What is fatty liver what are it types it's home health treatment
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Loading Image
Reading File
Now I have comprehensive information from multiple textbooks. Here is a thorough, well-sourced answer:
Fatty Liver Disease
What Is It?
Fatty liver disease (hepatic steatosis) is a condition where fat — primarily triglycerides — accumulates in liver cells (hepatocytes), affecting 5% or more of them. It ranges from a benign, reversible finding to a progressive disease leading to cirrhosis and liver cancer.
The global prevalence of NAFLD is approximately 25% of the general population, making it the most common chronic liver disease worldwide.
— Yamada's Textbook of Gastroenterology, 7th ed.
Types of Fatty Liver Disease
1. Alcoholic Fatty Liver Disease (AFLD)
Caused by heavy or chronic alcohol consumption. The liver metabolizes alcohol into toxic byproducts (like acetaldehyde) that disrupt fat metabolism, causing fat to build up. This is often the first stage of alcohol-related liver disease, and can progress to alcoholic hepatitis and cirrhosis.
2. Non-Alcoholic Fatty Liver Disease (NAFLD)
Occurs in people who drink little or no alcohol. It is strongly linked to:
- Obesity (especially central/abdominal obesity)
- Type 2 diabetes or insulin resistance
- High blood triglycerides (dyslipidemia)
- Hypertension / Metabolic syndrome
NAFLD itself has a spectrum of subtypes:
| Subtype | What It Means |
|---|---|
| NAFL (Non-Alcoholic Fatty Liver) | Simple fat accumulation, no significant inflammation. Generally benign. |
| NASH (Non-Alcoholic Steatohepatitis) | Fat + inflammation + hepatocyte injury (ballooning) ± fibrosis. Can progress. |
| NASH with Fibrosis | Scarring develops; fibrosis stage F1–F4 |
| Cirrhosis (F4) | End-stage scarring; risk of liver failure and hepatocellular carcinoma |
The diagram below shows how NAFLD progresses:
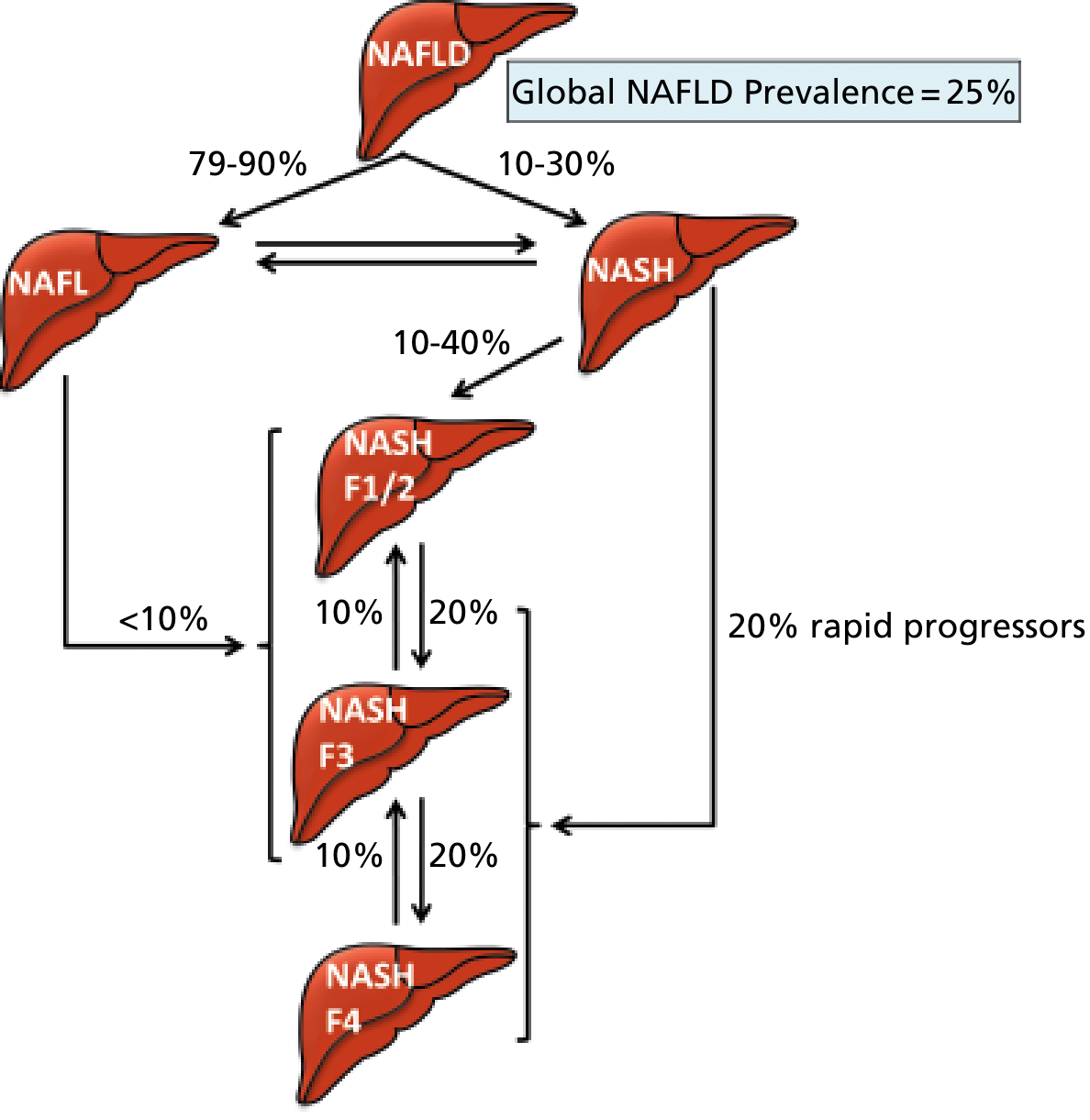
3. Acute Fatty Liver of Pregnancy (AFLP)
A rare but serious condition occurring in the third trimester, where fat accumulates in liver cells and can cause acute liver failure. It is a medical emergency.
4. Drug- or Toxin-Induced Fatty Liver
Certain medications and agents can cause steatosis, including corticosteroids, amiodarone, methotrexate, tamoxifen, and some chemotherapy agents.
— Robbins & Kumar Basic Pathology; Washington Manual of Medical Therapeutics
How Does It Develop? (Pathogenesis)
In NAFLD/NASH, the key driver is insulin resistance:
- Insulin resistance causes excessive lipolysis (fat breakdown) in adipose tissue
- Free fatty acids flood into the liver
- The liver stores them as triglycerides (steatosis)
- Excess lipids cause direct toxicity — oxidative stress, ER stress, mitochondrial dysfunction
- This triggers inflammation (inflammasome activation, IL-1 release), hepatocyte injury, and eventually fibrosis
Altered gut microbiome and increased gut-derived endotoxins also contribute to liver inflammation.
— Robbins & Kumar Basic Pathology; Yamada's Textbook of Gastroenterology
Symptoms
Most people are asymptomatic. When symptoms occur:
- Fatigue and general malaise
- Mild right upper quadrant discomfort or heaviness
- Incidentally found elevated liver enzymes (ALT/AST) on blood tests
- In advanced disease: jaundice, swelling, easy bruising (signs of cirrhosis)
Home & Lifestyle Treatment
Lifestyle modification is the most effective and evidence-based treatment for fatty liver disease — and often the only treatment needed for simple NAFLD.
🥗 1. Weight Loss (Most Important)
- Losing 3% of body weight can improve steatosis
- Losing 7–10% can resolve NASH
- Losing ≥10% can reverse fibrosis
- Fewer than 20% of patients maintain weight loss long-term, so consistent effort is key
🏃 2. Diet
- Mediterranean diet is strongly recommended — rich in vegetables, fruits, whole grains, legumes, fish, and olive oil; low in red meat and processed foods
- Reduce refined carbohydrates and added sugars (especially fructose/sugar-sweetened beverages)
- Limit saturated fats and trans fats
- Avoid alcohol entirely, even in NAFLD, as it worsens liver injury
- Reduce overall caloric intake to create a caloric deficit
🏋️ 3. Exercise
- Both aerobic exercise and resistance training are beneficial
- Aim for at least 150 minutes of moderate-intensity exercise per week
- Exercise reduces liver fat even without significant weight loss
- Reduces insulin resistance, a root cause of NAFLD
🩺 4. Control Underlying Conditions
- Tight blood sugar control if diabetic (metformin may have a mild benefit)
- Treat high cholesterol/triglycerides with appropriate diet and, if needed, medications
- Manage high blood pressure
- Stop potentially offending medications if drug-induced
☕ 5. Other Helpful Habits
- Coffee: Regular coffee consumption (2–3 cups/day, unsweetened) has been associated in studies with lower rates of NASH progression and fibrosis
- Avoid unnecessary supplements or herbal remedies — some can worsen liver injury
- Sleep: Treat obstructive sleep apnea if present (hypoxia worsens fatty liver)
Medical & Surgical Treatments (When Needed)
- Vitamin E: An antioxidant that can improve NASH in non-diabetic adults (biopsy-proven NASH only)
- Pioglitazone: An insulin sensitizer that may improve NASH, especially in diabetic patients
- GLP-1 agonists (e.g., liraglutide, semaglutide): Promising in reducing liver fat alongside weight loss
- Bariatric surgery: For obese patients with NASH — studies show significant improvement or resolution of NASH post-surgery
- Liver transplant: For end-stage cirrhosis
— Washington Manual of Medical Therapeutics; Robbins & Kumar Basic Pathology; Current Surgical Therapy 14e
Key takeaway: Simple fatty liver (NAFL) is largely reversible with lifestyle changes. The danger lies in progression to NASH and fibrosis, which is why early intervention with weight loss, a healthy diet, and regular exercise is so important. Anyone with suspected fatty liver should work with a doctor to rule out more advanced disease.
What is fatty liver what are it types it's home health treatment
I already covered this topic in detail in my previous response above. Here's a quick summary:
Fatty Liver — Quick Summary
What it is: A condition where fat accumulates in ≥5% of liver cells. Ranges from harmless to life-threatening depending on stage.
Types
| Type | Cause |
|---|---|
| Alcoholic (AFLD) | Heavy alcohol use |
| Non-Alcoholic - Simple (NAFL) | Obesity, insulin resistance — fat only, no inflammation |
| Non-Alcoholic Steatohepatitis (NASH) | Fat + inflammation + cell injury; can scar the liver |
| Acute Fatty Liver of Pregnancy | Third trimester emergency |
| Drug-induced | Steroids, methotrexate, amiodarone, etc. |
Home & Lifestyle Treatment
| Action | Target |
|---|---|
| Lose 7–10% body weight | Resolves NASH; 10%+ can reverse scarring |
| Mediterranean diet | Reduce sugar, refined carbs, red meat, saturated fat |
| Exercise 150 min/week | Reduces liver fat even without weight loss |
| Avoid alcohol completely | Even small amounts worsen liver injury |
| Control blood sugar & cholesterol | Address the root cause (insulin resistance) |
| Drink unsweetened coffee | 2–3 cups/day linked to slower disease progression |
| Treat sleep apnea | Nighttime oxygen drops accelerate liver damage |
For the full detailed answer with diagrams and textbook citations, scroll up to my previous response. If you have a more specific question — such as about a particular stage, symptoms, or medications — feel free to ask.
What is fatty liver what are it types it's home health treatment
I've already answered this question twice in this conversation — please scroll up to see the full detailed response, including:
- What fatty liver is (definition, prevalence, how it develops)
- All types — AFLD, NAFL, NASH, Acute Fatty Liver of Pregnancy, Drug-induced
- A diagram showing NAFLD disease progression
- Home & lifestyle treatments — weight loss targets, diet, exercise, alcohol avoidance, coffee, sleep apnea, and more
- Medical treatments when lifestyle changes aren't enough
If you have a new or more specific question about fatty liver — such as:
- Diet plans or meal ideas
- How to know if you have it
- Specific medications
- Fatty liver in children
- Fatty liver and diabetes
...just ask and I'll go deeper on that topic.
Yes
Asking for Preferences
No problem! Here is the complete, consolidated guide on fatty liver — covering everything in one place:
🫀 Fatty Liver Disease — Complete Guide
What Is Fatty Liver?
Fatty liver (hepatic steatosis) is a condition where excess fat builds up inside liver cells, accounting for more than 5% of liver weight. The liver becomes enlarged and, over time, the fat can trigger inflammation and scarring.
It affects 1 in 4 people worldwide and is now the most common chronic liver disease globally.
Types of Fatty Liver
1. 🍺 Alcoholic Fatty Liver Disease (AFLD)
- Caused by heavy or regular alcohol use
- Alcohol is broken down into toxic byproducts that disrupt fat metabolism
- First and most reversible stage of alcohol-related liver disease
- Stops progressing if alcohol is cut out
2. 🍔 Non-Alcoholic Fatty Liver (NAFL) — Simple Steatosis
- Fat accumulates in the liver without significant inflammation
- Caused by obesity, insulin resistance, high cholesterol, type 2 diabetes
- Generally benign and reversible with lifestyle changes
- No alcohol involvement
3. 🔥 Non-Alcoholic Steatohepatitis (NASH)
- Fat plus inflammation plus liver cell injury
- Can lead to scarring (fibrosis) → cirrhosis → liver failure → liver cancer
- Often has no symptoms until advanced
- About 10–30% of NAFL patients progress to NASH
4. 🤰 Acute Fatty Liver of Pregnancy (AFLP)
- Rare, occurs in the third trimester
- A medical emergency — can cause acute liver failure
- Requires immediate hospital care and often early delivery
5. 💊 Drug/Toxin-Induced Fatty Liver
- Caused by medications: steroids, methotrexate, amiodarone, tamoxifen, some chemotherapy drugs
- Reversible once the offending drug is stopped
Disease Progression

NAFLD progresses from simple fat (NAFL) → inflammation (NASH) → fibrosis → cirrhosis. About 20% of NASH patients are rapid progressors.
Symptoms
Most people have no symptoms until the disease is advanced. When present:
- Fatigue and weakness
- Mild discomfort or heaviness in the upper right abdomen
- Elevated liver enzymes found on routine blood tests
- In advanced disease: jaundice (yellowing), swelling of legs/abdomen, easy bruising
Home & Lifestyle Treatment
These are the most effective treatments — often better than any medication:
🥗 Diet
| ✅ Eat More | ❌ Eat Less |
|---|---|
| Vegetables & leafy greens | Sugary drinks & fruit juices |
| Fruits (in moderation) | White bread, white rice, pasta |
| Whole grains (oats, quinoa) | Fried & fast foods |
| Legumes (lentils, beans) | Red & processed meat |
| Fish (especially fatty fish) | Sweets, cakes, pastries |
| Olive oil | Saturated & trans fats |
| Nuts & seeds | Alcohol (avoid completely) |
Mediterranean diet is the most recommended dietary pattern for fatty liver.
⚖️ Weight Loss Targets
| Weight Lost | Benefit |
|---|---|
| 3% | Reduces liver fat (steatosis) |
| 7–10% | Can resolve NASH completely |
| ≥10% | Can reverse liver scarring (fibrosis) |
🏃 Exercise
- 150 minutes/week of moderate aerobic exercise (brisk walking, cycling, swimming)
- Add resistance/strength training 2–3 times per week
- Exercise reduces liver fat even without significant weight loss
🚫 Avoid Alcohol
- Alcohol worsens fatty liver even in non-alcoholic types — avoid it entirely
☕ Coffee
- 2–3 cups of plain, unsweetened coffee daily is linked to slower disease progression and lower fibrosis risk
😴 Sleep & Stress
- Treat obstructive sleep apnea — nighttime oxygen drops accelerate liver damage
- Chronic stress raises cortisol, which worsens insulin resistance
🩸 Control Underlying Conditions
- Keep blood sugar well controlled (diabetes is a major driver)
- Manage high triglycerides and cholesterol
- Control blood pressure
- Review medications with your doctor — some drugs cause fatty liver
Medical Treatments (When Lifestyle Isn't Enough)
| Treatment | Who It's For |
|---|---|
| Vitamin E | Non-diabetic adults with biopsy-proven NASH |
| Pioglitazone | Diabetic patients with NASH |
| GLP-1 agonists (semaglutide, liraglutide) | Obesity + NASH; reduces liver fat significantly |
| Bariatric surgery | Obese patients with NASH unresponsive to lifestyle |
| Liver transplant | End-stage cirrhosis only |
Key Takeaway
Fatty liver caught early is fully reversible. The single most powerful intervention is gradual, sustained weight loss through diet and exercise. No medication has been proven as effective as consistent lifestyle change.
If you suspect fatty liver, see a doctor for blood tests (liver enzymes, lipid panel, blood sugar) and an abdominal ultrasound.
Nafld what is how to manage it best fruits vegetables with there mechanism
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Now I have comprehensive textbook data. Here is a thorough, well-sourced answer on NAFLD with all the specifics requested:
NAFLD — What It Is, How to Manage It & Best Fruits/Vegetables with Their Mechanisms
What Is NAFLD?
Non-Alcoholic Fatty Liver Disease (NAFLD) is a clinicopathologic syndrome defined as fat accumulation in ≥5% of liver cells (hepatocytes) in the absence of significant alcohol consumption, viral hepatitis, or steatogenic medications.
It is the most common chronic liver disease globally, affecting ~25% of the world's population.
The NAFLD Spectrum
| Stage | What Happens | Risk of Progression |
|---|---|---|
| Simple Steatosis (NAFL) | Fat only — no inflammation | Low; often benign |
| NASH | Fat + inflammation + hepatocyte ballooning ± fibrosis | 10–40% progress to fibrosis |
| Fibrosis (F1–F3) | Liver scarring develops | Can regress with treatment |
| Cirrhosis (F4) | End-stage scarring | Risk of liver failure & cancer |

How Does NAFLD Develop? (Mechanism)
Two core, interrelated defects drive NAFLD:
1. Insulin Resistance & Hyperinsulinemia
- Insulin resistance causes excessive lipolysis in adipose tissue
- Free fatty acids (FFAs) flood into the liver
- The liver esterifies them into triglycerides → macrovesicular steatosis (primarily centrilobular)
- Simultaneously, the liver increases de novo lipogenesis (making new fat from carbohydrates)
2. Lipotoxicity → Inflammation → Fibrosis
- FFAs that remain unesterified inside hepatocytes are directly toxic (lipotoxicity)
- This triggers:
- Oxidative stress (from mitochondria and microsomes)
- Endoplasmic reticulum (ER) stress
- Inflammasome activation → IL-1 release → hepatocyte injury
- Apoptosis (liver cell death)
- Hepatic stellate cell activation → collagen deposition → fibrosis
- Altered gut microbiome and increased gut-derived endotoxins amplify liver inflammation
- Key adipocytokines: ↓ adiponectin (protective) and ↑ TNF-α (damaging)
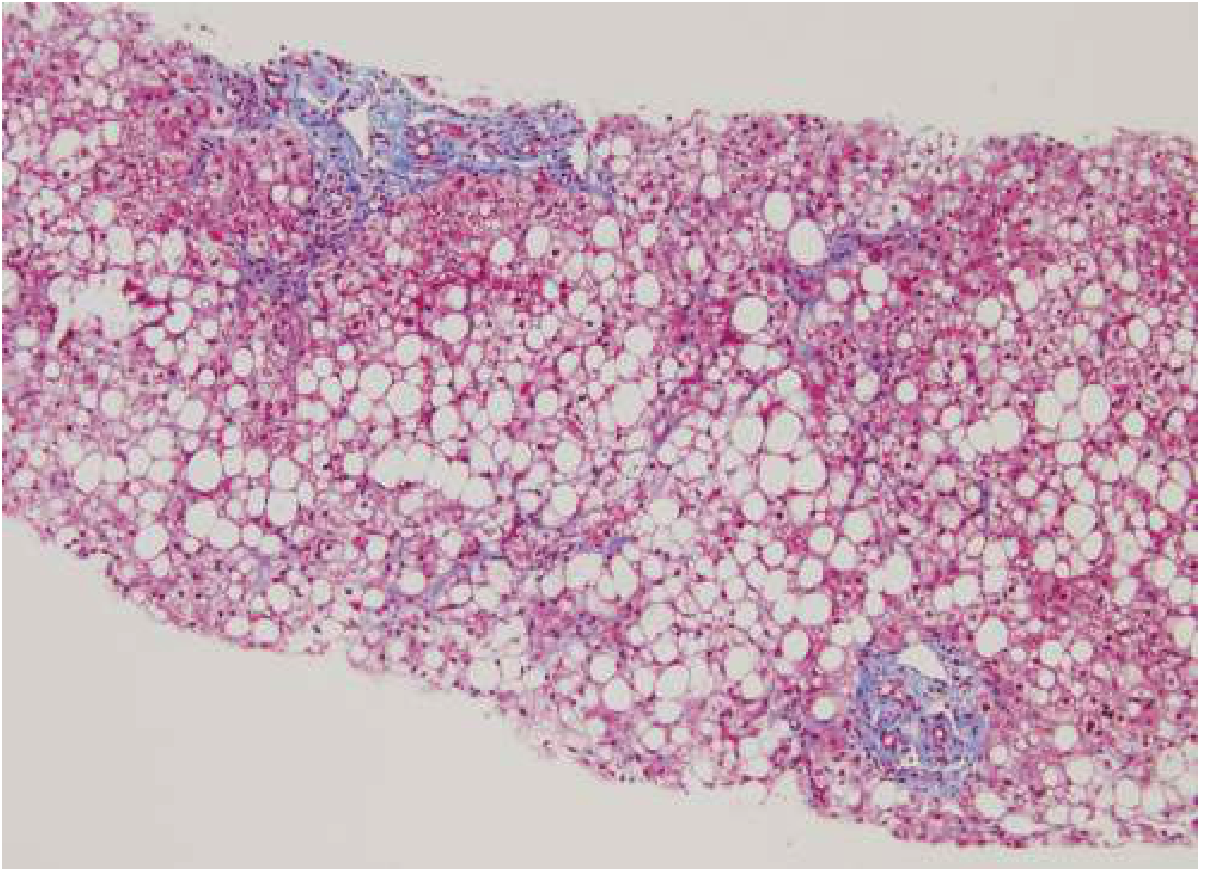
Risk Factors
- Obesity (especially central/abdominal)
- Type 2 diabetes / insulin resistance
- Dyslipidemia (high triglycerides, low HDL)
- Hypertension / metabolic syndrome
- Polycystic ovary syndrome (PCOS)
- Hypothyroidism
- Obstructive sleep apnea
- Genetic factors: PNPLA3, TM6SF2, GCKR gene variants increase risk
Symptoms
Most patients are asymptomatic. When present:
- Fatigue, malaise
- Right upper quadrant heaviness/discomfort
- Incidentally elevated ALT/AST on blood tests (ALT > AST, rarely >250 IU/L)
- In advanced cirrhosis: jaundice, ascites, encephalopathy, easy bruising
Management of NAFLD
🥇 First-Line: Lifestyle Modification
This is the most effective treatment and the foundation of all NAFLD management.
| Weight Loss Target | Benefit |
|---|---|
| 3% body weight | Reduces steatosis |
| 7% body weight | Improves NASH histology |
| 10% body weight | Can cause fibrosis regression |
- Low refined-sugar diet — reduces de novo lipogenesis
- Regular aerobic + resistance exercise — improves insulin sensitivity and reduces liver fat independently of weight loss
- Avoid saturated fat, high fructose, alcohol
- A multidisciplinary approach (dietician + exercise specialist + behavioral therapy) gives the best results
💊 Medical Treatments (when lifestyle is insufficient)
| Drug | Mechanism | Who It's For |
|---|---|---|
| Vitamin E (800 IU/day) | Antioxidant — reduces oxidative stress and hepatocyte injury | Non-diabetic adults with biopsy-proven NASH |
| Pioglitazone | PPAR-γ agonist → improves insulin sensitivity | Diabetic patients with NASH |
| GLP-1 agonists (semaglutide, liraglutide) | Reduce appetite, weight, liver fat & inflammation | Obese NASH patients |
| Statins | Reduce cardiovascular risk (primary cause of death in NAFLD) | Patients with dyslipidemia |
🔪 Surgical Treatment
- Bariatric surgery — for obese patients; prospective studies show significant NASH resolution
- Liver transplant — end-stage cirrhosis only
— Goldman-Cecil Medicine; Washington Manual of Medical Therapeutics; Robbins & Kumar Basic Pathology
Best Fruits for NAFLD — With Mechanisms
| Fruit | Key Compounds | Mechanism of Benefit |
|---|---|---|
| Blueberries / Berries | Anthocyanins, resveratrol, Vitamin C | Potent antioxidants → neutralize reactive oxygen species (ROS) from lipotoxicity; reduce NF-κB-mediated liver inflammation |
| Avocado | Monounsaturated fats (oleic acid), glutathione | Replaces saturated fat; oleic acid reduces de novo lipogenesis; glutathione is a master antioxidant protecting hepatocytes |
| Citrus fruits (lemon, orange, grapefruit) | Naringenin, hesperidin, Vitamin C | Flavonoids activate PPAR-α → promote fatty acid oxidation; reduce hepatic triglyceride synthesis; improve insulin sensitivity |
| Apples | Quercetin, pectin (soluble fiber) | Pectin feeds beneficial gut bacteria → reduces gut-derived endotoxin reaching the liver; quercetin reduces hepatic inflammation |
| Grapes / Red grapes | Resveratrol, polyphenols | Activates SIRT1 (sirtuin pathway) → improves mitochondrial function and fatty acid oxidation; reduces liver fat accumulation |
| Pomegranate | Punicalagins, ellagic acid | Reduces oxidative stress markers; inhibits inflammatory cytokines (TNF-α, IL-6); shown to lower liver enzymes in NAFLD |
| Papaya | Papain, lycopene, Vitamin C | Anti-inflammatory; lycopene reduces lipid peroxidation; enzyme papain aids digestion |
⚠️ Important: Eat whole fruits, not fruit juice. Fruit juice concentrates fructose, which is metabolized entirely by the liver → directly drives de novo lipogenesis and worsens NAFLD.
Best Vegetables for NAFLD — With Mechanisms
| Vegetable | Key Compounds | Mechanism of Benefit |
|---|---|---|
| Broccoli / Cruciferous vegetables | Sulforaphane, indole-3-carbinol, fiber | Sulforaphane activates Nrf2 pathway → upregulates antioxidant enzymes (glutathione peroxidase, SOD); reduces liver fat accumulation and fibrosis |
| Spinach / Dark leafy greens | Nitrates, Vitamin E, folate, chlorophyll | Nitrates improve mitochondrial efficiency → less oxidative stress; Vitamin E reduces lipid peroxidation; folate reduces homocysteine (ER stress trigger) |
| Garlic | Allicin, S-allylcysteine | Reduces TNF-α and IL-6; improves insulin sensitivity; reduces hepatic fat; allicin has direct hepatoprotective effects |
| Onions | Quercetin, organosulfur compounds | Quercetin inhibits NF-κB → reduces liver inflammation; improves adiponectin levels |
| Beets / Beetroot | Betaine (trimethylglycine), betalains | Betaine is a methyl donor → reduces hepatic fat via improved phosphatidylcholine synthesis (better fat export from liver); reduces oxidative stress |
| Artichoke | Cynarin, silymarin precursors, inulin | Cynarin stimulates bile production → better fat digestion; inulin (prebiotic fiber) improves gut microbiome → reduces endotoxin load on liver |
| Sweet potato | Beta-carotene, resistant starch | Beta-carotene converts to Vitamin A → reduces hepatic stellate cell activation and fibrosis; resistant starch feeds gut bacteria and improves insulin sensitivity |
| Turmeric (as a spice/root) | Curcumin | Inhibits NF-κB, TNF-α, and TGF-β → reduces liver inflammation AND fibrosis; improves insulin signaling; one of the best-studied natural hepatoprotectants |
| Tomatoes | Lycopene, Vitamin C | Lycopene reduces lipid peroxidation and hepatic fat accumulation; strong antioxidant effect on mitochondria |
| Green tea (as a beverage) | EGCG (epigallocatechin gallate), catechins | EGCG inhibits fatty acid synthase (FASN) → reduces de novo lipogenesis; improves insulin sensitivity; reduces liver enzyme levels |
Dietary Pattern Summary
MOST PROTECTIVE: Mediterranean Diet
→ High in: vegetables, fruits, olive oil, legumes, whole grains, fish
→ Low in: red meat, sugar, refined carbs, processed foods
→ Avoid entirely: alcohol, sugary drinks, fructose syrup
The Mediterranean diet specifically reduces liver fat, improves insulin sensitivity, and lowers inflammatory markers — and is the single most recommended dietary pattern for NAFLD by gastroenterology guidelines.
Prognosis
- Simple steatosis: generally benign — 1/3 may remit with modest weight loss
- NASH: progressive — up to 1/3 develop worsening fibrosis over ~5 years
- The most common cause of death in NAFLD is cardiovascular disease, not liver failure — highlighting why controlling the whole metabolic syndrome matters
- NAFLD is now the 2nd leading cause of liver transplant listing in the US
— Goldman-Cecil Medicine; Yamada's Textbook of Gastroenterology; Robbins & Kumar Basic Pathology; Washington Manual of Medical Therapeutics
This is a shared conversation. Sign in to Orris to start your own chat.