Prosthetic eye types
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Here is a structured overview of prosthetic eye types, drawn from Kanski's Clinical Ophthalmology and Cummings Otolaryngology.
Prosthetic Eye Types
Context: Why a Prosthesis is Needed
After enucleation (removal of the entire globe) or evisceration (removal of intraocular contents with sclera retained), the orbit requires both volume replacement and a cosmetically matched surface shell. These are two separate components:
- Orbital implant — replaces lost orbital volume (sits deep in the socket, not visible)
- Ocular prosthesis — the painted shell placed over the implant that faces the outside world
1. Conformer (Temporary Device)
- Placed immediately after enucleation/evisceration to maintain the conjunctival fornices
- Made of silicone or acrylic (PMMA)
- Remains in place until a fitted prosthesis is ready (typically 6–8 weeks postoperatively)
- Not cosmetically painted — purely a structural spacer
2. Stock (Pre-fabricated) Prosthetic Eye
- Mass-produced in standard sizes and iris colours
- Used as a temporary artificial eye while a custom prosthesis is being manufactured
- Less cosmetically accurate but immediately available
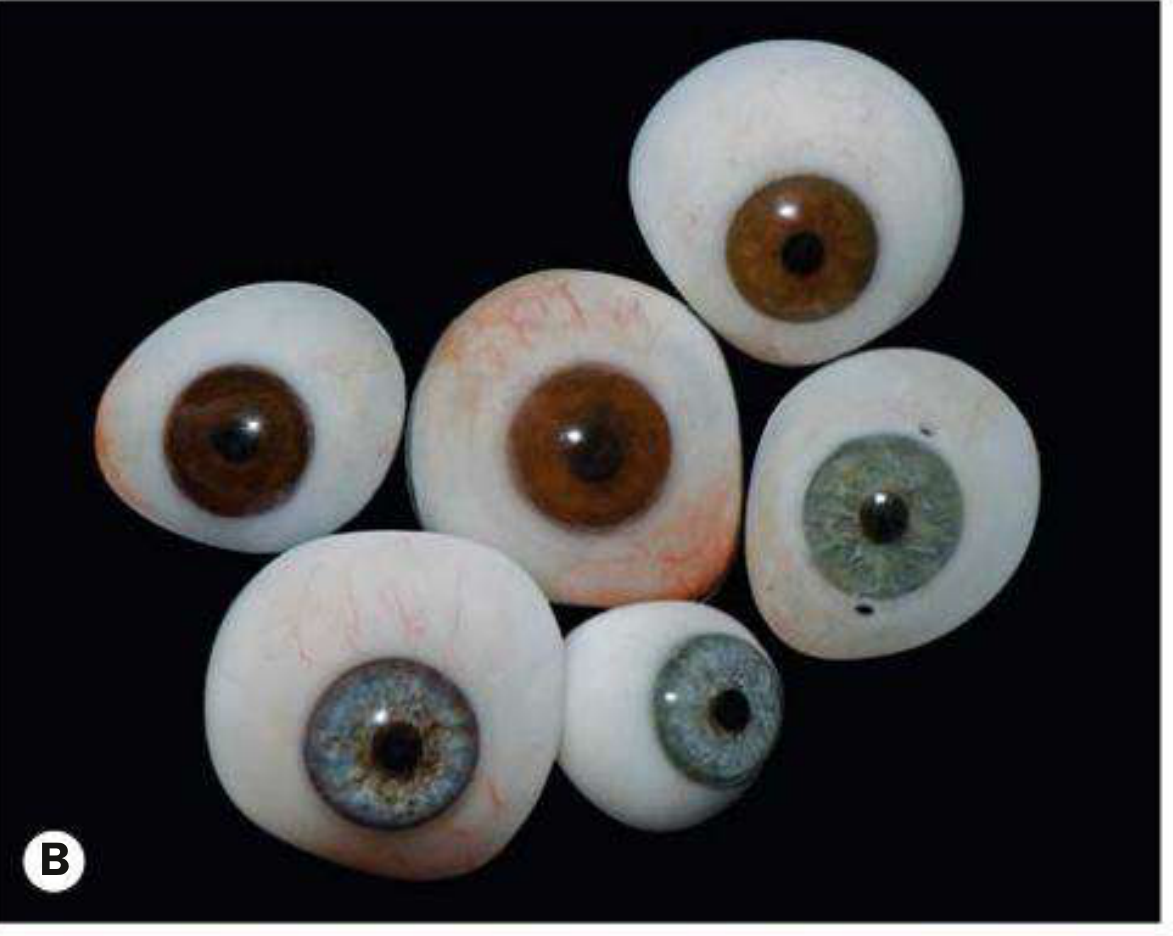
3. Custom Acrylic (PMMA) Prosthetic Eye
- Polymethylmethacrylate (PMMA) — the dominant material for modern ocular prostheses
- Individually cast from an impression of the patient's socket
- Painted by an ocularist to match the iris colour, limbal ring, and conjunctival vasculature of the fellow eye
- Lightweight, durable, polishable
- The most widely used type in clinical practice
4. Glass Eye (Historical)
- Traditionally made from cryolite glass (a sodium aluminium fluoride compound)
- Lightweight and with a natural surface sheen
- Fragile, prone to breakage and surface degradation
- Largely replaced by acrylic in most countries, though still manufactured by specialist glassblowers (notably in Germany and the UK)
5. Orbital Implants (Supporting the Prosthesis)
These sit beneath the conjunctiva and are not directly visible, but they determine prosthetic motility:
| Type | Material | Properties |
|---|---|---|
| Non-integrated (solid) | Silicone, acrylic | No fibrovascular ingrowth; simpler; lower cost |
| Integrated (porous) | Hydroxyapatite, porous polyethylene (Medpor) | Fibrovascular ingrowth occurs; improves motility of the overlying prosthesis |
A peg can be inserted into porous implants after vascularisation to further couple implant movement to the prosthesis, though it cannot attach directly — the peg must be covered by socket tissue.
Extrusion is a risk with all implant types. Deep, well-vascularised placement is more important than material choice. — Kanski's Clinical Ophthalmology, p. 168–169
6. Orbital Prosthesis (for Exenterated Sockets)
Used after orbital exenteration (removal of the entire orbital contents including eyelids), where a simple ocular shell is insufficient:
- A full orbital prosthesis is fabricated from silicone, incorporating:
- A PMMA ocular component (painted to match the contralateral eye)
- Sculpted eyelids and surrounding periorbital tissue
- Eyelashes (and sometimes an eyebrow)
- May be retained by adhesive or attached to spectacles frames
- Orientation of the ocular component is calibrated to match the gaze direction of the remaining eye using light reflection and rulers
Complications Common to All Prosthetic Eyes
- Giant papillary conjunctivitis (GPC) — from chronic mechanical irritation of the tarsal conjunctiva
- Post-enucleation socket syndrome (PESS) — upper lid ptosis, superior sulcus hollowing, enophthalmos, sagging lower lid; results from orbital volume deficit, especially without an implant
- Implant extrusion — most feared implant complication
Summary table:
| Type | Material | Use |
|---|---|---|
| Conformer | Silicone / acrylic | Immediate post-op socket maintenance |
| Stock prosthesis | PMMA | Temporary, off-the-shelf |
| Custom prosthesis | PMMA (painted) | Definitive, individually fitted |
| Glass eye | Cryolite glass | Historical; still available |
| Orbital prosthesis | Silicone + PMMA ocular component | Post-exenteration |
| Non-integrated implant | Silicone / acrylic | Volume replacement, simple |
| Integrated implant | Hydroxyapatite / porous polyethylene | Volume + improved motility |
— Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed., pp. 167–169; Cummings Otolaryngology Head and Neck Surgery
This is a shared conversation. Sign in to Orris to start your own chat.