Squint explain
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Reading File
Finding Sources
Reading File
Now I have comprehensive information to give a thorough answer on squint (strabismus). Let me compile it.
Squint (Strabismus)
Definition
Squint, formally called strabismus, is a misalignment of the eyes in one or more visual coordinates — horizontal, vertical, or rotational — such that both eyes cannot simultaneously direct their gaze at the same point in space.
— Guyton & Hall Textbook of Medical Physiology; Kanski's Clinical Ophthalmology, 10th ed.
Types
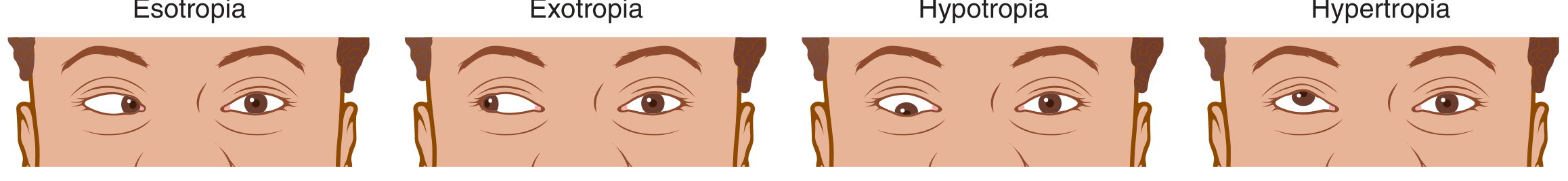
| Type | Direction of deviation |
|---|---|
| Esotropia | Eye turns inward ("cross-eyed") |
| Exotropia | Eye turns outward ("wall-eyed") |
| Hypertropia | Eye turns upward |
| Hypotropia | Eye turns downward |
When the deviation is latent (only manifest when binocular fusion is disrupted), it is called a phoria (esophoria, exophoria, etc.). When it is manifest at all times, it is a tropia.
Incomitant strabismus: the angle of deviation varies with gaze direction (usually due to muscle palsy).
Concomitant strabismus: the angle of deviation stays the same regardless of gaze direction.
Causes
Childhood onset
- Failure of development of normal binocular fusion mechanisms
- Anisometropia (difference in refractive error between the eyes) → oculomotor imbalance
- Abnormal neuronal "set" of the conjugate eye movement control pathways in early infancy
- Associated conditions: cerebral palsy, retinopathy of prematurity, prematurity/low birth weight
Adult onset
- Weakness or mechanical restriction of extraocular muscles
- Cranial nerve palsies (III, IV, VI)
- Systemic disease: diabetes mellitus, stroke, brain tumours, trauma
Sensory Consequences
When a squint develops, two troublesome perceptions arise:
- Confusion — Two different images are superimposed because separate objects stimulate corresponding retinal points (including both foveae) simultaneously.
- Pathological diplopia (double vision) — The same object stimulates non-corresponding retinal points in the two eyes, producing two images in different positions.
- In esotropia → homonymous (uncrossed) diplopia
- In exotropia → heteronymous (crossed) diplopia
Sensory adaptations (children only — up to age 6–8 years)
Due to visual cortical plasticity, children adapt by:
- Suppression — active cortical inhibition of the image from the deviating eye
- Abnormal retinal correspondence (ARC) — a new pairing between the non-foveal point of the deviated eye and the fovea of the fixating eye
Persistent unilateral suppression leads to strabismic amblyopia ("lazy eye") — reduced best-corrected visual acuity in the deviating eye with no structural pathology.
Amblyopia (Lazy Eye)
A critical complication. Types include:
- Strabismic amblyopia — from continuous monocular suppression of the deviating eye
- Anisometropic amblyopia — from blurred image in the more ametropic eye
- Stimulus deprivation amblyopia — from media opacities (cataract, ptosis)
The earlier the onset of squint in childhood, the greater the risk of amblyopia.
Motor Adaptation — Compensatory Head Posture (CHP)
Children and adults with incomitant strabismus (e.g. muscle palsy) often adopt a head posture to maintain binocular single vision (BSV) and avoid diplopia:
- Face turn — for horizontal deviations (head turns toward the field of the weak muscle)
- Head tilt — for torsional/vertical deviations (e.g. right superior oblique palsy → head tilt to the left)
- Chin elevation/depression — for elevator/depressor muscle weakness
Pseudo-squint
A large angle kappa (>5°) can simulate an exotropia when none exists. This is common in retinopathy of prematurity where macular displacement causes the corneal light reflex to appear nasally displaced, mimicking a squint.
Clinical Evaluation
History: age of onset, duration, variability (intermittent = some binocularity retained), diplopia type, family history (strabismus is frequently familial), birth history, prior spectacle/patch use.
Key principle: the later the onset of esotropia in childhood, the more likely an accommodative component (arising especially between 18–36 months).
Management Principles
| Goal | Intervention |
|---|---|
| Correct refractive error | Spectacles (especially for accommodative esotropia) |
| Treat amblyopia | Occlusion (patching) of the dominant eye; must be done during the sensitive period |
| Restore binocular alignment | Strabismus surgery (recession/resection of extraocular muscles); adjustable sutures improve outcomes |
| Non-surgical alignment | Prisms; botulinum toxin injection |
| Orthoptic exercises | For convergence insufficiency |
Organic disease must be excluded before treating amblyopia. Surgery is more likely needed the earlier the onset of the squint.
Sources: Kanski's Clinical Ophthalmology, 10th ed. | Guyton & Hall Textbook of Medical Physiology
This is a shared conversation. Sign in to Orris to start your own chat.