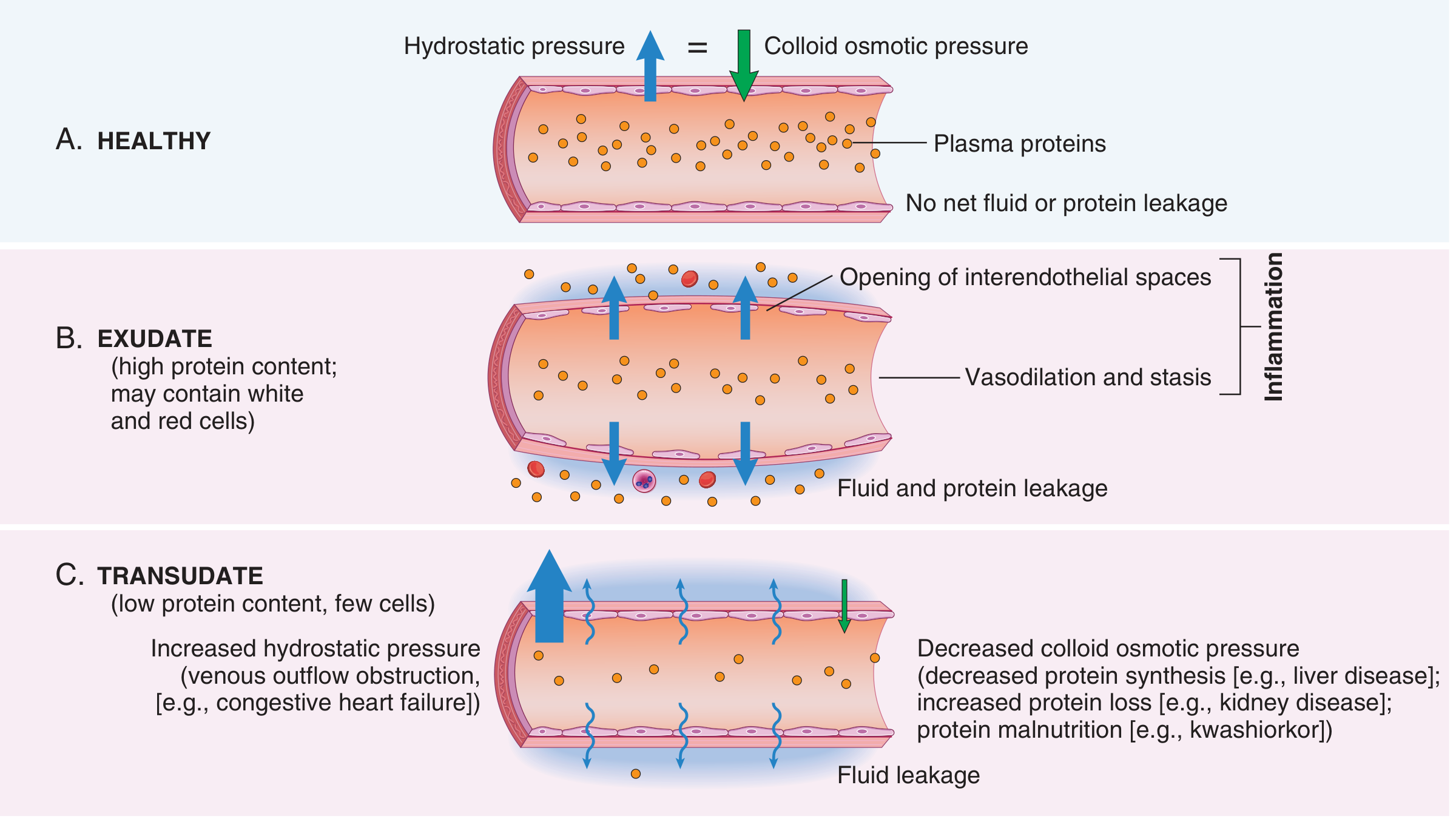
- Increased hydrostatic pressure — pushes fluid out of vessels (e.g., in heart failure, venous obstruction)
- Decreased colloid osmotic pressure — less protein in the blood means less force pulling fluid back in (e.g., liver disease → less protein made; kidney disease → protein lost in urine; protein malnutrition like kwashiorkor)
Transudate vs. Exudate
| Feature | Transudate | Exudate |
|---|---|---|
| Protein content | Low | High |
| Cells | Few or none | White cells, debris present |
| Vascular permeability | Normal | Increased |
| Cause | Pressure imbalance | Inflammation |
| Common causes | Heart failure, cirrhosis, nephrotic syndrome, malnutrition | Infection, injury, cancer |
Common clinical examples
- Congestive heart failure → fluid backs up, hydrostatic pressure rises → transudative pleural effusion or leg edema
- Liver cirrhosis → less albumin made → osmotic pressure drops → ascites (fluid in abdomen)
- Nephrotic syndrome → protein lost in urine → osmotic pressure drops → generalized edema

In simple terms: transudate is watery, protein-poor fluid caused by plumbing pressure problems, while exudate is protein-rich fluid caused by the body's inflammatory response.
— Robbins & Kumar Basic Pathology | Robbins, Cotran & Kumar Pathologic Basis of Disease
This is a shared conversation. Sign in to Orris to start your own chat.