Non Hodgkin's lymphoma
Reading File
Finding Sources
Finding Sources
Reading File
Searching Images
non-Hodgkin lymphoma pathology classification
Reading File
Loading Image
Here is a comprehensive overview of Non-Hodgkin's Lymphoma (NHL):
Non-Hodgkin's Lymphoma (NHL)
Definition
Lymphomas are solid tumors of the immune system. Non-Hodgkin lymphoma (NHL) is a heterogeneous group of malignancies arising from lymphoid cells, predominantly B cells (~85–90%) and T/NK cells (~10–15%). Unlike Hodgkin lymphoma, NHL lacks the pathognomonic Reed-Sternberg cell and does not follow predictable contiguous nodal spread.
Epidemiology
- ~80,000 new cases/year in the United States; ~20,000 deaths/year
- Accounts for ~5% of new cancers and ~3% of cancer deaths in the US
- Lifetime risk: 2.4% (men) and 1.9% (women)
- Incidence rises dramatically with age; higher in Whites than other ethnic groups
- Geographic variation up to 5-fold: highest in US, Europe, and Australia; lower in Asia
- Incidence increased 3–4%/year from 1950 to early 2000s; has since plateaued; death rate declining
Pathobiology & Risk Factors
Genetic Factors
- Familial clusters described; slightly higher risk among first-degree relatives
- Associated polymorphisms in immunity genes: chemokines, TNF, IL-10, lymphotoxin-α
- Cell-cycle and apoptosis gene variants also implicated
Immune System Abnormalities
- Inherited immunodeficiencies can increase risk up to 250-fold (e.g., X-linked lymphoproliferative disorder via SH2D1A mutations and EBV)
- Post-transplantation lymphoproliferative disorder (PTLD) in up to 20% of solid organ transplant recipients
- HIV/AIDS, rheumatoid arthritis, Sjögren syndrome (30–40× risk for marginal zone lymphoma), Hashimoto thyroiditis (thyroid lymphoma), celiac disease (enteropathy-type T-cell lymphoma)
Infectious Agents
| Agent | Associated Lymphoma |
|---|---|
| Epstein-Barr virus (EBV) | Burkitt (>95% endemic), PTLD, AIDS lymphomas, NK/T-cell lymphoma, plasmablastic |
| HTLV-1 | Adult T-cell leukemia/lymphoma (virtually 100%) |
| HHV-8 | Primary effusion lymphoma |
| Hepatitis C virus | Lymphoplasmacytic lymphoma, splenic/nodal marginal zone lymphoma |
| H. pylori | Gastric MALT lymphoma |
| Borrelia burgdorferi | Cutaneous marginal zone B-cell lymphoma |
| Chlamydia psittaci | Ocular adnexal lymphoma |
Environmental Exposures
- Phenoxy herbicides (2,4-D, Agent Orange), ionizing radiation, organic solvents, nitrates in drinking water
- Heavy smoking → increased risk for follicular lymphoma
- Anti-TNF agents may increase risk (especially hepatosplenic T-cell lymphoma)
- Prior Hodgkin lymphoma treatment → ~20-fold increased NHL risk
Classification (WHO)
NHL is broadly divided into B-cell and T/NK-cell neoplasms. Key subtypes:
Indolent (Low-Grade) B-cell Lymphomas
| Subtype | Key Features |
|---|---|
| Follicular lymphoma | Most common indolent NHL; t(14;18) BCL2 translocation; waxing/waning adenopathy |
| Small lymphocytic lymphoma (SLL) | Tissue counterpart of CLL |
| Marginal zone lymphoma (MZL) | MALT (gastric, pulmonary, etc.), nodal, splenic forms |
| Lymphoplasmacytic lymphoma | Associated with hepatitis C, produces IgM (Waldenström macroglobulinemia) |
Aggressive (High-Grade) B-cell Lymphomas
| Subtype | Key Features |
|---|---|
| Diffuse large B-cell lymphoma (DLBCL) | Most common NHL overall (~30–40%); potentially curable with chemoimmunotherapy |
| Burkitt lymphoma | Extremely high proliferation rate (Ki-67 ~100%); c-MYC translocation t(8;14); "starry sky" pattern |
| Mantle cell lymphoma | t(11;14) cyclin D1 overexpression; typically aggressive |
| Primary mediastinal B-cell lymphoma | Young women; mediastinal mass |
T-cell and NK-cell Lymphomas
| Subtype | Key Features |
|---|---|
| Peripheral T-cell lymphoma (PTCL), NOS | Most common peripheral T-cell lymphoma |
| Anaplastic large cell lymphoma (ALCL) | ALK+ (better prognosis) or ALK− |
| Adult T-cell leukemia/lymphoma | HTLV-1 associated; hypercalcemia |
| Extranodal NK/T-cell lymphoma, nasal type | EBV associated; destructive midline lesions |
| Angioimmunoblastic T-cell lymphoma | Polyclonal hypergammaglobulinemia, autoimmune features |
Clinical Features
- Painless lymphadenopathy is the most common presentation (cervical, axillary, inguinal)
- Indolent lymphomas: waxing and waning nodes, often incidentally found
- Aggressive lymphomas: rapidly enlarging nodes, systemic symptoms
- B symptoms: fever >38°C, drenching night sweats, weight loss >10% body weight over 6 months
- Extranodal involvement is more common in NHL than Hodgkin lymphoma (GI tract, bone marrow, CNS, skin, liver, lung)
- Waldeyer's ring, spleen, and bone marrow are common extranodal sites
Staging (Ann Arbor/Lugano Classification)
| Stage | Description |
|---|---|
| I | Single lymph node region or single extranodal site |
| II | Two or more lymph node regions on the same side of the diaphragm |
| III | Lymph node regions on both sides of the diaphragm |
| IV | Diffuse/disseminated involvement of extranodal organs (liver, bone marrow, etc.) |
Modifiers: A = no B symptoms; B = B symptoms present; E = extranodal extension; S = spleen involvement
Diagnosis
Each new patient should be evaluated systematically:
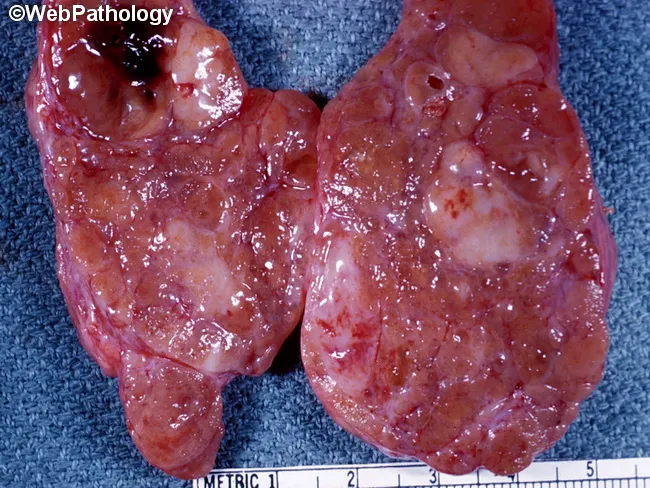
- Excisional lymph node biopsy is preferred (not fine-needle aspiration) to preserve nodal architecture
- Histopathology + immunohistochemistry (IHC): CD20, CD3, CD10, BCL2, BCL6, MYC, cyclin D1, Ki-67
- Flow cytometry for surface marker immunophenotyping
- Cytogenetics/FISH: key translocations (t(14;18), t(8;14), t(11;14))
- Molecular studies: clonality (PCR for IgH/TCR gene rearrangement)
- Staging workup: CT chest/abdomen/pelvis, PET-CT (standard for FDG-avid lymphomas), bone marrow biopsy, LDH, CBC, metabolic panel, HIV, hepatitis B/C serology
Prognostic Scoring
International Prognostic Index (IPI) — for DLBCL
One point each for:
- Age >60
- Stage III or IV
- Elevated LDH
- ECOG performance status ≥2
-
1 extranodal site
Score 0–1 = Low risk (~73% 5-year OS); Score 4–5 = High risk (~26% 5-year OS)
Follicular Lymphoma International Prognostic Index (FLIPI)
One point each for: age >60, stage III–IV, hemoglobin <12 g/dL, >4 nodal sites, elevated LDH
Treatment
Indolent NHL (e.g., Follicular Lymphoma)
- Early stage (I–II): Involved-field radiotherapy may be curative in a minority
- Advanced stage: Often "watch and wait" until symptomatic progression
- First-line chemoimmunotherapy: R-CHOP (rituximab + cyclophosphamide, doxorubicin, vincristine, prednisone) or R-bendamustine
- Rituximab maintenance after response improves PFS
- H. pylori eradication for early gastric MALT (high response rates without chemotherapy)
Aggressive NHL (e.g., DLBCL)
- R-CHOP × 6 cycles is standard first-line (potentially curative)
- CNS prophylaxis (intrathecal or high-dose methotrexate) for high-risk features
- Relapsed/refractory: Salvage chemotherapy (e.g., R-ICE, R-DHAP) → autologous stem cell transplantation (ASCT) if chemosensitive
- CAR-T cell therapy (axicabtagene ciloleucel, tisagenlecleucel) for relapsed/refractory DLBCL after ≥2 prior lines
- Polatuzumab vedotin (anti-CD79b antibody-drug conjugate) in combination for R/R disease
Burkitt Lymphoma
- Highly intensive regimens (e.g., CODOX-M/IVAC, HyperCVAD) + rituximab
- CNS prophylaxis mandatory
- Highly curable even at advanced stage with appropriate therapy
T-cell Lymphomas
- CHOP-based regimens ± etoposide (CHOEP)
- Brentuximab vedotin for CD30+ ALCL
- Pralatrexate, romidepsin, belinostat for relapsed PTCL
Special Situations
- HIV-associated lymphoma: EPOCH-R (dose-adjusted) with concurrent ART
- CNS lymphoma: High-dose methotrexate-based regimens ± rituximab; whole-brain radiotherapy reserved for salvage
Prognosis
- Depends heavily on histologic subtype, stage, and IPI score
- Indolent lymphomas: not curable with standard therapy (median survival 8–10 years) but patients can live many years
- DLBCL: curable in ~60–70% of patients with R-CHOP
- Burkitt lymphoma: curable in >80% with intensive therapy
- Mantle cell lymphoma: intermediate prognosis; median survival ~5–7 years improving with BTK inhibitors (ibrutinib, acalabrutinib)
- T-cell lymphomas: generally worse prognosis than B-cell counterparts
— Goldman-Cecil Medicine International Edition, Block 23 (Vose & Armitage)
This is a shared conversation. Sign in to Orris to start your own chat.