Arthroscopic bankart repair
Reading File
Finding Sources
Finding Sources
Searching PubMed
arthroscopic Bankart repair shoulder instability
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
arthroscopic Bankart repair shoulder labrum suture anchor
Reading File
I now have comprehensive information. Let me compile the full answer.
Arthroscopic Bankart Repair (ABR)
Source: Rockwood and Green's Fractures in Adults, 10th ed. 2025
Background & Rationale
The Bankart lesion — detachment of the anteroinferior capsulolabral complex from the glenoid rim — is the pathological hallmark of traumatic anterior shoulder instability. Open Bankart repair was historically the gold standard, with recurrence rates <10%, but carries risks including subscapularis injury, arthrofibrosis, and restricted external rotation.
ABR has now supplanted open repair as the treatment of choice for most anterior instability injuries. In a MarketScan database review (2008–2012), ABR accounted for 90.5% of shoulder stabilization surgeries vs. 9.5% open procedures. Modern suture anchor techniques achieve recurrence rates comparable to open repair with superior ROM preservation.
Indications
| Category | Details |
|---|---|
| Primary | ≥2 subluxations/dislocations with anterior labral detachment |
| Primary | Recurrent anterior instability despite adequate PT |
| Relative | First-time dislocation in high-risk athlete (contact/overhead sport) with documented Bankart on MRI |
Relative Contraindications
- Uncooperative patient or active seizure disorder
- Capsular deficiency or prior thermal capsulorrhaphy
- Primary collagen disorders (Ehlers-Danlos, Marfan syndrome)
- Atraumatic instability with ligamentous laxity
- Critical glenoid bone loss >17.3% (consider Latarjet/bone block instead; lower threshold of 13.5% in high-demand athletes)
- Engaging Hill-Sachs lesion (may require remplissage or Latarjet)
- Multidirectional instability
Preoperative Planning
- Radiographs + MRA: MRA is more sensitive/specific than MRI for anteroinferior labral tears
- Glenoid bone loss quantification: Critical bone loss threshold between 13.5% and 17.3% determines shift from ABR to bony procedure
- Hill-Sachs lesion assessment
- Identify capsular redundancy, ALPSA vs. classic Bankart, HAGL lesions
Patient Positioning
Two options — surgeon preference:
- Lateral decubitus (authors' preference): Bean bag, pillow under leg (protect peroneal nerve), arm holder with Coban, 5–10 lb balanced traction with lateral distraction
- Beach chair: 70–80° flexion, head holder, spider arm holder
A small axillary bump improves glenohumeral joint distraction in both positions.
Key Surgical Steps
Portal Placement
| Portal | Location | Purpose |
|---|---|---|
| Posterior (viewing) | ~2 cm distal, 1 cm medial to posterolateral acromion | 30° scope; diagnostic arthroscopy |
| Anterolateral | ~1 cm distal to anterolateral acromion | Working portal; viewing (6 mm threaded cannula) |
| Anteroinferior | Just above subscapularis, slightly above glenoid fossa surface | Suture passing and anchor drilling (8 mm cannula) |
A 70° scope can be used in the posterior portal if visualization is difficult; alternatively the 30° scope can be placed in the anterolateral portal.
Technique
- Diagnostic arthroscopy: Evaluate labrum, rotator cuff, biceps, cartilage, glenoid bone loss, Hill-Sachs lesion
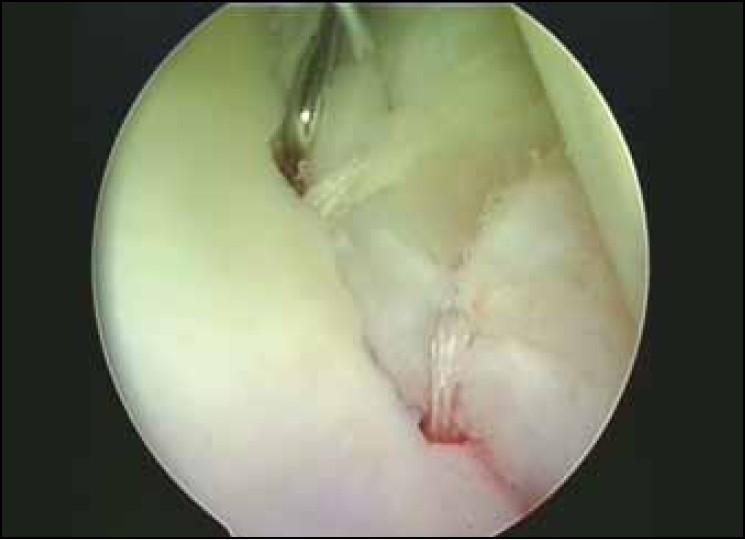
- Labral mobilization: A labral elevator (CoVator) via anterolateral portal mobilizes the anteroinferior capsulolabral complex off the glenoid rim → subscapularis muscle belly must be visible below (confirms adequate mobilization)
- Suture passing: Curved suture passer (right curve for right shoulder) penetrates capsule ~1 cm distal and 1 cm from glenoid rim via anteroinferior cannula — allows adequate superior shift and capsular volume reduction
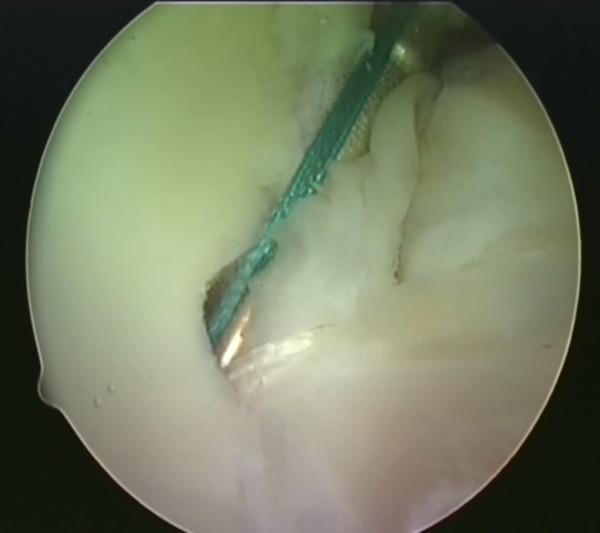
- Anchor fixation (knotless or knotted):
- Authors prefer knotless fixation (Labral Tape + Arthrex 2.9 mm PushLock anchors)
- Critical: first anchor placed at 5:30 position (right) or 6:30 position (left) on the anterior glenoid face — must be inferiorly placed
- Sequentially up to 4:30, 3:30, 2:30 (right) / 7:30, 8:30, 9:30 (left)
- Minimum 3 anchors recommended
- Endpoint: Soft tissue bumper at the chondrolabral junction confirms excellent shift of the capsulolabral complex
Outcomes
Recurrence
- Recurrence risk after ABR: ~10.7–13.1% (recent systematic reviews)
- Risk factors for failure: young age, high number of preoperative dislocations, significant bone loss (glenoid or humeral head), inferior capsule hyperlaxity
ROM
- Loss of external rotation expected: 3–9° at side, 3.5–6° at 90° abduction
- Forward flexion loss minimal (1–3°)
- ROM is superior to open repair — important for overhead-throwing athletes
Functional Scores (Long-term)
- 13-year retrospective study (n=180): VAS pain 0.0 ± 1.7, Rowe 90.0 ± 20.5, ASES 92.0 ± 17.0; patient satisfaction 92.3%
- ABR vs. open: comparable functional scores, but open Bankart has lower recurrence and ABR has better ROM
vs. Latarjet
| Parameter | ABR | Latarjet |
|---|---|---|
| Recurrence | 10.7–13.1% | ~5–10% |
| ROM | Better preserved | More restricted |
| Return to sport | ~71% | ~73% |
| Complication rate | Low (0.2–0.3%) | 10.6–15% |
Complications
| Complication | Notes |
|---|---|
| Recurrent instability | Most common adverse outcome; revise with open repair if no bone loss; Latarjet/bone block if significant glenoid deficiency |
| Postoperative stiffness | Less than open repair; main concern is ER loss |
| Neurologic injury | Musculocutaneous or axillary nerve; rate 0.3% |
| Infection | Rate 0.2% |
| Glenohumeral arthrosis | Long-term concern, less likely than after open repair |
Overall ABR complication rate is significantly lower than open Bankart (4.3%), Latarjet (10.6–15%), or bone block (17.6%).
Special Considerations
- Remplissage: Adjunct to ABR for engaging Hill-Sachs lesions — infraspinatus tenodesis into the Hill-Sachs defect; alternative is Latarjet
- Bipolar bone loss ("Glenoid track" concept): On-track vs. off-track Hill-Sachs guides whether ABR alone suffices
- Skeletally immature patients: Conservative management may be appropriate after primary dislocation without significant bone defect; surgery indicated with recurrence
- Knotless vs. knotted anchors: A 2025 meta-analysis (PMID 40483425) compares these approaches — both achieve comparable stability
Recent Evidence: A 2024 systematic review (PMID 39428642) confirms favorable outcomes for ABR in anterior shoulder instability. A 2025 meta-analysis (PMID 40483425) evaluates knotless vs. knotted techniques.
Rockwood and Green's Fractures in Adults, 10th ed. 2025 — Chapter 35, pp. 1276–1283
This is a shared conversation. Sign in to Orris to start your own chat.