Explain upper limb orthosis in detail
Reading File
Finding Sources
Finding Sources
Searching the Web
upper limb orthosis classification types indications clinical
Finding Sources
Finding Sources
Reading Web Page
upper limb orthosis types classification indications biomechanics
Reading File
Finding Sources
Finding Sources
Reading File
Reading Web Page
upper limb orthosis types wrist hand shoulder elbow classification indications materials
Searching Images
upper limb orthosis wrist hand elbow shoulder splint
I now have comprehensive material to compile a detailed answer. Let me synthesize everything.
Upper Limb Orthosis — Detailed Overview
1. Definition
An orthosis (plural: orthoses) is an externally applied device designed to modify the structural and functional characteristics of the neuromuscular and skeletal systems. Upper limb orthoses (ULO) encompass devices applied from the shoulder down to the fingertips to support, protect, correct, or assist the upper extremity.
2. Objectives / Principles
The goals of upper limb orthotic application fall into three main categories:
| Objective | Mechanism |
|---|---|
| Protection | Provides compressive forces and traction; restricts/prevents joint motion; stabilizes unstable bony components; promotes healing of soft tissue and bone |
| Correction | Corrects joint contractures and subluxation of joints or tendons; prevents and reduces deformity |
| Assistance with function | Compensates for deformity, muscle weakness, or increased muscle tone to restore functional activity |
3. Classification Systems
A. By Functional Design (ASHT Splint Classification System, 1991)
The American Society of Hand Therapists (ASHT) standardized nomenclature based on:
- Articular vs. Non-articular (does it cross a joint?)
- Location of the body part covered
- Direction of force applied
- Purpose: Mobilization, Immobilization, or Restriction
B. By Design Category
| Design | Description | Example |
|---|---|---|
| Non-articular | Does not cross a joint | Humeral fracture brace |
| Static | No moving parts; maintains joint in one position | Resting hand splint, cock-up splint |
| Serial static | Repeatedly re-molded or re-adjusted to achieve progressive ROM gains | Serial casting for contracture |
| Static-progressive | Has a mechanism for incremental adjustment but no dynamic force | Turnbuckle elbow orthosis |
| Dynamic | Has spring-loaded or elastic components that apply continuous passive force | Kleinert pulley splint, dynamic extension assist |
C. By Purpose
- Immobilization – Prevents movement for healing or pain relief
- Mobilization – Applies gentle, prolonged force to increase ROM
- Restriction – Limits motion in one direction while allowing it in another
4. Biomechanical & Anatomic Considerations
Effective orthosis design requires:
- Three-point pressure system: The fundamental biomechanical principle — two forces in one direction oppose a third force in the opposite direction
- Lever arm length: Longer lever arms distribute forces more broadly; short lever arms concentrate stress
- Tissue creep: Low-load prolonged stretch (LLPS) exploits viscoelastic tissue properties to gain ROM
- Intrinsic-plus ("safe") position: For hand orthoses — wrist in slight extension, MCPs flexed 70–90°, IPs in full extension, thumb abducted and opposed — prevents shortening of collateral ligaments and intrinsic muscles
Hand prehension patterns that orthoses aim to preserve:
- Power grip (cylindrical, spherical, hook)
- Precision grip — lateral key pinch, oppositional pinch (three-jaw chuck), precision pinch
5. Types of Upper Limb Orthoses by Region
A. Shoulder Orthoses
| Type | Indication |
|---|---|
| Arm sling (simple) | Fractures, post-surgical support |
| Hemicuff / Bobath sling | Shoulder subluxation + pain in upper limb paralytic disorders (hemiplegia, stroke) |
| Gunslinger orthosis | Brachial plexus injuries; positions arm in abduction and external rotation |
| Balanced forearm orthosis (BFO) / Mobile arm support | Proximal muscle weakness (e.g., C3–C5 SCI, muscular dystrophy); supports the arm against gravity via a ball-bearing system so residual wrist/hand function can be used |
B. Elbow Orthoses
| Type | Indication |
|---|---|
| Hinged elbow orthosis | Ligament instability; post-surgical ROM control |
| Dynamic spring-loaded orthosis | Flexion and extension contractures |
| Static progressive elbow orthosis | Post-traumatic or post-surgical stiffness |
| Long arm splint (elbow at 45°) | Cubital tunnel syndrome |
| Lateral epicondylitis strap (tennis elbow brace) | Placed ~2 fingerbreadths distal to lateral epicondyle; offloads extensor origin by changing the lever arm |
| Medial epicondylitis brace (golfer's elbow) | Similar principle to tennis elbow strap |
C. Wrist Orthoses
| Type | Indication |
|---|---|
| Cock-up splint (wrist extension splint) | Wrist drop (radial nerve palsy), carpal tunnel syndrome, de Quervain's tenosynovitis |
| Wrist immobilization orthosis | Carpal tunnel syndrome, wrist sprains, TFCC injuries, post-surgical |
| Wrist-hand orthosis (WHO) | Post-injury care, spastic conditions |
| Wrist-driven flexor-hinge orthosis | Lower cervical quadriplegia (C6–C7); tenodesis action — wrist extension powers finger pinch |
D. Hand & Finger Orthoses
| Type | Indication |
|---|---|
| Resting hand splint | Rheumatoid arthritis, spastic hand, post-trauma immobilization |
| Opponens splint | Median nerve palsy; pre-positions thumb for opposition; note: impairs tactile sensation |
| Ulnar deviation splint | Rheumatoid arthritis with ulnar drift |
| Thumb spica splint (forearm-based) | De Quervain's tenosynovitis, CMC joint arthritis, scaphoid fractures |
| Mallet finger splint | Distal phalanx extensor tendon avulsion; holds DIP in extension |
| Boutonnière splint | PIP flexion deformity with DIP hyperextension |
| Swan-neck splint | PIP hyperextension deformity in RA |
| Dynamic finger extension splint | Extensor tendon repairs; Kleinert splint for flexor tendon repair (rubber-band traction) |
| Buddy splinting | Finger fractures, PIP sprains |
E. Combined / Complex Orthoses
| Type | Indication |
|---|---|
| SEWHO (Shoulder-Elbow-Wrist-Hand Orthosis) | Brachial plexus palsy, extensive paralysis |
| EWHO (Elbow-Wrist-Hand Orthosis) | Combined elbow + hand pathology |
| WHO (Wrist-Hand Orthosis) | Hand paralysis, spasticity |
| Wrist-driven hand orthosis | Cervical quadriplegia; body-powered prehension device |
6. ISO Nomenclature
The International Standards Organisation (ISO) names upper limb orthoses by the joints they encompass:
| Abbreviation | Coverage |
|---|---|
| SO | Shoulder orthosis |
| EO | Elbow orthosis |
| WHO | Wrist-hand orthosis |
| WHFO | Wrist-hand-finger orthosis |
| HO | Hand orthosis |
| FO | Finger orthosis |
| SEWHFO | Shoulder-elbow-wrist-hand-finger orthosis |
7. Materials
| Material | Properties | Use |
|---|---|---|
| Thermoplastics (low-temp) | Mouldable at 60–70°C, lightweight, easily re-molded | Custom hand/wrist splints (most common) |
| Thermoplastics (high-temp) | Stronger, more durable | Long-term use orthoses |
| Carbon fibre | Very lightweight and stiff | Functional orthoses demanding strength |
| Neoprene / soft materials | Flexible, compressive, comfortable | Mild support, edema control |
| Metal (aluminum/steel uprights) | Maximum durability | Elbow, shoulder orthoses requiring rigid control |
| Plaster of Paris | Serial casting material | Contracture management |
8. Specific Conditions & Corresponding Orthoses
| Condition | Preferred Orthosis |
|---|---|
| Stroke / hemiplegia | Resting hand splint, hemicuff sling, BFO |
| Radial nerve palsy (wrist drop) | Cock-up wrist splint, dynamic wrist extension splint |
| Median nerve palsy | Opponens splint (low), long opponens (high) |
| Ulnar nerve palsy | Anti-claw splint (lumbrical bar) |
| Brachial plexus injury | Gunslinger, SEWHO |
| Cervical SCI (C5–C6) | Balanced forearm orthosis, wrist-driven hand orthosis |
| Rheumatoid arthritis | Resting hand splint, ulnar deviation splint, swan-neck ring |
| De Quervain's tenosynovitis | Forearm-based thumb spica splint |
| Lateral epicondylitis | Counterforce forearm band/strap |
| Carpal tunnel syndrome | Neutral wrist immobilization splint (night) |
| Flexor tendon repair (Kleinert) | Dynamic rubber-band traction splint |
| Post-radioulnar synostosis excision | Dynamic pronosupination orthosis |
9. Assessment Before Prescription
A thorough assessment should include:
- ROM (active and passive) of all upper limb joints
- Muscle strength and tone (spasticity vs. flaccidity)
- Sensation (orthoses over insensate skin risk pressure sores)
- Functional needs — ADLs, work, leisure
- Skin integrity and swelling
- Cognition and compliance
Outcome measures used to evaluate efficacy include grip/pinch dynamometry, DASH (Disabilities of the Arm, Shoulder and Hand) questionnaire, Michigan Hand Outcomes Questionnaire, and patient-reported pain scores.
10. Fabrication and Fitting Principles
- Bony prominences must be relieved (ulnar styloid, radial styloid, lateral epicondyle)
- Straps should be broad and distribute pressure evenly
- Avoid circumferential pressure that impairs circulation
- Orthosis should be removable for skin checks and hygiene (unless post-surgical protocol demands continuous wear)
- Wearing schedule prescribed explicitly: e.g., "night splinting only" vs. "continuous"
- Patient education on donning/doffing and skin surveillance is mandatory
11. Complications
| Complication | Prevention |
|---|---|
| Pressure sores | Padding over bony prominences, regular skin checks |
| Joint stiffness | Appropriate mobilization schedule, not over-immobilizing |
| Muscle atrophy | Exercise programme alongside orthosis use |
| Sensory impairment | Avoid tight circumferential fits |
| Non-compliance | Patient education, lightweight comfortable materials |
12. Team Involved
Upper limb orthosis provision is multidisciplinary:
- Orthotist — device design, fabrication, fitting
- Occupational therapist / Certified Hand Therapist (CHT) — functional assessment, splinting, ADL training
- Physical therapist — strengthening and ROM programme
- Physician/surgeon — diagnosis, prescription, surgical planning where indicated
Illustrative Images
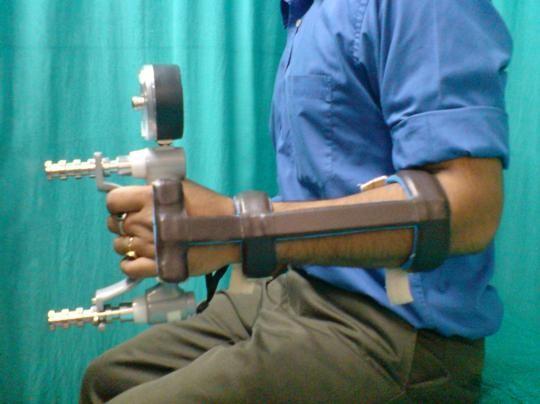
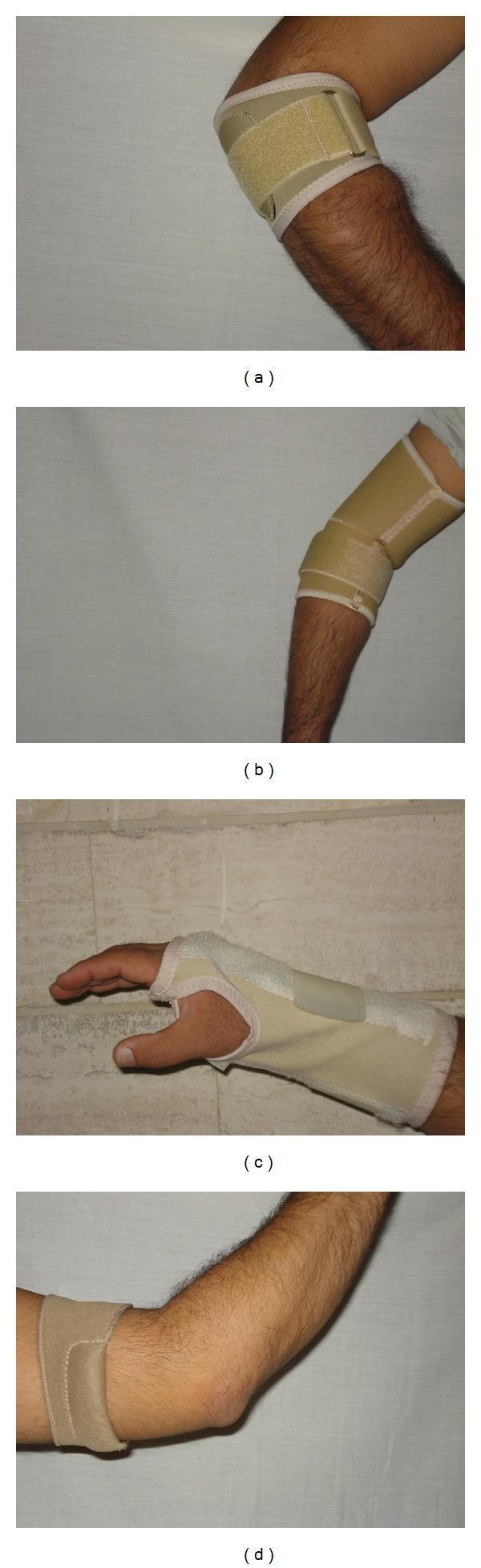
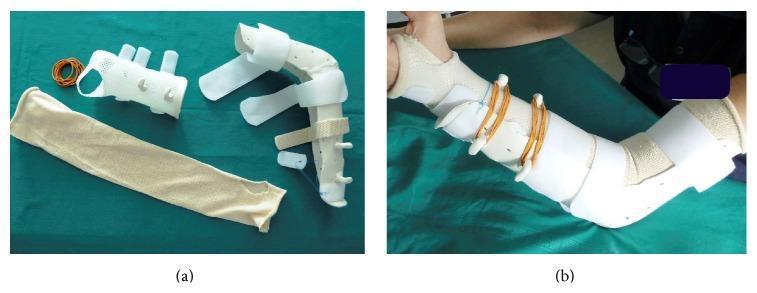
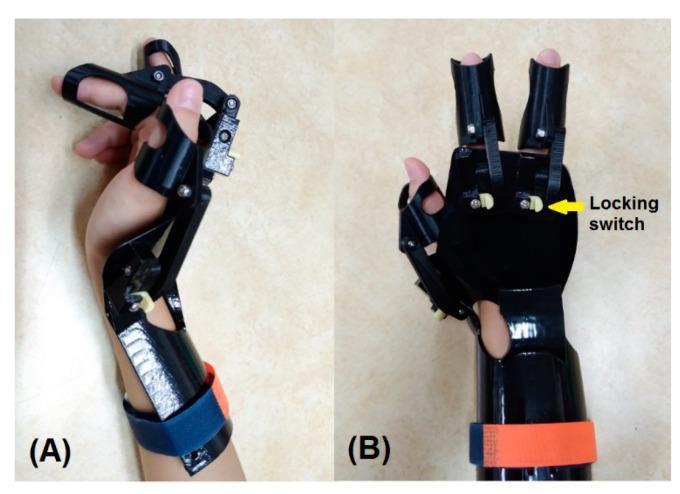
Sources:
- Miller's Review of Orthopaedics, 9th Edition — Elbow Orthosis, Wrist-Hand Orthosis, Fracture Braces sections
- Bradley and Daroff's Neurology in Clinical Practice — Balanced Forearm Orthosis, Hemicuff Sling
- Musculoskeletal Key — Upper Limb Orthotic Devices (Chapter 14)
- ASHT Splint Classification System (1991)
This is a shared conversation. Sign in to Orris to start your own chat.