Squint
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
I now have enough content to give a comprehensive answer on squint (strabismus). Let me compile it.
Squint (Strabismus)
Definition
Squint, formally called strabismus, is a condition in which the visual axes of the two eyes do not intersect at the point of fixation — i.e., the eyes are misaligned. It may be latent (phoria: deviation only when fusion is blocked) or manifest (tropia: always present).
"Strabismus, also called squint or cross-eye, means lack of fusion or misalignment of the eyes in one or more of the visual coordinates: horizontal, vertical, or rotational." — Guyton and Hall Textbook of Medical Physiology
Types
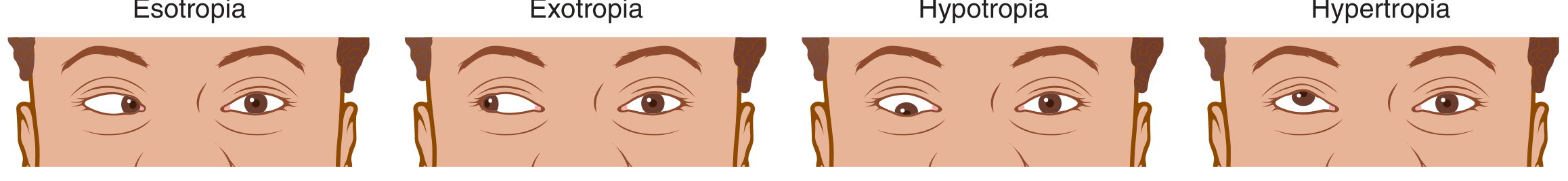
| Type | Direction of Deviation |
|---|---|
| Esotropia | One or both eyes turn inward (toward the nose) — "crossed eyes" |
| Exotropia | One or both eyes turn outward |
| Hypertropia | One or both eyes deviate upward |
| Hypotropia | One or both eyes deviate downward |
Heterophoria = latent deviation controlled by fusion reflex; becomes symptomatic when decompensating (asthenopia, diplopia).
Heterotropia = manifest deviation; image from the deviating eye is either diplopic or suppressed (especially in children).
Classification
By Comitance
- Comitant (concomitant): Angle of deviation is the same in all directions of gaze. Typically childhood-onset.
- Incomitant (paralytic/restrictive): Angle varies with gaze direction; due to extraocular muscle palsy or mechanical restriction (e.g. thyroid eye disease, blow-out fracture, nerve palsy).
By Onset
- Congenital / early-onset: Often presents within first 6 months
- Acquired: May be accommodative, paralytic, or secondary to systemic disease
Aetiology
- Failure of binocular fusion mechanisms in early development
- Refractive errors: Hypermetropia is the most common cause; accommodative esotropia typically appears between 18–36 months
- Anisometropia: Unequal refraction between the two eyes
- Extraocular muscle palsy: CN III, IV, or VI palsies
- Mechanical restriction: Thyroid ophthalmopathy, orbital floor fracture
- Systemic/neurological disease: Diabetes mellitus, stroke, brain tumours, cerebral palsy, raised intracranial pressure
- Underlying ocular pathology: Retinoblastoma, macular scarring, optic disc hypoplasia (mandatory to exclude)
Consequences
Amblyopia (Lazy Eye)
The deviating eye's image is suppressed at cortical level. The longer the duration of squint in early childhood, the greater the risk of amblyopia. Organic disease must be excluded before treating amblyopia.
Sensory Adaptations in Children
- Suppression: Active cortical inhibition of the deviating eye's image
- Abnormal retinal correspondence (ARC): A new, anomalous correspondence develops between non-corresponding retinal points
- Microtropia: Small-angle squint (<10Δ) with partial binocular cooperation; a central suppression scotoma is characteristic
In Adults
Sudden onset of diplopia is the predominant symptom (suppression does not develop as readily).
Clinical Evaluation
History
- Age of onset (earlier onset → higher amblyopia risk; later onset → more likely accommodative)
- Variability (intermittent vs. constant)
- Type of diplopia (horizontal, vertical, cyclovertical)
- Family history (strabismus is frequently familial)
- Birth history, developmental milestones, general health
Visual Acuity
- Pre-verbal children: fixation behaviour, preferential looking tests
- Verbal children (≥3 years): crowded logMAR letter/picture tests (Kay pictures, Keeler logMAR)
- LogMAR tests preferred over Snellen for monitoring amblyopia therapy
Cover Tests
- Cover test: Detects manifest deviation — cover the fixing eye and look for movement of the deviating eye to take up fixation
- Uncover test: Detects latent deviation — adduction of the uncovered eye = exophoria; abduction = esophoria
- Alternate cover test: Reveals the total deviation (manifest + latent) by disrupting fusion
- Prism cover test: Quantifies the angle of deviation in prism dioptres (Δ); performed in primary position, 8 diagnostic gaze positions, and near fixation
Sensory Tests
- Worth four-dot test: Differentiates binocular single vision (BSV), ARC, suppression
- Bagolini striated glasses: Detects BSV, ARC, or suppression under natural conditions
- Synoptophore: Tests 3 grades of binocularity — simultaneous perception, fusion (with motor fusion range), stereopsis; also detects ARC
Stereopsis Tests
- Titmus test: Polarized vectorgraph; fly (3000"), animals (400–100"), circles (800–40")
- TNO / Frisby: Random dot tests — best evidence of high-grade BSV
Other Tests
- Hess chart / Lees screen: Maps ocular motility in incomitant strabismus (muscle palsies, restrictive disease); primary and secondary deviation can be distinguished
- Field of binocular single vision: Goldmann or tangent screen; useful in paretic strabismus follow-up
- Diplopia charting / botulinum toxin test: For intractable diplopia
- Angle kappa: Large positive angle kappa can mimic exotropia (pseudo-squint) — important to distinguish
Refraction and Fundoscopy
- Cycloplegic refraction: Mandatory; hypermetropia is most common refractive cause
- Dilated fundoscopy: Mandatory — exclude retinoblastoma, macular scarring, optic disc hypoplasia
Management
Optical Correction
Prescribe the full cycloplegic refraction. In accommodative esotropia, correcting hypermetropia may fully or partially eliminate the deviation.
Amblyopia Treatment
- Occlusion (patching) of the dominant eye to stimulate the amblyopic eye
- Atropine penalisation as an alternative
- Best results achieved during the sensitive period (before ~8 years of age)
Prisms
- Fresnel or ground-in prisms to neutralise deviation, especially in diplopia management and in elderly adults with sagging eye syndrome (ARDE)
Botulinum Toxin
- Injected into the overacting muscle; diagnostic and therapeutic use (especially for acute paralytic strabismus and intractable diplopia)
Surgery
- Indicated when optical treatment fails to achieve alignment
- Recession (weakening): Muscle insertion moved posteriorly
- Resection (strengthening): Section of muscle removed, reattached at original insertion
- Adjustable sutures: Improve outcomes; suture tension adjusted postoperatively under topical anaesthesia
- Goal in early-onset esotropia: alignment within 8Δ with peripheral fusion and central suppression
- Inferior oblique overaction: Treated surgically if significant
Sources: Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed. | Guyton and Hall Textbook of Medical Physiology
This is a shared conversation. Sign in to Orris to start your own chat.