How can you differentiate whether it is hemorrhoids or prolapse
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive breakdown of how to differentiate hemorrhoids from rectal prolapse:
Differentiating Hemorrhoids from Rectal Prolapse
The single most important distinguishing feature is the orientation of the mucosal folds on the protruding tissue.
Key Differentiating Feature: Fold Pattern
| Feature | Prolapsed Hemorrhoids | Full-Thickness Rectal Prolapse |
|---|---|---|
| Mucosal folds | Radial (like spokes of a wheel), with grooves along hemorrhoid cushions | Concentric (ring-shaped, like onion layers) |
| Appearance | Separate cushion-like masses at 3, 7, 11 o'clock positions | Symmetrical, ball-like red mass |
| Sulcus | No sulcus between tissue and anus | A sulcus (groove) can be palpated between the extruded bowel and anus |
| Wall thickness on DRE | Thin wall | Thick muscular wall |
| Anal sphincter tone | Usually normal | Lax, patulous anus with decreased tone |
| Extent | Rarely extends >5 cm beyond the anal verge | Can protrude considerably further |
| Associated structures | May be thrombosed, skin tags present | May have anterior solitary rectal ulcer (10–15% of cases) |
"The full-thickness rectal prolapse has concentric folds, whereas prolapsed hemorrhoids or rectal mucosa is characterized by radial folds, with grooves along hemorrhoid cushions." — Sabiston Textbook of Surgery, block 23
"It is important to differentiate the circumferential appearance of a full-thickness rectal prolapse from the radial nature of prolapsing hemorrhoids." — Harrison's Principles of Internal Medicine 22E
Clinical Picture of Full-Thickness Rectal Prolapse
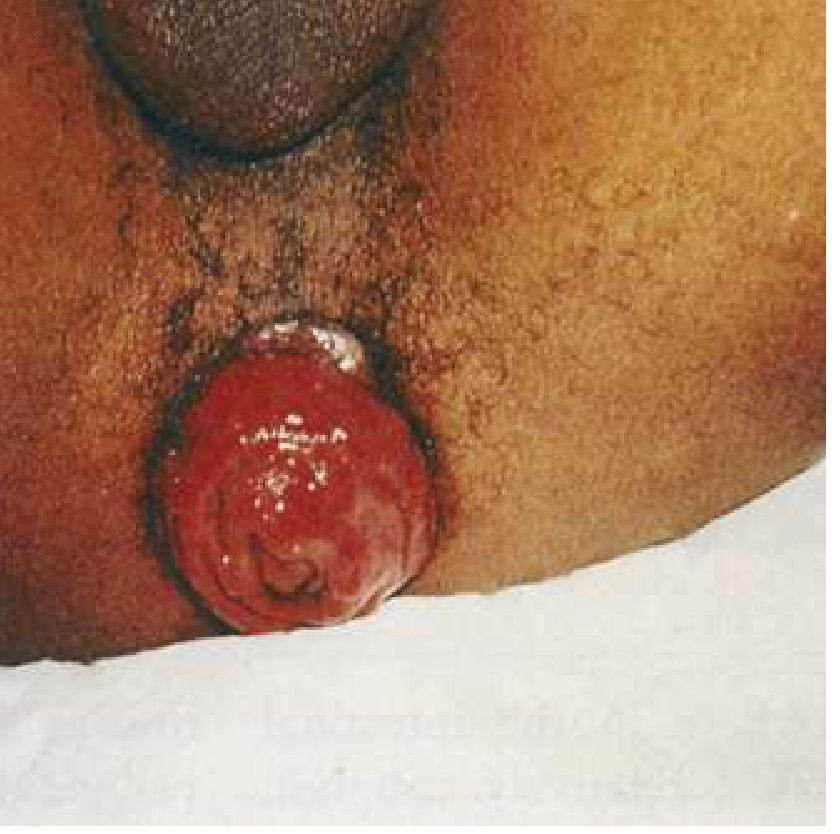
Rectal prolapse — note the concentric, circumferential mucosal folds of the protruding mass.
Complete rectal prolapse (procidentia) is most common in older women and is associated with:
- A lax, patulous anus with weak sphincter tone
- Possible fecal incontinence, mucoid/bloody discharge
- Protrusion during defecation, coughing, or straining
- Often coexists with uterine prolapse or cystocele
— Rosen's Emergency Medicine, block 14
Hemorrhoid Classification (for context)
Prolapsing hemorrhoids are graded by degree of protrusion:
| Grade | Description |
|---|---|
| I | Enlargement with bleeding, no protrusion |
| II | Protrude but reduce spontaneously |
| III | Protrude, require manual reduction |
| IV | Irreducible |
Hemorrhoidal bleeding is painless bright red blood. Pain, if present, usually indicates a thrombosed external hemorrhoid.
— Harrison's Principles of Internal Medicine 22E, block 36
Examination Approach
- Inspect at rest — look for a patulous anus (suggests complete prolapse)
- Ask the patient to strain — this brings out the prolapse
- Observe fold pattern — concentric = rectal prolapse; radial = hemorrhoids
- Digital rectal exam — feel wall thickness and probe for a sulcus
- Anoscopy/proctoscopy — erythema at 5–6 cm suggests the leading edge of a prolapse; also detects solitary rectal ulcer
If examination in the office is unrevealing, the patient can be asked to strain at home and photograph the protrusion. Defecography or MRI defecography can confirm rectal prolapse and identify coexisting disorders (rectocele, sigmoidocele, cystocele).
— Sabiston Textbook of Surgery, block 23
Special Note in Children
In children under 3 years, mucosal prolapse is common and often mistaken by parents for a hemorrhoid. Key clue: the mucosal prolapse in children appears as a painless, maroon-colored mass, rarely extending more than 5 cm, and is frequently associated with cystic fibrosis, malnutrition, or parasitic infection — all of which must be screened for.
— Tintinalli's Emergency Medicine, block 7
This is a shared conversation. Sign in to Orris to start your own chat.