Staphylococcus all detail with classification
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Loading Image
Loading Image
I now have comprehensive information from multiple authoritative textbooks. Let me compile the full detailed response.
Staphylococcus — Complete Overview
1. Taxonomy & General Characteristics
Kingdom: Bacteria | Phylum: Firmicutes | Class: Bacilli | Order: Bacillales | Family: Staphylococcaceae | Genus: Staphylococcus
The genus Staphylococcus contains at least 45 species. They are Gram-positive spherical cocci (~1 µm diameter) arranged in irregular grape-like clusters (the name derives from Greek staphylé = bunch of grapes). Single cocci, pairs, tetrads, and chains are also seen in liquid culture. They are:
- Non-motile
- Non-spore forming
- Catalase positive (distinguishes from Streptococcus)
- Facultative anaerobes
- Actively ferment carbohydrates
2. Classification
Primary Clinical Division: Coagulase Test
| Feature | Coagulase-Positive | Coagulase-Negative (CoNS) |
|---|---|---|
| Key species | S. aureus | S. epidermidis, S. saprophyticus, S. lugdunensis, S. haemolyticus, S. warneri, S. hominis |
| Pathogenicity | Major human pathogen | Opportunistic; device-associated |
| Coagulase | + (tube & slide) | − (except S. lugdunensis: slide+ tube−) |
| α-toxin | Present | Absent |
| Protein A | Present | Absent |
Note: S. lugdunensis is slide coagulase positive but tube coagulase negative, and it behaves more aggressively than typical CoNS.
The 4 Most Clinically Important Species
| Species | Key Feature | Common Infection |
|---|---|---|
| S. aureus | Coagulase positive, Protein A, golden pigment | Skin, bloodstream, endocarditis, pneumonia, toxin-mediated diseases |
| S. epidermidis | Biofilm formation on plastics | Prosthetic valve/device infections, neonatal bacteremia |
| S. saprophyticus | Novobiocin resistant | UTI in young women |
| S. lugdunensis | Slide coagulase positive | Aggressive endocarditis, skin infections |
3. Morphology & Culture
- Morphology: Spherical, ~1 µm, clusters (sometimes pairs/chains in broth)
- Gram stain: Gram-positive (older cells may appear Gram-variable)
- Growth: Grows readily on blood agar, nutrient agar; aerobic or microaerophilic; grows best at 37°C, but pigment forms best at 20–25°C
- Colony morphology:
- S. aureus: smooth, raised, glistening; gray to deep golden yellow (due to carotenoid pigments) → hence "aureus" (Latin: gold)
- S. epidermidis: gray to white colonies
- Beta-hemolysis: Seen with S. aureus (and occasionally others) on blood agar
- Selective media: Mannitol-salt agar (ferments mannitol → yellow halo), chromogenic agar
4. Structure & Virulence Factors
Cell Wall Components
| Component | Function |
|---|---|
| Peptidoglycan (thick) | Structural; allows survival on dry surfaces for prolonged periods; triggers inflammation |
| Teichoic acid (ribitol-type in S. aureus) | Cell wall integrity, adherence |
| Polysaccharide capsule | Antiphagocytic in some strains |
| Protein A | Binds Fc region of IgG (Fab directed outward) → blocks opsonization; present in most S. aureus clinical isolates |
| Clumping factors (ClfA, ClfB) | Bind fibrinogen → facilitate adhesion to tissue/foreign bodies |
| Fibronectin-binding proteins (FnBPA, FnBPB) | Adherence to fibronectin |
Enzymes (Extracellular)
| Enzyme | Action |
|---|---|
| Coagulase | Binds prothrombin → converts fibrinogen to fibrin → fibrin clot; the key diagnostic test |
| Catalase | Destroys H₂O₂ → helps survive inside phagocytes |
| Hyaluronidase | "Spreading factor" — degrades connective tissue |
| Staphylokinase (fibrinolysin) | Dissolves clots |
| Lipases | Hydrolyze lipids — important in skin colonization |
| Nucleases (DNase) | Degrade DNA in neutrophil extracellular traps |
| Penicillinase (β-lactamase) | Destroys β-lactam ring of penicillins |
Toxins
| Toxin | Mechanism | Disease |
|---|---|---|
| α-Hemolysin (α-toxin) | Pore-forming; inserts into lipid bilayer → transmembrane pores → cell lysis (keratinocytes, RBCs, platelets) | Tissue destruction in infections |
| β-Hemolysin | Sphingomyelinase → damages sphingomyelin-rich membranes | RBC lysis (cold-active) |
| δ-Hemolysin | Detergent-like disruption of membranes | General cytotoxin |
| γ-Hemolysin / PVL | Panton-Valentine leukocidin — pore-forming; attacks neutrophils and platelets → tissue necrosis; found in < 10% of isolates but highly virulent; associated with community-acquired MRSA | Necrotizing pneumonia, furunculosis |
| Exfoliative toxins A & B (ETA, ETB) | Serine proteases; cleave desmoglein-1 in stratum granulosum of epidermis → loss of intercellular adhesion | Scalded Skin Syndrome (SSSS), bullous impetigo |
| Staphylococcal Enterotoxins (SE) A–R | Superantigens — cross-link MHC II with T-cell receptor → massive cytokine release; heat-stable | Food poisoning (SE-A most common), Toxic Shock Syndrome |
| TSST-1 (Toxic Shock Syndrome Toxin-1) | Superantigen; causes massive T-cell activation and cytokine storm | Toxic Shock Syndrome (TSS) |
5. Epidemiology & Normal Flora
- Carriage sites: Anterior nares (20–30% of healthy adults), skin, perineum, vagina, oropharynx
- MRSA nasal carriage is the most common source of healthcare-associated transmission
- Organisms survive on dry surfaces for prolonged periods (thickened peptidoglycan, no outer membrane)
- Transmission: Direct contact, contaminated fomites (bed linens, clothing), droplets
- Risk factors: Foreign bodies (catheters, sutures, prostheses), prior surgery, antibiotic-suppressed normal flora, immunocompromise, extremes of age
6. Diseases Caused
A. Staphylococcus aureus Diseases
Toxin-Mediated Diseases
| Disease | Toxin | Clinical Features |
|---|---|---|
| Food Poisoning | SE-A (most common) | Rapid onset (1–6 h) — nausea, vomiting, watery diarrhea, cramps; resolves within 24 h; no fever; no live bacteria needed |
| Toxic Shock Syndrome (TSS) | TSST-1, SE | Fever, hypotension, diffuse macular erythematous rash, multiorgan failure; associated with tampons, wound packing |
| Scalded Skin Syndrome (SSSS) (Ritter disease) | ETA, ETB | Perioral erythema spreading over body → positive Nikolsky sign → bullae → desquamation; blisters have no organisms or leukocytes; seen in neonates and young children; toxin cleaves desmoglein-1 |
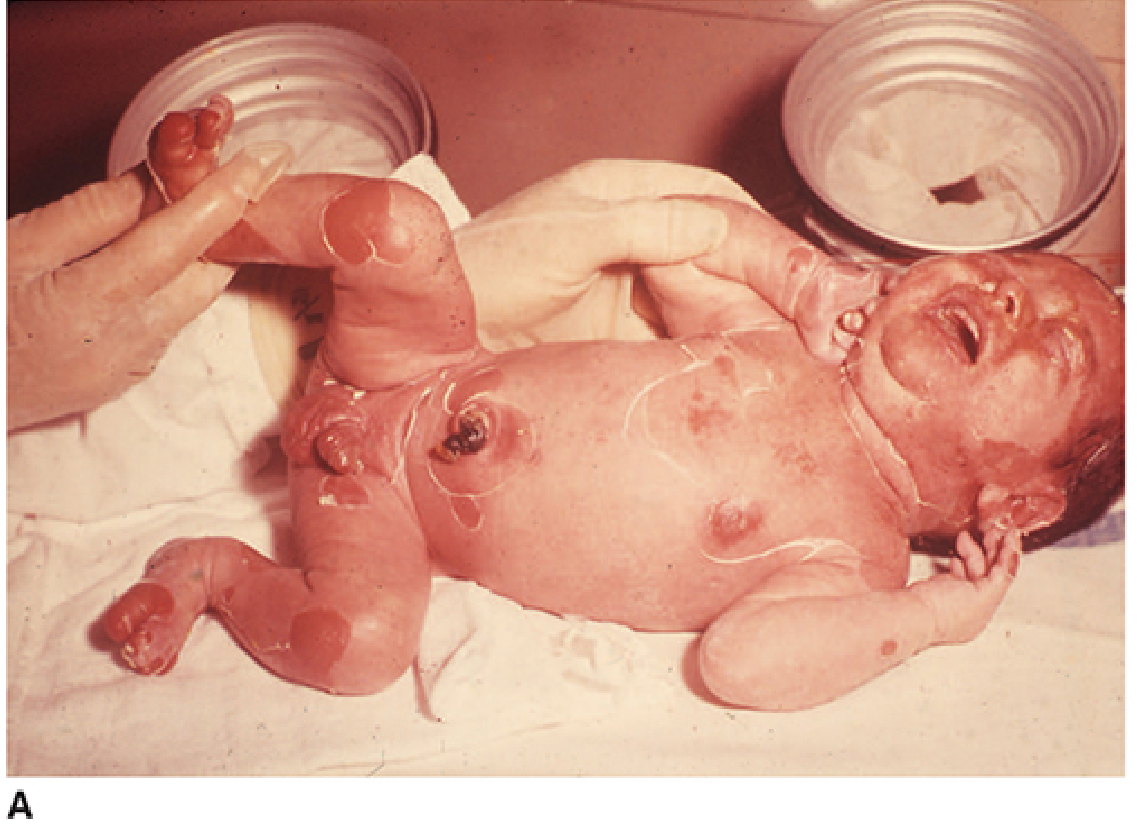
Pyogenic (Suppurative) Infections
| Infection | Description |
|---|---|
| Impetigo | Localized superficial cutaneous infection; pus-filled vesicles on erythematous base; seen in young children |
| Folliculitis | Infection of hair follicle |
| Furuncle (boil) | Large, painful, pus-filled cutaneous nodule; focal abscess |
| Carbuncle | Coalescence of furuncles extending into subcutaneous tissues; systemic signs (fever, chills, bacteremia) |
| Wound infections | Surgical or traumatic sites |
| Bacteremia | Seeding of bloodstream from skin/device focus; may be transient or sustained |
| Endocarditis | Right-sided (IV drug users) or left-sided; can destroy heart valves rapidly |
| Pneumonia | Consolidation + abscess formation; post-influenza; necrotizing pneumonia with septic shock (high mortality) |
| Empyema | Pus in pleural space |
| Osteomyelitis | Metaphysis of long bones (hematogenous); destructive; most common cause in children |
| Septic arthritis | Purulent joint effusion; painful erythematous joint |
| Meningitis | Via shunts or hematogenous spread |
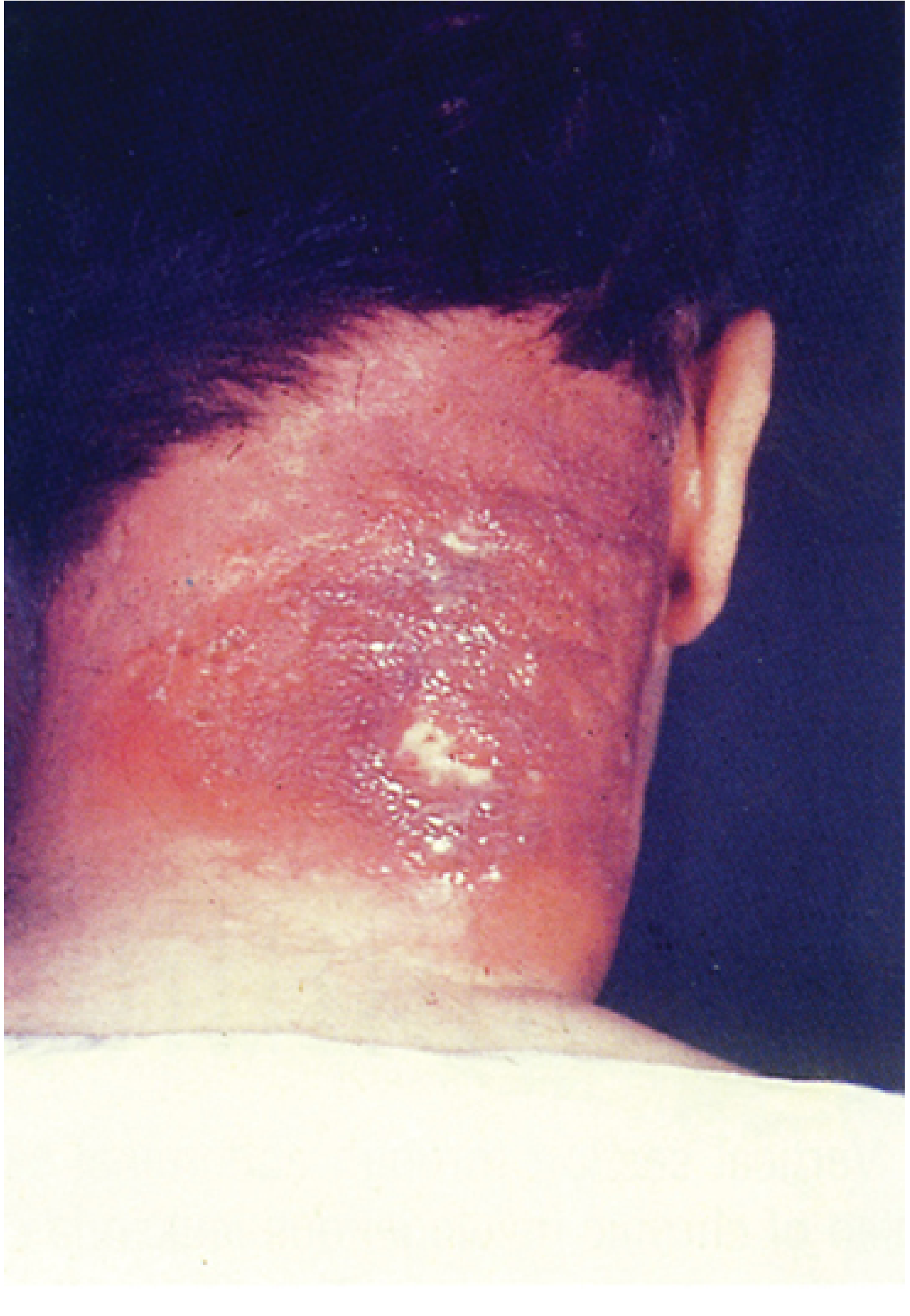
B. Coagulase-Negative Staphylococci (CoNS) Diseases
CoNS lack α-toxin, exfoliatin, and SAG toxins. Their pathogenicity depends on biofilm formation.
| Species | Disease |
|---|---|
| S. epidermidis | Prosthetic valve endocarditis, IV catheter infections, CSF shunt infections, neonatal sepsis in premature infants, prosthetic joint infections |
| S. saprophyticus | UTI in young sexually active women (2nd most common cause after E. coli) |
| S. lugdunensis | Aggressive native valve endocarditis, skin/soft tissue infections |
| S. haemolyticus | Catheter infections, multi-drug resistant isolates |
Biofilm mechanism (S. epidermidis): Attaches to medical devices (fibrinogen, fibronectin, collagen, plastics) → secretes extracellular polysaccharide (slime layer) → envelops bacteria → barrier against antibiotics and host defenses.
7. Laboratory Diagnosis
Staining
- Gram stain: Gram-positive cocci in clusters
- Useful for pyogenic infections; not reliable for blood or toxin-mediated infections
Culture & Biochemical Tests
| Test | S. aureus | CoNS |
|---|---|---|
| Coagulase (tube test) | + | − (except S. lugdunensis slide+) |
| Catalase | + | + |
| Mannitol fermentation | + (aerobic & anaerobic) | S. epidermidis: − |
| DNase | + | − |
| Protein A | + | − |
| Beta-hemolysis | +/− | − |
| Novobiocin sensitivity | Sensitive | S. saprophyticus: Resistant; others: Sensitive |
Selective Media
- Mannitol-salt agar (MSA): Selective for staphylococci (7.5% NaCl); S. aureus turns yellow (mannitol +)
- Chromogenic agar: Color-based identification of S. aureus / MRSA
Molecular Methods
- Nucleic acid amplification tests (NAAT): Screening for MSSA and MRSA nasal carriage
- PCR for mecA/mecC genes: Definitive identification of MRSA
- Mass spectrometry (MALDI-TOF): Rapid species identification
8. Antibiotic Resistance
Evolution of Resistance
| Stage | Mechanism |
|---|---|
| Penicillin resistance (>90% strains) | β-Lactamase (penicillinase) — hydrolyzes β-lactam ring |
| MRSA | mecA gene → encodes PBP2a (penicillin-binding protein 2a) with low affinity for all β-lactams → resistant to all penicillins, cephalosporins, carbapenems |
| Heterogeneous resistance | Not all cells in a population express resistance uniformly; requires mecA/mecC detection |
| VISA (Vancomycin-Intermediate S. aureus) | Thicker, disorganized cell wall traps vancomycin before it reaches cytoplasmic membrane |
| VRSA (Vancomycin-Resistant S. aureus) | vanA gene acquired from VRE → modified peptidoglycan does not bind vancomycin |
Community vs. Hospital MRSA
| Feature | Community-acquired MRSA (CA-MRSA) | Hospital-acquired MRSA (HA-MRSA) |
|---|---|---|
| Most common manifestation | Skin & soft tissue infections | Bloodstream, device-associated |
| PVL | Often positive | Usually negative |
| Antibiotic susceptibility | More susceptible to non-β-lactams | More broadly resistant |
9. Treatment
S. aureus Infections
| Scenario | Drug of Choice |
|---|---|
| MSSA, non-serious | Dicloxacillin, nafcillin, oxacillin |
| MSSA, serious (bacteremia, endocarditis) | Nafcillin or oxacillin IV |
| MRSA, oral | TMP-SMX, doxycycline/minocycline, clindamycin, linezolid |
| MRSA, IV (serious) | Vancomycin (drug of choice); alternatives: daptomycin, tigecycline, linezolid |
| Localized abscesses | Incision and drainage ± antibiotics |
| Food poisoning | Supportive (toxin is pre-formed; antibiotics not indicated) |
CoNS Infections
- Device removal often required
- Vancomycin for serious infections (many CoNS are methicillin-resistant)
- Rifampin added in biofilm-associated infections
10. Prevention & Control
- Hand hygiene (thorough handwashing) is the single most important measure
- Covering exposed skin surfaces for healthcare workers
- Nasal decolonization with intranasal mupirocin ± chlorhexidine body wash for MRSA carriers before elective surgery
- Proper wound cleansing and use of antiseptics (iodine, hexachlorophene, germicidal soap)
- Contact precautions for MRSA-colonized/infected patients
- Adequate aseptic technique for catheter insertion and maintenance
- No vaccine currently available for S. aureus (several in trials)
Summary Classification Table
Genus: Staphylococcus (≥45 species)
│
├── COAGULASE-POSITIVE
│ └── S. aureus ────── Major pathogen; MRSA; toxin-mediated diseases
│ (SSSS, TSS, food poisoning); pyogenic infections
│
└── COAGULASE-NEGATIVE (CoNS)
├── S. epidermidis ── Most common CoNS; device/biofilm infections
├── S. saprophyticus ─ UTI in young women; novobiocin-resistant
├── S. lugdunensis ── Aggressive endocarditis; slide-coagulase+
├── S. haemolyticus ─ Catheter infections; multidrug resistant
├── S. warneri
├── S. hominis
└── (40+ other species)
Sources:
- Jawetz, Melnick & Adelberg's Medical Microbiology, 28e — Ch. 13: The Staphylococci
- Murray's Medical Microbiology, 9e — Ch. 18: Staphylococcus
- Sherris & Ryan's Medical Microbiology, 8e — Ch. 24: Staphylococci
- Red Book 2021 — Coagulase-Negative Staphylococcal Infections
This is a shared conversation. Sign in to Orris to start your own chat.