Melonoma nail medicine
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Loading Image
I now have comprehensive information to provide a thorough answer on nail melanoma (subungual/ungual melanoma). Let me synthesize everything.
Nail Melanoma (Subungual / Ungual Melanoma)
Overview
Nail melanoma is a subtype of acral lentiginous melanoma arising from melanocytes of the nail matrix. It accounts for:
- 1.5–2.5% of all melanomas in light-skinned individuals
- 10–20% in Asians
- Up to 25% in Africans
Despite these figures, the absolute incidence is similar across ethnicities. Since nails represent <1% of body surface area but are overrepresented as a melanoma site, the nail matrix is considered a zone of concentrated melanoma risk.
Peak incidence: 5th–7th decades, though it can occur at any age. No clear gender predominance.
Most common sites: Thumbs > big toes > index fingers > middle fingers.
— Fitzpatrick's Dermatology, Vol. 1–2, p. 1636
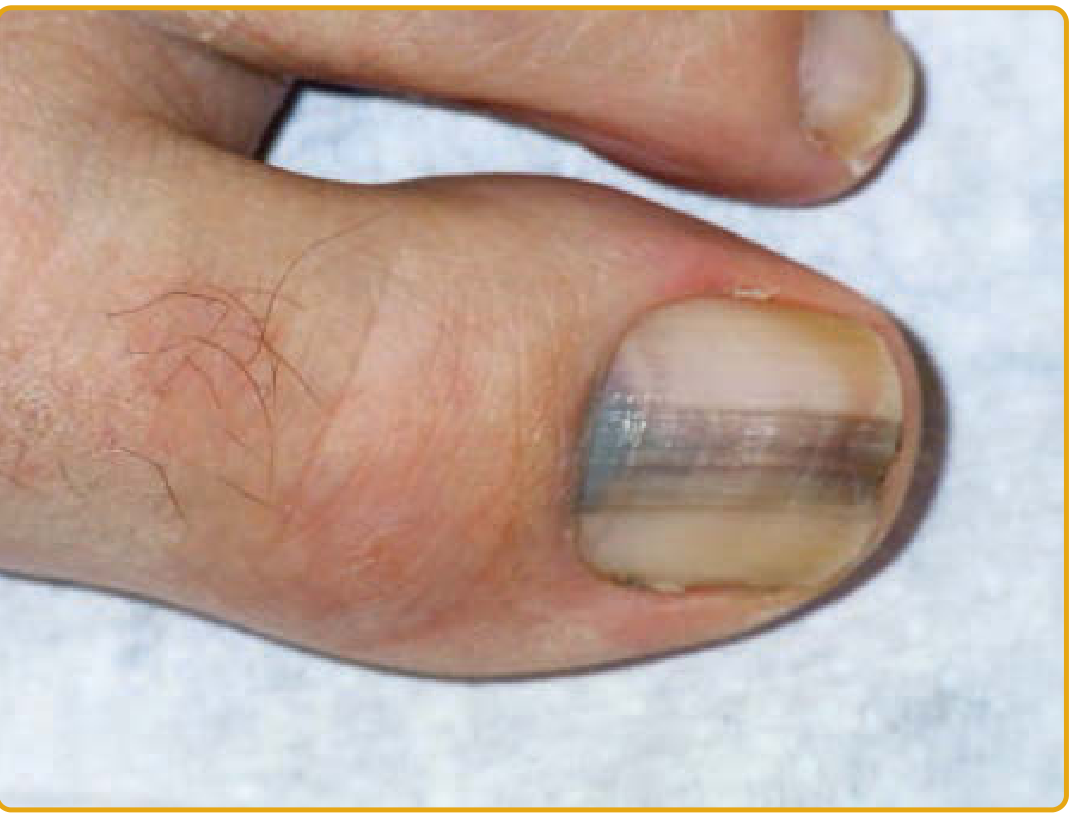
Clinical Presentation
1. Longitudinal Melanonychia (LM) — most common sign
A longitudinal brown-to-black band extending from the proximal nail fold to the distal margin. Melanoma-associated LM is irregular in outline and color, and proximal widening signals rapid growth.
2. Hutchinson Sign
Periungual pigmentation extending onto the proximal or lateral nail folds — represents periungual spread of the in situ component. A micro-Hutchinson sign (visible only on dermoscopy) may precede visible spread.
3. Amelanotic Nail Melanoma (~25–33%)
- Arises from the nail bed (not matrix)
- Causes onycholysis that may ooze
- Frequently misdiagnosed as pyogenic granuloma, ingrown nail, wart, or onychomycosis
- Poses the greatest diagnostic challenge
4. Advanced Disease Signs
- Nail dystrophy
- Bleeding or ulceration
Differential Diagnosis
Subungual melanoma can be mistaken for:
- Subungual hematoma
- Onychomycosis
- Pyogenic granuloma
- Verruca vulgaris (wart)
- Chronic paronychia
- Kaposi's sarcoma
- Glomus tumor
- Subungual hyperkeratosis
- Benign longitudinal melanonychia
— Andrews' Diseases of the Skin, p. 376
Approach to Longitudinal Melanonychia
Single-digit melanonychia in an adult with no systemic or local causative factors = biopsy to exclude melanoma.
Dermoscopy can help assess the internal structure and detect micro-Hutchinson sign, but has limitations:
- Cannot be performed on totally black or very thick nails
- May give false results (irregular lines can appear in benign lesions, especially in children)
- Histopathology remains the gold standard
— Dermatology 2-Volume Set 5e, p. 1446
ABCDEF Rule for Subungual Melanoma
A useful clinical detection framework:
| Letter | Feature |
|---|---|
| A | Age (peak 5th–7th decade); African, Asian, or American Indian ethnicity |
| B | Band of pigmentation: Brown/black, Breadth ≥3 mm, Borders irregular |
| C | Change in band (rapid growth or failure to improve after treatment) |
| D | Digit involved (thumb > hallux > index finger; single digit) |
| E | Extension of pigment onto proximal/lateral nail folds (Hutchinson sign) |
| F | Family or personal history of melanoma / dysplastic nevus syndrome |
— Dermatology 2-Volume Set 5e (eTable 71.1), adapted from Levit et al.
Diagnosis
- Nail matrix biopsy is essential for definitive diagnosis
- Nail plate biopsy can distinguish melanoma from other types of nail pigmentation
- A diagnostic algorithm has been proposed for pigmented melanomas, but is not useful for amelanotic forms
- Dermoscopy (onychoscopy) is a useful adjunct but not definitive
Prognosis
Nail melanomas are typically diagnosed very late — delays of years to decades are common. This contributes to poor outcomes:
- 5-year survival: 15–20% for invasive nail melanoma
The late diagnosis is partly because amelanotic forms are easily misdiagnosed, and even pigmented forms are underrecognized in clinical settings.
Management (Surgical)
- Wide local excision is the primary treatment
- Historically, amputation of the affected digit was standard, but more conservative digit-sparing excision is increasingly used
- Sentinel lymph node biopsy per melanoma staging guidelines
- Adjuvant systemic therapy follows standard melanoma protocols (immunotherapy, targeted therapy for BRAF-mutant disease)
— Sabiston Textbook of Surgery; Andrews' Diseases of the Skin
Key Takeaway: Any new single-digit longitudinal melanonychia in an adult, especially with an irregular band, proximal widening, or Hutchinson sign, should be evaluated urgently with dermoscopy and nail matrix biopsy to exclude melanoma. Diagnostic delay is the primary driver of poor outcomes in this condition.
This is a shared conversation. Sign in to Orris to start your own chat.