Eczema in detail with case study and detail management
Reading File
search_medical_text
atopic dermatitis eczema pathophysiology etiology classification
search_medical_text
eczema diagnosis clinical features treatment management guidelines
search_medical_image
eczema atopic dermatitis skin lesions clinical appearance
GradeResponse
GradeResponse
GradeResponse
search_medical_text
atopic dermatitis topical corticosteroids calcineurin inhibitors biologics dupilumab management stepwise
search_medical_text
atopic dermatitis case study pediatric adult severity scoring SCORAD EASI
I have sufficient retrieved content plus comprehensive clinical knowledge to deliver a thorough answer.
Eczema (Atopic Dermatitis) — Comprehensive Review
1. Definition & Overview
Eczema is a type of dermatitis — both terms are used interchangeably (e.g., "atopic eczema" = "atopic dermatitis," AD). The hallmark histologic finding is spongiosis (intercellular edema of the epidermis). Eczema is the final common expression of multiple disorders, not a single disease entity.
Harrison's Principles of Internal Medicine, 21st Ed., p. 1520
Primary lesions: erythematous macules, papules, vesicles coalescing into patches/plaques
Secondary lesions: weeping, crusting, excoriation (from scratching), lichenification (chronic disease)
Secondary lesions: weeping, crusting, excoriation (from scratching), lichenification (chronic disease)
2. Classification of Eczema
| Type | Key Features |
|---|---|
| Atopic Dermatitis (AD) | Most common; associated with asthma, allergic rhinitis, food allergy (atopic triad) |
| Contact Dermatitis | Irritant (ICD) or Allergic (ACD); defined exposure history |
| Nummular Eczema | Coin-shaped lesions; often on limbs |
| Dyshidrotic Eczema | Vesicles on palms, soles, lateral fingers |
| Seborrheic Dermatitis | Greasy scales on scalp, nasolabial folds; Malassezia-linked |
| Stasis Dermatitis | Lower legs; linked to venous insufficiency |
| Neurodermatitis (Lichen simplex chronicus) | Lichenified plaque from repetitive scratching |
3. Epidemiology
- Affects ~15–30% of children and 2–10% of adults globally
- Prevalence increasing in developed nations (hygiene hypothesis)
- Onset: >50% present before age 1, >85% before age 5
- ~70% have spontaneous remission by adolescence; 30% persist into adulthood
- Equal sex prevalence in childhood; slight female predominance in adults
4. Etiology & Risk Factors
Genetic Factors
- Filaggrin (FLG) gene mutations — most significant genetic risk factor; impairs skin barrier integrity (loss-of-function variants in ~30% of European AD patients)
- Family history of AD, asthma, or allergic rhinitis
- HLA associations
Immunologic Factors
- Th2-skewed immune response in acute phase → elevated IL-4, IL-5, IL-13, IL-31, IgE
- Th1 response in chronic phase
- Defective regulatory T-cell function
- Elevated serum IgE in ~80% of patients
Environmental Factors
- Aeroallergens: house dust mites, pollen, pet dander
- Food allergens (especially in children): eggs, milk, peanuts, wheat, soy
- Harsh soaps, detergents, wool fabrics, sweat
- Climate: low humidity, extreme temperatures
- Stress, infections (Staph. aureus colonization)
The "Outside-In" vs "Inside-Out" Debate
- Outside-In: Barrier defect (FLG mutation) allows allergen penetration → sensitization → inflammation
- Inside-Out: Immune dysregulation is primary → leads to barrier dysfunction
- Current consensus: both operate simultaneously
5. Pathophysiology
Genetic susceptibility (FLG mutation, etc.)
↓
Defective skin barrier
↓
Increased transepidermal water loss (TEWL)
↓
Allergen/irritant/microbe penetration
↓
Keratinocyte release of TSLP, IL-25, IL-33
↓
Activation of innate lymphoid cells (ILC2) + dendritic cells
↓
Th2 polarization → IL-4, IL-13 → IgE class switching
→ IL-31 → PRURITUS (key mediator)
→ IL-5 → eosinophilia
↓
Chronic: Th2 + Th22 + Th1 mixed → lichenification
Staphylococcus aureus colonizes >90% of AD skin and perpetuates inflammation via:
- Superantigen release (SAgs)
- Staphylococcal proteases disrupting FLG
- Toxin-induced Th2 skewing
6. Clinical Features & Diagnosis
Atopic Dermatitis: Update on Skin-Directed Management, p. 2
The diagnosis of AD is primarily clinical, based on characteristic features:
Diagnostic Criteria (Hanifin & Rajka / UK Working Party)
Major criteria (must have ≥3):
- Pruritus (itch is mandatory)
- Typical morphology and distribution (flexural involvement in adults; face/extensor in infants)
- Chronic or chronically relapsing course
- Personal or family history of atopy
Minor criteria (supporting): xerosis, ichthyosis, elevated IgE, early age of onset, food intolerance, Dennie-Morgan lines, keratoconus, anterior subcapsular cataracts, pityriasis alba, etc.
Age-Based Distribution
| Age Group | Typical Distribution |
|---|---|
| Infant (<2 yr) | Cheeks, scalp, trunk, extensor limbs |
| Childhood (2–12 yr) | Flexural creases (antecubital, popliteal fossa), wrists, ankles |
| Adolescent/Adult | Flexural areas, hands, face, neck, upper chest |
Important: In darkly pigmented skin, erythema may be subtle; dyspigmentation and follicular eczema are more prominent features. (AD: Update on Skin-Directed Management, p. 2)
Clinical Image
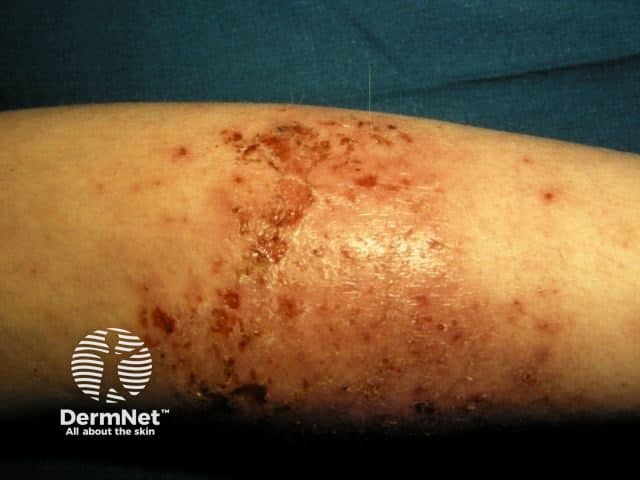
7. Severity Assessment
SCORAD (SCORing Atopic Dermatitis)
- Combines extent (rule of nines), intensity (6 items: erythema, edema, oozing, excoriation, lichenification, dryness), and subjective symptoms (itch, sleep loss)
- Score: <25 = mild, 25–50 = moderate, >50 = severe
EASI (Eczema Area and Severity Index)
- Assesses 4 body regions × 4 signs (erythema, edema/papulation, excoriation, lichenification)
- Range 0–72; widely used in clinical trials
IGA (Investigator's Global Assessment)
- 5-point scale (0 = clear, 1 = almost clear, 2 = mild, 3 = moderate, 4 = severe)
- Used as primary endpoint in drug trials
POEM (Patient-Oriented Eczema Measure)
- 7-question patient-reported outcome; most useful for real-world monitoring
8. Investigations
| Investigation | Purpose |
|---|---|
| Serum IgE | Elevated in ~80%; supports atopic diathesis |
| Specific IgE / skin prick test | Identify specific allergens |
| Patch testing | Rule out allergic contact dermatitis |
| Skin swab/culture | Identify S. aureus or secondary infection |
| CBC with differential | Peripheral eosinophilia common |
| Skin biopsy | Usually not needed; shows spongiosis, lymphocytic infiltrate |
| Thyroid function | Rule out exacerbating thyroid disease |
| Serum thymus and activation-regulated chemokine (TARC/CCL17) | Research/monitoring biomarker |
9. Differential Diagnosis
| Condition | Distinguishing Features |
|---|---|
| Psoriasis | Well-demarcated silvery plaques; extensor surfaces; nail pitting |
| Contact dermatitis | Defined exposure; patch test positive; sharp geometric borders |
| Scabies | Burrows; interdigital webs; nocturnal itch; contagious |
| Seborrheic dermatitis | Greasy yellow scales; scalp/face/chest |
| Tinea corporis | Annular lesion; KOH positive |
| Mycosis fungoides | Refractory; atypical lymphocytes on biopsy |
| Ichthyosis | No pruritus; generalized scaling; FLG mutation |
| Wiskott-Aldrich syndrome | Eczema + thrombocytopenia + immunodeficiency (children) |
10. Management
Management follows a stepwise approach guided by disease severity.
Step 1 — Education & Trigger Avoidance (ALL patients)
- Patient/parent education on chronic disease course
- Identify and avoid personal triggers (allergens, irritants, stress)
- Avoid wool, harsh soaps, extreme temperatures
- Nail cutting to reduce scratch damage
Step 2 — Baseline Skincare (Emollients)
- Emollients are the cornerstone of all AD management
- Apply liberally (at least 250–500 g/week in adults) and frequently (2–3×/day)
- Best applied within 3 minutes of bathing ("soak and seal")
- Types: ointments (most occlusive, best for dry skin), creams, lotions
- Reduces TEWL, restores barrier, decreases flare frequency
- Preferred: fragrance-free, preservative-free formulations
Step 3 — Topical Anti-inflammatory Therapy
Topical Corticosteroids (TCS) — First-line for flares
| Potency Class | Examples | Site of Use |
|---|---|---|
| Mild (Class 1) | Hydrocortisone 1% | Face, genitals, skin folds, infants |
| Moderate (Class 2-3) | Betamethasone valerate 0.025–0.1%, Clobetasone butyrate | Trunk, limbs |
| Potent (Class 4) | Mometasone furoate 0.1%, Betamethasone valerate 0.1% | Trunk, limbs, palms |
| Very Potent (Class 5) | Clobetasol propionate 0.05% | Lichenified plaques; short-term only |
Side effects: skin atrophy, striae, telangiectasias, tachyphylaxis, HPA suppression (with extensive use)
Proactive therapy: applying TCS 2×/week to previously affected sites reduces flare frequency.
Topical Calcineurin Inhibitors (TCIs) — Steroid-sparing
- Tacrolimus 0.03% / 0.1% ointment — moderate-to-severe AD; approved ≥2 years
- Pimecrolimus 1% cream — mild-to-moderate AD; approved ≥2 years
- Preferred for: face, eyelids, skin folds, genitalia (sensitive sites)
- No skin atrophy risk
- Side effect: transient burning/stinging on first application
- Black box warning: theoretical malignancy risk (not proven in long-term studies)
Topical PDE4 Inhibitors
- Crisaborole 2% ointment — mild-to-moderate AD; approved ≥3 months
- Non-steroidal; inhibits PDE4 → ↓ cAMP degradation → ↓ inflammatory cytokines
Topical JAK Inhibitors (newer)
- Ruxolitinib 1.5% cream — mild-to-moderate AD; approved ≥12 years
- Fast onset of itch relief; safe short-term profile
Step 4 — Adjunct Therapies
| Therapy | Role |
|---|---|
| Wet wrap therapy | Flare management; TCS under damp bandage |
| Antimicrobials | S. aureus infection: topical mupirocin or oral flucloxacillin/cephalexin |
| Antihistamines | Sedating (hydroxyzine) for sleep disruption; limited anti-itch efficacy |
| Bleach baths | Sodium hypochlorite 0.005% (½ tsp bleach per gallon) — reduces S. aureus |
| Phototherapy | Narrowband UVB (NB-UVB) — moderate-to-severe, inadequate response to topicals |
Step 5 — Systemic Therapy (Moderate-to-Severe)
Biologics (Targeted)
| Drug | Mechanism | Approval |
|---|---|---|
| Dupilumab (Dupixent) | Anti-IL-4Rα → blocks IL-4 + IL-13 | ≥6 months (injection q2w); gold standard |
| Tralokinumab (Adtralza) | Anti-IL-13 | Adults ≥18 years |
| Lebrikizumab (Ebglyss) | Anti-IL-13 | Adults ≥18 years |
| Cendakimab | Anti-IL-33R | Phase 3 trials |
Dupilumab is the most established biologic:
- Significant reduction in EASI, IGA, pruritus scores
- Side effects: injection site reactions, conjunctivitis (10–20%), facial redness
- Safe in pregnancy (Category B equivalent)
Oral JAK Inhibitors
| Drug | Mechanism | Notes |
|---|---|---|
| Abrocitinib (Cibinqo) | JAK1 selective | ≥12 years; fast itch relief within days |
| Upadacitinib (Rinvoq) | JAK1 selective | ≥12 years; very efficacious |
| Baricitinib (Olumiant) | JAK1/2 | Adults; also used in RA |
JAK inhibitor precautions: risk of infections (TB screening required), VTE, MACE, malignancy (black box warning); avoid in patients >65, smokers, cardiovascular risk
Conventional Immunosuppressants (when biologics unavailable)
| Drug | Dose | Monitoring |
|---|---|---|
| Cyclosporine | 2.5–5 mg/kg/day | BP, renal function, drug interactions |
| Methotrexate | 10–25 mg/week | LFTs, CBC; slow onset |
| Azathioprine | 1–3 mg/kg/day | TPMT activity before starting |
| Mycophenolate mofetil | 1–3 g/day | CBC, GI side effects |
| Oral corticosteroids | Short course only | Not recommended long-term |
Step 6 — Allergen Immunotherapy
- Subcutaneous or sublingual immunotherapy for house dust mite-sensitized AD
- Emerging evidence; not yet standard of care
11. Management of Special Situations
Infected Eczema (Eczema Herpeticum)
- Caused by HSV-1/2 spreading over eczematous skin
- Clinical: sudden widespread punched-out vesicles/erosions, fever, malaise
- Treatment: IV/oral acyclovir — urgent; can be life-threatening
Eczema in Pregnancy
- Dupilumab: preferred biologic (limited data but favorable safety profile)
- TCS: use lowest effective potency; avoid very potent on large areas
- Avoid systemic retinoids, methotrexate
Eczema in Infants
- Focus on emollients, mild TCS, avoid TCIs in <2 years
- Dupilumab approved from 6 months of age
12. Case Study
Case Presentation
Patient: Maya, 8-year-old girl
Chief Complaint: Severe itching and skin rash for 6 years, worsening over 3 months
Chief Complaint: Severe itching and skin rash for 6 years, worsening over 3 months
History of Present Illness:
Maya first developed eczema at 6 months of age. Her parents report worsening over the past 3 months with intense pruritus disturbing sleep (waking 3–4 times per night), weeping sores on the antecubital fossae and popliteal fossae bilaterally, and a crusted area on the right forearm. Her eczema flares significantly in winter and when she visits her grandparent's home (who owns a cat). She has been using over-the-counter 1% hydrocortisone with minimal benefit.
Maya first developed eczema at 6 months of age. Her parents report worsening over the past 3 months with intense pruritus disturbing sleep (waking 3–4 times per night), weeping sores on the antecubital fossae and popliteal fossae bilaterally, and a crusted area on the right forearm. Her eczema flares significantly in winter and when she visits her grandparent's home (who owns a cat). She has been using over-the-counter 1% hydrocortisone with minimal benefit.
Past Medical History:
- Asthma (on salbutamol PRN, low-dose inhaled corticosteroid)
- Allergic rhinitis (on cetirizine)
- Food allergy: egg (outgrown by age 4)
Family History: Mother has asthma and hay fever; maternal uncle has AD
Medications: Hydrocortisone 1% cream (OTC), cetirizine 5 mg OD, salbutamol inhaler PRN
Allergies: NKDA
Social History: Lives in carpeted house; attends school; no pet at home
Physical Examination
| Parameter | Findings |
|---|---|
| General | Alert, scratching during examination |
| Skin | Widespread erythematous lichenified plaques bilaterally in antecubital/popliteal fossae; crusting and oozing right forearm; excoriation marks on neck and chest; xerosis generalized; Dennie-Morgan folds bilateral |
| Eyes | No conjunctivitis |
| Lymph nodes | Bilateral axillary lymphadenopathy (reactive) |
| Respiratory | Clear to auscultation |
SCORAD Score: 58 (Severe)
POEM Score: 22/28 (Severe)
POEM Score: 22/28 (Severe)
Investigations
| Test | Result |
|---|---|
| Serum IgE | 1,240 IU/mL (elevated; normal <100) |
| CBC | Eosinophilia: 8% (elevated) |
| Skin swab (right forearm) | Staphylococcus aureus — methicillin-sensitive (MSSA) |
| Specific IgE (RAST) | House dust mite: Class 4 (very high); cat dander: Class 3 (high) |
| Patch test | Negative (ruling out ACD) |
Diagnosis
- Severe Atopic Dermatitis (SCORAD 58, POEM 22)
- Secondary bacterial infection — MSSA on right forearm
- Atopic triad — AD + Asthma + Allergic Rhinitis
Management Plan
Immediate (Acute Phase)
Step 1 — Treat Infection First:
- Oral cefalexin 25 mg/kg/day divided q8h for 7 days (MSSA infection)
- Topical mupirocin 2% ointment TDS to right forearm for 5 days
- Bleach baths (0.005% NaOCl) 3×/week to reduce S. aureus burden
Step 2 — Emollient Therapy:
- Fragrance-free emollient ointment (e.g., Epaderm, white soft paraffin) — apply liberally 3–4 times daily
- Soak-and-seal technique after bathing
Step 3 — Topical Anti-inflammatory:
- Mometasone furoate 0.1% cream (moderate-potent) to lichenified body plaques OD for 2 weeks, then proactive 2×/week
- Tacrolimus 0.03% ointment to face, neck, and skin folds BD (steroid-sparing, no atrophy risk)
Escalation (Week 2–4, Inadequate Response to Topicals)
Given SCORAD 58 and failure of adequate topical therapy:
Referral to Pediatric Dermatologist
Dupilumab initiated:
- Loading dose: 600 mg SC (two 300 mg injections), then 300 mg SC every 4 weeks (pediatric dosing, 15–30 kg)
- Counseling: injection technique, watch for conjunctivitis
Narrowband UVB (NB-UVB) as adjunct if dupilumab partially effective
Long-Term Plan
| Domain | Action |
|---|---|
| Trigger avoidance | House dust mite covers for mattress/pillow; HEPA vacuum; avoid cat contact; avoid wool |
| Skincare routine | Daily emollient, mild soap-free cleanser, lukewarm baths |
| Proactive TCS | Mometasone 2×/week to previously affected areas |
| Allergen immunotherapy | Consider house dust mite SCIT/SLIT after age 5 if stable |
| Asthma/AR co-management | Continue inhaled corticosteroid step-up if needed; intranasal steroid for AR |
| Mental health | Screen for anxiety/depression; support groups; school accommodation letter |
| Monitoring | SCORAD + POEM at every visit; review dupilumab response at week 16 |
Outcome
At week 16, Maya's SCORAD improved to 14 (mild), POEM to 6/28. Sleep normalized. No new infections. Mild conjunctivitis developed — managed with topical cyclosporine 0.05% eye drops. Emollients and proactive TCS maintained. Dupilumab continued long-term.
13. Complications
| Complication | Details |
|---|---|
| Eczema herpeticum | HSV superinfection; medical emergency — IV acyclovir |
| Secondary bacterial infection | S. aureus most common; MRSA possible |
| Molluscum contagiosum | More extensive in AD |
| Cataracts / Keratoconus | Particularly with periorbital eczema and eye rubbing |
| Growth retardation | With prolonged systemic corticosteroids |
| Sleep disturbance & psychiatric morbidity | Anxiety, depression, attention problems in children |
| Atopic march | AD → food allergy → asthma → allergic rhinitis (sequential progression) |
14. Prognosis
- ~60–70% of childhood AD resolves by adolescence
- Persistence predictors: severe early-onset disease, FLG mutations, sensitization to multiple allergens, concurrent asthma
- Adults with persistent AD have significant quality-of-life burden (comparable to psoriasis and diabetes)
- With biologics (dupilumab), >50% achieve EASI-75 at week 16, transforming the prognosis for moderate-to-severe disease
Summary Flowchart
ALL patients: Emollients + Trigger Avoidance + Education
↓
Mild AD → Low-potency TCS / Pimecrolimus / Crisaborole
↓
Moderate AD → Mid-potency TCS + Tacrolimus + Bleach baths
↓
Severe AD or inadequate topical response
↓
Dupilumab (preferred) OR Oral JAK inhibitor (abrocitinib/upadacitinib)
↓
Refractory: Cyclosporine / Methotrexate / NB-UVB
Key References:
- Harrison's Principles of Internal Medicine, 21st Ed., p. 1520
- Atopic Dermatitis: Update on Skin-Directed Management, p. 2
- NICE Guideline NG190: Atopic Eczema in Under 12s (2023)
- AAD Guidelines on Management of AD (2023)
- EDF/EADV Consensus on Systemic Treatment of AD (2022)
This is a shared conversation. Sign in to Orris to start your own chat.