Complications of fracture dislocation and their ED management
You are a medical research assistant. Your task is to gather comprehensive textbook content on "complications of fracture dislocation and their ED (Emergency Department) management" from the available medical library. Use the query_library_db tool to search, then read_file to retrieve relevant content. Key books available: - ROSEN's Emergency Medicine: isbn 9780323757898 - Tintinalli's Emergency Medicine: isbn 9781260019933 - Rockwood and Green's fractures in adults: isbn 9781975211608 - Roberts and Hedges' Clinical Procedures in Emergency: isbn 9780323354783 Steps to follow: 1. Search headings_fts for relevant sections on fracture dislocation complications and ED management: ```sql SELECT title, book_title, '/textbooks/' || block_file_path AS file_path, line_number, para_line_ranges, para_count FROM headings_fts WHERE headings_fts MATCH 'fracture dislocation' ORDER BY rank LIMIT 15 ``` 2. Search paragraphs_fts for content on complications: ```sql SELECT book_title, section_heading, '/textbooks/' || block_file_path AS file_path, line_start, line_end, snippet(paragraphs_fts, 0, '>>>', '<<<', '...', 30) AS snippet FROM paragraphs_fts WHERE paragraphs_fts MATCH '"fracture dislocation" AND (complication OR neurovascular OR vascular OR nerve)' ORDER BY rank LIMIT 10 ``` 3. Search paragraphs_fts for ED management approach: ```sql SELECT book_title, section_heading, '/textbooks/' || block_file_path AS file_path, line_start, line_end, snippet(paragraphs_fts, 0, '>>>', '<<<', '...', 30) AS snippet FROM paragraphs_fts WHERE paragraphs_fts MATCH '"fracture dislocation" AND (reduction OR immobilization OR splint OR emergency)' ORDER BY rank LIMIT 10 ``` 4. Search for complications of dislocation generally in Rosen's Emergency Medicine: ```sql SELECT title, book_title, '/textbooks/' || block_file_path AS file_path, line_number, para_line_ranges, para_count FROM headings_fts WHERE headings_fts MATCH 'dislocation complication emergency' ORDER BY rank LIMIT 10 ``` 5. Read relevant sections from Rosen's Emergency Medicine around dislocation complications (file: /textbooks/9780323757898/9780323757898_block7.md, starting around the Anterior Dislocations section which was at line 1036): - read_file(file_path="/textbooks/9780323757898/9780323757898_block7.md", offset=990, limit=250) 6. Search for general fracture complications: ```sql SELECT book_title, section_heading, '/textbooks/' || block_file_path AS file_path, line_start, line_end, snippet(paragraphs_fts, 0, '>>>', '<<<', '...', 30) AS snippet FROM paragraphs_fts WHERE paragraphs_fts MATCH 'fracture complication AND (compartment syndrome OR avascular necrosis OR nerve injury OR vascular injury OR malunion OR nonunion)' ORDER BY rank LIMIT 10 ``` 7. Read the Tintinalli TOC for fracture/dislocation sections: ```sql SELECT heading, block_file_path, line_number, level FROM v_toc WHERE book_isbn = '9781260019933' AND (heading LIKE '%fracture%' OR heading LIKE '%dislocation%' OR heading LIKE '%Fracture%' OR heading LIKE '%Dislocation%') LIMIT 20 ``` 8. Based on the results above, read the most relevant sections from the textbooks (up to 3 read_file calls, 250 lines each). Please return a COMPREHENSIVE synthesis of all findings covering: A. General complications of fracture-dislocations (immediate, early, late) B. Specific complications by region/type where available (shoulder, hip, elbow, spine, etc.) C. ED assessment and management principles D. Neurovascular assessment and monitoring E. Indications for emergency reduction and surgical referral F. Any relevant images or diagrams found Include exact file paths and line numbers where content was found so the main agent can follow up if needed.
Complications of Fracture-Dislocation and Their ED Management
Overview
General Complications
1. Neurovascular Injuries (Immediate)
- Axillary nerve injury — most common nerve injured in anterior glenohumeral dislocation; occurs in <10% of cases. Usually neuropraxic; expectant management with good prognosis for recovery.
- Axillary artery injury — less common but limb-threatening; suggested by expanding hematoma, absent distal pulses, or signs of ischemia. Requires urgent vascular surgery consultation.
- Brachial plexus injury — can accompany shoulder dislocations, particularly in high-energy trauma.
- Radial nerve — at risk in humeral shaft fractures, particularly with Holstein-Lewis fractures.
- Sciatic nerve / femoral vessels — at risk in hip dislocations.
- Popliteal artery — at high risk in knee dislocations (up to 40% incidence in some reports).
2. Associated Fractures (Immediate)
- Greater tuberosity fracture with anterior shoulder dislocation — changes the risk profile; associated with decreased recurrence risk. Reduces with the shoulder in many cases; persistent >5 mm displacement after reduction requires surgical fixation.
- Hill-Sachs deformity — impaction fracture of the posterolateral humeral head from the anterior glenoid rim; increases recurrence risk.
- Bankart lesion — avulsion of the anteroinferior glenoid labrum (bony or soft-tissue); primary cause of recurrent instability.
- Glenoid rim fracture — increases recurrence risk.
- Proximal humerus fractures — fracture-dislocations of the shoulder (2-, 3-, 4-part) involve simultaneous fracture and displacement; these are surgical emergencies if vascular supply to the humeral head is compromised.
3. Compartment Syndrome (Early, within hours)
- Can occur after any significant limb fracture or crush injury.
- Classical signs: Pain out of proportion, pain with passive stretch, tight/woody compartment, paresthesias, paralysis (late).
- ED management: Remove all constrictive bandaging/splints; measure compartment pressure. Compartment pressure >30 mmHg (or within 30 mmHg of diastolic BP) → emergency fasciotomy.
- Do not wait for all 5 P's (pulselessness is a late sign).
4. Vascular Injury (Immediate/Early)
- Posterior knee dislocation carries the highest risk of popliteal artery injury of any dislocation.
- Hip dislocation can injure the femoral vessels.
- Signs: Limb pallor, mottling, absent pulses, expanding hematoma, bruit/thrill.
- ED management: Immediate reduction to relieve vascular compression; CT angiography or surgical exploration. Vascular surgery consultation.
5. Recurrent Dislocation (Late)
- Strongly associated with young age and specific structural injuries (Hill-Sachs, Bankart, glenoid rim fracture).
- In anterior shoulder dislocation: recurrence rate 79–100% in patients <30 years; rates decline with increasing age.
- Presence of a greater tuberosity fracture is paradoxically protective against recurrence.
- ED management: Treat the acute episode; orthopedic referral for definitive stabilization (Bankart repair in young athletes).
6. Rotator Cuff Tears (Early/Late)
- Especially common after primary shoulder dislocation in patients >40 years (increases to 80% in patients >60 years).
- Supraspinatus tears mimic axillary nerve injury (both cause failure to abduct).
- ED management: Clinical suspicion; arrange MRI/ultrasound as outpatient. Orthopedic referral.
7. Avascular Necrosis (Late)
- Disruption of blood supply to articular bone.
- Most significant with: femoral head (posterior hip dislocation), humeral head (4-part fracture-dislocations), talus (subtalar dislocation).
- Incidence in posterior hip dislocation increases with delay to reduction: <6 hours → much lower risk; >6 hours → significantly higher risk (~20–50%).
- ED management: Prompt reduction is the most critical intervention to reduce AVN risk.
8. Malunion / Nonunion (Late)
- Result of inadequate reduction or fixation.
- Not an acute ED concern but should inform the urgency of orthopedic referral.
9. Post-traumatic Arthritis (Late)
- Cartilage damage at the time of injury, or from imperfect reduction, predisposes to degenerative arthritis.
- Not manageable in the ED; discussed with patients during follow-up.
Specific Fracture-Dislocations and ED Management
Shoulder (Glenohumeral) Fracture-Dislocation
- Axillary nerve injury (<10%)
- Axillary artery injury
- Rotator cuff tear (very common in elderly)
- Hill-Sachs deformity, Bankart lesion
- Greater tuberosity fracture (present in ~15–35%)
- Classic "squared-off" shoulder, arm held in abduction
- AP + trans-scapular Y + axillary lateral radiographs
- Pre-reduction neurovascular exam (axillary nerve: sensation over deltoid; axillary artery: radial pulse)
- Analgesia — IV opioids ± procedural sedation (propofol, ketamine, midazolam + fentanyl) or intra-articular lidocaine (10–20 mL of 1% lidocaine).
- Closed reduction — multiple techniques:
- Cunningham technique — patient seated, massages own muscle; no analgesia required
- Stimson technique — prone positioning with weights
- External rotation method — gentle ER with elbow at 90°
- Milch technique — arm elevated with traction
- Traction-countertraction — most common but requires sedation
- Post-reduction: Repeat X-ray (confirm reduction, identify occult fracture). Repeat neurovascular exam.
- Immobilization: Sling for 1–4 weeks depending on age.
- Disposition: Orthopedic follow-up in 1–2 weeks. Young athletes need Bankart evaluation. Associated greater tuberosity fracture with >5 mm post-reduction displacement → urgent orthopedic referral.
"Rotator cuff tears are especially common in primary dislocations in patients older than 40 years old, increasing to 80% in patients over 60 years old." — Rosen's Emergency Medicine, p. 654
Hip Fracture-Dislocation
- Sciatic nerve injury (~10–15%) — foot drop; assess prior to reduction
- Avascular necrosis of femoral head — risk rises sharply after 6 hours
- Femoral head fracture (Pipkin classification)
- Acetabular fracture — if large posterior wall fragment, joint unstable after reduction
- IV analgesia + procedural sedation (this is a major joint requiring significant force or relaxation).
- Allis maneuver (most common): Patient supine, hip and knee flexed to 90°, inline traction with countertraction on pelvis.
- Stimson gravity technique (alternative): Prone, hip at table edge, downward pressure.
- Post-reduction: CT scan to check concentric reduction and identify loose bodies or acetabular/femoral head fractures.
- CRITICAL: Reduction within 6 hours to minimize AVN risk.
- Disposition: Hospital admission. Orthopedic surgery for all hip fracture-dislocations.
Elbow Fracture-Dislocation
- "Terrible Triad" — posterior elbow dislocation + radial head fracture + coronoid fracture. Highly unstable; high complication rate.
- Posterior Monteggia — ulna fracture + radial head dislocation.
- Trans-olecranon fracture-dislocation — very unstable.
- Brachial artery injury — must check radial pulse before and after reduction
- Median nerve injury
- Ulnar nerve injury
- Heterotopic ossification (late)
- Stiffness / loss of range of motion (very common)
- Complex fracture-dislocations (Terrible Triad) have high re-dislocation rates with closed management alone
- Neurovascular exam: Brachial and radial pulses, median/radial/ulnar nerve function.
- X-rays: AP and lateral elbow (assess for radial head, coronoid, olecranon fractures).
- Reduction of simple elbow dislocation: Supinate forearm → traction on wrist, countertraction on distal humerus → flex elbow while pushing olecranon anteriorly. Requires procedural sedation.
- Post-reduction: Check stability in full range of motion. Obtain X-ray.
- Terrible Triad / complex fracture-dislocations → operative management (cannot be managed conservatively in ED). Urgent orthopedic consultation.
- Immobilization: Posterior splint at 90° of flexion for simple dislocations.
"Obesity and complex fracture-dislocations around the elbow can make closed management very challenging." — Rockwood & Green's, block8
Ankle Fracture-Dislocation
- Skin necrosis/pressure injury from displaced talus (may occur within 1–2 hours)
- Peroneal/tibial nerve injury
- Vascular compromise (posterior tibial artery)
- Open fracture (bone may tent or pierce skin)
- Immediate reduction — do not wait for formal imaging if skin is compromised/blanched. Reduce first, X-ray after.
- Technique: Traction + foot manipulation while countertraction on lower leg.
- Short posterior splint/plaster backslab with U-slab.
- Neurovascular recheck post-reduction.
- Orthopedic admission for all fracture-dislocations of the ankle.
Spine Fracture-Dislocation
- Spinal cord injury (complete or incomplete)
- Cauda equina syndrome (lumbar levels)
- Neurogenic shock — hypotension + bradycardia (not tachycardia) due to loss of sympathetic tone
- Vascular injury (vertebral artery in cervical injuries)
- Immobilization — spine precautions, hard collar for cervical injuries.
- ABC management first — neurogenic shock: IV fluids + vasopressors (norepinephrine preferred). Avoid hypotension (MAP ≥85 mmHg targeted in complete cord injury).
- CT spine is the primary imaging modality in trauma. MRI if neurological deficit or ligamentous injury suspected.
- Urgent neurosurgery/spine surgery consultation for all fracture-dislocations.
- Avoid high-dose methylprednisolone — no longer recommended as standard of care.
- Foley catheter (urinary retention), DVT prophylaxis.
Key ED Principles for All Fracture-Dislocations
| Step | Action |
|---|---|
| 1. Neurovascular assessment | Document pulses, sensation, motor function before ANY manipulation |
| 2. Analgesia/Sedation | IV opioids; procedural sedation (propofol, ketamine) for major joint reduction |
| 3. Imaging | X-rays pre-reduction to identify fracture pattern; CT for complex injuries |
| 4. Reduction | Prompt reduction (especially hip ≤6 hrs, ankle with skin compromise immediately) |
| 5. Post-reduction check | Repeat X-ray + neurovascular exam |
| 6. Immobilization | Appropriate splint/brace in functional position |
| 7. Disposition | Orthopedic consultation for all fracture-dislocations; admission for hip, spine, Terrible Triad, open injuries, vascular compromise |
Indications for Emergency Orthopedic/Surgical Consultation
- Any open fracture-dislocation
- Vascular injury / absent pulses post-reduction
- Compartment syndrome
- Irreducible dislocation (soft tissue interposition)
- Hip fracture-dislocation (AVN risk)
- Cervical/thoracolumbar fracture-dislocation (spinal cord)
- Terrible Triad elbow
- Ankle fracture-dislocation with skin compromise
- Knee dislocation (popliteal artery risk)
Basic principles of splinting and traction. Principles of splinting fracture of long bone
Basic Principles of Splinting and Traction — and Splinting of Long Bone Fractures
Part 1: Principles of Splinting
Definition and Purpose
- Haemostasis and swelling control — a well-padded splint applies stabilization and compression to soft tissues, reducing further bleeding and swelling.
- Soft tissue protection — prevents further injury to an already traumatized soft tissue envelope from mobile fracture fragments.
- Pain relief and safe transport — reduces patient discomfort and facilitates transport and radiographic evaluation.
"Immobilization of the joints above and below the fracture is generally recommended to ensure adequate stability and prevention of a lost reduction." — Sabiston Textbook of Surgery, p. 773
General Principles of Splinting
| Principle | Detail |
|---|---|
| Neurovascular assessment | Document pulses, sensation, and motor function before and after every splint application |
| Immobilize one joint above and one below | Ensures the fracture site is fully controlled; prevents rotation |
| Adequate padding | Bony prominences (malleoli, olecranon, fibular head) must be well padded to prevent pressure necrosis |
| Appropriate position | Each splint has a specific functional position (see below per region) |
| Mold the splint | Counteract the natural tendency of the fracture to displace back into deformity |
| Non-circumferential | Leaves room for swelling for 48–72 hours post-injury |
| Post-application X-ray | Postreduction radiographs are required to confirm maintained reduction |
| Convert to cast later | After swelling subsides (2–3 weeks), splints are exchanged for circumferential casts in the outpatient setting |
Splinting Materials
- Calcium sulfate hemihydrate impregnated bandage
- Exothermic setting reaction (warn the patient of warmth)
- Sets in ~5–10 minutes; weight-bearing strength in 24–48 hours
- Easily molded; inexpensive
- Heavier than fiberglass; degrades with moisture
- Lighter, stronger, water-resistant
- Sets faster (~3–5 minutes)
- Less moldable than plaster
- More expensive
- Stockinette (optional — protects skin)
- Cotton/synthetic cast padding (Webril) — several layers, extra over bony prominences
- Plaster or fiberglass slab (8–10 layers of plaster; fewer of fiberglass)
- Compressive wrap (bias bandage or elastic/ACE wrap) — applied without circumferential tension
Circumferential Cast vs. Splint in the Acute Setting
"Application of a circumferential cast is rarely indicated in the acute treatment of adult fractures, especially because soft tissues in the injured extremity will continue to swell for 48 to 72 hours after injury. A circumferential cast that does not allow room for swelling can be too constrictive and could potentially lead to pressure necrosis or compartment syndrome." — Sabiston, p. 775
Molding — Critical Technique
| Fracture | Molding Direction |
|---|---|
| Humeral shaft | Valgus mold — prevents varus deformity from deltoid pull |
| Dorsally displaced distal radius | Volar-directed mold — counters extensor pull |
| Ankle fractures with mortise disruption | Neutral ankle position; U-slab + posterior slab |
| Metacarpal/phalangeal fractures | Intrinsic-plus position (70–90° MCP flexion, IP extension) |
Part 2: Splinting of Long Bone Fractures — By Region
1. Humeral Shaft Fractures
- Splint type: Coaptation (U-slab) splint
- Runs from the axilla, under the elbow, and up the lateral arm to the shoulder
- Gravity assists in maintaining alignment (hanging arm effect)
- Arm hangs at the side in neutral
- Position: Elbow 90°, forearm neutral (hanging)
- Alternative: Functional brace (Sarmiento brace) — if minimal swelling, can apply acutely in ED
- Immobilizes: Shoulder and elbow
- Note: Valgus mold to counteract varus deforming force
2. Forearm Fractures / Wrist Fractures
- Splint type: Sugar tong splint
- Runs from the distal palmar crease volarly, around the elbow (with the elbow at 90°), and to the dorsal MCP joints
- Prevents pronation and supination of the forearm, and immobilizes both wrist and elbow
- Finger traps used to apply gravity traction during application
- Position for wrist/distal radius: Wrist in slight flexion and ulnar deviation (for Colles' fracture after reduction); slightly extended for Smith's fracture
- For isolated wrist injuries: Short-arm splint (volar slab) may suffice for nondisplaced distal radius
- Mold: Volar-directed mold for dorsally displaced (Colles') fractures
3. Elbow Fractures
- Splint type: Posterior long arm splint
- Runs from posterior forearm, around the elbow, up the posterior humerus
- Position: Elbow at 90° flexion, forearm in neutral or slight pronation
4. Femoral Shaft Fractures
- Splint type: Traction splint (Hare, Thomas, Sager splint)
- Commercially produced device
- Applies longitudinal traction via padded proximal ring on the ischial tuberosity and distal traction via an ankle hitch
- Restores femoral length, controls rotation, reduces pain and blood loss
- Helps control bleeding by limiting the volume the thigh can expand into
- Key complications of traction splints: Pressure ulcers at the ischial tuberosity and ankle/heel
- Indication: Isolated femoral shaft fractures (mid-shaft); NOT for proximal or distal femur fractures, knee injuries, or open fractures with contamination
5. Tibial Shaft / Ankle / Foot Fractures
- Splint type: Short leg splint — posterior slab + U-slab (stirrup/U component)
- Posterior slab: applied from behind the calf, under the heel, to the metatarsal heads
- U-slab/stirrup: medial and lateral slabs crossing the ankle
- Together they resist all ankle motion
- Position: Ankle in neutral (90°) — critical to prevent equinus contracture
- Knee slightly flexed (30°) during application — relaxes gastrocnemius pull
- Gravity traction: patient in figure-4 position across the bed (ipsilateral side down) — relaxes gastrocnemius, assists in maintaining fibular length and medial malleolus reduction
- Extension to long leg: Side slabs added from knee to proximal thigh → long leg splint for tibial plateau/shaft fractures or knee injuries
6. Hand / Metacarpal / Phalangeal Fractures
- Splint type: Long finger splint, ulnar/radial gutter splint, thumb spica
- Position — intrinsic-plus: MCP joints 70–90° flexion, IP joints in extension
- Prevents shortening of collateral ligaments → prevents contracture
- Thumb fractures (Bennett's, Rolando's): Thumb spica splint
- Ulnar metacarpal (4th, 5th): Ulnar gutter splint
- Radial metacarpal (2nd, 3rd): Radial gutter splint
Part 3: Principles of Traction
Definition
Types of Traction
| Type | Mechanism | Indications | Pros | Cons |
|---|---|---|---|---|
| Skin traction | Adhesive/foam straps on skin transmit force | Temporary; hip fractures in elderly pre-op (comfort) | Non-invasive | Limited force; skin breakdown risk |
| Skeletal traction | Transosseous pin (Kirschner wire or Steinmann pin) + traction bow + weights | Femoral shaft, pelvis, acetabulum, polytrauma | Directly controls bone; effective for prolonged use | Invasive; infection risk at pin site |
| Traction splint | External frame (Hare, Thomas, Sager) with ischial ring + ankle hitch | Femoral shaft fracture (prehospital and ED) | Controls pain and bleeding; maintains length; fast | Pressure ulcers; indirect control; not length stable |
Skeletal Traction
- Pin placed through distal femur or proximal tibia:
- Distal femur: better for controlling femoral shaft fractures; avoids the knee joint
- Proximal tibia: easier to place; used for femoral and pelvic fractures
- Technique: Strict aseptic technique; local anaesthesia; pin passed from medial → lateral through the bone perpendicular to the long axis; traction bow attached; weights applied
- Weight: Typically ~10% of body weight (adjusted by X-ray)
- Indications: Unstable pelvic ring fractures, acetabular fractures, femoral shaft fractures, polytrauma patients awaiting surgery, intraarticular fractures to offload cartilage
Skin Traction
- Foam boots/adhesive applied to skin; traction weights ≤2–3 kg
- Limited by skin tolerance
- Used for short-term comfort (e.g., elderly hip fractures pre-operatively)
- Not used for definitive fracture management
Traction Splint (Hare / Thomas / Sager)
- Primary use: Femoral shaft fractures in the prehospital or ED setting
- Mechanism: Padded proximal ring seats on the ischial tuberosity → countertraction; distal ankle strap applies traction distally
- Effect: Restores limb length, reduces muscle spasm, decreases pain, reduces blood loss (thigh compartment volume is limited)
- Contraindications:
- Proximal or distal femur fractures (near the joint)
- Associated knee, ankle, or foot injuries
- Pelvic fractures (may worsen)
- Open fractures with gross contamination
Part 4: Reduction Principles (Preceding Immobilization)
"Reduction maneuvers follow the same general set of principles for all fracture and dislocation types. First, in-line traction is applied to the limb after sedation is administered... If the soft tissue envelope is intact, in-line traction alone may produce satisfactory alignment through ligamentotaxis. In most cases, the deformity must be recreated and exaggerated to allow for appropriate mobilization and reduction." — Sabiston, p. 773
- Adequate analgesia/sedation — hematoma block (local anaesthetic), IV opioids, or procedural sedation
- In-line traction — applied along the long axis of the limb
- Recreate and exaggerate the deformity — unlocks the fragments
- Reduce — reverse the deformity (usually by manipulation and rotation)
- Ligamentotaxis — for articular and periarticular fractures, traction through intact soft tissue can reduce the fracture indirectly
- Mold and splint — immediately after reduction, before loss of muscle relaxation
- Postreduction X-ray — confirm alignment
- Repeat neurovascular exam — document post-reduction status
Summary Table: Splint Type by Fracture Location
| Fracture Location | Splint Type | Joints Immobilized | Position |
|---|---|---|---|
| Phalanges | Long finger / gutter splint | MCP + PIP | Intrinsic-plus |
| Metacarpals (2nd–3rd) | Radial gutter | Wrist + MCP | Intrinsic-plus |
| Metacarpals (4th–5th) | Ulnar gutter | Wrist + MCP | Intrinsic-plus |
| Thumb/1st metacarpal | Thumb spica | Wrist + 1st CMC | Thumb abducted |
| Distal radius (Colles') | Sugar tong | Wrist + elbow | Wrist slight flexion/UD |
| Forearm | Sugar tong | Wrist + elbow | Neutral forearm |
| Elbow | Posterior long arm | Elbow + wrist | Elbow 90° |
| Humeral shaft | Coaptation (U-slab) | Shoulder + elbow | Elbow 90°, arm at side |
| Femoral shaft | Traction splint | Hip + knee | Neutral |
| Tibial shaft / plateau | Long leg splint | Knee + ankle | Knee slightly flexed, ankle 90° |
| Ankle / foot | Short leg splint (posterior + U) | Ankle | Neutral (90°) |
Devices used in Ed and prehospital care for splinting
Devices Used in the ED and Prehospital Care for Splinting
Why Splint? — Goals of Immobilization
- Reduces pain — limits motion of fracture fragments
- Protects neurovascular structures — prevents compression or stretching of nerves/vessels by displaced fragments
- Prevents open fracture conversion — stops sharp bone fragments from piercing skin
- Facilitates safe transport — minimises fragment movement during movement and imaging
"In most cases where a musculoskeletal injury is suspected, a splint should be applied and maintained." — Roberts & Hedges', p. 1072
Classification of Splinting Devices
SPLINTING DEVICES
├── 1. Rigid/Semirigid Splints
│ ├── Cardboard splints
│ ├── SAM Splint (aluminium/foam)
│ ├── Preformed/prefabricated plastic splints
│ └── Plaster / fiberglass slabs (ED standard)
├── 2. Soft Splints
│ ├── Air (inflatable) splints
│ ├── Vacuum splints (extremity)
│ ├── Pillow splints
│ ├── Sling
│ └── Sling and swath
├── 3. Traction Splints (Lower Limb)
│ ├── Hare Traction Splint
│ ├── Sager Emergency Traction Splint
│ ├── Kendrick Traction Device (KTD)
│ └── Ferno-Trac Traction Splint
├── 4. Full-Body / Spinal Immobilisation Devices
│ ├── Long spine board (backboard)
│ ├── Short spine board / KED (Kendrick Extrication Device)
│ ├── Scoop stretcher
│ ├── Vacuum mattress splint (EVAC-U-SPLINT)
│ └── Miller body splint
└── 5. Pelvic Binders
├── Pelvic sling (SAM Pelvic Sling)
└── Sheet wrap
1. Rigid and Semirigid Splints
A. Cardboard Splints
- Made from plain or wax-impregnated cardboard (water resistant)
- Advantages: Easily shaped to any contour; inexpensive; lightweight; radiolucent; MRI-compatible; can accommodate ice packs
- Best for: Long-bone fractures of the upper extremity; ankle/foot
- Common in both prehospital and ED settings
B. SAM Splint (Sam Medical Products)
- Thin core of soft aluminium alloy sandwiched between two layers of closed-cell foam
- Extremely pliable when flat; becomes rigid and load-bearing when bent into one of three simple curves (C-curve, reverse C, or T-shape)
- Advantages: Water resistant; lightweight; radiolucent; reusable; unaffected by extreme temperatures or altitude
- Ideal for wilderness medicine, prehospital kits, and EDs
- Fastened with tape, gauze, or Velcro straps
- Note: Non-malleable (one-size) aluminium splints are less ideal — malleable versions are preferred as they conform to the limb contour
C. Prefabricated Padded Plastic/Foam Splints
- Commercially produced; available in various sizes for upper and lower limbs
- Pre-padded; secured with Velcro
- Convenient but less adaptable than SAM splint or plaster
D. Plaster / Fiberglass Slabs (ED Standard)
- The definitive ED splinting material
- Applied as non-circumferential slabs in acute setting (to accommodate swelling)
- Circumferential casts avoided acutely in adults — risk of compartment syndrome and pressure necrosis as swelling progresses over 48–72 hours
- Covered in previous session in detail (sugar tong, posterior slab, coaptation, long leg, etc.)
2. Soft Splints
A. Air (Inflatable) Splints
- Transparent plastic, zipper-sealed or non-zipper, zippered or slip-on design
- Inflated by mouth or pump until it resists slight finger indentation (not rigid)
- Advantages: Easy and quick to apply; provides compression (may reduce swelling)
- Best for: Ankle, wrist, forearm injuries
- Application: Slide the uninflated splint over the rescuer's forearm → grasp the patient's hand → assistant slides it onto the patient → inflate
- Do NOT apply over clothing — wrinkles cause pressure sores in swollen tissue
- Do NOT overinflate — impairs circulation; device should yield to moderate thumb pressure
- Not appropriate for humerus or femur fractures — do not extend sufficiently proximally for adequate immobilisation
- Altitude and temperature affect internal pressure (volume increases with altitude — risk of over-pressurisation during air transport)
- Risk of pressure-induced tissue ischaemia and compartment syndrome
"Overinflating the device may impair circulation. If the inflatable splint cannot be dented by moderate thumb pressure, it is probably overinflated." — Tintinalli's, p. 1657
B. Vacuum Splints (Extremity)
- Closed bag filled with tiny foam beads; air evacuated with a hand pump to ~0.25 atm
- Before evacuation: completely flexible → moulds to the extremity in the position found
- After evacuation: beads compressed → rigid, form-fitting splint
- Radiolucent
- No external pressure → maximum circulation preserved
- More comfortable than hard splints
- Immobilises in position found (useful for angulated fractures or knee injuries where forced realignment is undesirable)
- Lower sacral interface pressure and lower pain scores vs. traditional backboards (when used as a mattress variant)
C. Pillow Splints
- Standard hospital pillow wrapped around the injury and secured with tape, cravats, or gauze
- Nail beds kept exposed for neurovascular monitoring
- Best for: Ankle and foot injuries; simple and universally available
D. Sling
- Triangular bandage supports the forearm and hand
- Adjusted so hand is higher than elbow (promotes venous drainage)
- Fingertips exposed at all times
- Best for: Shoulder injuries, clavicle fractures, upper arm fractures (with swath)
"Many patients with suspected anterior shoulder dislocation have difficulty adducting the forearm, and forcibly binding it to the thorax may be painful. A simple sling is adequate in such cases." — Tintinalli's, p. 1659
E. Sling and Swath
- Sling (as above) + a cravat tied circumferentially around the thorax at the level of the mid-humerus, binding the arm to the chest
- Best for: Humeral shaft fractures; proximal humerus fractures; shoulder injuries
- Two cravats may need to be joined end-to-end for larger patients
3. Traction Splints
Historical context
Mechanism of Action
- Increases potential space → up to 1–2 litres of blood can accumulate at the fracture site
- Causes fragment override and rotation
- Increases tissue pressure → reduces the potential bleeding space
- Reduces pain
- Prevents further neurovascular damage
- Reduces incidence of fat embolism
Indication
Contraindications
- Suspected pelvic fracture — proximal ring/bar presses on the pelvis, may displace fracture and increase haemorrhage
- Hip dislocation with gross displacement
- Knee injury — longitudinal traction may damage popliteal neurovascular structures
- Avulsion or amputation of the ankle or foot — no distal fixation point
- Associated distal tibia-fibula or ankle fracture in the same limb — traction distracts the distal fracture
- Open femoral fracture — use only in austere/prolonged-transport environments; copious irrigation first; inform receiving team; start antibiotics
Individual Traction Splints
i. Hare Traction Splint (Dyna-Med / Dynamed)
- Half-ring design (partial ring)
- Proximal padded end abuts the ischial tuberosity from below
- Distal ratchet mechanism applies traction via ankle strap
- Elastic support straps along the thigh and leg
- Produces hip flexion of up to 30° — requires patient to be reclined ~30° from horizontal for full alignment
- Can be longer than an ambulance cot when fully extended — logistical issue in smaller vehicles
- Complications: pressure ulcers at ischial tuberosity and ankle/heel
ii. Sager Emergency Traction Splint (Minto Research & Development)
- Proximal end rests against the pubic symphysis (not ischial tuberosity) → does not cause hip flexion
- Positioned medially between the legs (rather than under the leg like Hare)
- Less bulky → takes up less room in ambulance or helicopter
- Can be used with scoop stretchers (Hare splint interferes slightly with ischial section of scoop)
- Allows both femurs to be splinted simultaneously with a single device (bilateral femoral fractures)
- Traction dial/gauge for controlled traction measurement
iii. Kendrick Traction Device (KTD) (Ferno-Washington)
- Compact, lightweight device
- Uses similar half-ring principle
- Ideal for confined spaces (helicopters, extrication)
iv. Ferno-Trac Traction Splint (Ferno-Washington)
- Similar half-ring design to Hare
- Varies in attachment and strap configuration
v. Thomas Splint (historical / in-hospital traction)
- Full-ring design originally; modified to half-ring by Jones
- Used in-hospital with a Pearson knee piece attached for balanced skeletal traction
- Still used in some centres for temporary femoral traction while awaiting surgery
- Pressure ulcers at ischial tuberosity and heel/ankle
- Peroneal nerve compression at the fibular head (from support straps)
- Overuse in inappropriate fracture locations (near the knee, with pelvic fracture)
4. Full-Body and Spinal Immobilisation Devices
A. Long Spine Board (Backboard)
- Hard, flat, radiolucent board
- Patient strapped to board; head secured with foam/cardboard head blocks and head straps
- Cervical collar alone is not adequate for cervical immobilisation — must be combined with backboard and lateral head support
- Adults: padding placed under the head (compensates for normal dorsal kyphosis)
- Children: padding placed under the shoulders/torso (large occiput otherwise forces neck into flexion)
B. Cervical Collars (C-Collar)
- Rigid collars (e.g., Stifneck, Miami J) — standard for prehospital care
- Available in multiple sizes; sized by shoulder-to-chin distance (use tallest collar that does not cause hyperextension)
- For very short necks: No-Neck collar (Laerdal)
- Newer collars have anterior openings to observe trachea and jugular veins
- Soft cervical collars — NOT appropriate for prehospital care (inadequate immobilisation)
- Do not apply if: mandible or soft-tissue neck injury (risk of masking airway compromise)
- If resistance/pain on head movement: immobilise in position found
C. Kendrick Extrication Device (KED) (Armstrong Medical)
- Short spine board designed for seated vehicle extrication
- Immobilises cervical and thoracic spine
- Applied while patient is still in the vehicle, then patient rotated onto long board
- Not used if scene is critical (fire, chemicals, water) — expedited extrication with collar only
D. Scoop Stretcher (Orthopaedic/Split Litter Stretcher)
- Ferno-Washington Model 65 most widely used
- Splits longitudinally into two halves → placed under the patient without log-rolling
- Fastened at head and foot
- Minimises patient movement during extrication
- Limitation: may trap clothes/skin between interlocking parts; interferes slightly with ischial section of Hare splint (works well with Sager)
E. Vacuum Mattress Splint (EVAC-U-SPLINT, Immobile-Vac)
- Full-body vinyl-coated polyester envelope filled with thousands of 1.1 mm polyester foam spheres
- Manual or electric pump evacuates interior to ~0.25 atm → mattress conforms to body contours
- Advantages over hard backboard:
- Lower sacral interface pressure
- Lower mean pain scores
- Better immobilisation in patients with known spinal cord injury
- Comfortable for prolonged transport
- Limitation: larger and more cumbersome than backboards; difficult ambulance storage
F. Miller Body Splint
- Polyethylene shell with closed-cell foam interior
- Radiolucent; buoyant (useful in water rescue)
- Removable head, thoracic, pelvic, and lower extremity harnesses
- Space between legs allows bandaging for lower extremity fractures
- Fits into basket-type rescue stretchers
- Paediatric versions available (e.g., Pedi-Pac)
5. Pelvic Binders
SAM Pelvic Sling (Sam Medical Products)
- Commercially designed circumferential pelvic binder
- Applied at the level of the greater trochanters — NOT at the iliac crests
- Closes the posterior pelvic ring (open-book fractures), reduces pelvic volume, tamponades bleeding
- Indicated for: Suspected unstable pelvic fracture (lateral compression or anterior-posterior compression mechanism)
Sheet Wrap
- Simplest method: bedsheet folded and wrapped around the pelvis at the level of the trochanters, secured with a clamp or haemostat
- Immediately available, no equipment needed
- NOT military anti-shock trousers (MAST/PASG) — these are now largely abandoned: cumbersome; prolong scene time; risk of compartment syndrome and electrolyte imbalance
Device Selection by Injury Location
| Injury Site | Preferred Device(s) |
|---|---|
| Fingers / toes | Buddy taping (adjacent digit) |
| Hand / metacarpals | SAM Splint, cardboard, plaster gutter splint |
| Wrist / forearm | SAM Splint, air splint + sling, plaster sugar tong |
| Elbow | Posterior plaster slab; sling and swath |
| Humerus / shoulder | Sling and swath; coaptation plaster splint |
| Clavicle | Sling (simple); sling and swath |
| Hip (pre-op, ED) | Full-body immobilisation; skeletal traction (in-hospital) |
| Midshaft femur | Traction splint (Hare, Sager, KTD) |
| Knee / distal femur | Vacuum splint or cardboard, as found |
| Tibial shaft | Long leg plaster splint; cardboard; air splint extending above knee |
| Ankle / foot | Short leg plaster slab + U-slab; pillow; cardboard; air splint |
| Cervical spine | Rigid cervical collar + long backboard + lateral head blocks |
| Thoracolumbar spine | Long backboard; vacuum mattress; scoop stretcher |
| Pelvis (unstable) | SAM Pelvic Sling; sheet wrap |
Key Principles When Applying Any Device
- Neurovascular check before and after every application — document pulses, sensation, capillary refill
- Immobilise joint above and below the fracture
- Expose nail beds / fingertips for continuous monitoring during transport
- Adequate padding over bony prominences — prevent pressure necrosis
- Do not apply over clothing (air splints especially) — wrinkles cause pressure injury
- Do not force realignment — immobilise in position found for unstable/angulated fractures (especially knee, suspected neurovascular injury)
- Life before limb — in multi-system trauma, rapid transport takes precedence over extremity splinting
Types of immobilization dressings
Types of Immobilisation Dressings
Classification Overview
IMMOBILISATION DRESSINGS
│
├── A. SPLINTS (Non-circumferential)
│ ├── 1. Plaster of Paris slabs
│ ├── 2. Fiberglass slabs
│ ├── 3. Specific named splint types (sugar tong, coaptation, etc.)
│ └── 4. Prefabricated / commercial splints
│
├── B. CIRCUMFERENTIAL CASTS
│ ├── 1. Plaster of Paris cast
│ ├── 2. Fiberglass cast
│ ├── 3. Bivalved cast
│ └── 4. Cast brace (hinged cast)
│
├── C. COMPRESSION / BULKY DRESSINGS
│ ├── 1. Robert Jones (bulky cotton compression) dressing
│ └── 2. Simple compressive bandage
│
├── D. FUNCTIONAL BRACES / ORTHOSES
│ ├── 1. Sarmiento functional brace
│ ├── 2. Fracture boot / walking boot
│ └── 3. Custom orthoses / splints
│
└── E. SPECIAL DRESSINGS
├── 1. Sling
├── 2. Sling and swath
├── 3. Velpeau dressing
├── 4. Buddy taping
└── 5. Collar and cuff
A. Splints (Non-Circumferential Immobilisation)
"Application of a circumferential cast is rarely indicated in the acute treatment of adult fractures, especially because soft tissues in the injured extremity will continue to swell for 48 to 72 hours after injury." — Sabiston Textbook of Surgery, p. 775
Construction (Layers, Inner to Outer)
- Stockinette — optional; protects skin from irritation
- Cast padding (Webril / cotton roll) — several overlapping layers; extra layers over bony prominences
- Plaster or fiberglass slab — the structural element; applied as a slab, not circumferentially
- Compressive wrap (bias bandage / ACE / elastic bandage) — holds the construct without circumferential pressure
1. Plaster of Paris (POP) Slabs
- Material: Calcium sulphate hemihydrate impregnated into open-weave cotton bandage
- Setting: Exothermic reaction when wetted (warn the patient of warmth); working time ~3–5 minutes; sets hard in ~10 minutes; full weight-bearing strength in 24–48 hours
- Slab thickness: 8–12 layers for upper limb; 12–15 layers for lower limb
- Advantages:
- Highly mouldable — excellent for maintaining fracture reduction
- Inexpensive
- Easy to apply and trim
- Disadvantages:
- Heavy
- Degrades with moisture
- Takes longer to set than fiberglass
2. Fiberglass Slabs
- Material: Polyurethane resin impregnated into fibreglass mesh
- Setting: Sets in ~3–5 minutes; stronger per thickness unit than plaster
- Advantages:
- Lighter
- Stronger per layer
- Water resistant
- Radiolucent (better imaging)
- MRI compatible (non-ferromagnetic)
- Disadvantages:
- Less mouldable than plaster — harder to achieve precise fracture moulding
- More expensive
- Rough edges can lacerate skin if not trimmed
Named Splint Types (Plaster or Fiberglass)
i. Sugar Tong Splint
- Course: From the distal palmar crease (volar) → around the elbow → to the dorsal MCP joints
- Joints immobilised: Wrist + elbow; prevents pronation and supination
- Used for: Distal radius fractures, forearm fractures
- Application tip: Finger traps applied first to create gravity traction during splint application
ii. Coaptation (U-Slab) Splint
- Course: From axilla → under the elbow → up the lateral arm to the shoulder, forming a U-shape around the arm
- Joints immobilised: Shoulder + elbow
- Used for: Humeral shaft fractures
- Mechanism: Gravity assists alignment (hanging arm effect); valgus mould applied to counteract varus deformity from deltoid pull
iii. Posterior Long Arm Splint
- Course: Posterior forearm → posterior elbow → posterior humerus
- Position: Elbow at 90°, forearm neutral
- Used for: Elbow fractures, proximal forearm fractures
iv. Short Arm (Volar) Splint
- Course: Volar forearm from distal palmar crease to proximal forearm
- Used for: Nondisplaced distal radius fractures, wrist sprains, carpal injuries
v. Thumb Spica Splint
- Course: Radial forearm → around the thumb to its tip
- Used for: Scaphoid fractures, Bennett's fracture (1st metacarpal base), thumb UCL injuries
vi. Ulnar Gutter Splint
- Course: Ulnar border of hand → ulnar forearm
- Position: MCP at 70–90° (intrinsic-plus), IP joints extended
- Used for: 4th and 5th metacarpal fractures (Boxer's fracture)
vii. Radial Gutter Splint
- Course: Radial border of hand → radial forearm
- Used for: 2nd and 3rd metacarpal fractures; index/middle finger fractures
viii. Short Leg Splint (Posterior Slab + U-Slab / Stirrup)
- Components: Posterior slab (calf → metatarsal heads) + U-slab (medial and lateral stirrups crossing the ankle)
- Position: Ankle in neutral (90°) — prevents equinus contracture; knee slightly flexed during application
- Application tip: Gravity traction — limb hung in figure-4 position; relaxes gastrocnemius, maintains fibular length
- Used for: Ankle fractures, foot fractures, Achilles tendon injuries
ix. Long Leg Splint
- Construction: Short leg splint extended with medial and lateral side slabs crossing the knee to the proximal thigh
- Used for: Tibial shaft/plateau fractures, knee dislocations, patella fractures
x. Posterior Knee Splint
- Course: Posterior thigh → posterior calf
- Position: Knee at 0–20° of flexion
- Used for: Knee ligament injuries, patella fractures, tibial plateau fractures
B. Circumferential Casts
When to Use Acutely
- Most paediatric fractures (bone is more compliant; swelling less severe)
- Some nondisplaced adult fractures where a cast is the definitive treatment
1. Plaster of Paris Cast
- Same material as POP slabs but applied circumferentially
- Heavy; degrades with moisture; good moulding
2. Fiberglass Cast
- Lighter, stronger, water resistant
- Standard for definitive outpatient casting
- Less mouldable
3. Bivalved Cast
- A circumferential cast that is cut longitudinally on both sides (bivalved) immediately after application
- Allows room for swelling while maintaining reduction better than an open splint
- Held together by an ACE wrap or re-applied after swelling subsides
"It is recommended to 'bivalve' the initial circumferential cast after it is applied... This technique remains effective in maintaining the reduction, more than an open splint." — Sabiston, p. 775
4. Cast Brace (Hinged Cast / Long-Leg Cast with Knee Hinge)
- Long-leg cast incorporating a mechanical knee hinge
- Historical use: Femoral shaft fractures — applied after a few weeks of traction to allow knee mobilisation
- Still occasionally used for tibial fractures to allow controlled knee range-of-motion
- Largely replaced by operative fixation in modern practice
- Complications of prolonged cast/traction use: malalignment, knee stiffness (30–50%), nonunion/malunion (11–29%), shortening >2 cm (14–30%)
C. Compression / Bulky Dressings
1. Robert Jones Dressing (Bulky Cotton Compression Dressing)
- Construction: Multiple layers of cotton wool (or orthopaedic cotton) applied circumferentially to the limb, interleaved with crepe bandage layers, building up a thick, compressive, bulky dressing
- Typically 3–4 alternating layers of cotton wool and crepe bandage
- Can incorporate a plaster back-slab for structural support
- Functions:
- Controls swelling by compression and padding
- Provides comfort and immobilisation
- Protects soft tissues
- Used for: Post-operative lower limb dressings (knee/ankle); acute soft tissue injuries with significant swelling; temporary immobilisation before surgery; as the inner padding layer for a short leg or long leg splint
- Referenced in Sabiston as the "circumferential Robert Jones cotton" applied before the plaster stirrup splint for ankle fractures
2. Simple Compressive Bandage
- Elastic (Ace) or cohesive (Coban) bandage applied with even circumferential tension
- Provides mild compression for oedema control (sprains, contusions)
- Not adequate alone for fracture immobilisation
D. Functional Braces and Orthoses
1. Sarmiento Functional Brace (Humeral / Tibial)
- A prefabricated or custom-moulded clamshell plastic brace with Velcro closures
- Humeral fracture brace (Sarmiento brace):
- Surrounds the humeral shaft; held in place by hydrostatic pressure of soft tissues
- Does not immobilise the shoulder or elbow — allows functional use of the arm
- Applied once initial swelling has stabilised (typically 1–2 weeks after injury)
- Can be applied acutely in the ED if minimal swelling is present
- Controls alignment through soft-tissue hydraulics rather than rigid fixation
- Tibial fracture brace:
- Similar principle for tibial shaft fractures
- Allows early weight-bearing and knee/ankle motion
- Advantages: Preserves joint motion; reduces muscle atrophy; allows early mobilisation
- Limitation: Requires intact soft tissue envelope; not suitable for unstable, displaced fractures
2. Fracture Boot (Walking Boot / Moon Boot / CAM Walker)
- Prefabricated rigid-shell boot with an air bladder and rocker-bottom sole
- Removable (unlike a cast) — allows wound inspection and hygiene
- Used for: Stable ankle fractures, metatarsal fractures, calcaneal fractures, Achilles tendon injuries, stress fractures
- Equivalent to a cast for many stable lower limb injuries
3. Custom Orthoses / Splints
- Thermoplastic material (e.g., Orthoplast, Aquaplast) heated to ~65–70°C, then moulded directly to the patient's limb and allowed to harden
- Fabricated by occupational/hand therapists
- Used for: Hand and wrist injuries, post-operative immobilisation, tendon repairs, nerve injuries
E. Special Dressings
1. Sling
- Triangular bandage supporting the forearm and elbow
- Adjusted so the hand is higher than the elbow (promotes venous drainage)
- Fingertips exposed for neurovascular monitoring
- Used for: Clavicle fractures, proximal humerus fractures, shoulder dislocations, acromioclavicular injuries, elbow injuries (as adjunct)
2. Sling and Swath (Sling and Swathe / Shoulder Immobiliser)
- Sling + cravat / bandage wrapped circumferentially around the thorax at mid-humerus level, binding the arm to the chest wall
- Prevents shoulder movement in all planes
- Used for: Humeral shaft fractures, proximal humerus fractures, shoulder injuries requiring complete immobilisation
- Note: Two cravats joined end-to-end for larger patients
3. Velpeau Dressing
- Arm is held in adduction with the forearm across the chest; bandage wraps around arm and thorax
- Immobilises the shoulder without a sling
- Used for: Proximal humerus fractures, shoulder dislocations post-reduction (in elderly or when a sling is impractical)
- Less commonly used; replaced largely by the sling and swath
4. Collar and Cuff
- Simple suspension: a padded strap from the wrist to the neck, supporting the forearm
- The weight of the arm provides gentle gravity traction to the humerus
- Used for: Undisplaced or minimally displaced humeral shaft fractures, some proximal humerus fractures
- Preferred over a sling in specific humeral fractures where gravity-assisted alignment is desirable
- Allows elbow to hang freely (Sarmiento principle)
5. Buddy Taping (Neighbour Strapping)
- Injured digit is taped to an adjacent, uninjured digit which acts as a living splint
- Padding (gauze or foam) placed between the digits prevents maceration
- Used for: Undisplaced phalangeal fractures (fingers and toes), PIP dislocations, collateral ligament sprains
- Allows functional motion while preventing excessive deviation
Summary Comparison Table
| Type | Circumferential | Swelling Accommodation | Rigidity | Best Timing | Common Use |
|---|---|---|---|---|---|
| Plaster slab | No | Yes | High | Acute (ED) | Most acute fractures |
| Fiberglass slab | No | Yes | High | Acute (ED) | Most acute fractures |
| Plaster cast | Yes | No | Very high | 2–3 weeks post-injury | Definitive treatment |
| Fiberglass cast | Yes | No | Very high | 2–3 weeks post-injury | Definitive treatment |
| Bivalved cast | Yes (split) | Partial | High | Acute (selected) | Paediatric; nondisplaced |
| Robert Jones | Yes | Moderate | Low | Acute/post-op | Swelling control |
| Cast brace | Yes + hinge | No | Moderate | Subacute | Femur/tibia (historical) |
| Sarmiento brace | Yes | No | Moderate | Subacute | Humeral/tibial shaft |
| Fracture boot | Yes | No | Moderate | Acute/subacute | Stable ankle/foot |
| Sling | No | N/A | None | Acute | Upper limb |
| Sling and swath | No | N/A | Low | Acute | Shoulder/humerus |
| Collar and cuff | No | N/A | None | Acute | Humerus (gravity traction) |
| Buddy taping | No | N/A | Minimal | Acute | Finger/toe fractures |
"The use of plaster of Paris casts remains widespread as they are inexpensive and easy to apply. However, fiberglass casts are now more frequently used as they are lighter and more radiolucent. In addition, plastic orthoses, braces, and splints are now more frequently used." — Rockwood & Green's Fractures in Adults, 10th ed.
mechanism of injury, patient profile, classification, clinical features, how to examine – bony as well as nerve injuries, diagnosis, management, methods of pain management, complications For following fractures- Colles, smith, clavicle, proximal humerus, supra condylar humerus, pelvic, hip, neck of femur, shift of femur, IT
Colles' Fracture and Smith's Fracture
PART 1 — COLLES' FRACTURE
1. Definition
- Dorsal displacement and angulation of the distal fragment
- Radial shortening
- Volar apex angulation → classic "dinner fork deformity"
- Frequently associated with ulnar styloid fracture (indicates TFCC disruption)
"The Colles fracture is the commonest wrist injury sustained in adults." — Grainger & Allison's Diagnostic Radiology, p. 1149
2. Mechanism of Injury
- Fall on outstretched hand (FOOSH) with the wrist in extension and radial deviation
- The thenar eminence takes the impact; compressive force drives the distal radius dorsally and proximally
- Dorsal cortex is crushed → comminution on dorsal side
- In elderly: low-energy ground-level fall (osteoporosis)
- In young adults: high-energy trauma (MVA, sporting injury)
3. Patient Profile
| Feature | Detail |
|---|---|
| Most common | Post-menopausal women (osteoporosis) — bimodal with young male athletes |
| Peak age | 50–70 years (women); teenage/young adult (men) |
| Risk factors | Osteoporosis, female sex, Caucasian race, low BMI |
| Incidence | Most common adult fracture; ~640,000/year in USA |
| Side | Usually dominant hand |
"Women older than age 50 possess a 15% lifetime risk of a distal ulna and/or radius fracture." — Tintinalli's, p. 1846
4. Classification
Frykman Classification (most widely cited)
- Whether fracture is extra- or intra-articular (radiocarpal / radioulnar joint)
- Presence or absence of ulnar styloid fracture
- Higher grades = more complex, higher risk of complications
| Grade | Articular involvement | Ulnar styloid |
|---|---|---|
| I | Extra-articular | Absent |
| II | Extra-articular | Present |
| III | Radiocarpal | Absent |
| IV | Radiocarpal | Present |
| V | Radioulnar | Absent |
| VI | Radioulnar | Present |
| VII | Both joints | Absent |
| VIII | Both joints | Present |
AO / Universal Classification (Modern)
- Type A — Extra-articular
- Type B — Partial intra-articular (one joint)
- Type C — Complete intra-articular
Stability Criteria (determines ED management)
- Dorsal angulation >20°
- Intra-articular involvement
- Marked comminution
- Shortening >1 cm
- Associated ulnar fracture
5. Clinical Features
Symptoms
- Severe wrist pain after FOOSH
- Swelling, bruising over dorsal wrist
- Restricted wrist movement
- Paresthesias in the hand (median nerve distribution — thumb, index, middle finger)
Signs — The Classic Deformities
- "Dinner fork deformity" — on lateral view; dorsal hump proximal to wrist from dorsal displacement
- "Bayonet deformity" — radial shortening with overlap of fragments (AP view)
- Radial deviation of the hand (radial shortening)
- Tenderness over distal radius (within 2 cm of joint)
- Swelling over the dorsal wrist
- Skin tenting over the fracture site (with severely displaced fractures)
6. How to Examine
General
- Inspection: deformity, swelling, bruising, skin integrity (open fracture?)
- Palpation: maximal tenderness over distal radial metaphysis; check anatomical snuffbox (exclude scaphoid)
- Movement: active ROM of wrist (flexion/extension/pronation/supination) — reduced and painful
Bony Examination
- Palpate the distal radius from radial styloid to sigmoid notch
- Check DRUJ stability — dorsoventral stress while stabilising ulna
- Palpate ulnar styloid (TFCC injury if tender + fracture)
- Palpate carpals — exclude associated scaphoid fracture
Nerve Examination — Three Nerves at Risk
| Nerve | Test | Distribution |
|---|---|---|
| Median nerve (most at risk) | Light touch over thenar pad / index finger pulp; thumb opposition | Volar thumb, index, middle, radial half of ring finger |
| Radial nerve (superficial branch) | Light touch over dorsal first web space | Dorsal radial hand |
| Ulnar nerve | Light touch over little finger; finger abduction | Little finger, ulnar half of ring; intrinsics |
- Acutely from displacement, contusion, or stretch
- After reduction: from nerve compression in cast/splint → Acute Carpal Tunnel Syndrome (ACTS)
- After swelling subsides: chronic CTS
Vascular Examination
- Radial pulse (radial artery at wrist)
- Capillary refill of all digits
- Skin colour and temperature
"It is important to evaluate neurologic function before and after fracture reduction and splint application." — Rosen's, p. 4051
7. Diagnosis
Radiographs — Standard (PA + Lateral)
- Fracture line within 2 cm of articular surface
- Radial shortening (compare ulnar variance — normally radius is 1–3 mm longer than ulna)
- Normal radial inclination = 22–23° (reduced in Colles')
- Intra-articular extension
- Ulnar styloid fracture
- Normal volar tilt = 11–12° (volar face of articular surface tilts toward palm)
- In Colles': volar tilt is lost or reversed to dorsal tilt
- Dorsal displacement and comminution
CT Scan
- Indicated if intra-articular extension is suspected or poorly characterised on plain films
- Essential for surgical planning
MRI
- For associated soft tissue injuries (TFCC, scapholunate ligament) — rarely in acute ED setting
8. Management
ED Decision — Reduce or Not?
- Neurovascular compromise (especially median nerve symptoms, absent radial pulse)
- Significant skin tenting
- Dorsal angulation >20°
- Marked shortening
- Severe deformity causing patient distress
- Compression dressing + dorsal/volar splint (not circumferential cast)
- Orthopedic follow-up in 7–10 days
Methods of Pain Management / Anaesthesia for Reduction
1. Haematoma Block (most common in ED)
- 22-gauge needle inserted into the fracture site via the dorsal approach
- Aspirate until haematoma is obtained (confirms needle in fracture)
- Inject 5–10 mL of 1% or 2% lidocaine (± bupivacaine for longer duration)
- Onset in ~5–10 minutes
- Avoids procedural sedation; reduces ED length of stay
- Also safe in paediatric patients (avoid injecting into growth plate)
2. Bier Block (IV Regional Anaesthesia)
- Double-cuff tourniquet on the arm
- IV access in the ipsilateral hand
- Exsanguinate limb (elevation or Esmarch bandage)
- Inflate proximal cuff to 100 mmHg above systolic
- Inject 40 mL of 0.5% prilocaine or lidocaine IV
- Provides excellent analgesia and muscle relaxation
- Duration limited to tourniquet time; risk of local anaesthetic toxicity on cuff release
3. Procedural Sedation (IV)
- IV opioid (morphine, fentanyl) ± midazolam, or ketamine, or propofol
- Used for severe displacement, failed haematoma block, anxious patients
4. Regional Nerve Blocks
- Median, radial, and ulnar nerve blocks at the wrist
- Or ultrasound-guided brachial plexus block (most complete)
Reduction Technique (Closed)
- Adequate anaesthesia
- Finger traps applied to index and middle fingers; counter-traction via weight around elbow — to distract and disimpact
- Recreate the deformity slightly (increase dorsal angulation briefly to unlock impacted fragments)
- Apply distal and volar-directed force on the distal fragment while maintaining countertraction on the forearm
- Ulnar deviation corrects the radial shortening
- Apply volar mould to maintain reduction
Post-Reduction Splinting
- Sugar tong splint (forearm + around the elbow) — prevents pronation/supination
- Wrist in slight flexion and ulnar deviation (Cotton-Loder position)
- Note: excessive flexion risks ACTS — wrist should not be >15° flexion
- Convert to cast at 1–2 weeks when swelling resolves
Indications for Surgical Referral (ORIF / CRPP / External Fixation)
- >3 mm of radial shortening
- >10° of dorsal tilt
- >2 mm intra-articular step-off
- Unstable fracture that cannot be maintained closed
- Open fracture
- Severe comminution
- Neurovascular compromise not resolved by reduction
- Compartment syndrome
Disposition
- Simple stable → splint + orthopaedic follow-up 7–10 days
- Reduced → check post-reduction X-ray + repeat neuro exam → follow-up 5–7 days
- Emergent orthopaedic consult: open fracture, vascular compromise, uncontrolled ACTS, irreducible
9. Complications
| Timing | Complication |
|---|---|
| Immediate | Median nerve injury (ACTS), radial artery injury |
| Early | Loss of reduction (especially in elderly + comminuted) |
| Early | Compartment syndrome |
| Late | Malunion (most common) — radial shortening, dorsal angulation |
| Late | Chronic carpal tunnel syndrome |
| Late | Post-traumatic wrist osteoarthritis |
| Late | Sudeck's atrophy (Complex Regional Pain Syndrome, CRPS) |
| Late | EPL (extensor pollicis longus) tendon rupture — at Lister's tubercle |
| Late | Distal radioulnar joint (DRUJ) instability |
| Late | Stiffness / reduced range of motion |
PART 2 — SMITH'S FRACTURE
1. Definition
- Volar displacement and angulation of the distal fragment
- Often called the "reverse Colles' fracture"
- May extend into the radiocarpal joint
2. Mechanism of Injury
- Direct blow to the dorsum of the wrist/hand → forced palmar flexion
- Fall onto a flexed, pronated wrist (dorsal surface strikes the ground)
- Backward fall on an outstretched hand with the forearm in supination, which then pronates — the radius is pulled forward by the forearm
3. Patient Profile
| Feature | Detail |
|---|---|
| Age | Younger than typical Colles' patient; also seen in the elderly |
| Sex | Slightly more common in males (higher-energy mechanism) |
| Common settings | Cycling accidents (fall onto dorsum of hand); motorcycle/bicycle injuries; sporting injuries |
| Less common | Elderly FOOSH with wrist in flexion |
4. Classification — Thomas Classification
| Type | Description | Equivalent |
|---|---|---|
| Type I | Extra-articular; oblique fracture; volar and proximal displacement | Classic Smith's |
| Type II | Intra-articular fracture through dorsal lip of radius; carpus displaces volarly | Dorsal Barton's equivalent |
| Type III | Intra-articular fracture through volar lip; volar rim fracture with carpal subluxation | Volar Barton's |
- Type III is the most unstable and virtually always requires surgical fixation.
5. Clinical Features
Symptoms
- Painful, swollen wrist after fall/direct blow
- Palmar paraesthesias (median nerve under volar displacement)
Signs
- "Garden spade deformity" — on lateral examination; fullness on the volar aspect (opposite to Colles')
- Swelling predominantly volar
- Wrist deformed volarly and proximally
- Restricted motion
- The PA radiograph looks similar to Colles' (shortened distal radius) — the lateral view is diagnostic
6. How to Examine
Bony Examination
- Same as Colles' (see above)
- Tenderness over the distal radius
- Check DRUJ stability
- Palpate ulnar styloid
Nerve Examination
- Median nerve — most at risk (volar displacement compresses the nerve at the wrist)
- Test sensation over thenar pad, index pulp; thumb opposition
- Radial and ulnar nerves (as per Colles')
- Smith's fracture has a higher tendency for neurovascular compromise than Colles'
Vascular Examination
- Radial pulse; capillary refill; colour and temperature of digits
- Volar displacement can kink or compress the radial artery
7. Diagnosis
Radiographs
- Distal metaphyseal fracture (looks similar to Colles' on this view)
- Comminution possible; may appear shortened
- Distal fragment displaced and angulated volarly (toward palm)
- Volar "step" of distal radius relative to proximal shaft
- Carpus displaced with distal fragment
- Indicated for intra-articular extension (Types II and III)
- Essential for surgical planning
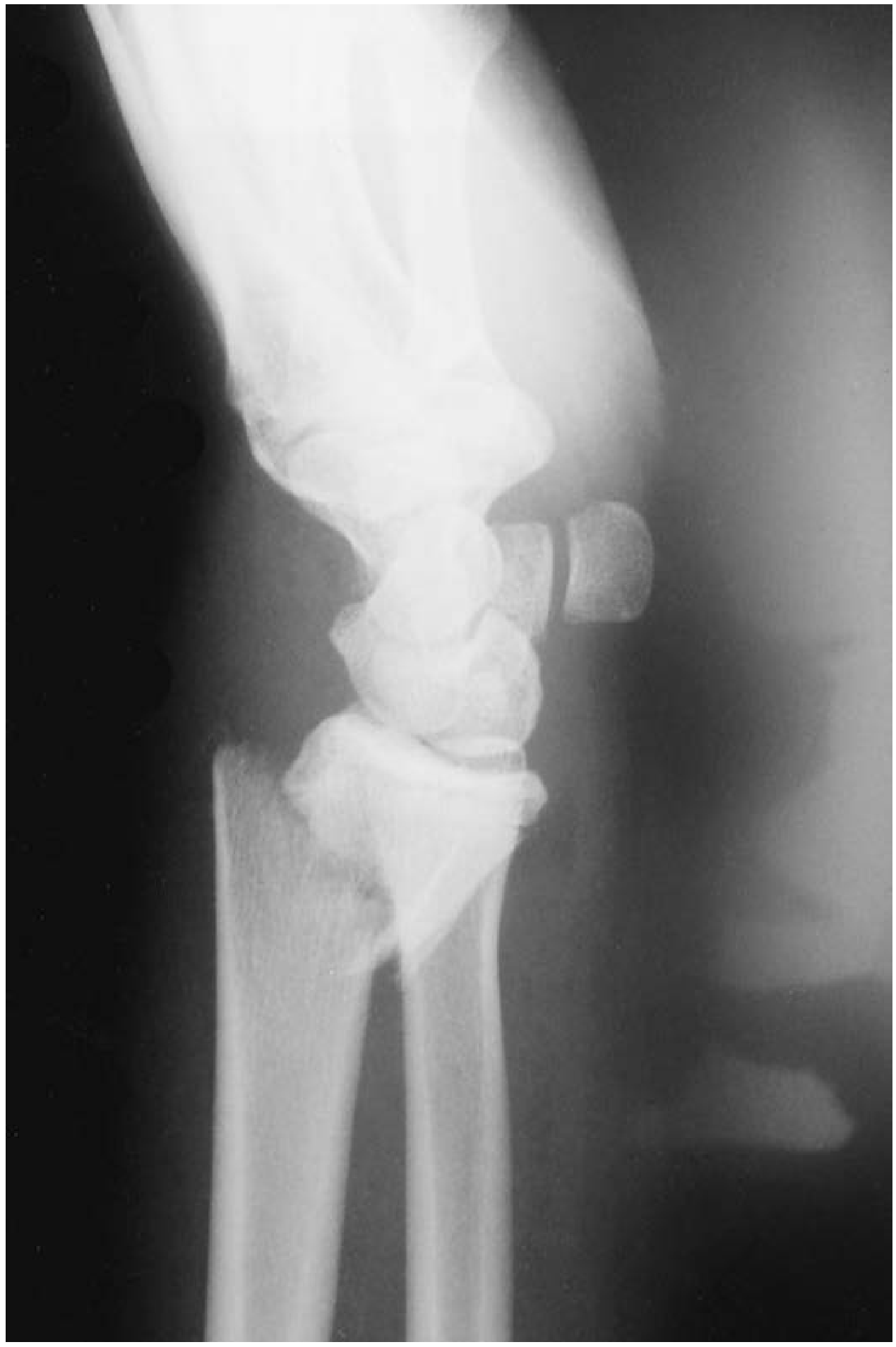
8. Management
Closed Reduction (Extra-articular / Type I)
- Same anaesthesia options as Colles' (haematoma block, Bier block, procedural sedation)
- Reduction: traction + dorsal-directed pressure on the volar distal fragment (opposite to Colles')
- Recreate mechanism slightly → reverse
Post-Reduction Splinting
- Sugar tong splint (prevents pronation/supination)
- Key difference from Colles': Wrist immobilised in dorsiflexion (extension), not flexion — to maintain reduction and prevent re-displacement
- Forearm in supination
Methods of Pain Management
Operative Management
- High tendency for loss of reduction with closed management
- Types II and III are virtually always operative (ORIF with volar locking plate)
- Type I with significant displacement or inability to maintain reduction → ORIF
"Unlike Colles fracture, Smith fracture is more likely to be unstable and to require operative repair." — Rosen's Emergency Medicine, p. 4086
- Any intra-articular extension (Types II, III)
- Inability to maintain closed reduction
- Neurovascular compromise
- Delayed tendon complications (EPL entrapment)
Disposition
- Urgent orthopaedic follow-up within 2–3 days (due to instability — unlike Colles' which can wait 7–10 days)
- Emergent consultation: open fracture, vascular compromise, uncontrolled nerve symptoms
9. Complications
| Timing | Complication |
|---|---|
| Immediate | Median nerve compression (higher risk than Colles') |
| Early | Loss of reduction (more common than Colles') |
| Early | Compartment syndrome |
| Late | EPL entrapment and rupture |
| Late | Malunion with volar angulation |
| Late | Post-traumatic arthritis |
| Late | CRPS (Sudeck's atrophy) |
| Late | Chronic carpal tunnel syndrome |
| Late | DRUJ instability |
Colles' vs Smith's — Quick Comparison
| Feature | Colles' | Smith's |
|---|---|---|
| Displacement | Dorsal | Volar |
| Deformity | "Dinner fork" | "Garden spade" |
| Mechanism | Fall on extended wrist (FOOSH) | Fall/blow on flexed wrist / supinated FOOSH |
| Patient | Elderly female | Younger; also elderly |
| PA X-ray | Short distal radius (± ulnar styloid) | Similar to Colles' |
| Lateral X-ray | Dorsal tilt | Volar tilt |
| Nerve at risk | Median (ACTS) | Median (higher risk) |
| Stability | Variable (often reducible) | More unstable |
| Splint position | Wrist slight flexion + ulnar deviation | Wrist extension + supination |
| Operative rate | Selected cases | Higher — Types II/III almost always |
Viral extanthems in er
viral exanthems emergency department approach diagnosis management 2024
viral exanthems emergency department measles varicella roseola fifth disease hand foot mouth diagnosis management
viral exanthem rash types measles varicella roseola erythema infectiosum hand foot mouth
measles morbilliform rash koplik spots rubeola
varicella chickenpox vesicular rash stages
roseola infantum exanthem subitum rash maculopapular trunk
rubella German measles rash lymphadenopathy forchheimer spots
hand foot mouth disease vesicles oral lesions herpangina coxsackievirus
viral exanthems ED emergency approach fever rash dangerous vs benign red flags isolation 2024
Viral Exanthems in the Emergency Department
What Is a Viral Exanthem?
- Direct viral infection of skin cells (e.g., VZV, HSV)
- Secondary immune/inflammatory response following viraemia (e.g., parvovirus B19, measles)
- Toxic effect of viral proteins on cutaneous vasculature
"The rash follows a viremia and is accompanied by fever." — Medical Microbiology 9e
ED Approach to Fever + Rash
Step 1 — Is This Child/Patient Sick or Not Sick?
| RED FLAGS — Admit / Urgent Action | Reassuring Features |
|---|---|
| High fever + petechiae/purpura → meningococcaemia | Well-appearing child |
| Haemodynamic instability | Rash appearing as fever resolves (roseola pattern) |
| Mucosal involvement + skin peeling → SJS/TEN | No mucosal involvement |
| Widespread blistering + Nikolsky sign | Localised or centrifugal spread |
| Immunocompromised host | Vaccinated child |
| Pregnant woman exposed to rubella/parvovirus | Normal WBC; benign prodrome |
| Non-blanching rash | Blanching rash |
| Altered consciousness | Interactive, playful |
Step 2 — Describe the Rash
| Morphology | Key causes |
|---|---|
| Maculopapular (morbilliform) | Measles, rubella, roseola, EBV, enteroviruses, drugs |
| Vesicular | Varicella, HSV, HFMD, zoster |
| Petechial/purpuric | Meningococcaemia, dengue, EBV, rickettsial |
| Scarlatiniform | Scarlet fever (Group A Strep), Kawasaki |
| Reticular/lacy | Erythema infectiosum (parvovirus B19) |
Step 3 — Distribution of Spread
| Starting location | Condition |
|---|---|
| Face → trunk → extremities | Measles, rubella, erythema infectiosum |
| Trunk → arms → face | Roseola, scarlet fever |
| Extremities (palms, soles, oral) | HFMD |
| Centripetal (trunk-heavy) | Varicella |
Step 4 — Isolation Precautions in the ED
| Disease | Transmission | Isolation |
|---|---|---|
| Measles | Airborne | Airborne (negative pressure room) |
| Varicella | Airborne + contact | Airborne + contact |
| Rubella | Droplet | Droplet |
| Roseola, HFMD | Contact/droplet | Contact |
| Erythema infectiosum | Droplet | Droplet (only if immunocompromised or pregnant exposure) |
Classic Viral Exanthems
1. MEASLES (Rubeola) — First Disease
Clinical Features
- High fever (may reach 40°C)
- The 3 Cs: Cough, Coryza (runny nose), Conjunctivitis
- Photophobia
- Child appears toxic/ill
- Koplik spots — bluish-white/grey "grains of salt" on an erythematous base on the buccal mucosa, appearing 1–2 days before the rash
- Begins on the face and behind the ears → spreads cephalocaudally to trunk → extremities over 3–4 days
- Erythematous, maculopapular, confluent in high-density areas
- Lasts 4–7 days; fades in the order it appeared (branny desquamation may follow)
- Blanches on pressure initially
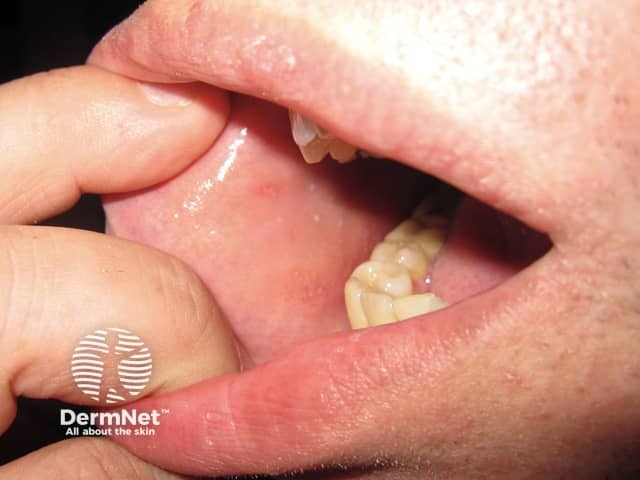
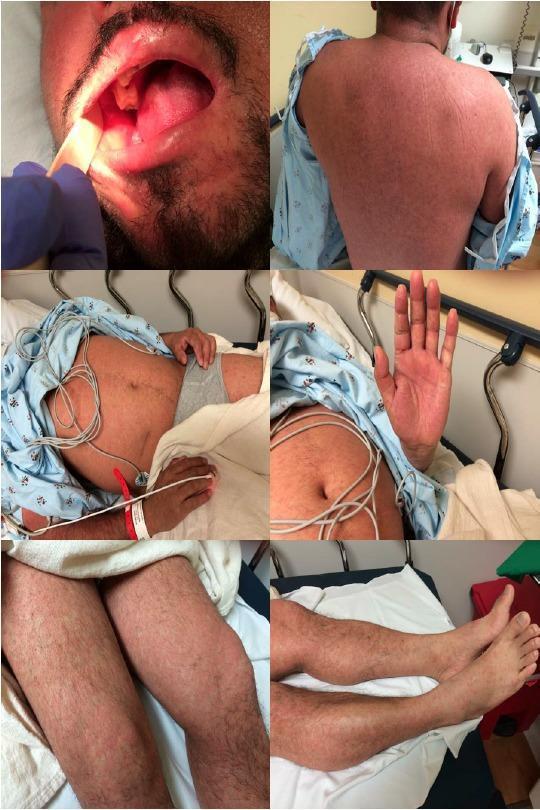
Diagnosis
- Clinical (Koplik spots + 3 Cs + rash)
- Confirmatory: Measles IgM serology or RT-PCR (nasopharyngeal swab, urine) — mandatory as notifiable disease
ED Management
- Supportive: Antipyretics (paracetamol/ibuprofen), hydration, eye care
- Vitamin A — reduces morbidity and mortality; WHO recommends for all children with measles:
- <6 months: 50,000 IU × 2 days
- 6–11 months: 100,000 IU × 2 days
- ≥12 months: 200,000 IU × 2 days
- Airborne isolation immediately on suspicion
- No specific antiviral
- Notify public health authorities
Complications
- Pneumonia (most common cause of death)
- Encephalitis (~1 in 1000)
- Otitis media
- Keratoconjunctivitis → corneal ulceration
- Subacute sclerosing panencephalitis (SSPE) — years later
- Immunosuppression ("immune amnesia") for weeks–months
2. RUBELLA (German Measles) — Third Disease
Clinical Features
- Low-grade fever, malaise, headache
- Lymphadenopathy — tender, posterior auricular, occipital, and posterior cervical nodes (highly characteristic)
- Mild coryza and conjunctivitis
- Forchheimer spots — small, red petechiae on the soft palate (non-specific but suggestive)
- Begins on face → spreads to trunk → extremities within 24–48 hours (faster than measles)
- Pink-red, discrete maculopapules; rarely confluent
- Less pronounced than measles; may not appear at all in some patients
- Lasts only 3 days ("3-day measles")
- No cephalocaudal desquamation
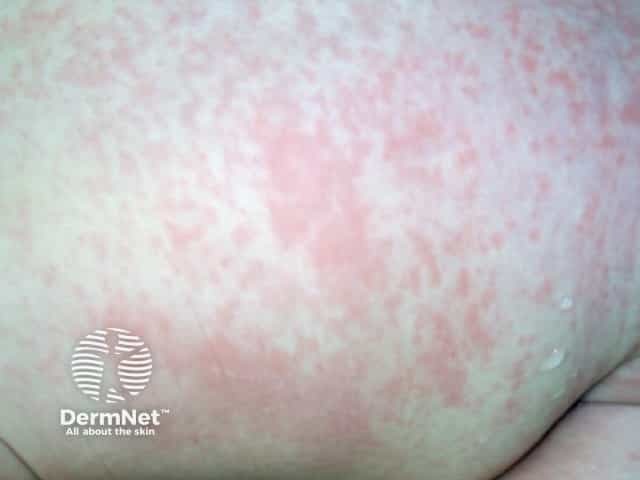
Diagnosis
- Clinical (lymphadenopathy pattern + 3-day rash)
- Confirmatory: Rubella IgM or RT-PCR
- Crucially important in pregnant women — congenital rubella syndrome risk
ED Management
- Supportive only; no antiviral
- Droplet precautions
- Most important action: Identify contact with pregnant women → notify public health; check maternal immune status
- Congenital rubella syndrome: deafness, cataracts, cardiac defects, microcephaly if infection in first trimester
3. ROSEOLA INFANTUM (Exanthem Subitum) — Sixth Disease
Clinical Features — Classic Pattern
- Abrupt onset high fever (39–40°C) with no obvious source
- Child may appear relatively well between febrile peaks
- Febrile seizures in ~10–15% (most common cause of febrile seizures in this age group)
- Mild coryza, lymphadenopathy, mild pharyngitis
- Nagayama spots — erythematous papules on soft palate/uvula
- Characteristic: fever defervesces → rash appears (fever rarely returns)
- Small, discrete, pale-pink macules and papules; some with surrounding blanching halos
- Begins on trunk → spreads to neck, arms, face (centrifugal)
- Lasts 1–3 days then disappears without desquamation
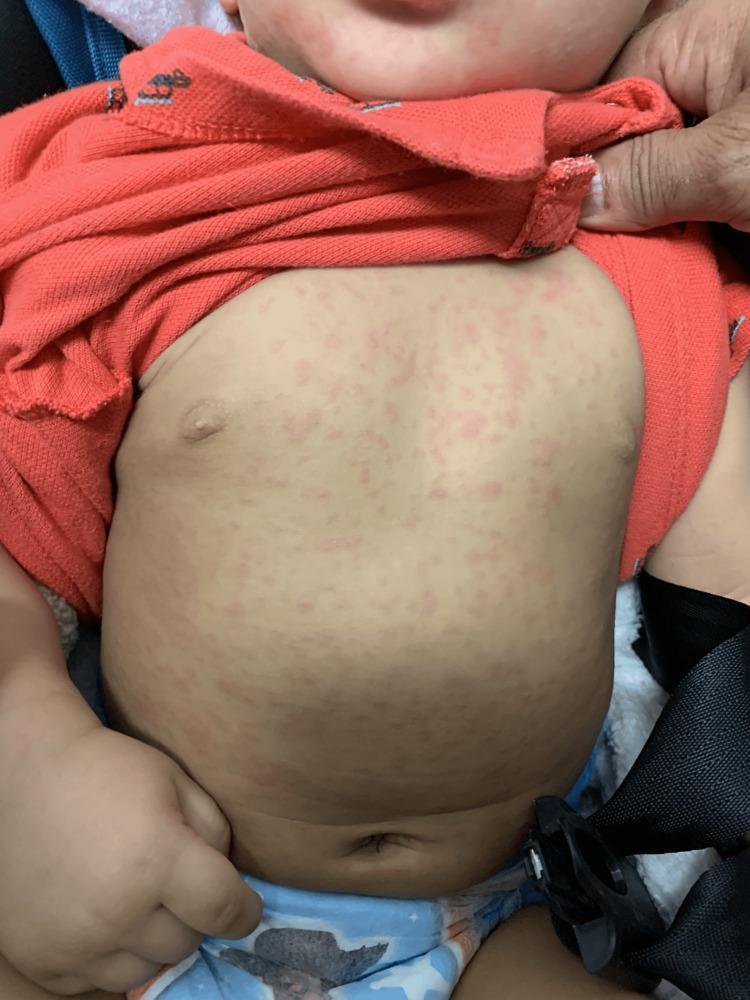
Key ED Teaching Point
The rash of roseola is a reassuring sign — it signals that the fever is over and the illness is resolving.
Diagnosis
- Entirely clinical — the pattern of high fever → defervescence → rash is pathognomonic
- Rarely: HHV-6 PCR or serology if uncertain
ED Management
- Supportive: Antipyretics (paracetamol/ibuprofen), hydration, reassurance
- Febrile seizure management if required (benzodiazepines acutely; reassure parents)
- No antiviral needed in immunocompetent children
- Contact precautions (mild)
4. ERYTHEMA INFECTIOSUM — Fifth Disease
Clinical Features — Three Phases
- Mild prodrome: low-grade fever, malaise, headache, myalgia
- Child is most contagious at this stage (viraemic phase)
- Bright red, bilateral malar erythema ("slapped cheeks")
- Perioral pallor preserved (circumoral sparing)
- Child is no longer contagious once rash appears
- Spreads to trunk and extremities as a lacy, reticular, net-like erythema
- May wax and wane over 1–3 weeks, exacerbated by sun, heat, exercise
- May be mildly pruritic
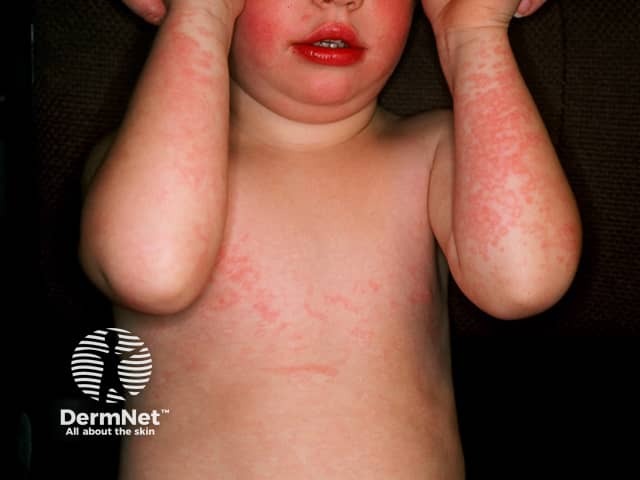
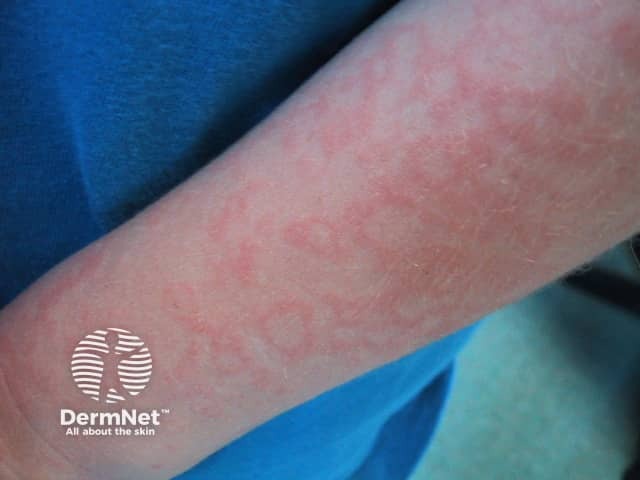
ED Special Concerns
| Population | Risk | Action |
|---|---|---|
| Pregnant women | Hydrops fetalis (especially 1st/2nd trimester) | Notify obstetrician; parvovirus B19 IgM/IgG; fetal US |
| Sickle cell / haemolytic anaemia | Aplastic crisis (transient red cell aplasia) — severe anaemia | FBC urgently; may need transfusion |
| Immunocompromised | Chronic anaemia from persistent infection | IV immunoglobulin (IVIG) |
| Arthritis | Adults (especially women) develop symmetric polyarthritis | Symptomatic; NSAIDs |
Diagnosis
- Clinical in children (slapped cheek + lacy rash)
- Parvovirus B19 IgM (acute); IgG (past exposure/immunity)
- PCR for viraemia (immunocompromised, aplastic crisis)
ED Management
- Supportive for healthy children — reassurance, antipyretics
- Do NOT use corticosteroids (rash will worsen when stopped)
- Screen all contacts — identify pregnant women or haematologically vulnerable individuals
5. VARICELLA (Chickenpox) — Second Disease
Clinical Features
- Fever, malaise, headache, anorexia
- Pruritic rash (often severe)
- "Dew drop on a rose petal" — clear vesicles on an erythematous base
- Lesions at multiple stages simultaneously (macule → papule → vesicle → pustule → crust)
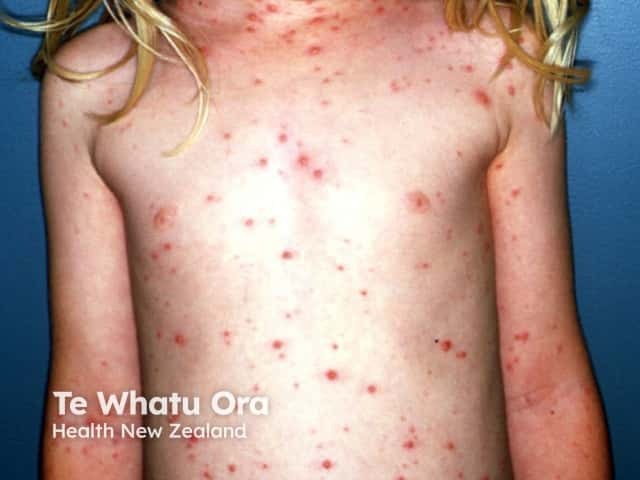
Diagnosis
- Clinical in most cases
- Confirmatory (if needed): VZV PCR from vesicle swab; DFA of vesicle scraping
ED Management
- Supportive: antipyretics (paracetamol — NOT aspirin, risk of Reye's syndrome), calamine lotion, antihistamines for pruritus, trim fingernails
- Airborne + contact isolation
- No antivirals needed in healthy children <12 years with uncomplicated disease
- Adults and adolescents (≥12 years) — reduce duration and severity
- Children with skin/pulmonary conditions (e.g., eczema, asthma on steroids)
- Immunocompromised patients → IV acyclovir (10 mg/kg IV q8h)
- Neonates with maternal varicella within 5 days before or 2 days after delivery → IV acyclovir
- VZIG (Varicella-Zoster Immune Globulin) — for susceptible immunocompromised, pregnant women, neonates
Complications
| Complication | Risk group |
|---|---|
| Bacterial superinfection (Group A Strep, Staph) — most common | All |
| Varicella pneumonia | Adults, immunocompromised, smokers |
| Encephalitis / cerebellitis | Children (cerebellitis more common, benign) |
| Haemorrhagic varicella | Immunocompromised |
| Reye's syndrome | If aspirin given |
| Neonatal varicella (severe/fatal) | Perinatal exposure |
6. HAND, FOOT AND MOUTH DISEASE (HFMD)
Clinical Features
- Low-grade fever, malaise, anorexia, sore mouth, cough
- Painful oral ulcers — shallow, grey-yellow erosions on an erythematous base on the tongue, buccal mucosa, hard and soft palate, tonsillar pillars, uvula
- May precede skin lesions
- Small oval/elliptical vesicles (2–5 mm) on erythematous base — long axis parallel to skin creases
- Distribution: palms, soles, dorsum of feet and hands (acral); also oral, perianal, buttocks, elbows, knees
- May be asymptomatic or painful
- Lesions crust within 7–10 days
- More widespread; involves trunk, face, extremities
- May mimic varicella or eczema herpeticum
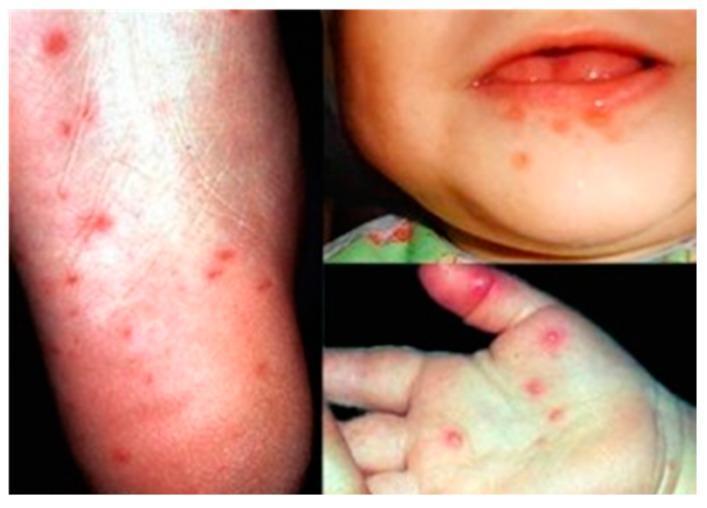
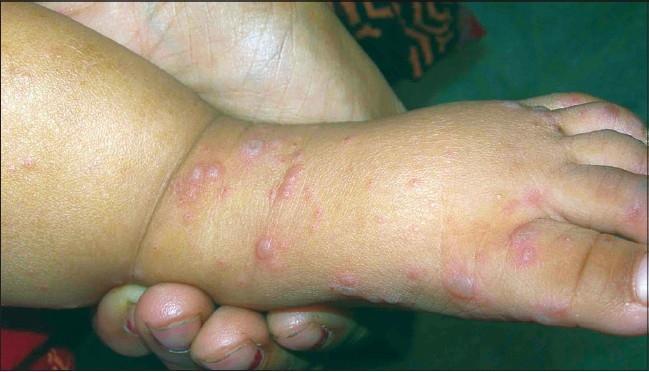
Diagnosis
- Clinical (distribution is pathognomonic)
- PCR if enterovirus 71 suspected (CNS complications)
ED Management
- Supportive: adequate hydration (oral ulcers reduce intake), oral analgesics (paracetamol, ibuprofen)
- Topical oral anaesthetics (viscous lidocaine in older children/adults) for mucosal pain
- Contact precautions
- Enterovirus 71: watch for neurological complications — aseptic meningitis, encephalitis, pulmonary oedema (rare but potentially fatal); consider lumbar puncture if CNS signs
Complications
- Dehydration from poor oral intake
- Nail loss (onychomadesis) — weeks later
- EV71-associated: meningitis, encephalitis, pulmonary oedema
7. INFECTIOUS MONONUCLEOSIS (EBV)
Clinical Features
- Triad: Fever + exudative pharyngitis + lymphadenopathy (posterior cervical)
- Splenomegaly (50%)
- Rash in 5–15% spontaneously
- Ampicillin/amoxicillin rash — 80–100% of EBV patients given aminopenicillins develop a widespread maculopapular rash within days → this is NOT true penicillin allergy
ED Note
- Avoid aminopenicillins
- Avoid contact sports (splenomegaly → splenic rupture risk)
Comparison Table — Classic Viral Exanthems
| Disease | Agent | Age | Prodrome | Enanthem | Rash start | Rash type | Duration | Contagious |
|---|---|---|---|---|---|---|---|---|
| Measles | Paramyxovirus | Any | 3–4d; 3Cs, high fever | Koplik spots | Face → trunk → limbs | Maculopapular, confluent | 4–7d | Before rash to day 4 |
| Rubella | Togavirus | Any | 1–5d; mild; lymphadenopathy | Forchheimer spots | Face → trunk | Discrete macules | 3d | 7d before to 7d after |
| Roseola | HHV-6/7 | 6mo–3yr | 3–5d HIGH fever | Nagayama spots | Trunk → arms (as fever breaks) | Pale-pink macules | 1–3d | Fever phase |
| Fifth Disease | Parvovirus B19 | 5–14yr; adults | 1wk; mild | None | Face (slapped cheek) → lacy body | Reticular/lacy | Wks (waxing) | Before rash (viraemic) |
| Varicella | VZV | Any | 1–2d | None (mild) | Trunk → head → limbs | Vesicular, all stages | 5–7d | 2d before → all crusted |
| HFMD | Coxsackie/EV | <10yr | 12–36h; mouth pain | Oral ulcers | Palms/soles/oral | Oval vesicles (acral) | 7–10d | During illness |
ED Management Summary
Universal Principles
- Isolate early — correct precautions (airborne vs droplet vs contact)
- Identify high-risk contacts — pregnant women, immunocompromised, neonates
- Notify public health for notifiable diseases (measles, rubella)
- Avoid aspirin in children with viral illness (Reye's syndrome)
- Do not prescribe corticosteroids for viral rashes (masking, worsening)
- Do not label aminopenicillin rash in EBV as true penicillin allergy
Specific Treatments
| Disease | Specific Treatment |
|---|---|
| Measles | Vitamin A; supportive |
| Rubella | Supportive only; urgent for pregnant contact |
| Roseola | Supportive; febrile seizure management |
| Fifth disease | Supportive; IVIG in immunocompromised; transfusion in aplastic crisis |
| Varicella | Acyclovir in high-risk groups; VZIG post-exposure |
| HFMD | Supportive; watch EV71 for CNS |
When to Admit from ED
| Indication | Condition |
|---|---|
| Haemodynamic instability, petechiae, purpura | Meningococcaemia, rickettsial, dengue |
| Aplastic crisis with anaemia | Parvovirus B19 in sickle cell |
| Varicella pneumonia, encephalitis | VZV |
| Immunocompromised with severe viral rash | Any VZV, HSV disseminated |
| Poor oral intake / dehydration | Severe HFMD/herpangina |
| EV71 neurological signs | HFMD with CNS involvement |
| Neonate with maternal varicella exposure | Neonatal VZV — IV acyclovir |