Electroretinogram for 20marks
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Loading Image
Finding Sources
I now have comprehensive, well-illustrated content from two authoritative textbooks. Let me compile the full 20-mark answer.
Electroretinogram (ERG)
Definition
The electroretinogram (ERG) is a diagnostic test that measures the electrical activity of the retina in response to a light stimulus. When photoreceptors and other retinal neurons are stimulated by light, ionic flow (principally Na⁺ and K⁺) is induced, generating a potential difference that can be recorded from the corneal surface.
— Kanski's Clinical Ophthalmology, 10th ed.
Principle & Recording Setup
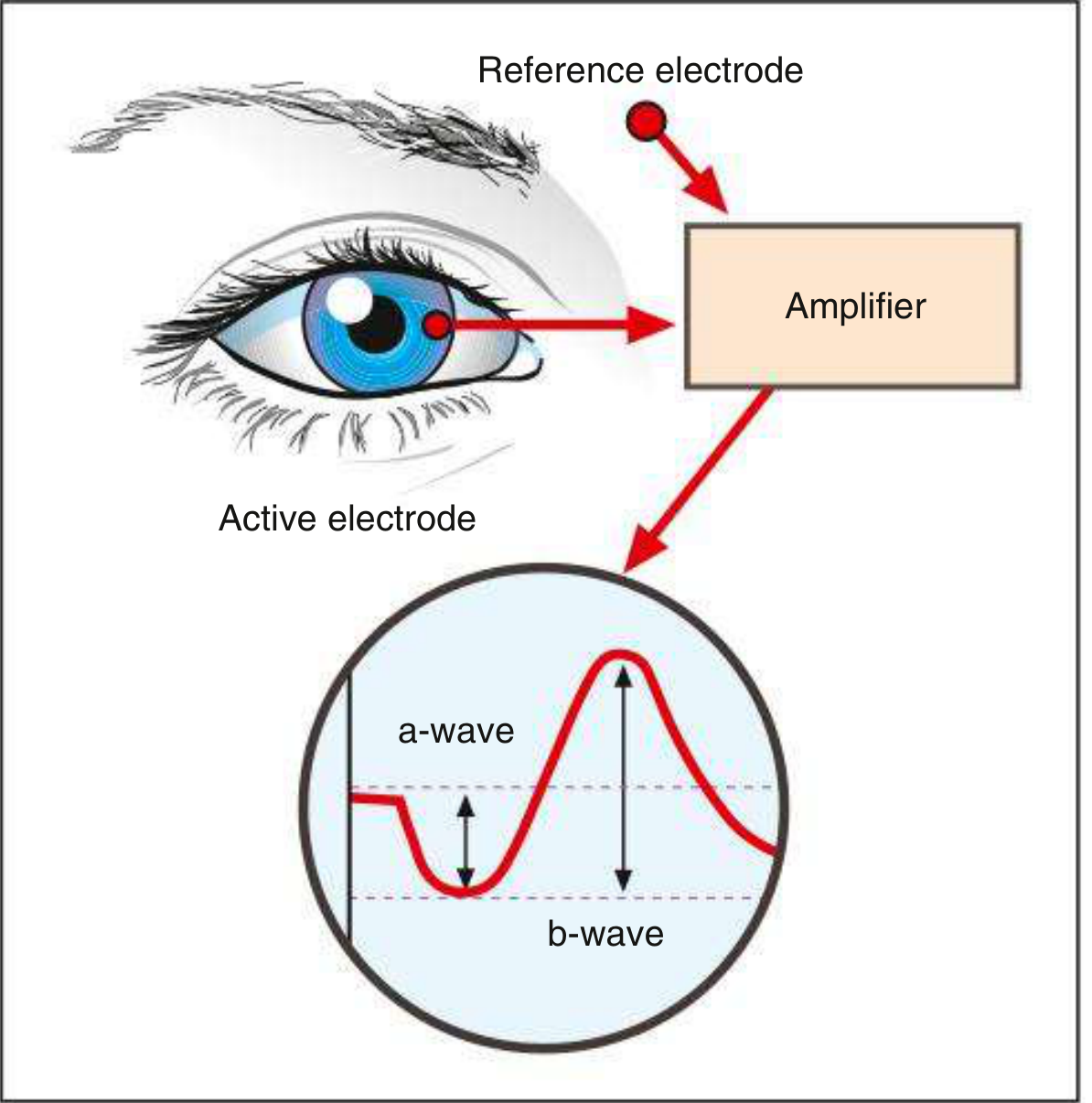
- An active (corneal) electrode — placed on or near the cornea (contact lens electrode)
- A reference electrode — placed on the forehead or earlobe
- A ground electrode — placed elsewhere on the body
- The potential difference between the two electrodes is amplified and displayed
The ERG is a summed mass response of the entire retina; normal results therefore do not exclude focal pathology.
Components of the Normal ERG Waveform
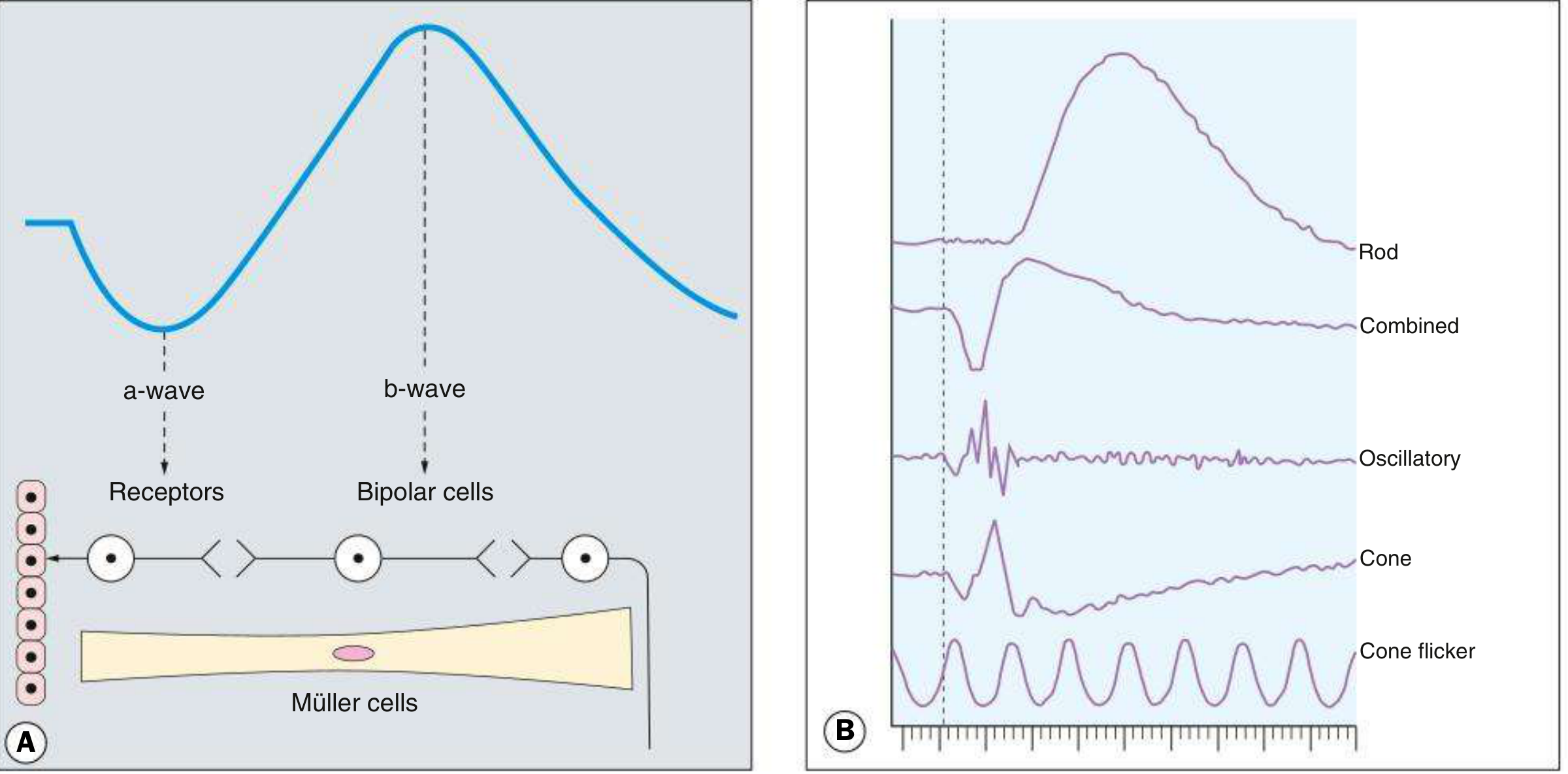
The normal ERG is predominantly biphasic:
| Component | Deflection | Origin | Significance |
|---|---|---|---|
| a-wave | Initial corneal-negative (downward) deflection | Photoreceptors (rods & cones) — hyperpolarization | Reflects photoreceptor integrity |
| b-wave | Subsequent large positive (upward) deflection | Müller cells & bipolar cells (ON-bipolar cells) — depolarization | Dependent on functional photoreceptors; most clinically useful |
| c-wave | Third negative deflection | RPE + photoreceptors | Less commonly measured clinically |
| Oscillatory potentials | Wavelets on the ascending limb of the b-wave | Inner retinal amacrine cells | Reflect inner retinal inhibitory processing |
Key measurements:
- Amplitude of b-wave — measured from the a-wave trough to the b-wave peak
- Latency — time from stimulus to commencement of the a-wave
- Implicit time — time from stimulus to b-wave peak
- b:a ratio — a reduced ratio indicates inner retinal dysfunction
Types of ERG
1. Full-field ERG (Ganzfeld ERG)
- Standardised by the International Society for Clinical Electrophysiology of Vision (ISCEV)
- Uses diffuse stimulation of the entire retina
- Consists of 6 standard recordings (ISCEV 2022 update)
- Assesses generalised retinal disorders; cannot detect localised pathology
Scotopic (dark-adapted) responses — after ≥20 min dark adaptation:
- Dim flash (0.01 cd·s/m²) → rod-only response: small b-wave, barely visible a-wave
- Bright white flash → combined rod-cone response: prominent a-wave and b-wave
- Oscillatory potentials → bright flash with modified recording parameters
Photopic (light-adapted) responses — after 10 min light adaptation (to suppress rods):
- Bright single flash → cone a- and b-wave
- 30 Hz flicker → isolates cones (rods cannot follow >20 Hz); measures cone b-wave amplitude and implicit time
2. Multifocal ERG (mfERG)
- Produces topographical maps of retinal function across the macular region
- Patient fixates on an array of flickering hexagons (scaled for photoreceptor density — smaller stimulus at the fovea where density is high)
- Results displayed as a 3D plot resembling the hill of vision
- Used in: early cone-rod dystrophies (occult macular dystrophy), autoimmune retinopathies (normal fundal appearance), macular RP
3. Pattern ERG (PERG)
- Uses pattern-reversal stimulus (same as VEP)
- Targets retinal ganglion cell function
- Used to detect subtle optic neuropathy and early glaucoma
4. Focal ERG
- Assesses macular function specifically
- Rarely used clinically
Interpretation Patterns
| ERG Pattern | Meaning | Associated Conditions |
|---|---|---|
| Extinguished (flat) ERG | No recordable responses | Advanced retinitis pigmentosa, cancer-associated retinopathy (CAR) |
| Electronegative ERG (b-wave < a-wave) | Impaired photoreceptor-to-bipolar cell signalling | CRAO, congenital stationary night blindness (CSNB), melanoma-associated retinopathy (MAR), X-linked retinoschisis |
| Selectively impaired rod responses | Rod-cone dystrophy | Retinitis pigmentosa |
| Selectively impaired cone responses | Cone/cone-rod dystrophy | Cone dystrophy |
| Reduced oscillatory potentials | Inner retinal amacrine cell dysfunction | Early diabetic retinopathy, mild CRVO |
| Prolonged implicit time | Delayed retinal signal transmission | Clinically significant in various dystrophies |
Clinical Applications
- Diagnosis of inherited retinal dystrophies — retinitis pigmentosa, cone-rod dystrophy, CSNB, Leber congenital amaurosis
- Monitoring disease progression in dystrophies and uveitis (e.g., birdshot retinopathy)
- Drug toxicity monitoring — e.g., hydroxychloroquine, vigabatrin toxicity
- Detecting retinal ischaemia — CRAO, CRVO, diabetic retinopathy
- Paraneoplastic retinopathies — CAR (extinguished ERG), MAR (electronegative ERG)
- Intraocular foreign body (IOFB) — serial ERGs to monitor for siderosis
- Screening before surgery — assessing retinal function when media are opaque (dense cataract, vitreous haemorrhage) before vitreoretinal surgery
- Neonatal/paediatric evaluation — visual function in infants unable to cooperate with subjective tests
Comparison: ERG vs EOG
| Feature | ERG | EOG (Electro-oculogram) |
|---|---|---|
| What it measures | Mass retinal electrical activity | Standing potential (cornea-positive, fundus-negative) |
| Origin | Photoreceptors, bipolar/Müller cells, RPE | RPE and photoreceptors |
| Key result | Wave amplitudes & implicit times | Arden ratio (light peak ÷ dark trough) |
| Normal Arden ratio | — | ≥1.85 |
| Classic disorder | Retinitis pigmentosa (extinguished ERG) | Best disease (markedly reduced EOG, normal ERG) |
Important Points for Examination
- ERG is a mass retinal response — cannot detect localised disease
- The b-wave is larger than the a-wave under normal conditions
- Dark adaptation for 30 min is required before scotopic testing; 10 min light adaptation for photopic testing
- An electronegative ERG (b/a ratio <1) is a critical diagnostic clue for CSNB, MAR, CRAO
- Retinitis pigmentosa → rods affected first → scotopic ERG reduced earlier than photopic
- Pattern ERG assesses ganglion cells; mfERG maps macular function
- Standardised by ISCEV (International Society for Clinical Electrophysiology of Vision)
Sources: Kanski's Clinical Ophthalmology: A Systematic Approach, 10th edition | Bradley and Daroff's Neurology in Clinical Practice
This is a shared conversation. Sign in to Orris to start your own chat.