perthes disease 20 mark exam written answer
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
I now have all the material needed. Here is a comprehensive 20-mark exam answer on Perthes disease.
Legg-Calvé-Perthes Disease (Perthes Disease)
Definition and Aetiology
Perthes disease (Legg-Calvé-Perthes disease, LCPD) is an idiopathic avascular necrosis (osteonecrosis) of the capital femoral epiphysis in children, resulting from interruption of blood supply to the femoral head. The aetiology is unknown, but a vascular insult leads to ischaemic necrosis of the proximal femoral epiphysis, followed by revascularisation, resorption, and eventual remodelling through a process of creeping substitution. There is a predominance of femoral head resorption over reformation, which risks permanent femoral head deformity.
— Miller's Review of Orthopaedics 9th Edition; ROSEN's Emergency Medicine
Epidemiology and Risk Factors
- Most common in boys aged 4–8 years (male:female ≈ 4–5:1)
- Peak incidence 5–8 years of age
- Bilateral in 10–15% of cases; when bilateral, involvement is typically asymmetrical and non-simultaneous
- Associated with: delayed skeletal maturation, positive family history, low birth weight, abnormal birth presentation, attention deficit hyperactivity disorder
- Female sex, older age at onset, and bilateral presentation carry a worse prognosis
— ROSEN's Emergency Medicine; Miller's Review of Orthopaedics 9th Edition
Clinical Features
Symptoms:
- Limp — the most common presenting complaint; often insidious onset
- Pain — typically in the hip, groin, or referred to the thigh or knee (referred knee pain is a classic trap for delayed diagnosis)
- Pain is worse with activity and relieved by rest
- Effusion from reactive synovitis
Signs:
- Restricted hip range of motion — particularly abduction and internal rotation
- Trendelenburg gait (abductor weakness)
- In advanced disease: muscular atrophy of the buttocks, thigh and calf; limb length discrepancy up to 2.5 cm
Differential diagnosis: Septic arthritis, transient synovitis, blood dyscrasias (sickle cell), hypothyroidism, multiple epiphyseal dysplasia, Gaucher disease
— ROSEN's Emergency Medicine; Miller's Review of Orthopaedics 9th Edition
Pathological Stages (Waldénström Classification)
There are four sequential stages that all cases pass through:
| Stage | Findings |
|---|---|
| 1. Initial (Ischaemic) | Sclerotic epiphysis, medial joint space widening; radiographs may be normal for 4–6 months |
| 2. Fragmentation | Bone resorption and collapse of the femoral head; crescent sign develops |
| 3. Reossification | New bone appears; femoral head gradually reshapes; may last up to 18 months |
| 4. Healed/Remodelled | Continued remodelling until skeletal maturity; residual deformity may persist |
— ROSEN's Emergency Medicine; Miller's Review of Orthopaedics 9th Edition
Investigations
Plain radiography (first line):
- AP pelvis and frog-leg lateral views
- Earliest sign: crescent sign — a radiolucent subchondral fissure indicating subchondral fracture
- Progression: loss of height, fragmentation, sclerosis, and widening of the medial joint space
- May be normal early in disease
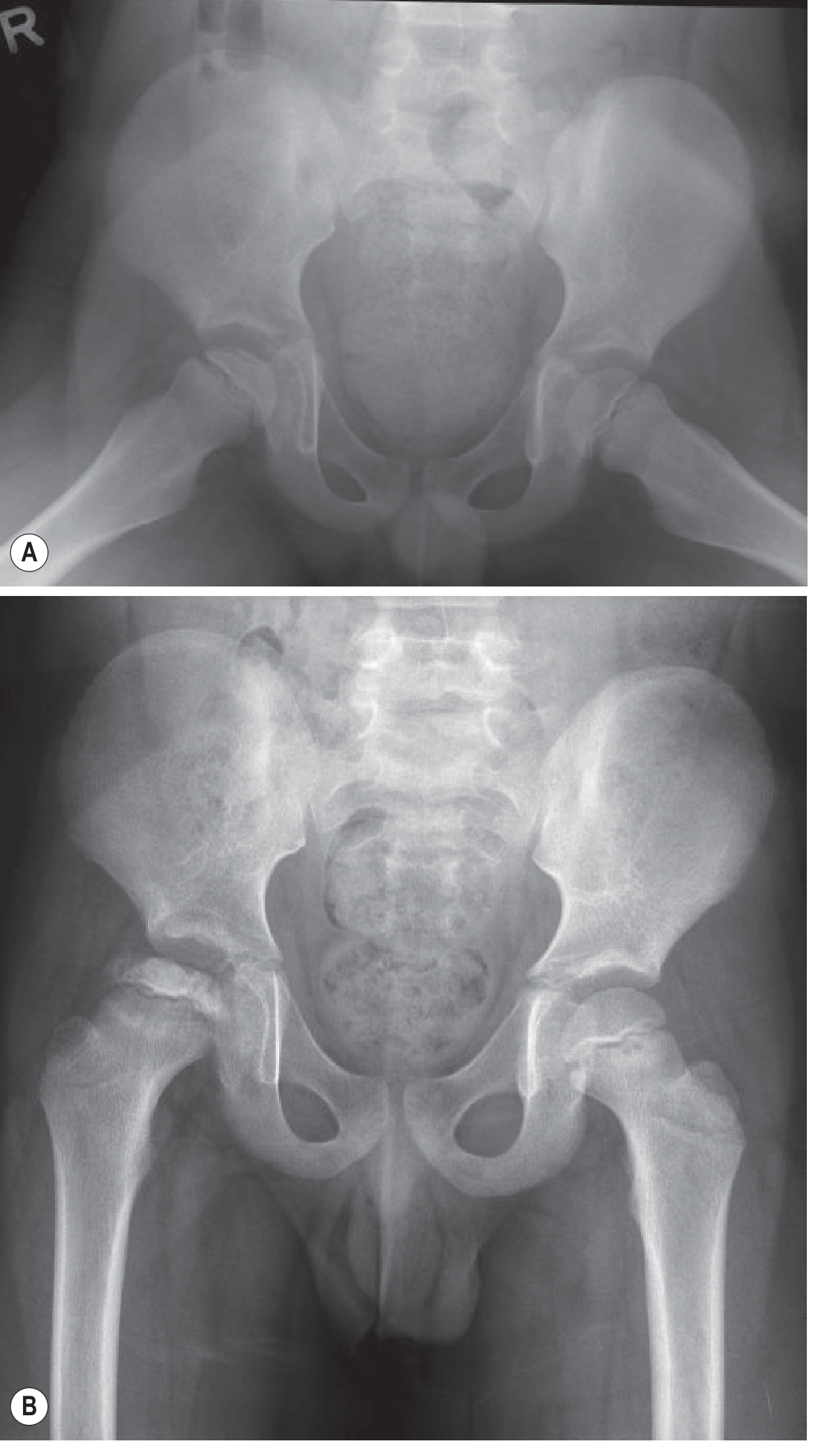
MRI:
- Now the imaging modality of choice when plain radiographs are normal but symptoms persist >6 weeks
- Highly sensitive for early avascular necrosis
- Intravenous contrast helps identify viable versus dead bone in equivocal cases
- Dead bone loses signal on both T1 and T2; MRI also defines extent of involvement
Bone scintigraphy: Highly sensitive and specific, but largely replaced by MRI
— Grainger & Allison's Diagnostic Radiology; ROSEN's Emergency Medicine
Classification Systems
1. Herring Lateral Pillar Classification (most prognostically important)
Assessed during the fragmentation stage on the AP radiograph; based on height of the lateral pillar of the capital femoral epiphysis:
| Group | Lateral Pillar Height | Prognosis |
|---|---|---|
| A | Little/no involvement | Uniformly good outcome |
| B | >50% of height maintained | Good if bone age <6 years; poorer if older |
| B/C | Borderline (50% height, narrow or poorly ossified) | Intermediate |
| C | <50% of height maintained | Poor in all age groups |
2. Catterall Head-at-Risk Signs (radiographic poor prognostic indicators)
- Lateral calcification
- Gage sign (V-shaped defect at lateral physis)
- Lateral subluxation of the femoral head
- Metaphyseal cyst formation
- Horizontal growth plate
3. Modified Catterall Classification (I–IV)
Based on the extent of femoral head involvement (used alongside Herring in some centres).
— Miller's Review of Orthopaedics 9th Edition; Grainger & Allison's Diagnostic Radiology
Prognosis
The single most important determinant of outcome is maintenance of femoral head sphericity. An aspherical femoral head at skeletal maturity leads to early degenerative hip disease.
Poor prognostic factors:
- Older age at onset (chronological age >8 years; bone age >6 years)
- Female sex
- Lateral pillar C classification (poor at any age)
- Lateral pillar B in older children (bone age >6 years)
- Restricted hip range of motion (especially decreased abduction)
- Presence of Catterall head-at-risk signs
— Miller's Review of Orthopaedics 9th Edition
Management
Principles
The overarching goal is containment — keeping the femoral head centred within the acetabulum during the vulnerable period of fragmentation and reossification, to allow the malleable femoral head to remodel into a spherical shape.
Conservative (Non-operative)
- Activity restriction and partial weight-bearing with crutches (days to weeks depending on symptoms)
- NSAIDs/anti-inflammatory medications for pain and synovitis
- Physiotherapy to maintain hip range of motion
- Traction (inpatient or outpatient) to relieve pain and restore abduction
- Petrie casting (bilateral hip abduction cast) — maintains containment
- Bracing (Scottish Rite orthosis and other dynamic abduction orthoses) — used for containment though evidence for bracing over observation alone is debated
Surgical (Operative)
Indicated for older children (chronological age >8 years, bone age >6 years) with lateral pillar B and B/C disease, where surgery improves radiographic outcome at skeletal maturity.
Containment procedures:
- Proximal femoral varus osteotomy — redirects femoral head into acetabulum
- Pelvic osteotomy (Salter, triple, Dega, or Pemberton) — redirects acetabulum over the femoral head
- Shelf osteotomy — prevents lateral subluxation and epiphyseal overgrowth
Salvage procedures (for hips that can no longer be contained or have hinge abduction):
- Valgus femoral osteotomy — for hinge abduction deformity
- Chiari pelvic osteotomy and/or shelf procedure — for irreducible hips
- Later in life: total hip arthroplasty for established secondary osteoarthritis
— Miller's Review of Orthopaedics 9th Edition; ROSEN's Emergency Medicine; Grainger & Allison's Diagnostic Radiology
Complications and Long-Term Outcome
- Early degenerative hip arthritis — the principal long-term complication, arising from aspherical femoral head deformity (coxa magna)
- Coxa magna — enlarged, flat femoral head with lateral uncovering
- Limb length discrepancy — up to 2.5 cm
- Hinge abduction — flattened head catches on the acetabular rim on abduction, a mechanically unfavourable pattern
- Children presenting at bone age <6 years with lateral pillar A or B disease generally have good outcomes even without surgical intervention
Summary Table
| Feature | Detail |
|---|---|
| Age | 4–8 years (peak 5–8) |
| Sex | Boys >> girls (4:1) |
| Aetiology | Idiopathic AVN of capital femoral epiphysis |
| Presentation | Limp, hip/knee pain, restricted abduction & IR |
| Key radiograph sign | Crescent sign (subchondral fracture) |
| Best prognostic tool | Herring lateral pillar classification |
| Treatment goal | Containment — preserve femoral head sphericity |
| Worst outcome | Lateral pillar C, age >8, female sex |
Sources: Miller's Review of Orthopaedics 9th Edition | ROSEN's Emergency Medicine | Grainger & Allison's Diagnostic Radiology | Tintinalli's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.