Give me detail explanation of this pic related to step 1 usmle exam With high yeild points related to mcqs step 1
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
I now have rich content from authoritative textbooks. Let me compile a comprehensive, high-yield USMLE Step 1 breakdown of everything in that image.
🧠 GI Intestinal Disorders — USMLE Step 1 High-Yield Breakdown
This page from First Aid for the USMLE Step 1 (Section III: Gastrointestinal) covers Volvulus and several Other Intestinal Disorders. Here is a detailed, exam-focused explanation of each.
1. VOLVULUS
What it is
Twisting of a bowel segment around its mesentery → leads to obstruction and potentially infarction due to vascular compromise.
Two Types (HIGH-YIELD)
| Feature | Midgut Volvulus | Sigmoid Volvulus |
|---|---|---|
| Population | Infants & children (minors) | Elderly (seniors) |
| Cause | Malrotation of gut during development | Long, redundant sigmoid colon |
| X-ray finding | Barium shows "corkscrew" appearance | "Coffee bean sign" — massively dilated loop pointing to RUQ |
| Complication | Bowel necrosis/infarction | Obstruction, necrosis |
High-Yield MCQ Points
- Midgut volvulus → due to intestinal malrotation (failure of 270° counterclockwise rotation during fetal development) → Ladd's bands may compress duodenum
- Sigmoid volvulus → most common in elderly, institutionalized, or chronic constipation patients; also associated with Chagas disease (megacolon)
- Coffee bean sign on plain X-ray = classic for sigmoid volvulus ← MCQ favorite
- Treatment: Sigmoid volvulus → endoscopic decompression (flexible sigmoidoscopy); Midgut → surgical (Ladd procedure)
2. ACUTE MESENTERIC ISCHEMIA
What it is
Critical blockage of intestinal blood flow → ischemia and necrosis of bowel. Most often embolic occlusion of the Superior Mesenteric Artery (SMA).
Causes (HIGH-YIELD)
| Cause | % |
|---|---|
| Arterial embolism (SMA) — e.g., from Afib | ~50% |
| Arterial thrombosis (atherosclerosis) | ~25–30% |
| Nonocclusive (low-flow states, vasoconstrictors) | ~20% |
| Mesenteric venous thrombosis (hypercoagulable states) | <10% |
Classic Presentation (MCQ trigger)
"Pain out of proportion to physical exam findings" — the hallmark
- Severe periumbilical/diffuse abdominal pain
- "Red currant jelly" stools = late sign of bowel necrosis (bloody mucus)
- CT angiography = best initial study
- X-ray: gasless abdomen or adynamic ileus pattern early on; later pneumatosis intestinalis or portal venous gas (ominous)
High-Yield Associations
- Source of embolus → atrial fibrillation (#1 cardiac source for SMA embolus)
- Nonocclusive ischemia → digoxin, vasopressors, cocaine (vasoconstrictors)
- Mesenteric venous thrombosis → hypercoagulable states: Factor V Leiden, protein C/S deficiency, antiphospholipid syndrome, OCP use
- Mortality remains 50–80% → early diagnosis critical
3. ADHESION
What it is
Fibrous bands of scar tissue forming after abdominal surgery → most common cause of small bowel obstruction (SBO) in adults.
High-Yield MCQ Points
- #1 cause of SBO in adults = adhesions (post-surgical)
- X-ray: multiple dilated small bowel loops with air-fluid levels; look for arrows in the textbook image (image B in the page)
- No transition zone visible (vs. mechanical obstruction which often has one)
- Other causes of SBO: hernias (#2), Crohn's disease, intussusception (in children)
- Management: NPO, NG tube decompression; surgery if no improvement
4. ANGIODYSPLASIA
What it is
Tortuous dilation (ectasia) of submucosal and mucosal vessels → arteriovenous communications in the GI wall.
Key Features (HIGH-YIELD)
- Location: Cecum and right colon (#1 site) — because the cecum has the largest diameter → highest wall tension → chronic venous obstruction
- Age: Elderly (>60 years) — most common cause of significant lower GI bleeding in the elderly
- Presentation: Hematochezia (bright red blood per rectum), often painless; may be chronic/intermittent or acute/massive
- Diagnosis: Angiography (gold standard, can also treat) or colonoscopy
- Associated conditions: von Willebrand disease, aortic stenosis (Heyde syndrome: AS + angiodysplasia + bleeding due to vWF destruction), end-stage renal disease
High-Yield MCQ Points
- Elderly patient + right-sided painless lower GI bleed → think angiodysplasia
- Heyde syndrome = aortic stenosis + angiodysplasia bleeding → due to loss of high-molecular-weight vWF multimers by high shear stress across stenotic valve
- Confirmed by angiography; treated by endoscopic coagulation or angiographic embolization
5. CHRONIC MESENTERIC ISCHEMIA ("Intestinal Angina")
What it is
Atherosclerotic narrowing of celiac artery, SMA, or IMA → inadequate postprandial blood flow → "intestinal angina."
Classic Triad (MCQ)
- Postprandial epigastric pain (30–60 min after eating)
- Food aversion (sitophobia) — patient avoids eating due to pain
- Weight loss
High-Yield Points
- Caused by atherosclerosis (same risk factors: smoking, DM, HTN, hyperlipidemia)
- Requires ≥2 of 3 mesenteric vessels to be significantly stenosed (due to rich collaterals)
- Diagnosis: CT angiography or Doppler US of mesenteric vessels
- Treatment: Revascularization (endovascular stenting preferred)
6. COLONIC ISCHEMIA
What it is
Most common form of intestinal ischemia; crampy abdominal pain + hematochezia; typically in elderly.
Key Features
- Affects watershed areas — sites with least collateral blood flow:
- Splenic flexure (junction of SMA and IMA territories) — "Griffiths' point"
- Rectosigmoid junction — "Sudeck's point"
- Thumbprint sign on imaging = mucosal edema/hemorrhage (submucosal hemorrhage pushes mucosa inward) ← classic MCQ
- Self-limiting in most cases; severe cases → transmural infarction, perforation
High-Yield MCQ Triggers
- Post aortic aneurysm repair (IMA ligation) → highest risk for colonic ischemia
- Thumbprint sign = hallmark imaging finding
- Does NOT require arterial occlusion — low-flow states sufficient
7. ILEUS (Paralytic Ileus)
What it is
Intestinal hypomotility WITHOUT mechanical obstruction → bowel stops moving.
Presentation
- Constipation, ↓ flatus
- Distended, tympanic abdomen
- ↓ or absent bowel sounds
- No transition zone on imaging (differentiates from mechanical obstruction)
Causes (HIGH-YIELD)
| Category | Examples |
|---|---|
| Post-surgical | Abdominal surgery (most common) |
| Metabolic | Hypokalemia (K⁺ required for smooth muscle function) |
| Medications | Opiates, anticholinergics |
| Systemic illness | Sepsis, peritonitis |
Treatment
- Bowel rest, NPO
- Correct electrolytes (especially K⁺)
- Cholinergic drugs (neostigmine — for Ogilvie syndrome/acute colonic pseudo-obstruction)
- Minimize opiates
MCQ Pearl
- Hypokalemia → ileus → look for this in patients on diuretics, vomiting, or diarrhea
- Neostigmine (cholinesterase inhibitor) stimulates intestinal motility in severe ileus/Ogilvie syndrome
8. MECONIUM ILEUS
What it is
Thick, inspissated (dried) meconium obstructs the terminal ileum at birth → neonate fails to pass first stool.
HIGH-YIELD Association
Meconium ileus = Cystic Fibrosis until proven otherwise
- CF → CFTR dysfunction → thick, viscous secretions → abnormally thick meconium obstructs bowel
- Presents at birth with bilious vomiting, abdominal distension, failure to pass meconium
- X-ray: "soap-bubble" appearance in RLQ (meconium + air)
- Treatment: Gastrografin enema (hyperosmotic — draws fluid to loosen meconium) or surgery
9. NECROTIZING ENTEROCOLITIS (NEC)
What it is
Acute ischemic necrosis of intestinal mucosa (most commonly terminal ileum and proximal colon) → most common acquired GI emergency in neonates.
HIGH-YIELD Risk Factors
| Factor | Detail |
|---|---|
| Prematurity | #1 risk factor |
| Formula feeding (not breastfed) | Breast milk is protective |
| Immature immune system | Can't handle bacterial translocation |
| Low birth weight |
Classic Findings (MCQ)
- Pneumatosis intestinalis (gas in bowel wall) — pathognomonic on X-ray → seen as arrows in image D on the page
- Portal venous gas — ominous sign
- Pneumoperitoneum if perforation occurs
- Bloody stools, abdominal distension, feeding intolerance, bilious vomiting
Treatment
- Medical: NPO, IV antibiotics, NG decompression
- Surgical: if perforation or failure → bowel resection
MCQ Pearl
- Breast milk is protective against NEC
- NEC → can lead to short bowel syndrome (long-term complication after bowel resection)
- Pathology: transmural necrosis of bowel wall
🔑 RAPID-FIRE MCQ Summary Table
| Condition | Classic Buzzword | Population | Key Association |
|---|---|---|---|
| Midgut volvulus | Malrotation | Infant | Ladd's procedure |
| Sigmoid volvulus | Coffee bean sign on X-ray | Elderly | Chagas, constipation |
| Acute mesenteric ischemia | Pain out of proportion | Adults | Afib → SMA embolus |
| Adhesion | #1 cause of SBO in adults | Post-surgical | Dilated small bowel loops |
| Angiodysplasia | Painless lower GI bleed | Elderly | Heyde syndrome (AS + vWF) |
| Chronic mesenteric ischemia | Food aversion + weight loss | Atherosclerotic adults | Postprandial pain |
| Colonic ischemia | Thumbprint sign | Elderly | Watershed areas; post-AAA repair |
| Ileus | No bowel sounds, no transition zone | Post-op, hypokalemia | Opiates, sepsis |
| Meconium ileus | Failure to pass meconium | Newborn | Cystic fibrosis |
| NEC | Pneumatosis intestinalis | Premature, formula-fed neonate | Breast milk protective |
Sources: Robbins & Kumar Pathologic Basis of Disease; Harrison's Principles of Internal Medicine 22E; Sleisenger and Fordtran's Gastrointestinal and Liver Disease; Schwartz's Principles of Surgery
Ludwig angina
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a complete, high-yield breakdown of Ludwig Angina for USMLE Step 1:
Ludwig Angina — Complete High-Yield Review
Definition
Ludwig angina is a rapidly progressive, bilateral gangrenous cellulitis of the submandibular space (sublingual + submylohyoid/submaxillary spaces), subdivided by the mylohyoid muscle. It is NOT a true abscess — it is a diffuse brawny cellulitis with potential for fatal airway obstruction within hours.
Key anatomical concept: The submandibular space extends from the floor of the mouth to muscular attachments at the hyoid bone. It is bilateral because both sides communicate freely at the posterior aspect.
Anatomy — Why Molars Are the #1 Source
- Roots of mandibular molars (2nd and 3rd) insert below the mylohyoid line
- Infection tracks through the thin lingual cortex of the mandible → directly into the submandibular space
- This bypasses normal lymphatic drainage → spreads rapidly via fascial planes (NOT lymphatics — high-yield distinction!)
Etiology & Risk Factors
| Cause | Details |
|---|---|
| Odontogenic (#1) | Periapical abscess of mandibular molars (especially 2nd/3rd molars) — accounts for ~80% |
| Mandibular fracture | |
| Oral trauma | Tongue piercing, lingual laceration, intubation injury |
| Secondary infection | Oral malignancy, suppurative parotitis |
| Adjacent head/neck infections |
Risk factors for severe disease:
- Diabetes mellitus — impaired neutrophil function
- Immunocompromised (HIV, steroids, chemotherapy)
- Poor dental hygiene
Microbiology (HIGH-YIELD)
- Polymicrobial — mixed oral flora
- Organisms: Streptococcus viridans (most common), Staphylococcus, anaerobes (Peptostreptococcus, Bacteroides, Fusobacterium)
- The polymicrobial/anaerobic nature explains the gangrenous, non-fluctuant character (gas-producing organisms)
Pathophysiology & Spread
Dental root infection → periapical abscess
↓
Penetrates lingual cortex of mandible
↓
Enters submandibular space (bilateral communication)
↓
Spreads via fascial planes (NOT lymphatics)
↓
Posterior spread → parapharyngeal space (via styloglossus muscle)
↓
Deep neck infection → mediastinitis (descending necrotizing mediastinitis)
↓
AIRWAY OBSTRUCTION / SEPSIS / DEATH
Clinical Features
Classic Presentation (MCQ Buzzwords)
- "Bull neck" — tense, brawny, indurated edema from submandibular region to hyoid
- Woody, indurated floor of mouth (not fluctuant — not a true abscess)
- Tongue displacement — posteriorly and superiorly (→ airway obstruction)
- Drooling + dysphagia + odynophagia
- Trismus — limited mouth opening due to masticator space involvement
- Muffled/hot potato voice
- Fever, tachycardia, toxic appearance
- No palpable lymphadenopathy and no fluctuance (distinguishes it from abscess)
"Sniffing position" (MCQ)
Children (and adults) lean forward in "sniffing position" to maximize airway diameter — same as epiglottitis
CT Scan Findings
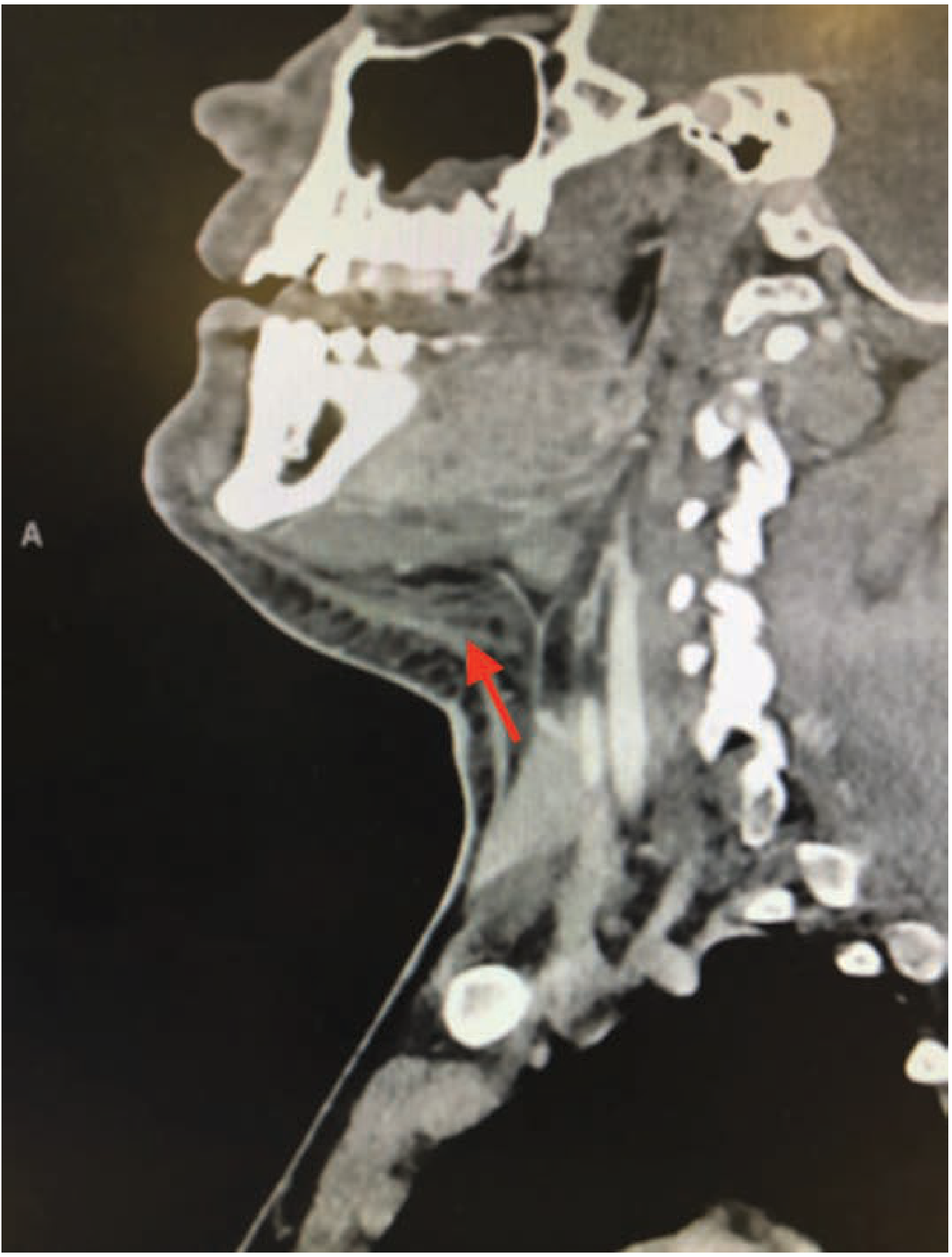
Sagittal CT scan showing soft tissue stranding and inflammation in the submandibular space (arrow) — Tintinalli's Emergency Medicine
- Contrast-enhanced CT is the imaging of choice
- Shows: soft tissue stranding, thickening, gas within fascial planes (gas = anaerobic organisms), extent of spread
- Helps guide surgical drainage planning
Diagnosis
- Clinical diagnosis — based on history and exam findings
- CT scan confirms extent and identifies drainable collections
- No fluctuance = no simple abscess to drain
Management (HIGH-YIELD Algorithm)
⚠️ AIRWAY FIRST — Always
| Step | Action |
|---|---|
| 1. Airway | Most critical — asphyxia is the #1 cause of death |
| 2. Intubation method | Awake fiberoptic nasal intubation preferred (due to trismus and distorted anatomy) |
| 3. If fiberoptic fails | Surgical airway (tracheotomy/cricothyrotomy) — difficult due to anterior neck edema |
| 4. IV Antibiotics | Immediate, broad-spectrum with anaerobic coverage |
| 5. Surgery | Infected tooth extraction, debridement of necrotic tissue, drainage of purulent collections |
| 6. Disposition | ICU admission |
Antibiotic Regimens (HIGH-YIELD)
| Agent | Coverage |
|---|---|
| Ampicillin-sulbactam | Aerobic + anaerobic gram-positive cocci + gram-negative bacilli (1st line) |
| Penicillin G + metronidazole | Alternative |
| Clindamycin | Alternative; excellent anaerobic coverage |
| Add vancomycin | If MRSA risk (community-acquired MRSA) |
Complications
| Complication | Mechanism |
|---|---|
| Airway obstruction / asphyxia | #1 cause of death — tongue displacement, edema |
| Descending necrotizing mediastinitis | Spread via retropharyngeal/parapharyngeal space → mediastinum |
| Septicemia / septic shock | Bacteremia from polymicrobial infection |
| Cavernous sinus thrombosis | Retrograde spread via valveless ophthalmic veins |
| Aspiration pneumonia | From drooling/inability to manage secretions |
| Jugular vein thrombosis | Lemierre syndrome (Fusobacterium necrophorum) |
🔑 Rapid-Fire High-Yield MCQ Points
| Point | Detail |
|---|---|
| #1 cause | Odontogenic — mandibular molar periapical abscess |
| Spaces involved | Bilateral sublingual + submylohyoid (submaxillary) = entire submandibular space |
| Spread mechanism | Fascial planes — NOT lymphatics |
| Character | Brawny woody cellulitis — NOT a fluctuant abscess |
| Key exam finding | Bull neck + tongue displacement + trismus + NO fluctuance |
| #1 cause of death | Asphyxia (airway obstruction) |
| Airway management | Awake fiberoptic nasal intubation (trismus prevents oral intubation) |
| Organisms | Polymicrobial — viridans Strep + anaerobes |
| Antibiotic of choice | Ampicillin-sulbactam (anaerobic coverage mandatory) |
| Risk factors | Diabetes, immunocompromised |
| Imaging | Contrast CT neck |
| Disposition | ICU |
| Deadly complication | Descending necrotizing mediastinitis |
Comparison with Similar Deep Space Infections (MCQ Differentiator)
| Feature | Ludwig Angina | Peritonsillar Abscess | Retropharyngeal Abscess |
|---|---|---|---|
| Location | Submandibular space (bilateral) | Peritonsillar space (unilateral) | Retropharyngeal space |
| Fluctuance | Absent | Present | Present |
| Trismus | Yes | Yes (common) | Less common |
| Uvula deviation | No | Yes (to opposite side) | No |
| Age | Adults (dental) | Adolescents/young adults | Children <5 yrs |
| Source | Mandibular molars | Tonsillitis | URI / lymphadenitis |
| Airway risk | Extremely high | Moderate | High |
Sources: Rosen's Emergency Medicine 9e; Tintinalli's Emergency Medicine; K.J. Lee's Essential Otolaryngology; Miller's Anesthesia 10e
Give me detail explanation of this pic related to step 1 usmle exam With high yeild points related to mcqs
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
This is a shared conversation. Sign in to Orris to start your own chat.