Conjuctivitis childreb
Reading File
Finding Sources
Searching PubMed
conjunctivitis children management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Loading Image
Reading File
I now have sufficient comprehensive content. Here is the full clinical overview:
Conjunctivitis in Children
Conjunctivitis is inflammation of the conjunctiva and one of the most common causes of "red eye" in the paediatric age group. Most cases are viral, benign, and self-limited — the key clinical task is identifying the minority of cases that require urgent treatment.
Aetiology
| Type | Common Causes |
|---|---|
| Viral | Adenovirus (most common), herpes simplex, measles, influenza, mumps |
| Bacterial | S. pneumoniae, H. influenzae, Staphylococcus spp., Neisseria gonorrhoeae, Chlamydia trachomatis |
| Allergic | Environmental allergens, atopy |
| Other | Toxic, chemical irritation |
Clinical Features by Type
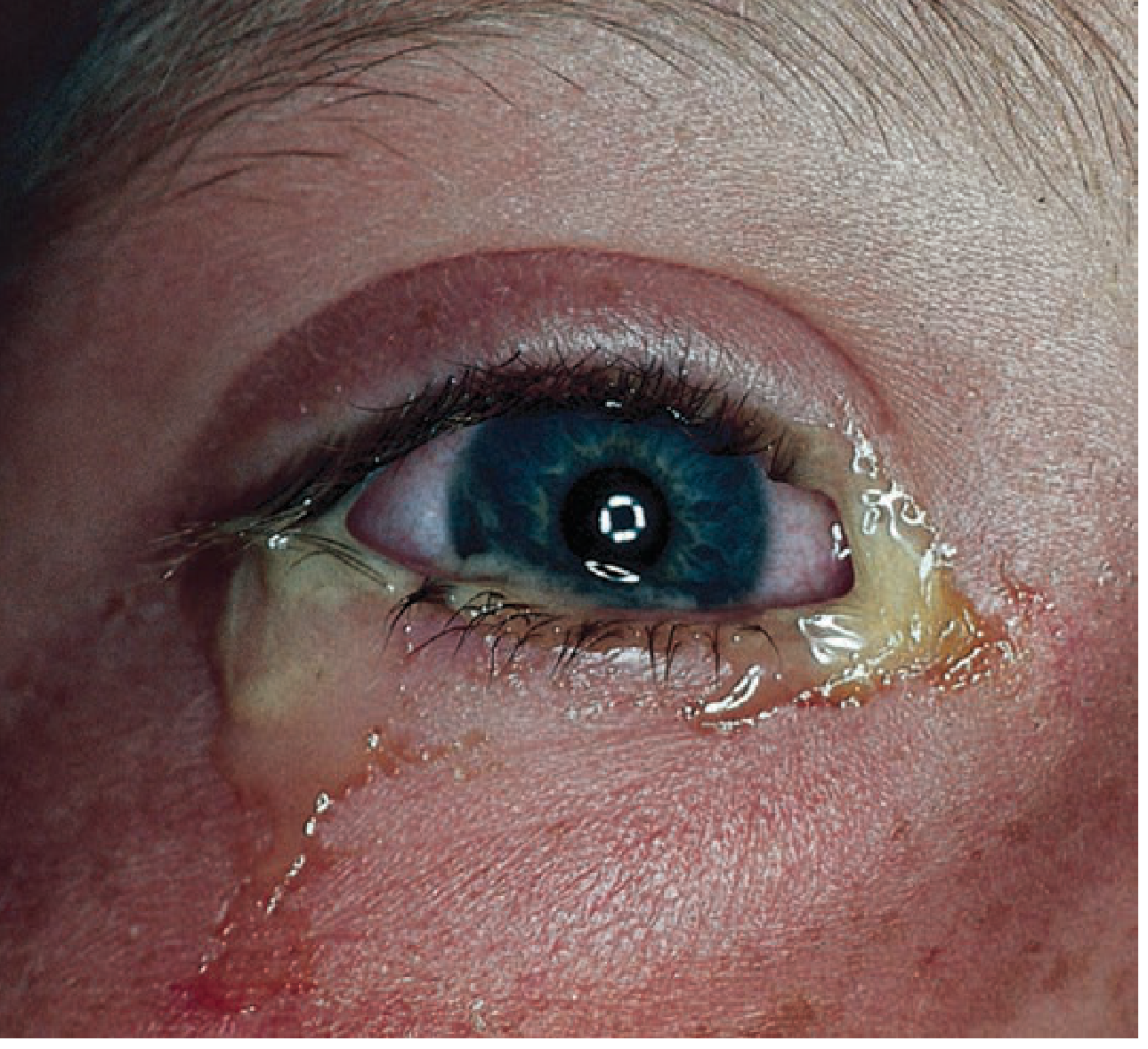
1. Bacterial Conjunctivitis
- Discharge: mucopurulent, often causing eyelid adherence on waking
- Usually painless; starts unilateral, may become bilateral
- Conjunctiva injected; cornea clear
- Chemosis (conjunctival oedema) is common
- Preauricular lymphadenopathy is absent (except in gonococcal infection)
- Typical pathogens: Staphylococcus and Streptococcus spp.
- H. influenzae is a common childhood pathogen
2. Viral Conjunctivitis
- Often preceded by upper respiratory infection or systemic viral illness
- Watery discharge, "red eye," mild to moderate
- One eye involved initially → other eye within days
- Physical exam: conjunctival injection ± chemosis, small subconjunctival haemorrhages, preauricular lymphadenopathy, follicles on inferior palpebral conjunctiva
- Epidemic keratoconjunctivitis (EKC): severe adenoviral form — high fever, malaise, myalgias, photophobia, marked redness; highly contagious
- Always examine cornea with fluorescein to exclude herpetic dendrite
3. Allergic Conjunctivitis
- Watery discharge + itching (hallmark symptom)
- Erythematous swollen eyelids, injected/oedematous conjunctiva
- Papillae on inferior conjunctival fornix (vs. follicles in viral)
- Prominent chemosis may be seen
- Associated with atopy/allergic rhinitis
4. Neonatal Conjunctivitis (Ophthalmia Neonatorum) — special case
- Gonococcal: profuse purulent discharge, requires systemic treatment
- Chlamydial: most common infectious cause in neonates — requires systemic antibiotics (not just topical)
Diagnosis
- Primarily clinical
- Always perform fluorescein staining — especially in infants — to exclude corneal abrasion, ulcer, or herpetic dendrite
- Culture and sensitivity in severe bacterial cases
- Key distinguishing features:
- Itching → allergic
- Watery discharge + lymphadenopathy → viral
- Purulent discharge + lid adherence, no itch → bacterial
- Fever + purulent discharge → bacterial
Management
Bacterial Conjunctivitis
- Most cases are self-limited but antibiotics shorten duration
- First-line: Trimethoprim–polymyxin B eye drops — effective, avoids sulfa/neomycin allergy risks
- Ophthalmic ointments are preferred in young children (easier to administer)
- Contact lens wearers → treat with a fluoroquinolone (besifloxacin, gatifloxacin, moxifloxacin, ofloxacin) or tobramycin to cover Pseudomonas
- Gonococcal/chlamydial: requires systemic antibiotics in addition to topical therapy
Viral Conjunctivitis
- Supportive care — no antivirals for adenovirus
- Cool compresses; artificial tears 5–6×/day
- Ocular decongestants (e.g., Naphcon-A) for redness/congestion
- Course: 1–3 weeks; very contagious → strict hand hygiene, separate towels
- If viral vs. bacterial is uncertain → prescribe topical antibiotics empirically and reassess
Allergic Conjunctivitis
- Identify and eliminate the offending allergen
- Cool compresses 4× daily
- Mild: artificial tears alone
- Moderate–severe: topical antihistamine/mast cell stabilisers (olopatadine, ketotifen, azelastine, bepotastine, emedastine)
- Avoid topical steroids unless directed by ophthalmologist
When to Refer to Ophthalmology
- Photophobia or vision loss
- Severe pain
- Recurrent episodes
- Suspected gonococcal infection
- No improvement with treatment
- Contact lens wearer with worsening symptoms
Key Differences from Adult Presentation
- H. influenzae is a more prominent pathogen in children
- Ointment formulations are preferred over drops in young children
- Neonatal conjunctivitis is a distinct entity requiring specific workup and systemic treatment
- School exclusion should follow local policy — bacterial/viral forms are highly contagious
Sources: Tintinalli's Emergency Medicine, p. 1582–1583 | The Harriet Lane Handbook, 23rd ed. (Ophthalmology reference table)
This is a shared conversation. Sign in to Orris to start your own chat.