Help me with this MRI finding in a 50 year old male with sudden onset unilateral weakness and slurring of speech, know case of dyslipidemia and no other comorbid illness
Reading File
search_medical_text
pontine brainstem infarct MRI findings dysarthria hemiplegia acute ischemic stroke
search_medical_text
acute ischemic stroke management thrombolysis dyslipidemia atherosclerosis
search_medical_image
pontine infarct MRI DWI brainstem stroke axial
GradeResponse
GradeResponse
GradeResponse
MRI Findings & Clinical Analysis
Image Interpretation
The MRI shown is a T2-weighted axial sequence at the level of the posterior fossa/brainstem. The green arrow points to a hyperintense (bright) lesion in the pons (basis pontis / pontine tegmentum), consistent with an acute pontine infarction.
This correlates perfectly with the clinical presentation:
- Sudden onset unilateral weakness → corticospinal tract involvement at the basis pontis
- Dysarthria (slurring of speech) → corticobulbar/pontine involvement
- Known dyslipidemia → atherosclerotic small vessel or basilar artery disease
Diagnosis: Acute Pontine Infarct (Posterior Circulation Ischemic Stroke)
Anatomical Correlation
| Structure Affected | Clinical Deficit |
|---|---|
| Corticospinal tract (basis pontis) | Contralateral hemiplegia/hemiparesis |
| Corticobulbar fibers | Dysarthria |
| If tegmentum involved | Ipsilateral CN VI/VII palsy (check for this) |
| Medial lemniscus | Contralateral hemisensory loss |
Classic lacunar syndromes to consider here:
- Pure Motor Hemiplegia — most common (basis pontis, internal capsule)
- Dysarthria-Clumsy Hand Syndrome — pontine lacune (dysarthria + ipsilateral hand clumsiness)
- Ataxic Hemiparesis — pons or internal capsule
Etiology in This Patient
Given dyslipidemia as the sole risk factor:
- Small vessel disease (lacunar infarct) — lipohyalinosis of small penetrating pontine arteries — most likely
- Atherosclerosis of basilar artery — large vessel disease with branch occlusion
- Cardioembolic — less likely without atrial fibrillation, but must be ruled out
Recommended MRI Protocol
The ideal workup should include:
| Sequence | Purpose |
|---|---|
| DWI + ADC | Confirms acute ischemia (bright DWI, dark ADC = restricted diffusion) |
| T2/FLAIR | Identifies lesion; may be negative in first 6 hours |
| MRA (intracranial) | Evaluate basilar artery stenosis/occlusion |
| MRA (neck) | Vertebral artery dissection or stenosis |
| SWI/GRE | Rule out hemorrhagic component |
Per the literature, early DWI-MRI within 48h misses 10–22% of posterior circulation strokes and up to 50% of small posterior fossa infarcts. If initial DWI is negative but clinical suspicion is high, repeat MRI at 24–72 hours is warranted (Acute Dizziness and Vertigo in the Emergency Department, p. 9).
Imaging Reference — Pontine Infarcts on DWI
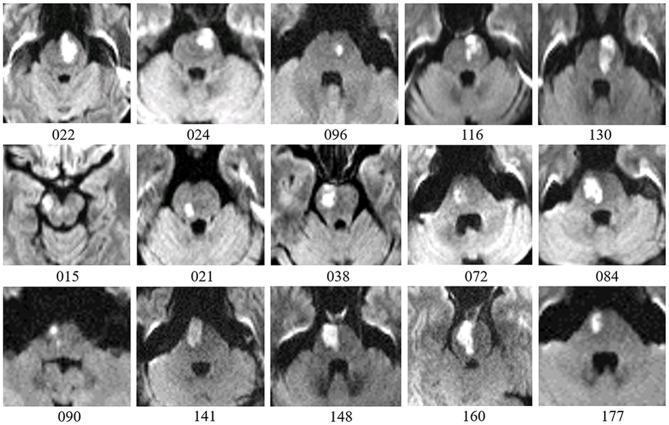
Axial DWI maps showing focal hyperintense pontine lesions (restricted diffusion) in acute brainstem infarction — same pattern expected in this patient.
Acute Management
1. Check thrombolysis eligibility (tPA / Tenecteplase)
- Time of symptom onset — if within 4.5 hours, IV thrombolysis is indicated
- NIHSS score
- BP < 185/110 mmHg required before thrombolysis
- No contraindications (recent surgery, bleeding, anticoagulants)
"Use either tenecteplase or alteplase in patients with acute ischemic stroke who qualify for thrombolysis" — Level B recommendation (Critical Issues in Management of Acute Ischemic Stroke, p. 10)
2. If beyond thrombolysis window or not eligible:
- Dual antiplatelet therapy: Aspirin 300 mg loading + Clopidogrel 75 mg (for minor stroke/TIA — POINT/CHANCE trial)
- Antiplatelet monotherapy for larger strokes
3. Supportive care:
- Admit to stroke unit / ICU monitoring
- Keep BP < 180/105 (permissive hypertension if not thrombolysed)
- NPO + swallowing assessment (dysarthria = aspiration risk)
- Avoid hypoglycemia/hyperglycemia (target glucose 140–180 mg/dL)
- DVT prophylaxis
4. Workup to guide secondary prevention:
- ECG + 72h cardiac monitoring (rule out AF)
- Echocardiogram (rule out cardioembolic source)
- Fasting lipid panel (LDL target < 70 mg/dL in atherosclerotic stroke)
- HbA1c, fasting glucose
- CBC, coagulation, homocysteine
Secondary Prevention
| Intervention | Target/Agent |
|---|---|
| High-intensity statin | Atorvastatin 40–80 mg (LDL < 70 mg/dL) |
| Antiplatelet | Aspirin ± Clopidogrel (based on mechanism) |
| Blood pressure control | < 130/80 mmHg after acute phase |
| Lifestyle | Low-fat diet, aerobic exercise, smoking cessation |
| Anticoagulation | Only if cardioembolic source confirmed (AF) |
Red Flags Requiring Urgent Escalation
- Worsening deficits → evolving basilar artery occlusion → mechanical thrombectomy evaluation
- Decreased consciousness → increased ICP, hydrocephalus
- Bilateral signs → basilar artery thrombosis (life-threatening)
Bottom line: This is an acute pontine ischemic infarct in a 50-year-old male with dyslipidemia as the primary modifiable risk factor. Immediate priorities are confirming the diagnosis with DWI sequences, assessing thrombolysis eligibility, and initiating stroke unit care with secondary prevention planning centered on aggressive statin therapy and antiplatelet treatment.
This is a shared conversation. Sign in to Orris to start your own chat.