Show me the complete screening algorithm and management plan for rhesus negative mothers from booking visit
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Reading File
Reading File
I now have comprehensive content from multiple authoritative sources. Let me compile the complete screening algorithm and management plan.
Rh-Negative Mothers: Complete Screening Algorithm & Management Plan
Background: Why This Matters
The D antigen of the Rh blood group system is the primary cause of Rh incompatibility. An Rh-negative mother carrying an Rh-positive fetus can have fetal red cells cross the placenta into her circulation, triggering maternal IgG anti-D antibody formation. In subsequent pregnancies, these antibodies cross the placenta and destroy fetal red cells, causing hemolytic disease of the fetus and newborn (HDFN) — manifesting as erythroblastosis fetalis, hydrops fetalis, jaundice, and kernicterus.
First pregnancies are usually safe because the primary immune response generates IgM (which cannot cross the placenta). The danger escalates with subsequent pregnancies: ~3% of 2nd babies are affected, ~10% of 3rd babies, and rising thereafter. — Guyton and Hall Textbook of Medical Physiology
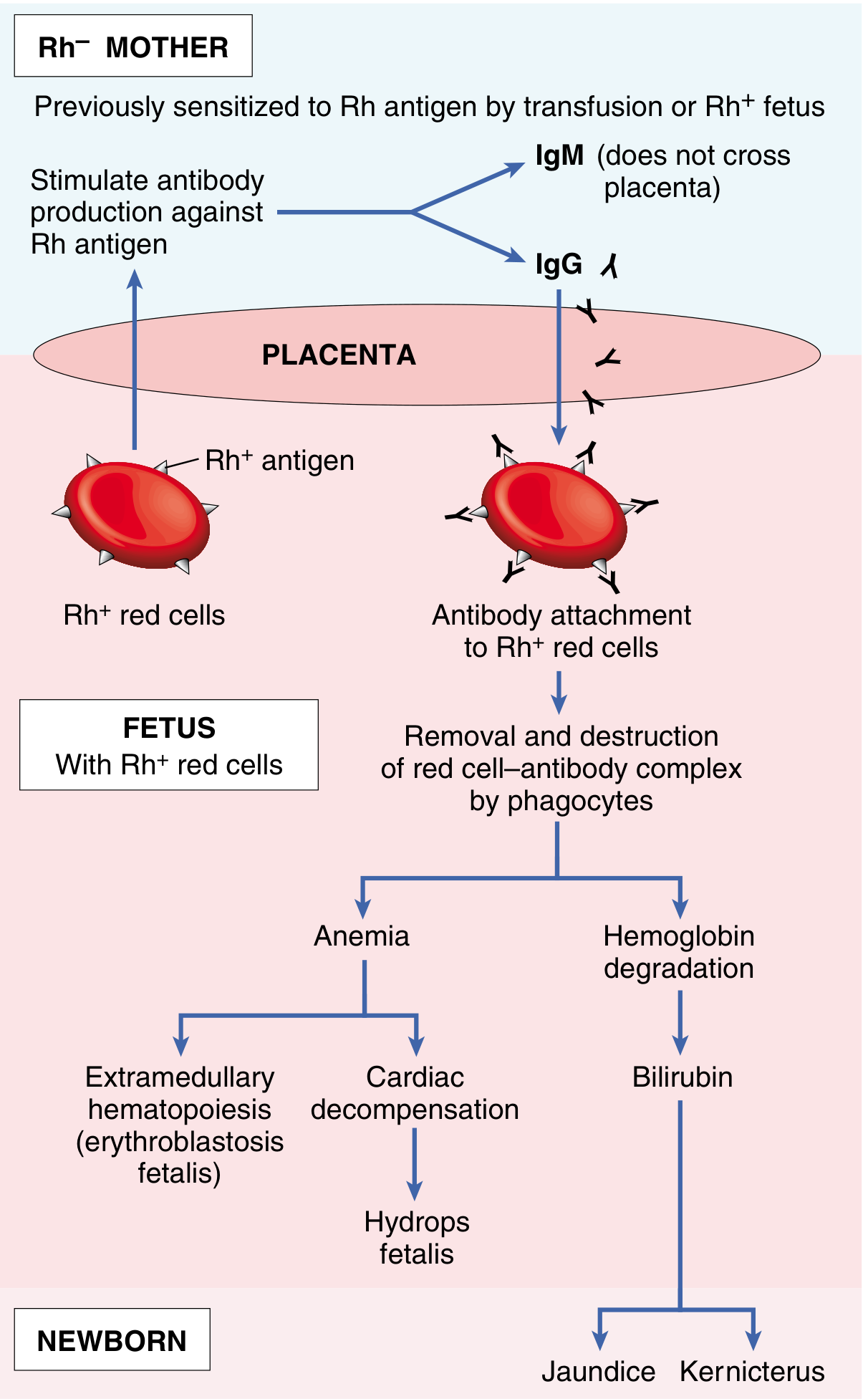
Screening Algorithm from Booking Visit
STEP 1 — Booking Visit (First Antenatal Visit, ~8–12 weeks)
| Action | Detail |
|---|---|
| Blood group & Rh typing | ABO and RhD status must be determined for ALL pregnant women |
| Indirect Coombs Test (ICT) / Antibody Screen | Test for pre-existing anti-D (or other) antibodies in maternal serum |
| Partner blood grouping | Determine if father is Rh-positive (if Rh-negative father → fetus must be Rh-negative → no risk) |
Interpret the antibody screen:
- Antibody screen NEGATIVE + Rh-negative → Unsensitized → proceed with prophylaxis protocol below
- Antibody screen POSITIVE (anti-D detected) → Already sensitized → escalate to alloimmunized pregnancy management
STEP 2 — Antenatal Monitoring (Unsensitized Rh-Negative)
| Timing | Action |
|---|---|
| ~20 weeks | Repeat ICT/antibody screen |
| 28 weeks | Repeat ICT — if still negative, administer routine antenatal anti-D prophylaxis |
| 34–36 weeks | Repeat antibody screen before second dose (where two-dose regimen used) |
STEP 3 — Routine Antenatal Anti-D Prophylaxis (RAADP)
Who: All unsensitized (antibody screen negative) Rh-D-negative pregnant women
Dose & Timing:
- Standard regimen: Anti-D immunoglobulin 300 mcg IM at 28 weeks (single-dose protocol — ACOG-endorsed)
- Alternative two-dose: 100–125 mcg at 28 weeks AND 34 weeks
The anti-D antibody is given antepartum at 28–30 weeks of gestation. The mechanism involves clearing Rh-positive fetal cells from maternal circulation before B-lymphocyte sensitization can occur — thereby preventing formation of memory B cells that would activate in future pregnancies. — Guyton and Hall Textbook of Medical Physiology
Rh(D) immune globulin (300 mcg IM) is a concentrated solution of human IgG with high-titer anti-Rh(D) antibodies. For this prophylaxis to succeed, the mother must be Rh-D-negative and not already immunized. — Katzung's Basic and Clinical Pharmacology, 16th Edition
STEP 4 — Sensitizing Events Requiring Additional Anti-D Doses
Anti-D must be given within 72 hours of any potential fetomaternal hemorrhage (FMH), regardless of gestational age:
| Sensitizing Event | Anti-D Dose |
|---|---|
| Miscarriage / threatened miscarriage | 50 mcg if <12 weeks; 300 mcg if ≥12 weeks |
| Ectopic pregnancy | 50 mcg (<12 weeks); 300 mcg acceptable |
| Chorionic villus sampling (CVS) | 300 mcg |
| Amniocentesis | 300 mcg |
| External cephalic version (ECV) | 300 mcg |
| Antepartum hemorrhage (APH) | 300 mcg; repeat if continued bleeding |
| Abdominal trauma | 300 mcg — "If as little as 0.1 μL of Rh-positive fetal blood enters an Rh-negative mother's circulation, the mother can develop Rh antibodies" — Tintinalli's Emergency Medicine |
| Intrauterine procedures | 300 mcg |
| Delivery of Rh-positive baby | 300 mcg within 72 hours of delivery |
ACOG and ACEP both recommend 50 mcg for procedures/events before 12 weeks (due to small fetoplacental blood volume ~4.2 mL at 12 weeks); 300 mcg for events at ≥12 weeks. — Tintinalli's Emergency Medicine
Kleihauer-Betke (KB) test / Flow cytometry: Performed when large FMH is suspected (e.g., trauma, significant APH, abruption after 12 weeks). Quantifies fetal cells in maternal blood — additional anti-D vials are given if FMH exceeds the coverage of 300 mcg (~30 mL fetal whole blood).
STEP 5 — Postnatal Management
| Neonatal result | Action |
|---|---|
| Baby Rh-positive, mother still unsensitized | Give anti-D 300 mcg IM within 72 hours of delivery |
| Baby Rh-negative | No anti-D required |
| Large FMH on KB test | Additional anti-D doses proportional to estimated hemorrhage |
Management of the Sensitized (Alloimmunized) Rh-Negative Mother
When anti-D antibodies are already present at booking or develop during pregnancy, prophylaxis is futile and management shifts to fetal surveillance:
Monitoring Protocol for Alloimmunized Pregnancy
| Anti-D Titer | Management |
|---|---|
| Low titre (<1:4–1:8) | Serial antibody titres every 4 weeks; fetal surveillance with growth scans |
| Rising titre (≥1:16 or critical titre) | Doppler assessment of fetal middle cerebral artery peak systolic velocity (MCA-PSV) every 1–2 weeks |
| MCA-PSV >1.5 MoM | Strongly predictive of fetal anemia → proceed to fetal blood sampling (FBS) |
Fetal Blood Sampling (FBS) & Intrauterine Transfusion (IUT)
- FBS via cordocentesis (umbilical vein) confirms fetal hemoglobin
- If fetal Hb <2 SD below mean for gestational age → Intrauterine intravascular transfusion (IVT) with O-negative, CMV-negative, irradiated, leukodepleted blood
- May be repeated every 2–4 weeks until fetus is mature enough for delivery
Delivery Timing
- Unaffected or mildly affected fetuses: Deliver at 37–38 weeks
- Severely affected or post-IUT: Deliver at 34–37 weeks depending on fetal condition
- Post-delivery: neonatal exchange transfusion and/or phototherapy for jaundice/hyperbilirubinemia; monitor for kernicterus
Antenatal identification and management of the at-risk fetus have been greatly facilitated by amniocentesis and chorionic villus and fetal blood sampling. Severe intrauterine hemolysis may be treated by fetal intravascular transfusions via the umbilical cord and early delivery. — Robbins, Cotran & Kumar Pathologic Basis of Disease
Complete Algorithm Summary
BOOKING VISIT
│
▼
Blood group + Rh typing + ICT (antibody screen)
│
├─── Rh POSITIVE ──────────────────► Standard antenatal care
│
└─── Rh NEGATIVE
│
├─── ICT POSITIVE (anti-D present)
│ │
│ └─► ALLOIMMUNIZED pathway:
│ • Serial titres q4 weeks
│ • MCA-PSV Doppler if titre ≥ critical level
│ • FBS + IUT if MCA-PSV >1.5 MoM
│ • Planned delivery 34–38 wks
│
└─── ICT NEGATIVE (unsensitized)
│
▼
Check partner Rh type
│
├─ Partner Rh-NEGATIVE → Fetus must be Rh-negative
│ → No anti-D needed; routine care
│
└─ Partner Rh-POSITIVE or unknown
│
▼
PROPHYLAXIS PROTOCOL:
• Repeat ICT at 20 wks
• Anti-D 300 mcg IM at 28 wks (± 34 wks)
• Anti-D at ANY sensitizing event within 72 hrs
• Post-delivery: check baby's Rh type
│
├─ Baby Rh-POSITIVE → Anti-D 300 mcg within 72 hrs
│ ± KB test if large FMH suspected
└─ Baby Rh-NEGATIVE → No anti-D needed
Key Points to Remember
| Point | Detail |
|---|---|
| Window for anti-D | Must be given within 72 hours of sensitizing event (ideally within 24 hrs) |
| First pregnancy risk | Usually safe — initial IgM response doesn't cross placenta; danger is in subsequent pregnancies |
| ABO protection | Concurrent ABO incompatibility partially protects the mother (fetal cells cleared by anti-A/B IgM before sensitization occurs) |
| Rh-negative = homozygous deletion | Rh-negative individuals lack the RHD gene entirely — so no "d" antibody exists |
| Weak D / partial D | Some women type as Rh-positive but have partial D antigens — may still be at risk; management is institution-specific |
| Non-D antigens | Anti-Kell (K), anti-c, anti-E can also cause HDFN — detected by ICT; managed similarly to anti-D alloimmunization |
Sources:
- Robbins, Cotran & Kumar Pathologic Basis of Disease — Immune Hydrops / Etiology & Pathogenesis
- Guyton and Hall Textbook of Medical Physiology — Erythroblastosis Fetalis & Prevention
- Katzung's Basic and Clinical Pharmacology, 16th Edition — Rh(D) Immune Globulin
- Tintinalli's Emergency Medicine — Rh Seroconversion & Anti-D Indications
- Emery's Elements of Medical Genetics and Genomics — Rhesus Hemolytic Disease of the Newborn
This is a shared conversation. Sign in to Orris to start your own chat.