Stages of bone healing
Reading File
Finding Sources
Finding Sources
Reading File
Searching Images
stages of bone fracture healing callus
Loading Image
Loading Image
Reading File
Here is a comprehensive overview of the stages of bone healing, drawing from Rockwood and Green's Fractures in Adults and Bailey and Love's Short Practice of Surgery.
Types of Bone Healing
Bone heals by one of two fundamental mechanisms depending on the mechanical environment at the fracture site:
| Type | Also Called | Condition Required |
|---|---|---|
| Natural (secondary) | Indirect / callus healing | Relative stability, some interfragmentary motion |
| Primary (direct) | Contact / gap healing | Absolute stability, <0.15 mm motion, anatomic compression |
Natural (Secondary) Bone Healing — 4 Stages
This is the most common pathway, occurring with casts, intramedullary nails, external fixators, or bridging plates. It proceeds through callus formation across three overlapping phases:
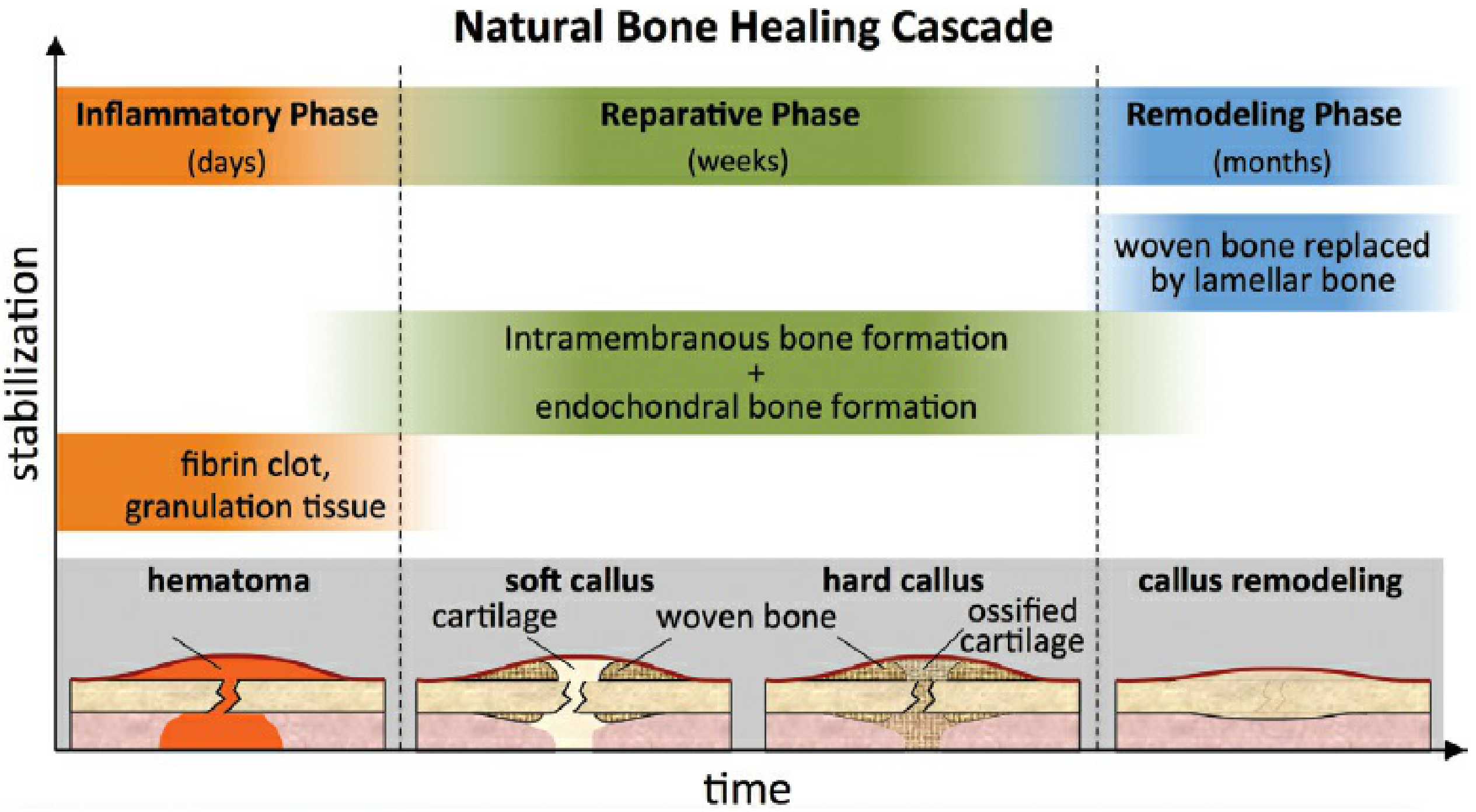
Stage 1 — Hematoma / Inflammatory Phase
(Hours to days)
- Fracture immediately fills with hematoma, which forms a fibrin clot
- Provides minimal structural stability; tolerates up to 100% strain
- Most stability at this stage comes from surrounding soft tissues
- Inflammatory mediators recruit mesenchymal stem cells and initiate repair
- Vascular disruption triggers angiogenic response
Stage 2 — Soft Callus (Reparative Phase, early)
(Days to weeks)
- Intramembranous bone formation occurs circumferentially on periosteal and endosteal surfaces proximal and distal to the fracture
- Strain near the fracture is still too high for cartilage or bone → granulation tissue deposits near the fracture first
- As granulation tissue improves stability, endochondral ossification begins: mesenchymal cells differentiate into chondrocytes, depositing cartilage across the fracture
- Soft callus is flexible, allows large deformation, tolerates 10–12.8% strain
- Provides bridging but not rigid stability
Stage 3 — Hard Callus (Reparative Phase, late)
(Weeks)
- Endochondral ossification proceeds: cartilaginous soft callus undergoes calcification
- Callus volume increases, depositing woven bone further from the neutral axis — this dramatically increases bending stiffness (stiffness increases with the 4th power of the distance from the neutral axis)
- Fracture becomes progressively more stable
- Hard callus tolerates much lower strain (ultimate tensile strength rises from ~4–19 N/mm² for soft callus to ~170 N/mm² for mature lamellar bone)
Stage 4 — Remodeling Phase
(Months to years)
- Once mechanically strong mature bone bears load, the large callus volume is no longer needed
- Woven bone is progressively replaced by lamellar bone along lines of mechanical stress (Wolff's Law)
- Medullary canal is restored; excess callus is resorbed by osteoclasts
- Original bone architecture is eventually recreated
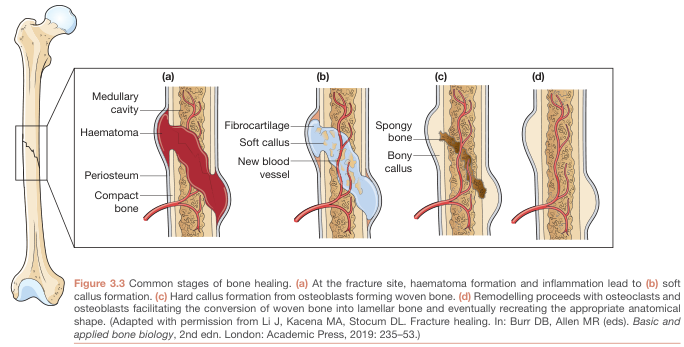
Tissue Properties at Each Stage
| Tissue | Maximum Strain (%) | Ultimate Tensile Strength (N/mm²) |
|---|---|---|
| Hematoma | 100 | 0.1 |
| Granulation tissue / soft callus | 10–12.8 | 4–19 |
| Hard callus (woven bone) | ~2 | ~70 |
| Mature lamellar bone | ~1–2 | ~170 |
— Rockwood and Green's Fractures in Adults, 10th ed.
Primary (Direct) Bone Healing
When fracture ends are compressed with absolute stability (e.g., compression plating with <2–5% interfragmentary strain):
- No callus forms — osteoclast cutting cones cross directly between fracture surfaces
- Contact healing: cutting cones bore across the fracture, followed by osteoblast bone deposition
- Gap healing: in small residual gaps, lamellar bone forms perpendicular to the long axis, then is remodeled longitudinally
- Skips intermediate tissue stages — proceeds directly to remodeling
- Paradoxically slower than callus healing; radiographically healed bone may still fail at the fracture site at 48 weeks
- Plate removal should be delayed up to 2 years to avoid refracture
Key Modulators of Bone Healing
- Mechanical: fracture geometry, interfragmentary motion, fixation stiffness
- Biological: blood supply, periosteal integrity, growth factors (BMP, VEGF, TGF-β)
- Systemic: age, smoking, diabetes, NSAIDs (impair prostaglandin-mediated inflammation), corticosteroids, nutrition (calcium, vitamin D, phosphate)
- Local: open fractures, bone loss, infection, soft tissue damage
This is a shared conversation. Sign in to Orris to start your own chat.