Define pain. Difference between preventive and preemptive analgesia
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Here is a comprehensive answer synthesized from authoritative anesthesia and physiology textbooks.
Definition of Pain
The International Association for the Study of Pain (IASP) defines pain as:
"An unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage."
Key notes on this definition:
- Pain is always a personal experience — it has both sensory and emotional/psychological components.
- Pain can exist in the absence of tissue damage or identifiable pathophysiology. If a patient reports an experience in the same way as pain caused by tissue damage, it should be accepted as pain.
- Pain is distinct from nociception, which is defined as the neural process of encoding noxious stimuli (neurophysiologic activity in peripheral sensory neurons and higher nociceptive pathways). Nociception is not synonymous with pain.
Classification of Pain
| Type | Features |
|---|---|
| Acute (physiologic) | Sudden onset, recedes with healing; serves a protective role ("good pain") |
| Chronic (pathologic) | Persists >3 months; often refractory to NSAIDs/opioids; may be inflammatory or neuropathic |
| Neuropathic | Results from nerve injury; features burning, shooting pain, allodynia, hyperalgesia |
— Ganong's Review of Medical Physiology, 26e | Miller's Anesthesia, 10e
Preemptive vs. Preventive Analgesia
Preemptive Analgesia (older concept)
- Defined as an analgesic intervention administered before surgical incision that is more effective at pain relief than the same intervention given after surgery.
- The rationale: blocking nociceptive input before tissue injury prevents the establishment of central sensitization in the dorsal horn (wind-up, facilitation, expansion of receptive fields, long-term potentiation).
- Clinical reality: Randomized controlled trials have had mixed results. A single analgesic treatment before incision does not reduce postoperative pain beyond the expected duration of the analgesic effect. Once the block diminishes, surgical injury can reinitiate central sensitization.
- This terminology is now considered obsolete and has largely fallen out of favor.
Preventive Analgesia (current concept)
- Defined as any antinociceptive regimen delivered at any time during the perioperative period that attenuates pain-induced sensitization.
- Timing is not the defining criterion — the intervention can be preoperative, intraoperative, or postoperative.
- The focus is on intensity and duration of the analgesic intervention, not when it starts.
- Goal: block the development of sustained chronic pain by preventing NMDA receptor activation in the dorsal horn.
Three Critical Principles for Successful Preventive Analgesia:
- Depth: The analgesia must be adequate to block all nociceptive input during surgery.
- Extent: The technique must cover the entire surgical field.
- Duration: The analgesia must encompass both the surgical and post-surgical periods.
Patients with pre-existing chronic pain may respond less well due to pre-existing nervous system sensitization.
Summary Comparison
| Feature | Preemptive Analgesia | Preventive Analgesia |
|---|---|---|
| Timing | Must be before incision | Any time perioperatively |
| Mechanism targeted | Central sensitization from incision only | Central sensitization from incision + inflammation + postoperative pain |
| Key parameter | Timing of intervention | Intensity + duration of intervention |
| Clinical evidence | Mixed/negative trials | Broader, more clinically applicable |
| Current status | Obsolete terminology | Current standard concept |
Maximal clinical benefit is observed when there is complete multi-segmental blockade of noxious stimuli extended into the postoperative period, using intensive multimodal analgesic regimens.
— Miller's Anesthesia 10e | Barash Clinical Anesthesia 9e | Cummings Otolaryngology
Define pain. Difference between preventive and preemptive analgesia
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Here is a comprehensive, textbook-sourced answer.
Definition of Pain
The International Association for the Study of Pain (IASP) defines pain as:
"An unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage."
Key points in the definition:
- Pain is always a personal experience — it has both sensory (physical) and emotional/psychological dimensions.
- Pain can occur in the absence of tissue damage or identifiable pathophysiology. If a patient reports an experience consistent with pain, it must be accepted as pain.
- Pain is distinct from nociception: nociception is the neural process of encoding noxious stimuli — neurophysiologic activity in peripheral nociceptors and higher pathways. Nociception is not synonymous with pain.
Classification:
| Type | Characteristics |
|---|---|
| Acute (physiologic) | Sudden onset; recedes with healing; serves a protective role ("good pain") |
| Chronic (pathologic) | Persists or recurs for >3 months; often refractory to NSAIDs/opioids |
| Inflammatory | From tissue inflammation; mediated by bradykinin, prostaglandins, substance P, histamine |
| Neuropathic | From nerve injury (cutting, traction, compression); burning/shooting quality, allodynia, hyperalgesia |
— Miller's Anesthesia 10e; Ganong's Review of Medical Physiology 26e
Preemptive vs. Preventive Analgesia
Preemptive Analgesia (older, now obsolete concept)
Definition: An analgesic intervention administered before surgical incision that is more effective at relieving postoperative pain than the same intervention given after surgery.
Rationale: Blocking nociceptive input before tissue injury was hypothesized to prevent the establishment of central sensitization in the dorsal horn — thereby preventing pain hypersensitivity, reducing hyperalgesia, and reducing the magnitude and duration of postoperative pain.
Why it failed clinically:
- A single analgesic treatment before incision does not reduce postoperative pain beyond the expected duration of the analgesic effect.
- Once the block diminishes, surgical injury can reinitiate central sensitization.
- Randomized controlled trials have had mixed/negative results.
- The concept is now considered obsolete and has fallen out of favor.
Preventive Analgesia (current concept)
Definition: Any antinociceptive regimen delivered at any time during the perioperative period (preoperative, intraoperative, or postoperative) that attenuates pain-induced sensitization.
Key distinction from preemptive: The focus is not on timing but on the intensity and duration of the analgesic intervention.
Goal: Block the development of sustained chronic pain by preventing NMDA receptor activation in the dorsal horn — the mechanism underlying wind-up, facilitation, central sensitization, expansion of receptive fields, and long-term potentiation.
Three critical principles for success:
- Depth — Adequate to block all nociceptive input during surgery
- Extent — Must cover the entire surgical field
- Duration — Must encompass both the surgical and postsurgical periods
An intervention before incision is not preventive if it is incomplete or insufficient to prevent central sensitization.
Important caveat: Patients with pre-existing chronic pain and pre-established central sensitization may respond less well to preventive analgesia techniques.
Maximal benefit is achieved with complete multi-segmental blockade of noxious stimuli extended into the postoperative period, using intensive multimodal analgesic regimens.
Summary Comparison
| Feature | Preemptive Analgesia | Preventive Analgesia |
|---|---|---|
| Timing | Must be before incision | Any perioperative time |
| Focus | Timing of intervention | Intensity + duration |
| Mechanism targeted | Central sensitization from incision only | Central sensitization from incision + inflammation + postoperative period |
| Clinical evidence | Mixed/negative trials | Broader, more clinically viable |
| Status | Obsolete | Current standard |
| NMDA pathway | Implied | Explicitly targeted |
— Barash Clinical Anesthesia 9e; Miller's Anesthesia 10e; Cummings Otolaryngology
Anaesthetic management of prolapsed intervertebral disc patient
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Here is a comprehensive, textbook-sourced account of the anaesthetic management of a prolapsed intervertebral disc (PIVD) patient.
Anaesthetic Management of Prolapsed Intervertebral Disc (PIVD)
Background
Prolapse of an intervertebral disc most often occurs at L4–L5 or L5–S1 in the lumbar spine, or C5–C6 in the cervical spine. Compression may arise from disc protrusion or osteophytic bone encroaching on the spinal canal or intervertebral foramen. Surgical options include microdiscectomy, laminectomy, or spinal fusion.
1. Preoperative Assessment
Neurological evaluation:
- Document existing neurological deficits (motor weakness, sensory loss, bladder/bowel dysfunction) before surgery — this forms the baseline for postoperative comparison.
- Assess level and completeness of any neurological compromise (ASIA grading if cord involvement is suspected).
Airway assessment:
- Critical in cervical disc disease: assess neck mobility, range of motion, and any cervical instability.
- Restricted neck movement from disease, traction, or cervical collars may complicate intubation.
- Plan for video laryngoscopy or awake fiberoptic intubation if cervical instability is present; if awake intubation is planned, assess patient cooperation.
Cardiovascular and respiratory:
- High cervical lesions (C4 and above) may impair phrenic nerve function → reduced vital capacity (up to 25% loss at C4 level).
- Intercostal muscle function may be impaired by thoracic/upper cervical injuries.
- Evaluate for comorbidities: hypertension, diabetes, obesity (all increase perioperative risk).
Investigations:
- Baseline hemoglobin, coagulation profile, renal and hepatic function.
- Imaging review: MRI/CT to understand level, extent of compression, and surgical approach.
— Miller's Anesthesia 10e; Morgan & Mikhail's Clinical Anesthesiology 7e; Barash Clinical Anesthesia 9e
2. Intraoperative Management
Anaesthetic Technique
General anaesthesia (GA) is standard for most disc surgeries (discectomy, laminectomy).
- Induction: Standard IV induction (propofol + opioid).
- Airway: Endotracheal intubation is preferred, given prone positioning.
- For cervical disc disease: video laryngoscopy or awake fiberoptic intubation if cervical spine is unstable; in-line stabilisation is used if intubating after induction.
- Maintenance: Total intravenous anaesthesia (TIVA) with propofol + opioid infusion is preferred when intraoperative neurophysiological monitoring (IOM) is employed, as deep inhalational agents impair evoked potential signals.
Regional anaesthesia (spinal/epidural) may be considered for selected lumbar procedures but GA dominates in practice due to positioning requirements.
Positioning
This is one of the most critical steps in spine surgery.
- Lumbar disc surgery: Prone position (most common).
- Cervical disc surgery (anterior approach): Supine position — easier airway management but risks injury to trachea, oesophagus, recurrent laryngeal nerve, sympathetic chain, carotid artery, or jugular vein.
- Lateral decubitus may be used for some lumbar procedures.
Key concerns during prone positioning:
- Induction and intubation in supine → then carefully turned prone; neutral neck position must be maintained throughout.
- Head supported on a cushioned holder, foam headrest, or secured with pins/tongs — face must be periodically checked to ensure no pressure on eyes, nose, or ears (risk of corneal abrasion, retinal ischaemia).
- Chest rolls or a frame must allow the abdomen to hang freely — abdominal compression raises epidural venous pressure → increased blood loss and risk of haemorrhage.
- Turning prone can cause hypotension — have vasopressors and IV access ready beforehand.
- Arms: tucked at sides or extended with elbows slightly flexed (avoid excessive shoulder abduction).
Monitoring
Standard monitoring: ECG, SpO₂, ETCO₂, temperature, urine output.
Additional monitoring:
- Intra-arterial blood pressure: mandatory when major blood loss is anticipated or pre-existing cardiac disease exists. Sudden catastrophic haemorrhage from great vessel injury (thoracic/lumbar procedures) can occur.
- Intraoperative neurophysiological monitoring (IOM):
- Somatosensory Evoked Potentials (SSEPs): Monitor dorsal column (sensory) integrity.
- Motor Evoked Potentials (MEPs): Monitor anterior (motor) cord integrity.
- Both require TIVA; avoid high-dose inhalational agents and neuromuscular blockers.
- Intraoperative wake-up test (Stagnara test): Nitrous oxide/narcotic or TIVA; patient briefly awakened to test voluntary motor function after spinal distraction — increasingly replaced by continuous IOM.
Blood Conservation
Multilevel surgery, fusion, and instrumentation carry risk of significant blood loss:
- Cell salvage (intraoperative autologous blood salvage) — reduces allogeneic transfusions in non-infective, non-tumour cases.
- Tranexamic acid (antifibrinolytic) — reduces bleeding with minimal thrombotic risk.
- Deliberate hypotension — historically used but now largely abandoned due to risk of perioperative vision loss (POVL) and neurological injury.
- Coagulation parameters, Hb, and platelets should be monitored regularly.
3. Perioperative Vision Loss (POVL)
A potentially devastating complication unique to prone spine surgery:
- Causes: Posterior ischaemic optic neuropathy (most common), central retinal artery occlusion, cortical blindness.
- Risk factors: Male sex, obesity, Wilson frame use, prolonged surgery, high blood loss, prolonged head-down position, diabetes, smoking.
- Prevention: Avoid hypotension, excessive blood loss; periodic eye pressure checks; colloid use may be protective.
- High-risk patients must be counselled preoperatively about this risk (ASA Practice Advisory).
4. Postoperative Care
Pain management:
- Postoperative pain after spine surgery can be severe and challenging.
- Multimodal analgesia: NSAIDs, paracetamol, regional nerve blocks (fascial plane blocks), and opioids.
- A single intraoperative dose of methadone has been shown to reduce postoperative analgesic requirements, improve pain scores, and provide analgesia lasting months.
- Epidural analgesia may be used in selected patients.
Neurological assessment:
- Reassess motor and sensory function as soon as the patient is awake — compare to preoperative baseline.
- New deficits require urgent imaging to rule out epidural haematoma or surgical complication.
DVT prophylaxis:
- Prone position, deliberate hypotension, and immobility increase DVT/PE risk.
- Lumbar fusion carries up to 4% symptomatic DVT and 2% PE incidence.
- Anticoagulation must be balanced against risk of epidural haematoma.
- Consider IVC filter in high-risk patients where anticoagulation is contraindicated.
Airway caution post-cervical surgery:
- Airway and facial oedema can develop after prolonged prone or head-down positioning — re-intubation may be significantly more difficult than at induction.
Summary Table
| Phase | Key Actions |
|---|---|
| Preop | Neurological baseline, airway assessment (especially cervical), imaging review, comorbidity optimisation |
| Induction | Careful intubation (FOB/video laryngoscopy if cervical instability), IV induction |
| Positioning | Prone (lumbar), ensure free abdomen, eye/pressure point protection, neutral neck |
| Maintenance | TIVA preferred (for IOM), avoid deep inhalational agents + NMBs |
| Monitoring | Arterial line, SSEP + MEP if cord at risk, frequent labs |
| Blood conservation | Cell salvage, tranexamic acid, avoid deliberate hypotension |
| Postop | Neurological reassessment, multimodal analgesia, DVT prophylaxis, airway vigilance |
— Morgan & Mikhail's Clinical Anesthesiology 7e; Miller's Anesthesia 10e; Barash Clinical Anesthesia 9e
Causes of low back pain
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Finding Sources
Reading File
Reading File
Here is a comprehensive, textbook-sourced account of the causes of low back pain.
Causes of Low Back Pain
Up to 97% of low back pain is mechanical or idiopathic in origin. Only 15% of patients have a specific identifiable cause. The remaining minority have non-mechanical spinal disease or visceral referred pain.
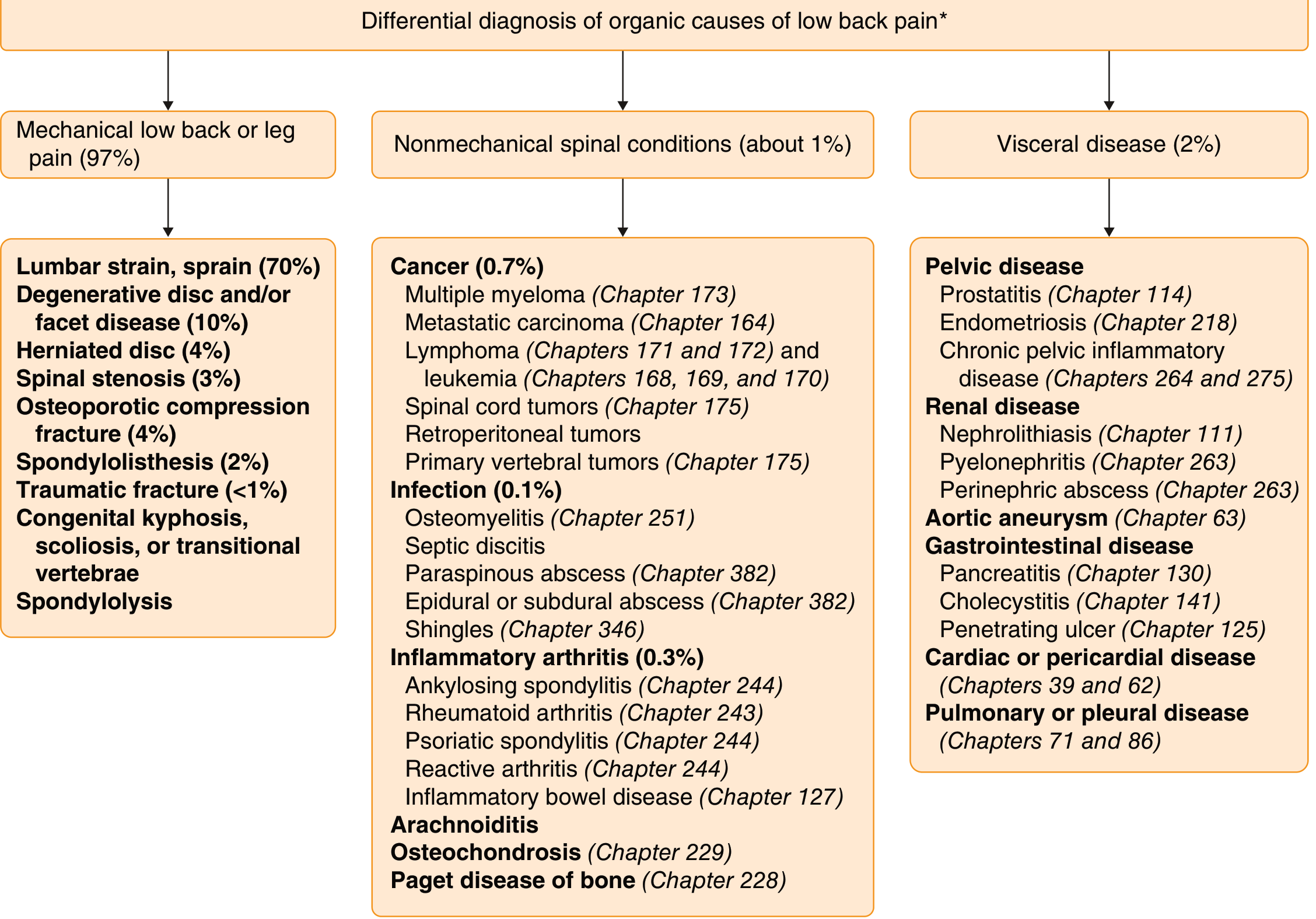
Classification
Low back pain is broadly divided into three categories:
1. Mechanical Low Back Pain (97%)
The most common category — pain arising from structural elements of the spine.
| Cause | Approximate Frequency |
|---|---|
| Lumbar muscle strain/sprain | ~70% |
| Degenerative disc and/or facet joint disease | ~10% |
| Herniated nucleus pulposus (disc prolapse) | ~4% |
| Osteoporotic compression fracture | ~4% |
| Spinal stenosis | ~3% |
| Spondylolisthesis | ~2% |
| Traumatic fracture | <1% |
| Congenital (kyphosis, scoliosis, transitional vertebrae, spondylolysis) | Rare |
Key features of mechanical LBP:
- Worsens with activity, improves with rest
- Acute onset, often following exertion
- No systemic symptoms
Additional mechanical/neuropathic causes to consider:
- Lateral recess stenosis — from spondylotic spurs, facet hypertrophy; can cause sciatica not relieved by disc surgery
- Synovial (facet joint) cysts — may compress nerve roots in the foramen
- Tarlov cysts — perineural sheath dilatations of sacral roots
- Piriformis syndrome — entrapment of the sciatic nerve by the piriformis muscle; controversial entity
- Sacroiliac joint inflammation
- Arachnoiditis — after spine surgery or intrathecal foreign substance exposure; causes chronic back and radicular pain
2. Non-Mechanical Spinal Conditions (~1%)
These are serious causes requiring urgent evaluation.
A. Malignancy (0.7%)
- Multiple myeloma
- Metastatic carcinoma (breast, prostate, lung)
- Lymphoma / Leukaemia
- Spinal cord tumours (primary)
- Retroperitoneal tumours
- Cauda equina compression from epidural tumour deposits (prostate, breast cancer, myeloma)
- Lumbar plexus infiltration (lymphoma, neurofibrosarcoma)
B. Infection (0.1%)
- Vertebral osteomyelitis
- Septic discitis — severe back pain worsened by movement
- Paraspinous/epidural/subdural abscess
- Herpes zoster (acute radicular pain may precede the rash)
- CMV infection (in AIDS), Lyme disease (Bannwarth syndrome), neoplastic meningitis
C. Inflammatory Arthritis (0.3%)
- Ankylosing spondylitis — insidious onset, morning stiffness, night pain, responds to NSAIDs
- Psoriatic spondylitis
- Reactive arthritis
- Rheumatoid arthritis
- Inflammatory bowel disease–associated spondylitis
Key distinguishing feature: Inflammatory LBP awakens the patient from sleep; improves with exercise, worsens with rest.
D. Other Non-Mechanical Spinal Causes
- Osteochondrosis
- Paget's disease of bone
- Arachnoiditis
3. Visceral Referred Pain (~2%)
Pain referred from abdominal and pelvic organs to the back — no primary spinal pathology.
| System | Causes |
|---|---|
| Vascular | Abdominal aortic aneurysm (mid/low back, radiates to hips), aortic dissection |
| Renal | Nephrolithiasis (colicky flank/costovertebral angle), pyelonephritis, perinephric abscess |
| Gynaecological | Endometriosis, ectopic pregnancy, pelvic inflammatory disease, ovarian cyst/carcinoma |
| Gastrointestinal | Pancreatitis (L1 level), diverticulitis, cholecystitis (mid-thoracic), penetrating peptic ulcer |
| Pelvic | Prostatitis, chronic pelvic inflammatory disease |
| Cardiac/Pericardial | Rarely referred to low back |
| Pulmonary/Pleural | Pleurisy, pulmonary embolism |
4. Neurological/Other Causes
- Guillain-Barré syndrome — back and radicular pain may precede weakness
- Lumbosacral plexus neuritis (Wartenberg plexitis) — akin to brachial neuritis
- Diabetic lumbosacral radiculoplexopathy
- Sickle cell anaemia — severe pain crises involving the spine
- Catamenial sciatica — endometriosis involving the sciatic nerve, temporal with menses
- Psychogenic/depression — diffuse, emotionally described back pain; seen in 20–50% of depressed patients
Red Flags in Low Back Pain
Features requiring urgent investigation to exclude serious pathology:
| Red Flag | Possible Cause |
|---|---|
| Cauda equina syndrome (urinary retention, faecal incontinence, saddle anaesthesia) | Emergency surgical cause |
| Severe, unremitting, non-mechanical pain (worse at night, lying down) | Infection or tumour |
| Significant trauma | Fracture |
| Unexplained weight loss, fever, HIV, history of cancer | Infection or malignancy |
| IV drug use or prolonged steroid use | Infection or osteoporotic fracture |
| Widespread neurological signs | Tumour or neurological disease |
| Age >50–65 with first episode of severe back pain | Malignancy, fracture |
| Duration >6 weeks without improvement | Serious underlying cause |
— Goldman-Cecil Medicine; Bradley & Daroff's Neurology in Clinical Practice; Adams & Victor's Principles of Neurology; Grainger & Allison's Diagnostic Radiology; Textbook of Family Medicine 9e
This is a shared conversation. Sign in to Orris to start your own chat.