Multinodular goiters with hypothyroidism
Reading File
search_medical_text
multinodular goiter hypothyroidism pathophysiology diagnosis management
search_medical_text
thyroid nodule evaluation TSH levothyroxine treatment guidelines
search_medical_image
multinodular goiter thyroid ultrasound imaging
GradeResponse
GradeResponse
GradeResponse
Here is a comprehensive overview of multinodular goiter (MNG) with hypothyroidism:
Multinodular Goiter with Hypothyroidism
Overview
A multinodular goiter (MNG) is an enlarged thyroid gland containing multiple nodules of varying size and composition. While MNG is more classically associated with euthyroidism or hyperthyroidism (toxic MNG), it can coexist with hypothyroidism — typically due to underlying autoimmune thyroiditis (Hashimoto's) destroying functional thyroid tissue despite structural enlargement, or iodine deficiency.
Pathophysiology
| Mechanism | Details |
|---|---|
| Iodine deficiency | Chronic low iodine → elevated TSH → diffuse goiter → nodule formation over years |
| Hashimoto's thyroiditis | Autoimmune destruction of follicles → compensatory TSH rise → nodularity + eventual hypothyroidism |
| Dyshormonogenesis | Genetic enzyme defects (e.g., thyroid peroxidase mutations) → impaired T4/T3 synthesis → chronic TSH stimulation → MNG |
| DICER1 mutations | Germline mutations predispose to MNG and associated malignancies |
| Sporadic/multifactorial | Somatic mutations in nodules (TSH-R, Gs-α) with background hypothyroidism |
The core pathway: chronic TSH stimulation → hyperplastic nodule growth → heterogeneous autonomy and cystic degeneration.
Clinical Presentation
Symptoms of MNG (structural):
- Visible or palpable neck mass, often asymmetric
- Dysphagia (esophageal compression)
- Dyspnea or stridor (tracheal compression)
- Hoarseness (recurrent laryngeal nerve involvement — raises concern for malignancy)
- Superior vena cava syndrome (large substernal goiters)
Symptoms of hypothyroidism:
- Fatigue, cold intolerance, weight gain
- Constipation, dry skin, coarse hair, brittle nails
- Bradycardia, diastolic hypertension
- Myxedema (periorbital/peripheral puffiness)
- Cognitive slowing, depression
- Menstrual irregularities
Diagnosis
Lab Evaluation
| Test | Finding in MNG + Hypothyroidism |
|---|---|
| TSH | Elevated (primary hypothyroidism) |
| Free T4 | Low (overt) or normal (subclinical) |
| Free T3 | Low or normal |
| Anti-TPO antibodies | Positive → suggests Hashimoto's etiology |
| Anti-thyroglobulin Ab | May be positive |
Per ATA guidelines, serum TSH should be obtained for any thyroid nodule >1 cm. A higher TSH — even within the upper normal range — is associated with increased malignancy risk in thyroid nodules (ATA Thyroid Nodule & DTC Guidelines, p. 11).
Imaging
Thyroid ultrasound is the primary imaging modality:
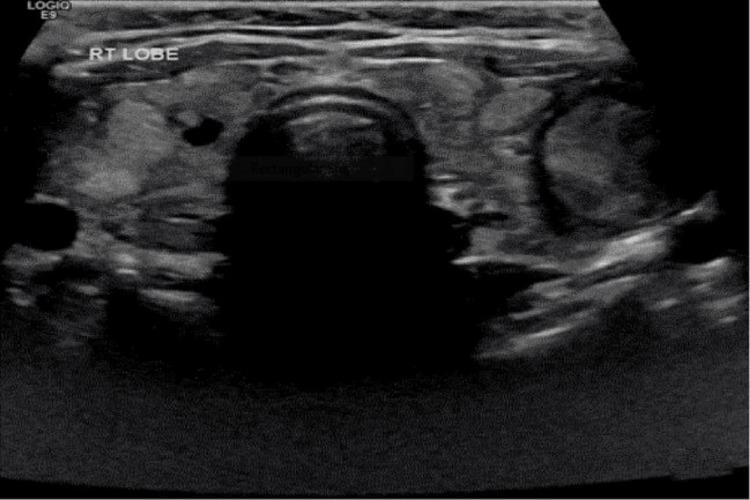
Ultrasound features to assess:
- Number, size, composition (solid vs. cystic)
- Echogenicity and margins
- Microcalcifications (suspicious for malignancy)
- Vascularity (Doppler)
- Lymphadenopathy
Radionuclide scan (¹²³I or Tc-99m):
- Indicated if TSH is subnormal (to identify hot/warm/cold nodules)
- In hypothyroid MNG, TSH is elevated → scan less useful to differentiate autonomy; ultrasound preferred
- Cold nodules have higher malignancy risk; hot nodules rarely malignant
Fine Needle Aspiration (FNA)
- Indicated for nodules with suspicious sonographic features (TIRADS 4–5) or size thresholds per ATA/ACR guidelines
- In MNG, the dominant or most suspicious nodule guides FNA decisions
- Bethesda system classifies cytology (I–VI)
Management
1. Treat the Hypothyroidism
- Levothyroxine (LT4) is the standard of care for overt hypothyroidism
- Dose: ~1.6 mcg/kg/day (adjusted by TSH)
- Target TSH: 0.5–2.5 mIU/L (lower end reasonable in younger patients)
- Subclinical hypothyroidism (TSH 4–10): treat if symptomatic, anti-TPO positive, pregnant, or TSH >10
2. Goiter/Nodule Management
Per Harrison's 21st Edition (p. 10749):
"Most nontoxic MNGs can be managed conservatively. T₄ suppression is rarely effective for reducing goiter size and introduces the risk of subclinical or overt thyrotoxicosis, particularly if there is underlying autonomy."
| Option | Indication | Notes |
|---|---|---|
| LT4 alone | Hypothyroid MNG with Hashimoto's | Treats hypothyroidism; not given to suppress TSH below normal |
| Radioiodine (¹³¹I) | Large MNG unsuitable for surgery | Reduces volume 40–60%; dose ~3.7 MBq/g tissue corrected for uptake; repeat may be needed (Harrison's, p. 10749) |
| Surgery (thyroidectomy) | Compressive symptoms, suspicious malignancy, large substernal goiter, cosmesis | Total or near-total thyroidectomy; post-op LT4 replacement mandatory |
| Watchful waiting | Small asymptomatic MNG, benign cytology, stable TSH management | Serial ultrasound q12–24 months |
| Percutaneous ethanol injection / RFA | Select benign cystic/solid nodules | Emerging; reduces nodule volume |
Note: Avoid iodine-containing contrast agents (risk of Jod-Basedow thyrotoxicosis if autonomous nodules are present), though this is less relevant in purely hypothyroid patients.
Special Considerations
- Substernal/retrosternal MNG: May cause SVC syndrome, Pemberton's sign (facial congestion on arm elevation); CT chest for airway assessment; surgical referral often needed
- Malignancy surveillance: MNG does not significantly increase overall cancer risk, but each dominant/suspicious nodule must be evaluated independently
- Pregnancy: TSH targets are trimester-specific; LT4 dose often needs to increase 25–30% in first trimester
- Elderly: Subclinical hypothyroidism may be left untreated cautiously; risk of atrial fibrillation with over-replacement
Summary Algorithm
MNG detected
↓
Check TSH
↓
TSH Elevated (Hypothyroidism)
↓
Free T4, anti-TPO, anti-TG antibodies
↓
Thyroid ultrasound → characterize nodules (TIRADS)
↓
FNA of suspicious/dominant nodules (per ATA criteria)
↓
Start LT4 for hypothyroidism
↓
Compressive symptoms / large goiter / malignancy concern?
→ Yes: Surgery or ¹³¹I (if surgery contraindicated)
→ No: Serial surveillance ultrasound q12–24 months
Sources:
- Harrison's Principles of Internal Medicine, 21st Edition, p. 10749
- ATA Guidelines: Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer, p. 11
This is a shared conversation. Sign in to Orris to start your own chat.