Cardiac arrest
Reading File
search_medical_text
cardiac arrest etiology pathophysiology rhythms ACLS management
search_medical_text
post-cardiac arrest care return of spontaneous circulation targeted temperature management prognosis
search_medical_image
cardiac arrest ACLS algorithm shockable non-shockable rhythms
GradeResponse
GradeResponse
GradeResponse
Cardiac Arrest
Definition
Cardiac arrest is the sudden cessation of effective cardiac mechanical activity resulting in loss of circulation, unconsciousness, and apnea (or agonal breathing). It is distinct from myocardial infarction (a plumbing problem) — cardiac arrest is an electrical problem that causes immediate hemodynamic collapse.
Epidemiology
- Out-of-hospital cardiac arrest (OHCA) affects ~350,000–400,000 people annually in the US
- In-hospital cardiac arrest (IHCA) affects ~200,000/year
- Survival to hospital discharge for OHCA remains ~10–12%; IHCA ~25%
- Witnessed arrests with shockable rhythms have the best prognosis
Etiology — The H's and T's
The reversible causes of cardiac arrest are taught via this mnemonic:
| H's | T's |
|---|---|
| Hypoxia | Tension pneumothorax |
| Hypovolemia | Tamponade (cardiac) |
| Hydrogen ion (acidosis) | Toxins/drug overdose |
| Hypo/Hyperkalemia | Thrombosis — pulmonary (PE) |
| Hypothermia | Thrombosis — coronary (MI) |
Most common underlying cause in adults: coronary artery disease / acute MI
Cardiac Rhythms in Arrest
There are four arrest rhythms. The first two are shockable; the last two are non-shockable.
| Rhythm | Shockable? | Key Features |
|---|---|---|
| Ventricular Fibrillation (VF) | ✅ Yes | Chaotic, disorganized, no identifiable QRS |
| Pulseless Ventricular Tachycardia (pVT) | ✅ Yes | Wide QRS tachycardia, no pulse |
| Pulseless Electrical Activity (PEA) | ❌ No | Organized QRS complexes, no pulse — look for H's & T's |
| Asystole | ❌ No | Flat (isoelectric) line — confirm in 2 leads |
The image below illustrates how these rhythms appear on ECG during and after CPR:
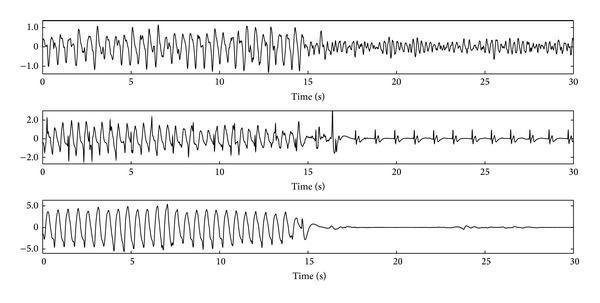
BLS — Basic Life Support (First Response)
- Call for help — activate EMS, get AED
- High-quality CPR immediately:
- Rate: 100–120 compressions/min
- Depth: ≥2 inches (5 cm), allow full recoil
- Minimize interruptions (keep pauses <10 seconds)
- Switch compressors every 2 minutes to reduce fatigue
- Defibrillate early — for every minute without defibrillation in VF, survival drops ~10%
- Ventilation: 30:2 ratio until advanced airway placed, then 1 breath every 6 seconds (10/min) asynchronously
ACLS — Advanced Cardiac Life Support
Shockable Rhythms (VF/pVT)
- Defibrillate immediately (biphasic: 120–200 J; monophasic: 360 J)
- Resume CPR for 2 minutes immediately after shock
- Establish IV/IO access, give epinephrine 1 mg IV/IO every 3–5 minutes
- After 2nd shock: consider amiodarone 300 mg IV (repeat 150 mg once) or lidocaine 1–1.5 mg/kg
- Reassess rhythm every 2 minutes
Non-Shockable Rhythms (PEA/Asystole)
- CPR immediately — no shock indicated
- Epinephrine 1 mg IV/IO every 3–5 minutes (give as soon as possible)
- Identify and treat reversible H's and T's
- Reassess rhythm every 2 minutes
Advanced Airway
- Endotracheal intubation or supraglottic airway (LMA/King)
- Confirm with waveform capnography (ETCO₂ goal ≥10 mmHg; ETCO₂ surge may signal ROSC)
Post-Cardiac Arrest Care (Post-ROSC)
Once return of spontaneous circulation (ROSC) is achieved, management focuses on preventing secondary injury:
1. Temperature Control
Per the Canadian Cardiovascular Society (CCS) and landmark RCTs, active temperature regulation should be considered for unconscious post-ROSC patients (Optimal Post Cardiac Arrest and Refractory Cardiac Arrest Patient Care, p. 5):
- Target temperature: 33°C–36°C for at least 24 hours
- The TTM2 trial defined "unconscious" as inability to obey verbal commands
- Avoid fever (>37.7°C) in all post-arrest patients — it worsens neurological outcomes
2. Hemodynamic Optimization
- MAP goal: ≥65–70 mmHg (some guidelines suggest ≥80 mmHg in comatose patients)
- Avoid hypotension — treat with fluids and vasopressors (norepinephrine preferred)
- Avoid hyperoxia: target SpO₂ 94–98%, PaO₂ 75–100 mmHg
- Avoid hypocapnia: target PaCO₂ 35–45 mmHg
3. Coronary Angiography
- Emergent PCI for ST-elevation on post-ROSC ECG
- For non-STEMI presentations: selective/deferred angiography is reasonable — evidence does not support routine emergent cath in the absence of ST elevation
4. Neuroprognostication
- Delay formal prognosis until ≥72 hours after arrest (and after rewarming if temperature management used)
- Multimodal approach: clinical exam (pupillary reflexes, motor response), EEG, SSEP, CT/MRI brain, serum biomarkers (NSE, GFAP)
5. Refractory Cardiac Arrest / eCPR
In selected patients with refractory cardiac arrest (no ROSC after ≥5 min of ACLS), extracorporeal CPR (ECMO-CPR) may be considered. However, the HYPERION trial found no statistically significant improvement in survival with good neurological outcome at 180 days with early invasive/eCPR strategy vs. standard ACLS (31.5% vs. 22.0%, P=0.09) — the trial was terminated early for futility (Optimal Post Cardiac Arrest and Refractory Cardiac Arrest Patient Care, p. 12).
Prognosis
| Factor | Impact |
|---|---|
| Witnessed arrest | Better |
| Bystander CPR | Better |
| Shockable rhythm (VF/pVT) | Better |
| Short time to defibrillation | Better |
| ETCO₂ <10 mmHg at 20 min | Poor |
| Asystole as initial rhythm | Worst |
| Prolonged downtime | Worse |
Overall, good neurological survival (CPC 1–2) occurs in roughly 8–10% of all OHCA and ~20–25% of IHCA.
Key teaching point: The single most impactful interventions are early high-quality CPR and early defibrillation for shockable rhythms — every other intervention is secondary to these two.
This is a shared conversation. Sign in to Orris to start your own chat.